Background
Uncommon and possibly fatal, spontaneous hemopneumothorax needs to be identified and treated promptly. It is mostly seen in 3% of patients with spontaneous pneumothorax [1] and is characterized by air and blood in the pleural space, which can lead to breathing difficulties, chest pain, and hemodynamic instability. While underlying lung disease or adhesion tears in spontaneous pneumothorax are assumed to be the causes of spontaneous hemopneumothorax, vascular aberrancy is a rather uncommon cause [2]. In this case study, we discuss a patient who, despite having an initially normal radiography, presented to our emergency department (ED) complaining of left-sided chest pain and shortness of breath and on further evaluation was found to have a spontaneous hemopneumothorax.
Case Presentation
The ED of a tertiary care hospital received a visit from a man in his 20s with back and left-sided chest pain at around 9:00 AM. The patient also complained of shortness of breath along with moderate to severe pain that started suddenly while at rest. He had undergone a chest X-ray (CXR) and blood tests to look for signs of pneumothorax. Once his X-ray and blood tests were reported normal, he was discharged on oral analgesia.
Throughout the day, his suffering worsened. This led him to visit his local General Practitioner (GP) who advised him to take analgesia and was discharged. By evening, he was increasingly breathless and restless, which then led him to call the emergency medical services (EMSs). Initial examinations by the EMS personnel revealed that he was tachypneic, tachycardic, and hypotensive; however, his oxygen saturation was 91%. When he was first assessed in our ED, he appeared frightened, was tachypneic, and in pain. Upon auscultation of his chest, the patient had good air entry on the right side in contrast to absent air entry on the left side. The patient also had resonant percussion on the left upper chest while having stony dullness on the left chest base. A CXR was performed following the administration of analgesia (Figure 1), and the results of a Venous Blood Gas (VBG) showed (pH 7.29, PCO2 7.45 kPa, PO2 2.01 kPa, cHCO3 26.3 mmol/l, lactate 3.2 mmol/l, and HB 127 g/l).
On the guidance of the cardiothoracic specialists, a chest tube was inserted using a Seldinger technique, which drained 950 ml of fresh blood, and then clamped. Intravenous (IV) fluids and packed red blood cells (PRBCs) were given. It was decided to perform a chest computed tomography (CT) scan with contrast (Figure 2). Following a surgical examination, the chest tube was unclamped, which immediately unveiled 700 ml of blood loss. The patient’s vital signs remained stable.
A new VBG was obtained following the infusion of 2 l of crystalloids and showed the following values: pH 7.30, PCO2 7.17 kPa, PO2 6.66 kPa, cHCO3 26.0 mmol/l, lactate 2.3 mmol/l, and HB 107 g/l. The chest tube was then unclamped, allowing for the drainage of an additional 600 ml of blood, resulting in a total drainage of 2.2 l, before the patient was transferred to our cardiothoracic intensive treatment unit for preoperative evaluation and stabilization.
The patient was transferred to the operating theatre and a left postero-lateral thoracotomy was performed in the fifth intercostal space. A small aberrant artery medial to the left subclavian artery was actively bleeding, which was clipped and stitched. The patient recovered well from surgery and the chest drain was removed following satisfactory repeat CXR.
Discussion
It is possible to define hemopneumothorax as the buildup of more than 400 ml of blood in the thoracic cage in the presence of spontaneous pneumothorax, where a tear in an adhesion would cause bleeding [3]. Whittaker successfully treated the illness for the first time by repeatedly aspirating pleural space in 1876, after Laennec initially identified it in 1828 during an autopsy [4].
Nearly 33% of individuals with the condition - who are mostly young men - present with hypovolemic shock. 87.6% of patients require surgical intervention, with blood loss ranging from 400 to 1,700 ml according to one research [3]. With good outcomes and few recurrences, surgical intervention using an open thoracotomy and video-assisted thorcoscopy was carried out. The core component of conservative management was tube thoracotomy.
A spontaneous pneumothorax that results in abrupt chest discomfort and shortness of breath is the usual course of events. However, occasionally pneumothorax can lead to the rupture of an aberrant blood vessel, resulting in hemopneumothorax. Although this was the case in our patient, proper management was delayed since his anomaly was not seen on initial chest imaging, which is rather uncommon. In hindsight, a chest CT scan performed early on would have allowed for a more accurate diagnosis, especially if the patient had been experiencing prolonged, unrelieved chest pain and shortness of breath. Given the fact that assessing pneumothorax in the early stages does not impose a diagnostic dilemma on CT chest examination, we would highly recommend it for patients with persistent acute chest pain considering diagnostic difficulties that arise with CXR interpretation.
