Background
Proliferating trichilemmal tumors (PTTs) are rare benign neoplasms that arise from the outer sheath of a hair follicle [1]. Only a few hundred cases have been described in the literature [2]. Accordingly, Ye et al. [3] classified PTTs into three groups, namely, benign, low-grade malignant, and high-grade malignant lesions, based on clinic-pathological characteristics. Group I PTTs are benign lesions. Recurrence is not observed in these lesions. They show histologically regular contours with surrounding tissues and mild nuclear atypia but do not involve increased mitotic activity, necrosis, and lymphovascular invasion. Group II PTTs are low-grade malignant tumors. Local recurrence may be observed in these lesions. These tumors have histologically irregular and local invasive contours, and they elongate to the deep dermis and subcutaneous tissue. Group III PTTs are high-grade malignant tumors reported to exhibit a high recurrence rate, lymph nodes, and a tendency to develop distant metastasis. Remarkable nuclear pleomorphism, atypical mitosis, necrosis, and lymphovascular invasion may be observed in these tumors.
Case Report
A 25-year-old female patient was presented to us with a history of recurring soft tissue scalp lesions. The lesion recurred three times within 1 year. There was no history of trauma. The patient got an excision of a 2 × 2 cm scalp lesion twice and histopathology of the specimen was not done. On the third recurrence, lesion was excised and diagnosed as a malignant proliferating trichilemmal tumor (MPTT) histopathologically. She had a scalp lesion of T size; 1.9 × 1.6 × 1.5 cm. The tumor was 0.7 cm from the first polar resection margin, 0.6 cm from the second polar resection margin, 0.1 cm from deep margins, and less than 0.1 cm from the peripheral resection margins. It was Grade III, lymphovascular invasion and perineural invasion was not identified. Nodal and distant metastatic status was unknown. She was referred for redo surgery to achieve margins.
When she came back after surgery, her histopathology report showed residual MPTT of T size: 0.8 × 0.6 × 0.5 cm, and mitosis was approximately 15/10 under high power field. All margins were free of tumor involvement on the frozen section, but the tumor was 0.1 cm away from the closest deep margin. Additional pathological findings included foci of chronically inflamed granulation tissue and foreign body-type multinucleated giant cell reaction was seen. These findings were consistent with previous surgical sites.
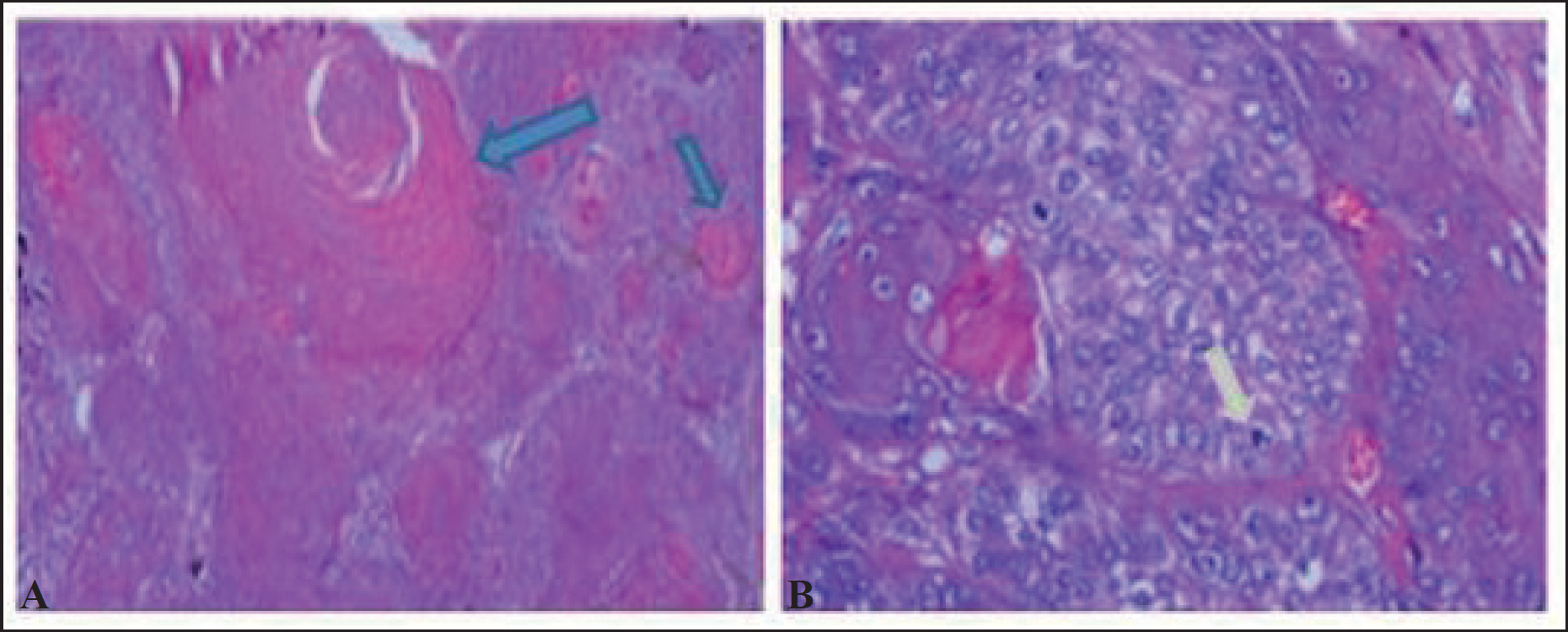
Histopathology of MPTT of scalp showing. (a) Trichilemmal keratinization represented by blue arrow (b) Tumor cell with wide cytoplasm represented by the light grey arrow.
