Background
In 1883, Marcus Gunn described a syndrome characterized by the unilateral involuntary disappearance of ptosis during the opening, protrusion, and lateral movements of the mandible in a patient with congenital ptosis [1]. This syndrome, now known as Marcus Gunn Jaw-Winking Synkinesis (MGJWS), seen in 2%-13% of the patients with congenital ptosis, is thought to be a unilateral congenital cranial disinnervation disorder [2,3].
Numerous studies on Marcus Gunn syndrome mention ptosis as a common symptom of the syndrome. Extremely rare cases of MGJWS without ptosis in resting position have also been reported in 1.2%-6.0% of the patients [4]. In our review of the existing literature, since 1883, only five reports of cases with MGJWP without ptosis were found, up until a case series of 14 patients published by Pearce et al. [4], Alam et al. [5], Kodsi [6].
Although MGJWS is thought to have an autosomal dominant inheritance pattern [7], reports of familial cases have been rare [8,9]. There are differing theories about the underlying etiopathogenesis of the syndrome. It has been considered in the spectrum of congenital cranial disinnervation disorders characterized by developmental deficiencies of the cranial nerves or nuclei that innervate the eyelid and jaw [4]. The underlying cause is believed to be a miswiring involving the third and fifth cranial nerves; the mandibular branch of the trigeminal nerve, which innervates the lateral and medial pterygoid muscles which are involved in mastication; and the oculomotor nerve branches that supply innervation to the levator palpebrae superioris muscle, resulting in a neural misdirection of trigeminal motor axons to the elevator palpebralis muscle [5,8,10,11]. Another reason suggested for the phenomenon is a neural misdirection in the brainstem [8]. Despite many theories regarding the neurological basis of this synkinesis, its etiology is not yet fully understood [5].
In our study, we report and discuss two cases with familial MGJWS diagnosed in two successive generations, without ptosis in resting position. To the best of our knowledge, this is the first study to date reporting on such a rare presentation of the syndrome.
Case Presentation
Case 1
A 41-year-old female patient with no significant medical history or head trauma presented to our clinic. Ptosis was not observed in the initial assessment. During the temporomandibular joint examination, an involuntary rapid upward motion of the left eyelid was seen in the lateral, forward, and masticatory movements of the mandible (Figure 1). The patient’s previous ocular examination records revealed anisometropia, and hyperopia (left eye: +8, right eye: +7.5) along with visual impairment in the left eye (70% loss). She had no preexisting systemic conditions. Ocular motility, palpebral structure, and movements were found to be normal. The phenomenon was confirmed to be present since birth by the patient’s parents. The patient stated that MGJWS had no negative impact on her life. When questioned about her family history, her 12-year-old daughter had the same congenital syndrome. She was born in the 40th week of the patient’s pregnancy, with normal delivery. There was no history of abnormalities before, during, or after birth.
