Background
Although a rare type of cancer, differentiated thyroid cancer is the commonest endocrine malignancy [1-3]. It usually has a rather indolent course; however, the patients can present with complications such as the distant spread of the disease [4]. Distant spread of thyroid cancer has been reported in the literature to be anywhere between 2% and 20% [5,6]. Mortality in the presence of distant metastasis can increase dramatically with a 10-year survival rate as low as 40%, as compared to 80%-95% in patients with non-metastasized disease [5,7,8]. Common sites of metastasis include the lungs and bones [9,10]. Bony metastasis often leads to increased morbidity and mortality [9,11]. We report an unusual case of a 60-year-old male who presented with backache and weakness of lower limbs due to the collapse of the 11th thoracic vertebra, which proved to be due to metastatic spread of follicular cancer of the thyroid, without any primary tumor in the thyroid.
Case Report
A 60-year-old male with back pain and inability to walk presented to a neurologist. An magnetic resonance imaging (MRI) was advised that revealed a partial collapse of the 11th thoracic vertebra with cord compression and severe right and moderate left foramen stenosis (Figure 1). The adjacent intervertebral heights were intact. The differential diagnosis included metastasis, myeloma, and lymphoma. He underwent laminectomy and internal fixation. The histopathology revealed glandular architecture lined by stratified columnar cells. There was moderate nuclear pleomorphism and hyperchromasia. Immunohistochemistry was positive for thyroglobulin (Tg), TTF1, and CK-7, thus confirming that it was metastatic spread of follicular cancer of the thyroid (Figure 2). To relieve the patient’s symptoms 20 Gy radiation was delivered in 5 fractions to 10th-12th thoracic vertebrae. An ultrasound and computed tomography (CT) of the neck were performed, which failed to reveal anything unusual in the thyroid. A CT chest was performed which revealed no pulmonary metastasis, while the bone scan revealed uptake only in the 11th thoracic vertebra (Figure 3). Subsequently, the patient underwent a total thyroidectomy. The histopathology revealed no malignancy in the thyroidectomy specimen. Tg level was in excess of 6,000 ng/ml (normal < 50 ng/ml), while the anti-Tg antibody (Anti-Tg) level was 10 IU/ml (normal 29 IU/ml). After discussion in the multidisciplinary clinic, it was decided that a dose of 7.4 GBq (200 mCi) of radioactive iodine (RAI) (I-131) be given to the patient. A post-therapy scan was performed which revealed uptake in the thyroid bed, with metastasis in the region of the lower thoracic vertebral region (Figure 4). Post-RAI Tg levels came down to 408 ng/ml. Six months later repeat blood test revealed Tg levels of 203 ng/ml (Anti-Tg = 0.02 IU/ml). A repeat of Tg levels at 1 year revealed an increase to 250 ng/ml (Anti-Tg = 2.8 IU/ml). It was decided that another dose of 7.4 MBq of RAI be given to the patient. The whole-body scan revealed uptake in the surgical site, with no other focus of abnormal tracer uptake noted (Figure 5). The post-second dose Tg decreased slightly to 236 ng/ml (Anti-Tg = 3.07 IU/ml) (Table 1).
| The patient presented to a neurologist | Back pain and inability to walk |
| MRI | Partial collapse of 11th thoracic vertebra with cord compression |
| Referred to neurosurgeon | Laminectomy plus internal fixation |
| Histopathology | Metastatic follicular ca thyroid |
| Radiotherapy | 20 Gy given to 10-12th thoracic vertebrae |
| Ultrasound and CT neck | No lesion detected in thyroid |
| Bone scan | Uptake in 11th thoracic vertebra |
| Patient underwent total thyroidectomy | No malignancy found on histopathology |
| Tg levels measured | >6,000 ng/ml |
| RAI administered | 7.4 GBq |
| Whole body scan | Uptake in thyroid bed and the lower thoracic vertebral region |
| Tg levels measured | 408 ng/ml |
| Repeat dose of I-131 after 1 year | 7.4 GBq |
| Whole body scan | Uptake in the region of the lower thoracic vertebra only |
| Tg levels measured | 236 ng/ml |
Discussion
Nearly a third of patients with cancer have a distant spread of the disease [12]. As many as 3%-4% of patients with bone metastasis have no identifiable primary tumor [13]. We report a case of metastasis of follicular cancer of the thyroid to the spine. However, when the thyroid gland was removed and histopathology performed, no primary tumor was discovered. In the review of the literature, one case series of seven cases of metastatic papillary thyroid cancer was found where no primary tumor could be found [14]. Boz et al. [15] have also reported a case of metastatic follicular cancer of the thyroid without an identifiable primary. Akdemir et al. [10] have reported a case where there were skeletal metastases in a patient without any primary being detected in the thyroid. In a 2012 study published in the Australia and New Zealand Journal of Surgery, regarding papillary thyroid cancer patients, three patients were reported to have distant metastasis without any discernible primary lesion [8]. Meanwhile, Anastasilakis et al. have reported a patient in whom they found lymph node metastasis of papillary cancer without any discernible primary [16].
