Background
Gas embolism is an uncommon and often preventable iatrogenic complication. Any air/gas entering the circulation could embolize distal capillaries and can result in tissue ischemia in vital organs. Organs with high blood flow and lack of collateral circulation are most vulnerable with the brain and heart at the biggest risk [1,2]. The symptoms of cerebral gas embolism (CGE) range from focal weakness, cranial nerve dysfunction, convulsions, and coma to irreversible cardiovascular collapse and death. In patients with a peri-procedural stroke or neurological event, the diagnosis of gas embolism should be considered and urgently diagnosed or ruled out to avoid delays in treatment.
Hyperbaric oxygen therapy (HBOT) is the treatment of choice for CGE and early referral is essential. A target of 6-7 hours is suggested in the literature to aim for a good outcome but clearly the sooner the better as every minute counts [3,4]. However, HBOT has been shown to be beneficial with full recovery even after delays as long as 60 hours [5] and late treatment should still be considered.
Case Presentation
A 64-year-old male was initially admitted to a cardiology center for investigation of a 2-year history of chest pains on exertion and shortness of breath. His past medical history included suspected coronary and peripheral vascular disease.
A ventriculogram was performed after his scheduled coronary angiography. Air was noted to be injected into the ventricle and the patient had a cardiac arrest. He was intubated immediately and successfully resuscitated. Diagnostic images were reviewed, and a computed tomography (CT) head was ordered on suspicion of CGE. Angiography and trans-thoracic echo confirmed air in the left ventricle and the CT scan of the brain showed extensive locules of air within the brain with surrounding ischemic changes (Figure 1). No sign of air in the coronary vessels was identified nor was there any ischemic change on ECG.
The significant delay in transfer due to logistical reasons raised concern about potential viability and the risk versus benefit associated with a long transfer was debated. A decision was made to perform a sedation hold to reassess neurological status by the referring unit which showed that the patient’s reflexes were hypertonic with extensor plantar reflexes. Thus, the conclusion was that there was some hope and benefit in transferring him to HBOT after all. Two seizure episodes occurred meanwhile which were treated with phenytoin.
He was transferred to a hemodynamically stable condition on sedative infusions for further management. On arrival at our unit, 14 hours after the event, it was noticed that the patient was having intermittent seizures despite the phenytoin loading dose and continuous propofol, remifentanil, and midazolam infusions.
The US Air Force variant of the US Navy Treatment Table 6 HBOT protocol [6] was started within 35 minutes of arrival, which resulted in the cessation of seizures within 20 minutes.
A CT scan of the brain done 48 hours after arrival demonstrated mild edema of the brain in the fronto-parietal aspect of the right cerebral hemisphere. Ongoing ventilation required continuous sedation, and this caused difficulty in excluding minor improvements in neurology to determine the point where a plateau is reached. A further four more HBOT sessions (US Navy TT9 equivalent) were provided during the following 72 hours [6] and at this point, no further improvement could be demonstrated.