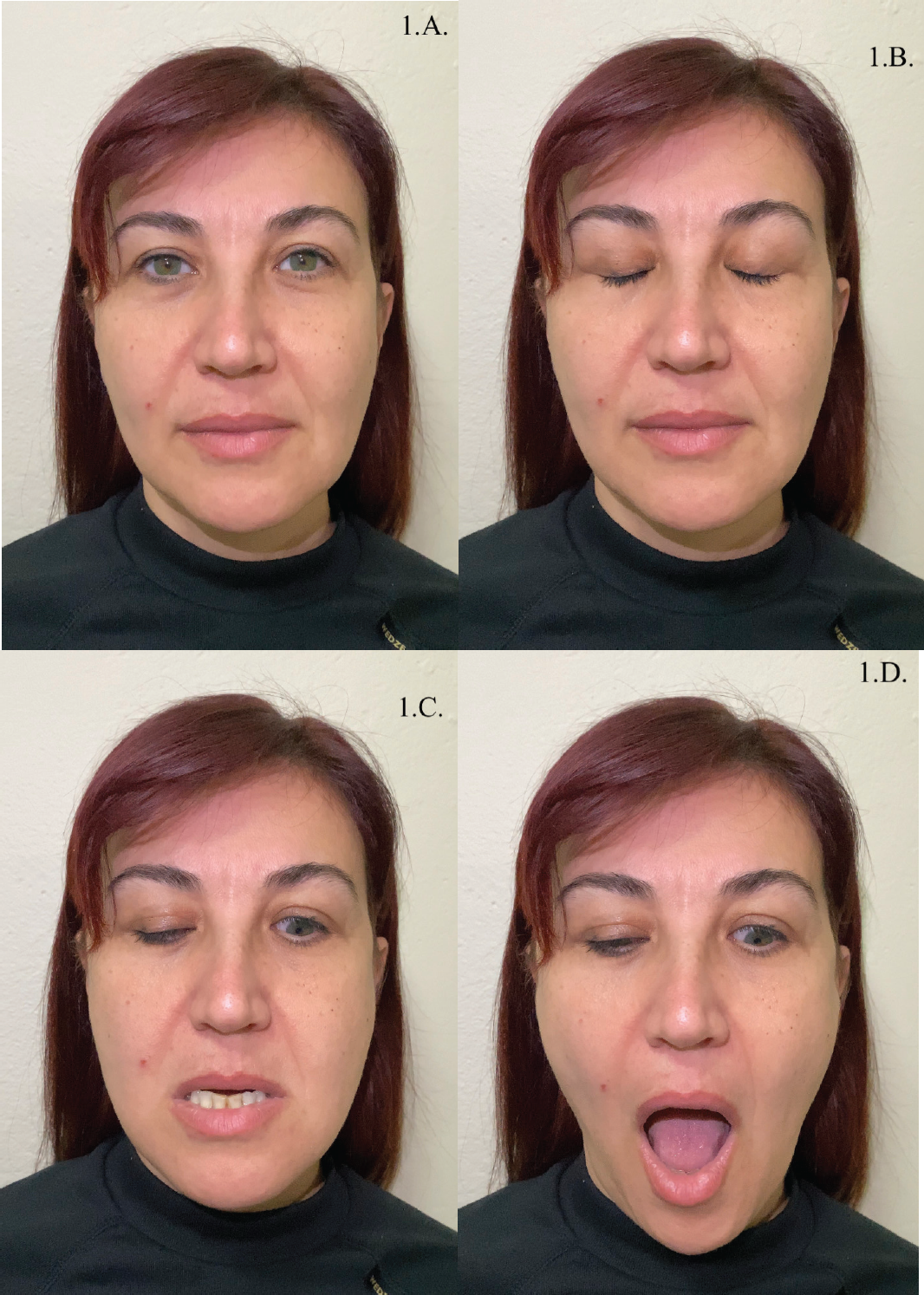
Photographs of Case 1, in resting position (A, B) and during mandibular protrusion and depression (C, D). The patient is a 41-year-old female with no significant medical history or history of head trauma. Ocular motility, palpebral structure, and movements were found to be normal. The synkinetic movement of the upper left eyelid was observed during the downward, forward, and lateral movements of the mandible. Congenital ptosis was absent. The patient stated that MGJWS had no negative impact on her life.
Case 2
The 12-year-old patient presented as a healthy girl with no preexisting conditions in her medical history. She was also diagnosed with Marcus Gunn Jaw-Winking Syndrome. Ptosis was not observed in the affected eyelid (left) and the involuntary rapid upward motion of the left eyelid was seen in the lateral, forward, and masticatory motions of the mandible (Figure 2). The patient’s previous ocular examination records revealed high hyperopia in both eyes (+5). She had received conservative treatment for amblyopia and strabismus between the ages of 1.5 and 8. She was delivered by cesarean section. Her history before, during, and after birth was normal. There were no additional abnormalities in ocular motility or eyelid movements. The phenomenon was confirmed to be present since birth by the patient’s parents. The patient stated that MGJWS had no negative impact on her life.
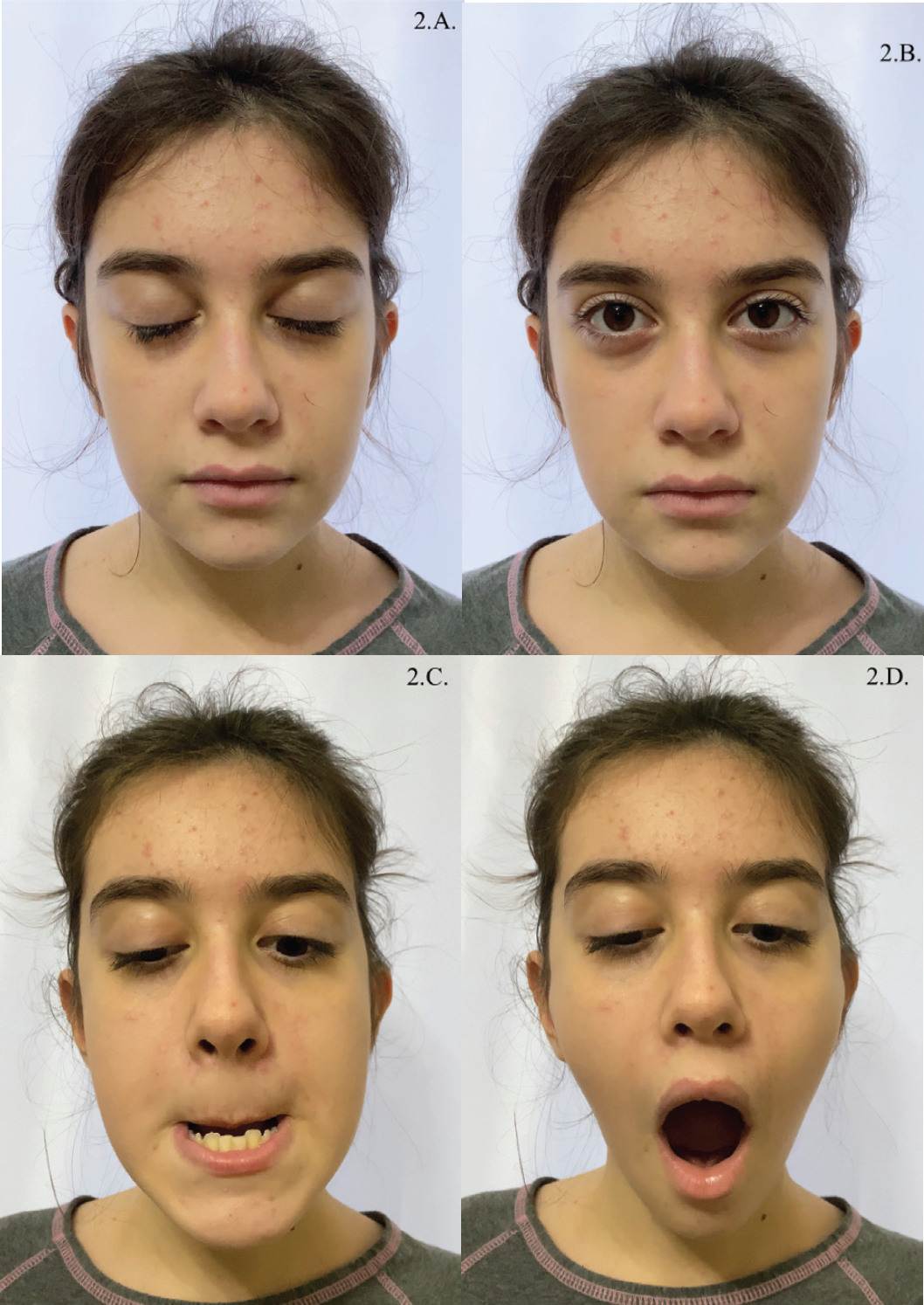
Photographs of Case 2, in resting position (A, B) and during mandibular protrusion and depression (C, D). The patient is a 12-year-old female, daughter of the patient presented as Case 1. The synkinetic movement was observed again on the left palpebra during the downward, forward, and lateral movements of the mandible, after a brief examination. Congenital ptosis was absent. There were no additional abnormalities in ocular motility or eyelid movements. The patient stated that MGJWS had no negative impact on her life.
Both patients report no change in their symptoms or quality of life at this time, which is the second year of our follow-up.
No surgical or conservative interventions were performed on the patients and they are under regular follow-up. Currently, in the second year of our follow-up, both patients report no change in their symptoms or quality of life.
Discussion
