Background
Gastric volvulus stands out as a rare condition to be diagnosed and is linked to a significant mortality rate among cases of acute abdominal pain presented in the emergency department (ED). The presenting complaint is usually due to symptoms related to gastric outlet obstruction, which might include abdominal pain, nausea and vomiting, bowel obstruction, and even perforation or peritonitis [1].
Gastric volvulus is considered a surgical emergency, prompting an appropriate approach to diagnosis and treatment [2]. Delay in either might lead to tissue ischemia and necrosis, followed by perforation and ultimately mortality [3]. This case report presents the case with a literature review, including the pathophysiology, clinical presentation, diagnosis, and early management of Gastric volvulus.
Case Presentation
A 78-year-old female was presented to the ED with a chief complaint of epigastric pain that started 2 hours prior. The patient reported a constant, severe, nonradiating epigastric pain, sharp in nature, with no alleviating or aggravating factor, associated with nausea and one episode of nonbloody and nonbilious vomiting. The remainder history was unremarkable.
The patient had a past medical history of hypertension, diabetes mellitus, dyslipidemia, gastroesophageal reflux disease (GERD), and Barrett’s esophagus diagnosed on upper endoscopy done in the year 2013. The patient’s vital signs were as blood pressure of 166/78 mmHg, heart rate of 73 beats/minute, temperature of 36.8 Celsius, respiratory rate of 20 breaths/minute, and oxygen saturation of 99% on room air.
Physical examination of the abdomen revealed an unremarkable inspection, while palpation yielded mild epigastric tenderness not associated with rigidity, guarding, or rebound tenderness. The rest of the physical examination was unremarkable. The working differentials at this point were biliary colic, cholecystitis, pancreatitis, GERD, peptic ulcer disease, gastritis, gastroenteritis, and atypical presentation of a myocardial infarction. Blood investigations included full blood count, liver function tests, kidney function tests, and levels of troponin, lipase, and blood glucose. The imaging modality was a plain abdominal radiograph, and an electrocardiogram (ECG) was requested (Figure 1).
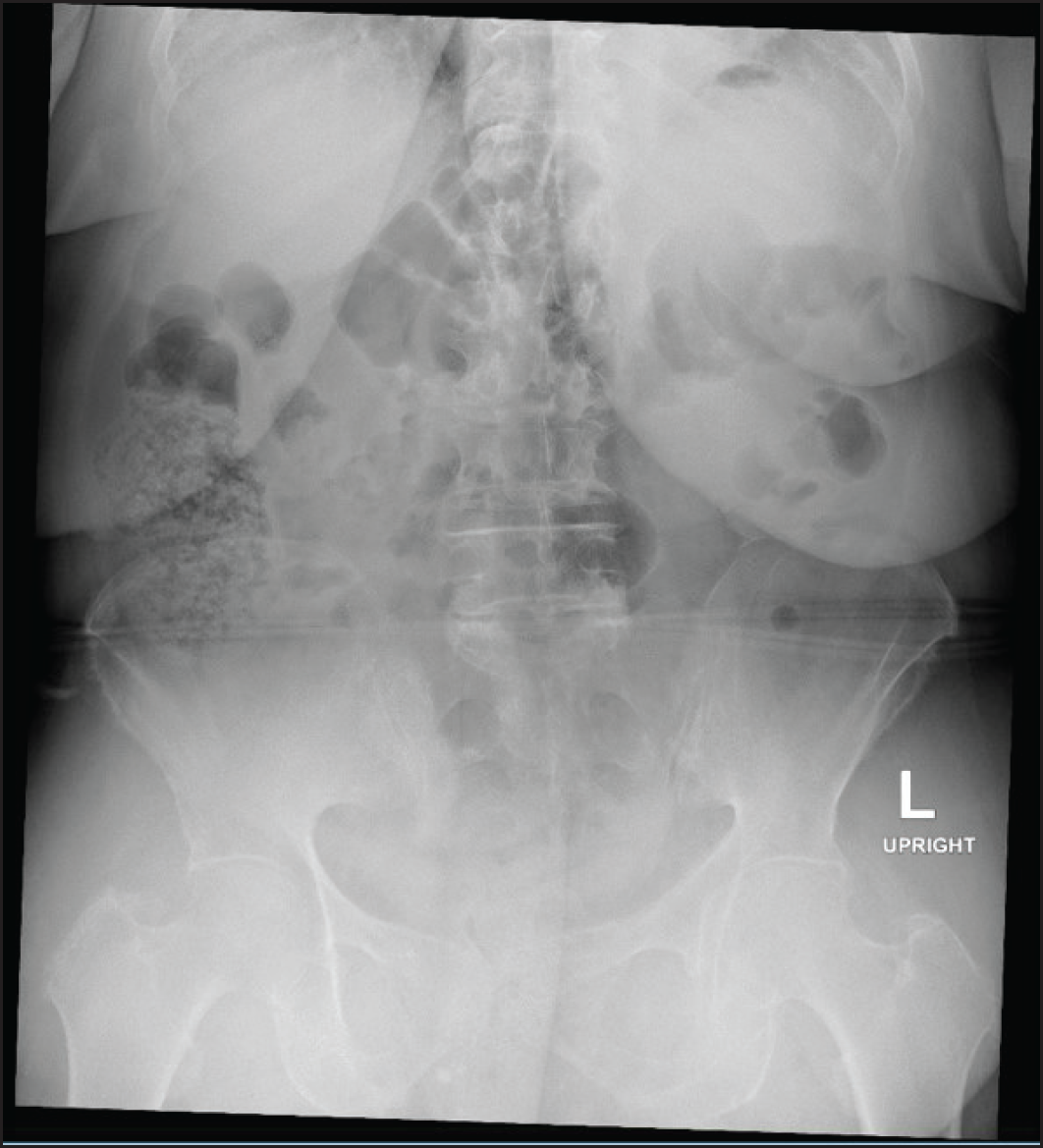