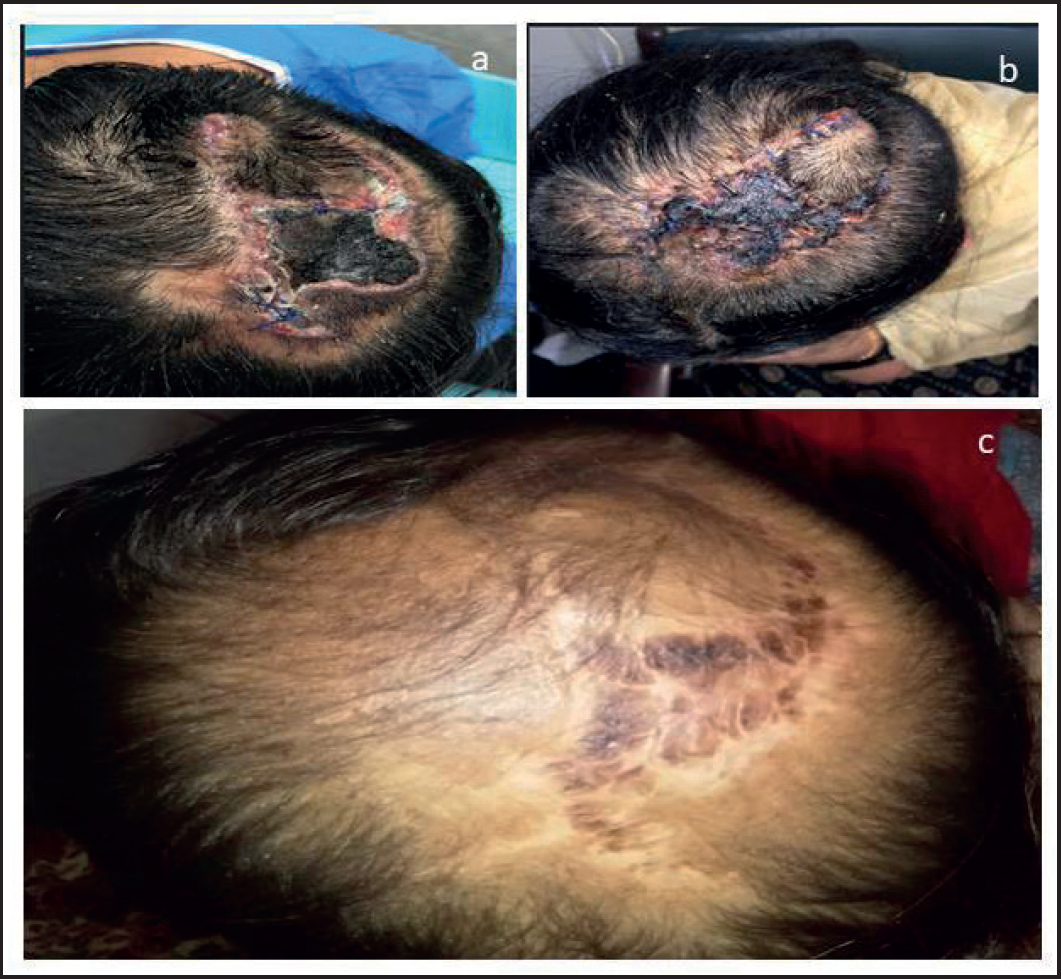
(a) After surgery. (b) 2 weeks after radiation therapy. (c) Patient on 9 months follow up with healed scalp and no recurrence.
Considering the young age of the patient and keeping in view the history of multiple recurrences and deep margin of 0.1 cm, the patient was planned scalp radiotherapy (RT) 50 gy/25 fx with 9 Mev electron using 0.5 cm bolus. The patient completed RT, and now she is on routine follow-up (Figure 2).
Discussion
MPTT is a rare malignancy, usually observed in the sixth decade of life [4]. The tumor may be misdiagnosed as squamous cell carcinoma (SCC) because cutaneous SCC is commonly observed in the scalp [5]. Moreover, the histological features of MPTT and SCC are more or less similar. It is commonly characterized by abnormal mitosis and infiltrating margins [5].
Similarly, benign and malignant PTT may also be confused and is important to differentiate. Three major groups have been identified in PTT namely benign, low-grade malignant, and high-grade malignant tumors [6]. Benign lesions usually do not have a recurrence while low- and high-grade lesions have low and high recurrence rates respectively. MPTT is generally transformed from a benign PTT but may appear as a malignant tumor de novo in a few cases [3].
According to the literature, >80% of cases of MPTT are observed in elderly women [7]. Our patient is a young female only 25 years of age. She is having high-grade MPTT and neoplasm has recurred thrice and the tumor has a high mitotic activity (Figure 1). All these features reflect high-grade malignant disease.
A mainstay of treatment is surgery with wide surgical margins as local recurrence is most common in MPTT [8]. Patients are usually closely monitored after surgery for any possible relapse of disease. Adjuvant RT was used in this case to prevent recurrence. Our patient is disease free on routine follow-up for 1 year after adjuvant RT.
What is new?
PTTs are rare. Only a few hundred cases have been described in the literature. The mainstay of treatment is surgery with wide surgical margins as local recurrence is most common in MPTT. In our study, considering the young age of the patient and keeping in view the multiple recurrences and deep margin of 0.1 cm, the patient was planned scalp RT 50 gy/25 fx with 9 Mev electron using 0.5 cm bolus. Our patient is disease free on routine follow-up for 1 year after adjuvant RT.

