Background
Mycosis fungoides (MF) represents the most common cutaneous T-cell lymphoma and approximately 4% of non-Hodgkin lymphomas. Clinical presentation includes erythematous and often pruritic skin lesions that progress sequentially to patches, plaques, and tumors, warranting local treatment.
Radiation therapy is an effective modality for local palliation with prescription doses between 8 and 20 Gy at 3-5 Gy per fraction, achieving adequate local control and symptom relief [1,2].
Electron-beam therapy is the most used type of radiation to treat superficial targets. However, large and irregular surfaces limit the use of bolus material and the possibility of achieving a uniform dose with electrons. In these clinical scenarios, photon-beam therapy with tissue compensation has been reported as an alternative method [3-7].
In this paper, we describe the use of a water tank in a patient with extensive MF plaques on the surfaces of the feet including digits.
Case Presentation
The patient is a 39-year-old male with a history of MF disease for 17 years presenting with generalized skin involvement and nodal spread on both sides of the diaphragm.
After skin-directed therapy with narrow-band ultraviolet B, immunosuppressive and immunomodulating drugs, and systemic chemotherapy, the disease was stable.
He was referred to the radiation oncology department by his hematologist for evaluation of extensive and infiltrative plaques in the feet. The patient reported debilitating pruritus with repercussion in daily activities such as walking and driving. The most symptomatic lesions affected the plantar, interdigital, lateral, and posterior surfaces (Figure 1).
The location and irregularity of lesions represented a dosimetric challenge and treatment using a water tank and two parallel opposed lateral photon-beam fields was planned to provide good coverage of target volumes.
The protocol included a previously tested and validated paraffin-built tank, and the patient was simulated with a Siemens Somatom X computed tomography scanner using a vacuum mattress and a triangular foam block (Figure 2). The foot was then immersed in the water-filled tank and the images were acquired, repeating the process for the other foot.
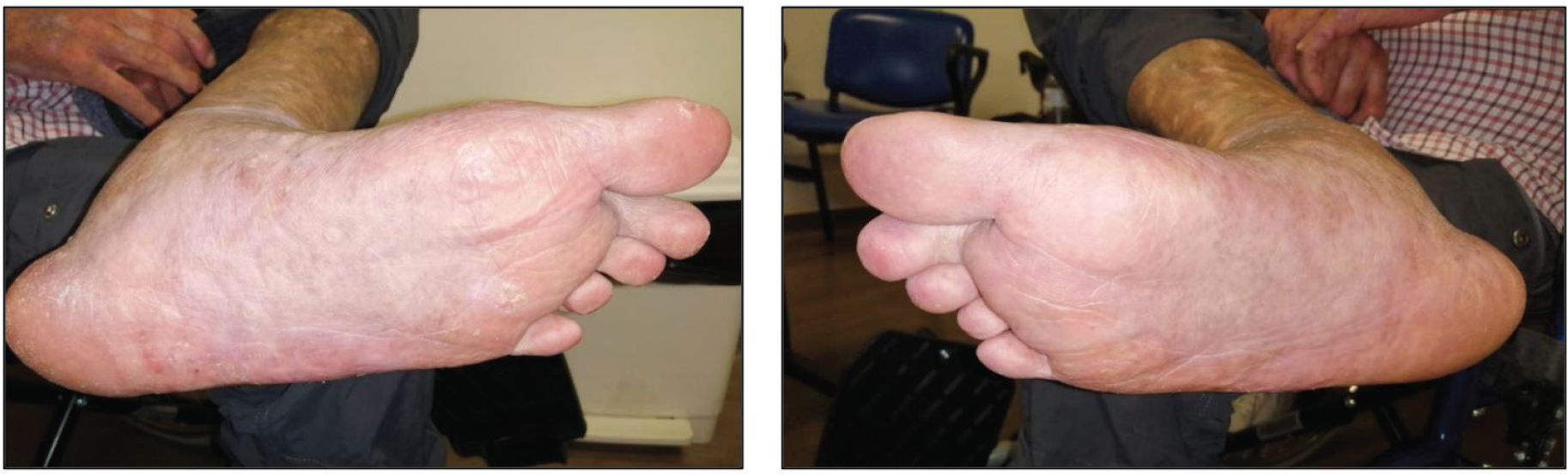
Clinical photograph records of ventral surfaces of both feet showing response to radiotherapy at 24 weeks after treatment completion.
A palliative dose of 8 Gy in two fractions was prescribed and feet were treated one at a time. For each treatment, kV verification images were taken to match the treatment fields.
Follow-up consultations occurred at 2, 4, and 24 weeks after treatment (Figure 3). After 1 month of treatment, there was a parcial response with minimal toxicity, achieving a complete response in most lesions after 6 months and no local discomfort when walking or driving.
Discussion
Electron-beam therapy has limitations in lesions involving extremities. There are few published case reports using photons and tissue compensating methods to irradiate skin diseases of the extremities, ranging from water to rice boluses. This technique has been applied in the presence of distinct histologies such as Kaposi’s sarcoma, cutaneous lymphomas, carcinoma in situ, and Bowen’s disease, also allowing definitive radiation therapy treatments when indicated.
In cases where the volume intended to treat requires a high dose of electrons to an irregular surface, dose coverage is suboptimal with more hotspots and no benefit in deep tissue sparing.
Except for the need for validation, clinical setup often requires little to no additional equipment. As such, the method covered in this case is readily available with low resources and should be considered within a multidisciplinary approach.
A tissue-equivalent material allows a homogeneous dose distribution to be achievable with photons. Among the alternatives previously reported in the literature, using a water bolus that has the necessary adaptability and availability provides better conformity around the target surfaces and assures adequate superficial dose coverage.
Conclusion
Photon-beam therapy for irregular surfaces such as extremities is a valid alternative to conventional electron-beam radiation by attaining uniform coverage while minimizing hotspots.
Treatment utilizing a water tank is well-tolerated and has good clinical outcomes even in the presence of extensive skin lesions.
What is new?
There are few published case reports using photons and tissue compensating methods to irradiate skin diseases of the extremities, ranging from water to rice boluses. This technique has been applied in the presence of distinct histologies such as Kaposi’s sarcoma, cutaneous lymphomas, carcinoma in situ, and Bowen’s disease, also allowing definitive radiation therapy treatments when indicated.