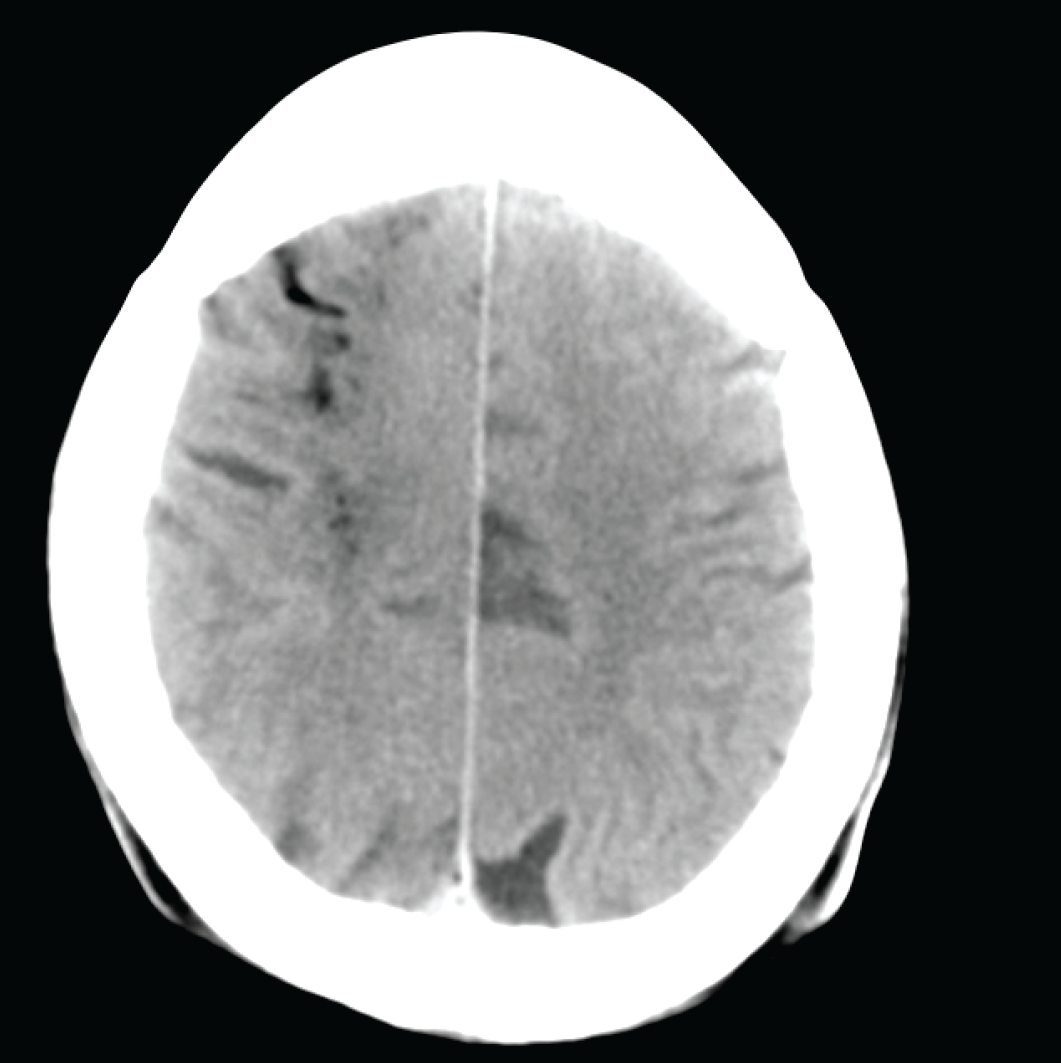
Noncontrast CT Brain immediately post cardiac arrest and successful resuscitation of the patient showing air locules.
Weaning from the ventilator was delayed, as the patient developed pneumonia, which was treated. He was eventually discharged home with near full recovery, except for mild left hemiparesis.
Discussion
CGE is often, an iatrogenic complication that can occur due to arterial, venous, or retrograde cerebral venous gas embolism but can also be seen as a complication of diving, explosions, or thoracic trauma [7].
Many etiological factors have been implicated, e.g.,
Placement, maintenance, and removal of central venous and dialysis catheters and sometimes, peripheral venous lines as well.
Numerous surgical procedures [4].
Trauma, including diving events.
Interventional radiology and endoscopy procedures.
Intra-cardiac air may lead to cardiac arrest due to blood ejection failure or embolization to the coronary and cerebral arteries, leading to arrhythmia or cardiac and cerebral ischemia with significant organ damage. In the sitting position (e.g., during neurosurgery) gas would tend to embolize the cerebral circulation due to buoyancy [4].
It is important to keep in mind that many episodes of gas embolism are preventable and thus all preventative steps should be put in place.
Even though no randomized trial has ever been performed on this subject, there is a class I recommendation for HBOT in the treatment of CGE [8]; however, many clinicians remain reluctant to refer patients for HBOT, leading to underuse of a possibly highly effective intervention.