As for the initial management of the patient’s current complaints, parenteral ondansetron of 4 mg, pantoprazole of 40 mg, and paracetamol 1 g along with half a liter of intravenous (IV) normal saline were administered. The patient’s pain index decreased after the initial symptomatic management. Blood results were unremarkable except for a creatinine of 85 micromoles/l and an eGFR of 57 ml/minute. The patient continued to complain of epigastric pain and tenderness, and an abnormal plain radiograph was reported to only show fecal loading in the colon with no free gas or dilated bowel loops (Figure 2).
Fecal loading of the colon. No free gas or distended bowel loops. The appearance is nonspecific.
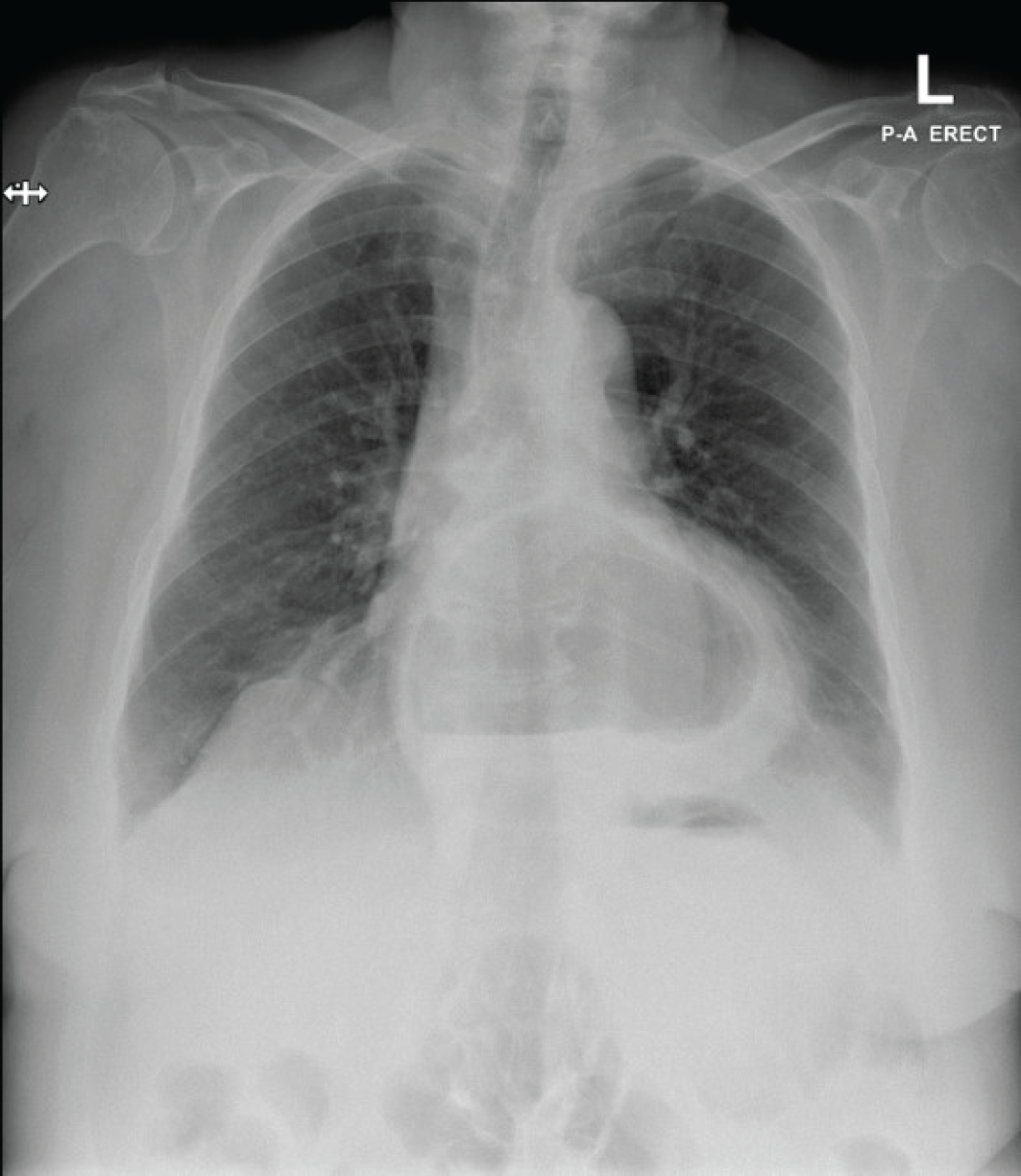
Upon review, the patient had another episode of vomiting; a chest X-ray (CXR) was then obtained that showed a large hiatal hernia, which was not mentioned in the patient’s medical records and was not present in the previous CXR (Figure 3).
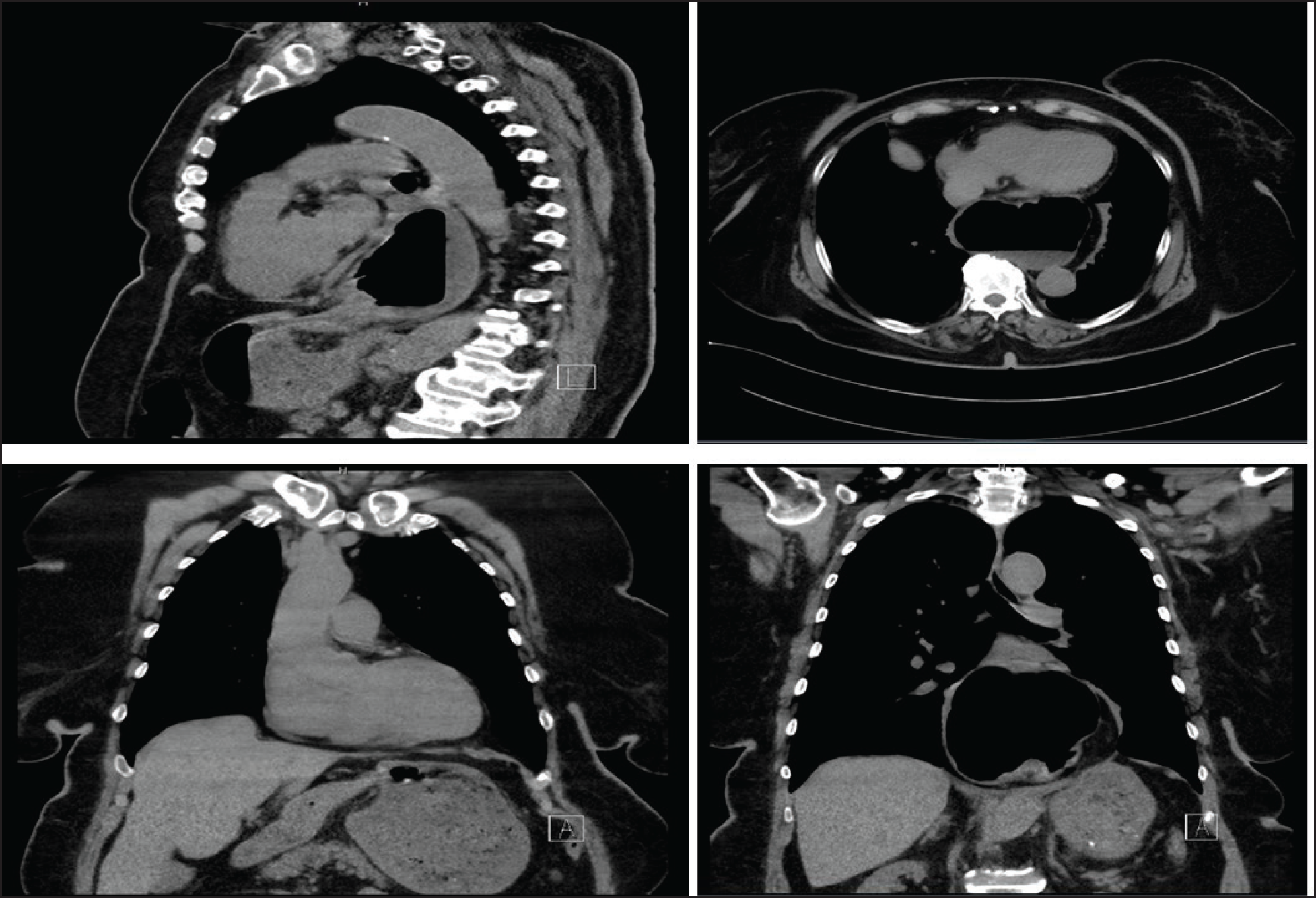
Attempts to insert a nasogastric tube in the ED were failed. The case was discussed with the general surgery team, and it was advised to proceed with a noncontrast computed tomography (CT) scan, which showed a large hiatus hernia behind the heart. There was a twist in the gastric mesentery with breaking at the point of twist, which is suspicious for mesenteroaxial gastric volvulus, with the antrum lying superior to the fundus in the thoracic cavity. Mucosal edema of the thoracic part of staunch was also noticed (Figure 4).
At this point in time, the general surgeons were consulted again to review and assess the patient. The plan was to proceed with admission, keeping the patient nil by mouth, providing IV fluids and analgesia with a decision to undergo laparoscopic repair of the hiatus hernia and gastric volvulus under general anesthesia the following day. The procedure note reported a diagnosis of type two hiatal hernia complicated by gastric volvulus; the surgical repair proceeded uneventfully, a nasogastric tube was inserted intraoperatively, and the patient was shifted to the surgical intensive care unit (ICU) for 1 day.
The patient’s vital signs were within normal limits, and she was under ICU observation for 1 day. Antibiotics, including third-generation cephalosporin and metronidazole, were given. The following day, the patient was extubated and shifted to the surgical ward for observation for the following 4 days, with the nasogastric tube being removed on day 2. On day 4 post-operatively, the patient tolerated oral intake well with no nausea, vomiting, or ambulation and no current complaints.