MGJWS, described by Marcus Gunn; is a rare congenital cranial disinnervation disorder in which the affected eyelid typically rises unilaterally during downward, anterior, and lateral movements of the mandible [11]. Generally reported with the presence of congenital ptosis, the MGJWS without congenital ptosis has been shown in only 6% of the cases [4,12]. Cases of MGJWP have mostly been sporadic, but with the presentation of some familial cases, an autosomal dominant inheritance pattern has been found. Familial MGJWS is extremely rare [5,8]. Although synkinesis with the absence of ptosis was observed in the left eyelid in both of the aforementioned cases and the prevalence of MGJWS in the left eye was reported in some of the current literature, a statistically significant difference between the two eyes regarding the involvement was not found [4,9,13].
The literature has reported varying degrees of ptosis-related amblyopia in 23% of the MGJWS cases [14]. MGJWS has been associated with amblyopia, anisometropia, and strabismus [2,12] The presence of amblyopia and anisometropia in our cases is in line with this information. However, studies on visual impairment and amblyopia in cases without ptosis are insufficient.
Despite the progress in neurophysiology since 1883, and studies on this rare syndrome, MGJWS is still not fully understood, although there is evidence of synkinesis of the orbicularis oculi muscle during the activation of the lateral pterygoid muscle due to peripheral anastomosis between the trigeminal and facial nerves [10,15], and the recent literature supports the hypothesis of a neural misdirection in the trigeminal motor axons resulting in the abnormal innervation of the elevator palpebralis muscle, which is normally innervated by the oculomotor nerve, due to a structural abnormality in the brainstem [7]. However, the neuroanatomical explanation of the syndrome is still unclear.
Marcus Gunn syndrome has been associated with varying amounts of ptosis [5,13]. Variations in the degree of eyelid retraction triggered by mandibular movements can also be observed [12]. MGJWP usually occurs unilaterally, but rare bilateral cases have also been reported. It is thought by some that jaw-winking ptosis has a tendency to improve with age [2]. While that is not the case with the first patient, she stated that her daughter has shown improvement, according to her observations.
No surgical or conservative interventions were performed on the patients, and they are under regular follow-up. Currently, in the second year of our follow-up, both patients report no change in their symptoms or quality of life.
To the best of our knowledge, our study is the first clinical case study of MGJWS with the absence of ptosis (MGJWS) observed in two successive generations.
Conclusion
The absence of the ptosis symptom, especially if other eye abnormalities and visual impairments are not present or severe, might make the diagnosis and sequential follow-up of MGJWS a challenge. The synkinetic movement being observed during masticatory movements presents a diagnostic opportunity for the dental clinician and surgeon since it will be observed during a routine temporomandibular joint examination. Thus, the authors think that it is important for dental clinicians and surgeons to be informed about the syndrome, and the need to refer patients to an ophthalmologist.