Fakkert et al. [9] in their systemic review and meta-analysis showed that patients with favorable outcomes were treated with HBOT 2.4 hours (95% CI 0.6-9.7) earlier than patients with unfavorable outcomes. However, their data suggest that the relationship between time-to-HBOT and outcome should not be seen as an on-off phenomenon with a cutoff point at 6-8 hour, but rather as a continuum in which sooner is better as time is the brain. Although they have adjusted their model for severity of manifestations, residual confounding may still be present. For instance, delayed start of HBOT may be indicative of delayed recognition and diagnosis of CGE. It may be possible that patients with the early start of HBOT were already admitted to a center with a hyperbaric chamber, and the presence of such a chamber may be related to increased clinical awareness. However, as several cases have been published with delays of more than 24 hours, in which there was a clear temporal relationship between HBOT and improvement of neurological status [10-12], they recommend considering HBOT even in cases with prolonged delay.
Several other reports of good outcomes with HBOT have been noted, e.g., Dutka [13] reports that in 230 cases treated with HBOT, 206 fully recovered (89%), and only 10 deaths were reported. In 586 untreated cases, there were 375 recoveries (65%) and 123 deaths.
Bitterman and Melamed [5] used HBO 15-60 hours after the embolic event with good outcomes in three out of five patients.
A study of nine patients [14] with hemodialysis-associated CGE who received conventional treatment demonstrated little improvement. Once HBOT was instituted, there was dramatic improvement within 10 minutes in seven of the patients and with resolution in the other two patients following an extended HBOT treatment regimen.
Another series of 30 patients [15] found near or complete resolution of symptoms following HBOT in 24 of the patients while only two died.
The proposed mechanisms of damage due to CGE include direct arterial occlusion as well as circulatory arrest or hypotension. The gas emboli can cause stripping of the vascular endothelium from the underlying basement membrane and thus can cause a progressive decrease in cerebral blood flow without vessel occlusion due to clumping of neutrophils in damaged arterioles. In addition, bubble regrowth, secondary thrombotic occlusion, and edema can lead to delayed deterioration even though there appears to be an initial clinical improvement [1].
Large volumes of gas entering the arterial system will result in immediate coronary or cerebral embolic occlusion and death.
Smaller volumes may reach peripheral capillary beds with less severe consequences. The research done on intra-coronary artery gas embolism in an animal model has demonstrated that as little as 0.02 ml/kg can lead to death, so all gas embolisms should be regarded as serious [7].
The beneficial effects of HBOT are due to several mechanisms, including reduction of air bubble size, facilitating nitrogen washout, lowering of intracranial pressure by cerebral vasoconstriction, and still, providing high arterial and tissue oxygen tension for the ischemic penumbra. Redistribution of smaller gas emboli from cerebral arteries to the venous circulation facilitates a further improvement in microcirculation [5].
It is imperative that physicians dealing with patients at risk of gas embolism as well as resuscitation teams should be aware of immediate management protocols and what services are available for the provision of HBOT, should this complication occur as this expertise varies from country to country. One limitation of HBOT is the location of hyperbaric chambers mostly in coastal areas due to the link with diving activities, necessitating the transfer of critically ill patients, which should be considered carefully and if feasible, HBOT should be considered immediately in cases of gas embolism.
The Intensive Care Society, UK, provides clear guidelines for the immediate management of patients with suspected CGE and gives contact numbers for the nearest hyperbaric unit. It is important that intensive care units are aware of these guidelines and where the nearest hyperbaric unit is located [4].
Conclusion
Cerebral air embolism is most often an iatrogenic and preventable complication of many invasive procedures.
All new neurological symptoms after an invasive procedure, should raise the suspicion of CGE.
Early referral and awareness of HBOT are important to ensure the best possible outcome for patients.
Delayed HBOT can still be effective and potentially lifesaving.