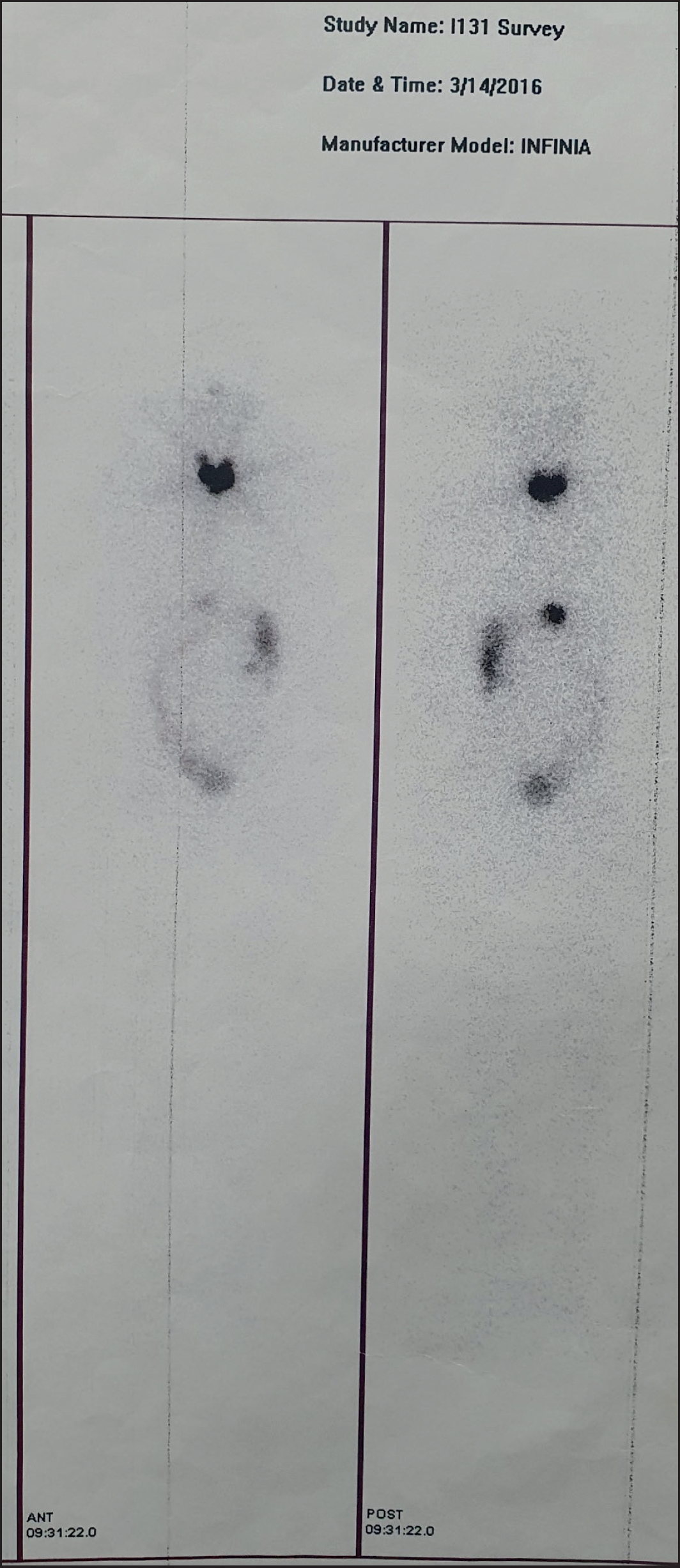
Post-ablation scan after administration of the first dose of 7.4 GBq of I-131 showing uptake in the thyroid bed (arrowhead) and the region of the lower thoracic vertebrae (outline arrow).

Post-ablation scan after the second dose of 7.4 GBq of I-131 still revealing uptake in the operation site.
It is rare to have a metastatic spread of the disease in follicular thyroid cancer without a primary. The lack of the detectable primary may be because of the spontaneous regression of the primary lesion.
Conclusion
This case report highlights that in cases of metastasis from an unknown primary, follicular thyroid cancer should be included in the differential diagnosis. Also, even if a primary is not found in the thyroid, total thyroidectomy with post-surgical administration of RAI can lead to a good prognosis as measured by the serum Tg levels.