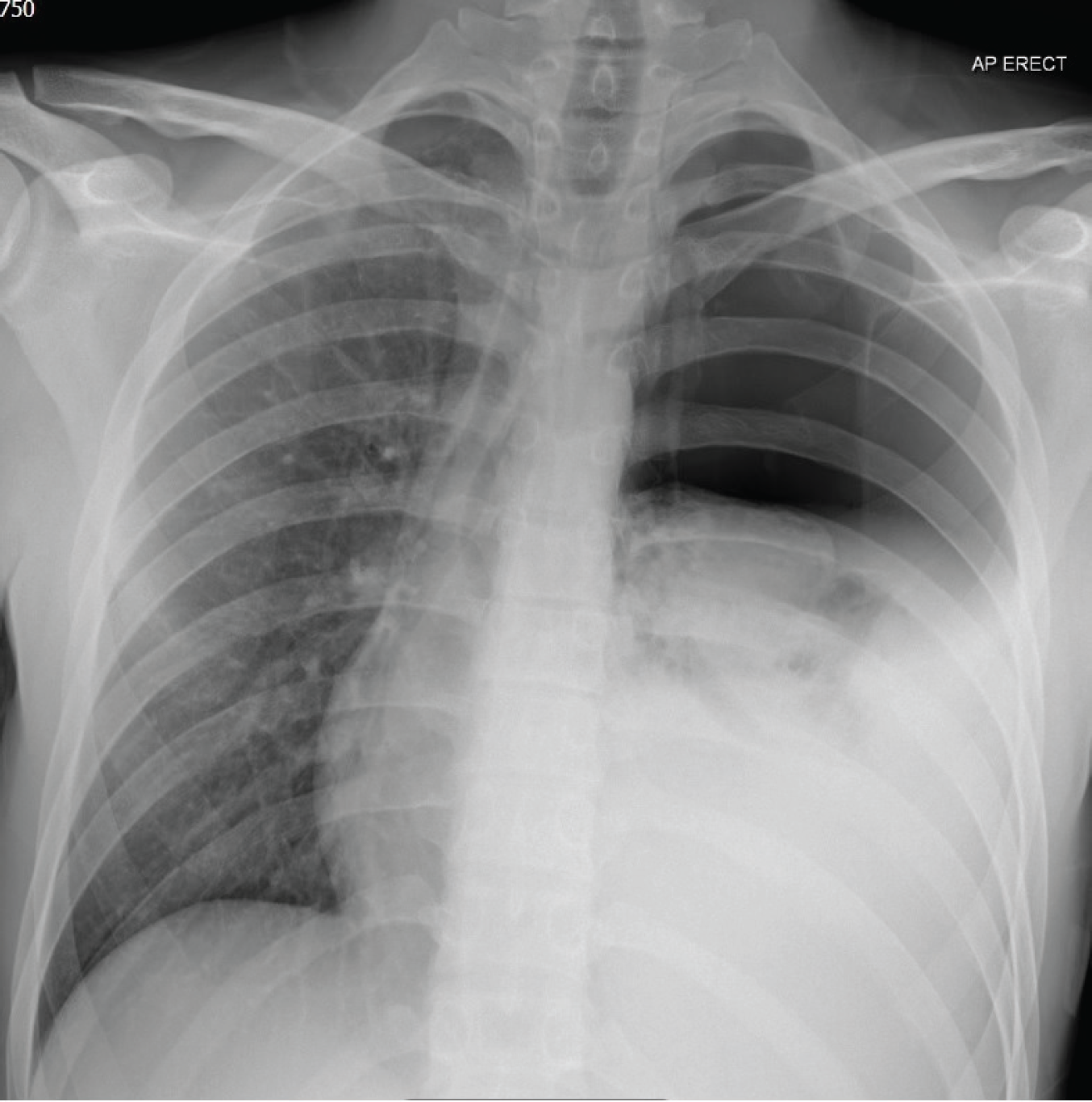
An expiratory view showing a totally collapsed left lung with a fluid level indicating hemothorax and absence of lung marking on the left upper zone indicating pneumothorax.