The patient was discharged home with a follow-up appointment at the surgery clinic and instructed to return to ED if any signs of infection or intestinal obstruction arose. During follow up the week after, the patient had mild surgical wound pain but denied epigastric pain, and the GERD symptoms also improved significantly.
Discussion
In common with many modern medical terminologies, the word volvulus is derived from the Latin word “Volvere,” which means to twist or roll [4]. Gastric volvulus is a rare but severe condition when the stomach twists on its axis, disrupting the normal flow of food and digestive juices. It can cause symptoms such as abdominal pain, nausea, vomiting, and bloating, leading to tissue death and perforation, if left untreated.
Approximately 282 acute cases of gastric volvulus have been reported between 1929 and 2007, with a mortality rate of 65% despite the proper diagnosis and surgical management [5]. The peak age for developing gastric volvulus occurs after the fifth decade, accounting for almost 90% of the cases [6].
Gastric volvulus can present acutely or with chronic symptoms. Acute volvulus is classically associated with Borchardt’s triad, first identified in 1904, which includes retching without vomiting, epigastric pain and distention, and the inability to pass a nasogastric tube [2]. This triad is seen in up to 70% of patients [7].
Meanwhile, chronic volvulus can be easily mistaken for peptic ulcer disease, as they both might be presented with mild pain, heartburn, and dysphagia [7]. Gastric volvulus can also be classified based on etiology or the axis of rotation. The etiological classification is divided into primary and secondary gastric volvulus. It is considered primary when it originates from the stomach or any of its anchoring ligaments and secondary when arises from any nearby structures, such as the diaphragm or esophagus. Secondary gastric volvulus represents 70% of cases [4]. The four main ligaments that maintain the stomach in its rightful axis are the gastrocolic, gastrohepatic, gastrosplenic, and gastrophrenic ligaments.
CXR showed a large hiatus hernia behind the heart. Normal heart size. No focal collapse or consolidation. No free gas under the diaphragm.
CT without contrast thorax and abdomen showing large hiatus hernia and twist in the gastric mesentery, which is suspicious for mesenteroaxial gastric volvulus.
Furthermore, the gastroesophageal junction is a cornerstone for anchoring the stomach and preventing malrotation. Thus, any disruption in the former structures might predispose to developing gastric volvulus. Other risk factors for gastric volvulus include hiatal hernia, previous abdominal surgery, and conditions that cause a weak or lax stomach wall, such as chronic vomiting or malnutrition. In this case, the patient had an incidental finding of a sliding hiatal hernia in which the upper part of the stomach protrudes through the diaphragm into the chest. This increases the risk of gastric volvulus by allowing the stomach to rotate more easily. Most cases of hiatal hernia are asymptomatic or present as vague, intermittent epigastric pain that can be confused with GERD. Furthermore, the patient presented with sudden onset of abdominal pain, vomiting, and distention, common symptoms of gastric volvulus. The current presented case had two components of Borchardt’s triad: epigastric pain and distension, and the failure to pass a nasogastric tube.
Diagnostic radiographic imaging techniques, such as plain radiography and CT scan, are important tools for diagnosing gastric volvulus. It is crucial to consider the patient’s symptoms and risk factors and the findings of imaging studies when making the diagnosis. Sometimes, it can be visualized as a retrocardiac air-filled mass on a CXR [7]. Additional tests, such as an upper GI series or upper GI endoscopy, might be required in other cases.
Gastric volvulus might show a distended, fluid-filled stomach in the thorax on an upper GI series; meanwhile, on CT imaging, it would appear as a dilated stomach, falsely allocated in the chest, which is the case in the presented patient. Notably, the presented patient had mesenteroaxial volvulus, which is not commonly seen with diaphragmatic defects.