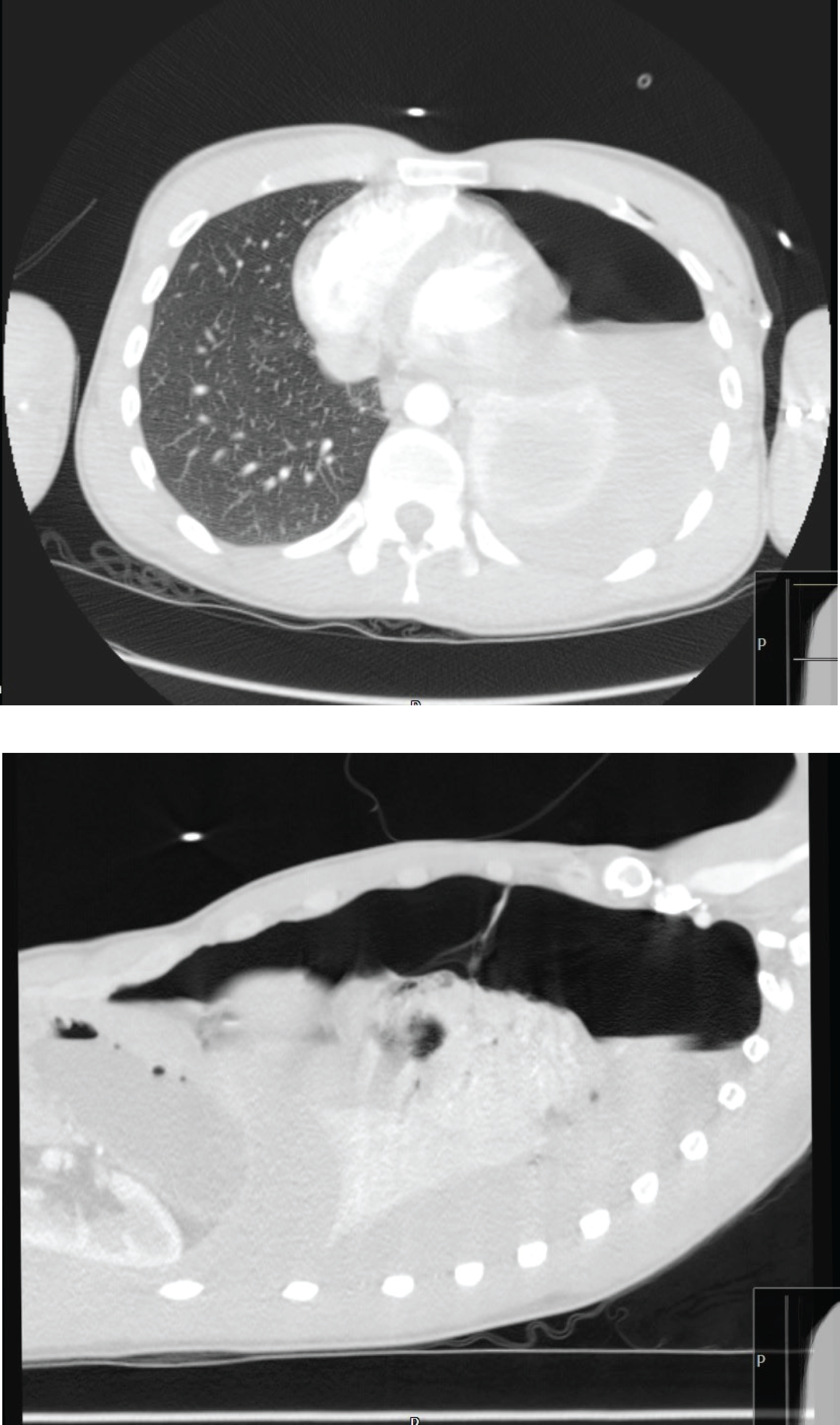
CT scan of the chest revealing the left-sided air-fluid level of the hemopneumothorax with the collapsed left lung.
When evaluating patients with spontaneous hemopneumothorax, we should include aberrant bleeding blood vessels in the differential diagnosis despite it being an uncommon etiology. A continuously bleeding small blood vessel would render the patient shocked as blood continues to accumulate in the hemi thorax with the absence of a tamponade effect from an inflated lung [5]. Therefore, we would advise aggressive resuscitation (using initial crystalloid infusion and PRBCs if needed) as well as seeking early specialist advice and referral for definitive management from the acute setting.
Conclusion
According to the case study and discussion, hemopneumothorax is a rare condition that can cause hypovolemic shock. Although a CXR is the preferred initial investigation, patients with persistent acute chest pain should be considered for further investigations and imaging including a chest CT scan to ensure an accurate diagnosis is reached [6], particularly if no clear cause for the patient symptoms is found on initial CXRs. The majority of patients continue to receive their care primarily through surgical intervention, with conservative management typically limited to tube thoracostomy. Rarely, aberrant bleeding blood vessels can cause hemopneumothorax; therefore, in the acute setting, it is important to seek early specialist guidance and referral for definitive management. Overall, timely and appropriate management can significantly improve patient outcomes in cases of hemopneumothorax.