Another sign that might be found on CT is a Swirl Sign, which results from the rotations of the stomach and the esophagus around one another on transverse plane imaging. Gastric necrosis might also be visualized on CT; evidence would involve pneumatosis of the gastric wall, free fluid, and air outside the stomach or lack of a contrast enhancement of the contrast. CT imaging is slowly replacing upper barium swallow due to increased availability and decreased cost of scanning. It can attain a more definitive diagnosis, identify other causes of abdominal pain, and better assess the extent of gastric herniation and the position of the stomach, all vital information for the surgeon operating on the patient.
Furthermore, the presence or absence of ischemia can guide whether the operation should be done urgently or emergently. In addition, it is noteworthy that in some cases, gastric volvulus might be intermittent or resolve spontaneously [8]. This poses a further challenge for diagnosis and management as the patient might present after spontaneous hernia reduction and show no pathology on imaging studies.
It is also important to note that the management of gastric volvulus might vary depending on the severity of the condition and the presence of complications. Inserting a nasogastric tube is typically a first step in managing acute gastric volvulus, as it can help decompress the stomach and alleviate symptoms. The patient should simultaneously undergo IV fluid resuscitation and electrolyte correction in cases of repeated vomiting episodes or decreased oral intake.
ECG 12 lead showed sinus rhythm, normal PR interval, and low voltage with T wave inversion in lead III.
A nasogastric tube should be inserted with the patient kept prone to facilitate gastric decompression [7]. Sometimes, placing a nasogastric tube can be difficult without endoscopic guidance. This is time-consuming and might delay definitive surgical intervention. Despite having a multisource blood supply, which might delay ischemia, the stomach is still prone to necrosis or perforation, meaning surgical intervention might be necessary to repair the damage and prevent further complications. Thus, a prompt surgical consultation was requested to help reduce morbidity due to ischemic necrosis and mortality [7].
The main surgical approaches for gastric volvulus include an open or laparoscopic approach to reduction with or without gastropexy. Other techniques, such as partial gastrectomy and fundo-antral gastrogastrostomy (Opolzer’s operation), are now less frequently employed. Moreover, when present, diaphragmatic hernia repair is also indicated to prevent recurrence. Laparoscopic surgery is a minimally invasive procedure that involves making small incisions and using specialized instruments to repair the stomach. It has several advantages over open surgery, including shorter recovery time, less scarring, and fewer complications. In this case, a laparoscopic approach allowed the surgeon to reduce the stomach and directly assess for necrotic damage, resulting in a successful outcome for the patient. The nasogastric tube was removed on Day 2 post-operatively, and the patient recovered uneventfully, she had follow up in the outpatient clinic post-operatively with no complaints or complications.
An alternative to surgical management is endoscopic detorsion, which might be indicated if the patient has multiple co-morbidities and cannot tolerate general anesthesia. It can also be done temporarily without surgical service before definitive surgical treatment, such as laparoscopic hernia repair or abdominal wall gastropexy. However, it is associated with a higher recurrence rate when not followed up with definitive fixation or the repair of the diaphragmatic defect. On the other hand, it has the advantage of directly visualizing the mucosa to assess for ischemia. Several cases have been reported with successful endoscopic detorsion [8-11], with some even securing an anterior gastropexy via PEG tube placement [10].
This case highlighted the importance of considering gastric volvulus in the differential diagnosis of acute abdominal pain, especially in patients with underlying risk factors such as hiatal hernia. Early recognition and appropriate treatment can be crucial in successfully managing this condition. A high index of suspicion is needed to reach the diagnosis, especially in the case of intermittent volvulus or patients who are not known to have diaphragmatic defects. Further research is required to identify strategies for preventing gastric volvulus, perhaps through prophylactic hiatal hernia repair. This might help in improving the outcomes in affected patients.
Conclusion
Acute gastric volvulus is a rare but serious condition that requires prompt diagnosis and treatment. In this case, the patient’s underlying risk factor of sliding hiatal hernia likely contributed to the development of gastric volvulus. Early recognition and laparoscopic repair were crucial in successfully managing this patient’s condition. This case highlights the importance of considering gastric volvulus in the differential diagnosis of acute abdominal pain, especially in patients with underlying risk factors.

