Background
Some recent systematic reviews demonstrated that the general population’s overall prevalence of congenital anomalies of the female urogenital system occurs in approximately 4%-7% of women. The Müllerian duct anomalies (MDA) result from altered fusion or reabsorption of the Müllerian ducts. Environmental and genetic factors can be possible causes [1]. Patients with a normally functioning uterus and obstructive anomalies of the lower genital tract may present with cyclic pelvic pain resulting from the accumulation of menstrual blood in the uterus o vaginal cavity. The obstruction can occur at several levels, giving presentations that develop a hematocolpos or hematometra. Patients may have difficulties in their sexual life and reproductive problems [2].
Up to 50% of patients affected by Mullerian duct abnormalities reported an association with renal anomalies. There is a high incidence of the spine (29%) and cardiac anomalies (14.5%) [3].
Case Presentation
A 15-year-old Caucasian girl with no history of any particular disease presented to her local emergency department with suspected primary amenorrhea associated with cyclical pelvic pain for 3 months. The beginning of pubertal development occurred at 9 years of age and early thelarche at 11 years of age. The patient had a normal development for both height and weight, with well-developed secondary sexual characters. The abdominal examination was normal. Gynecological examination showed a normal appearance of the external genitalia and the presence of a vaginal cup instead of the introitus. Blood tests including a hormone profile laboratory test were normal.
Pelvic ultrasound (US) imaging demonstrated normal-sized kidneys and ovaries. The presence of two separate divergent uterine horns with a large fundal cleft raised suspicion of uterus didelphys. Furthermore, the US image showed a distended, fluid-filled structure ending in a blind pouch at the lower margin of the vagina (Figure 1).
A pelvic magnetic resonance imaging (MRI) examination was conducted to integrate the US findings. The MRI study confirmed the presence of uterus didelphys showing two diverging uterine bodies with two separate endometrial cavities, two separate cervixes, and a short longitudinal septum in the distal vagina. MRI scans revealed a dilatation of the vagina and endometrial cavity with blood products (hematocolpos and hematometra). The axial T2W scan shows the lower margin of the vagina replaced by low signal intensity fibrous or fat tissue (Figures. 2 and 3).
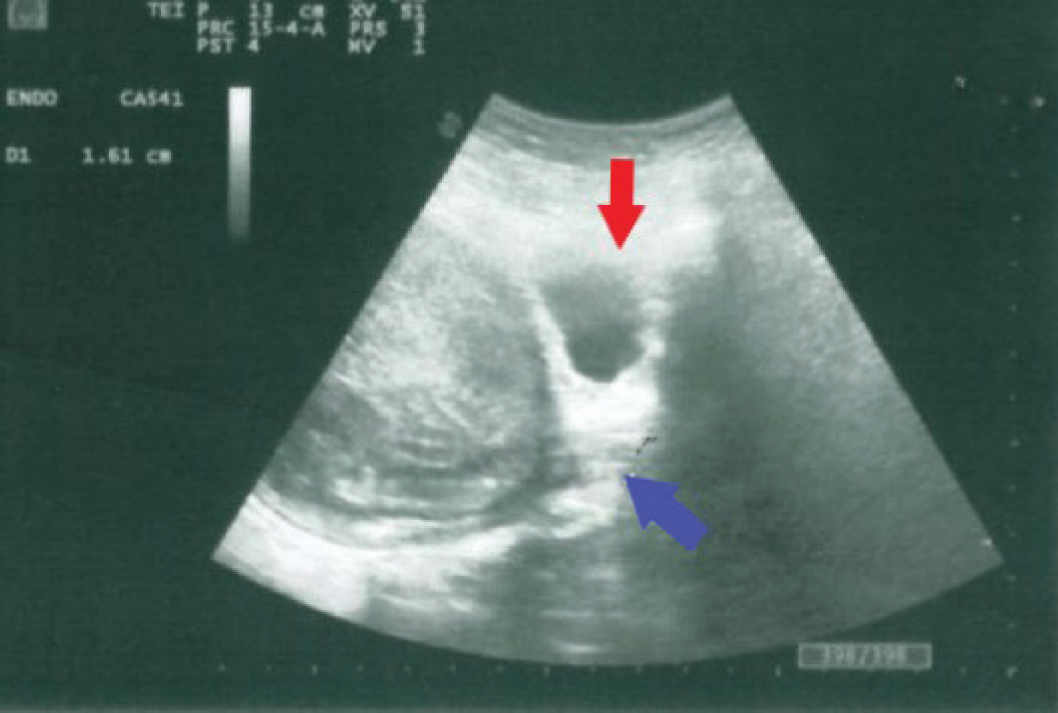
Transabdominal ultrasonography. Longitudinal scan shows a distended vagina containing echogenic fluid; the lower vagina is ending in a blind pouch (blue arrow). The urine bladder is indicated with a red arrow.
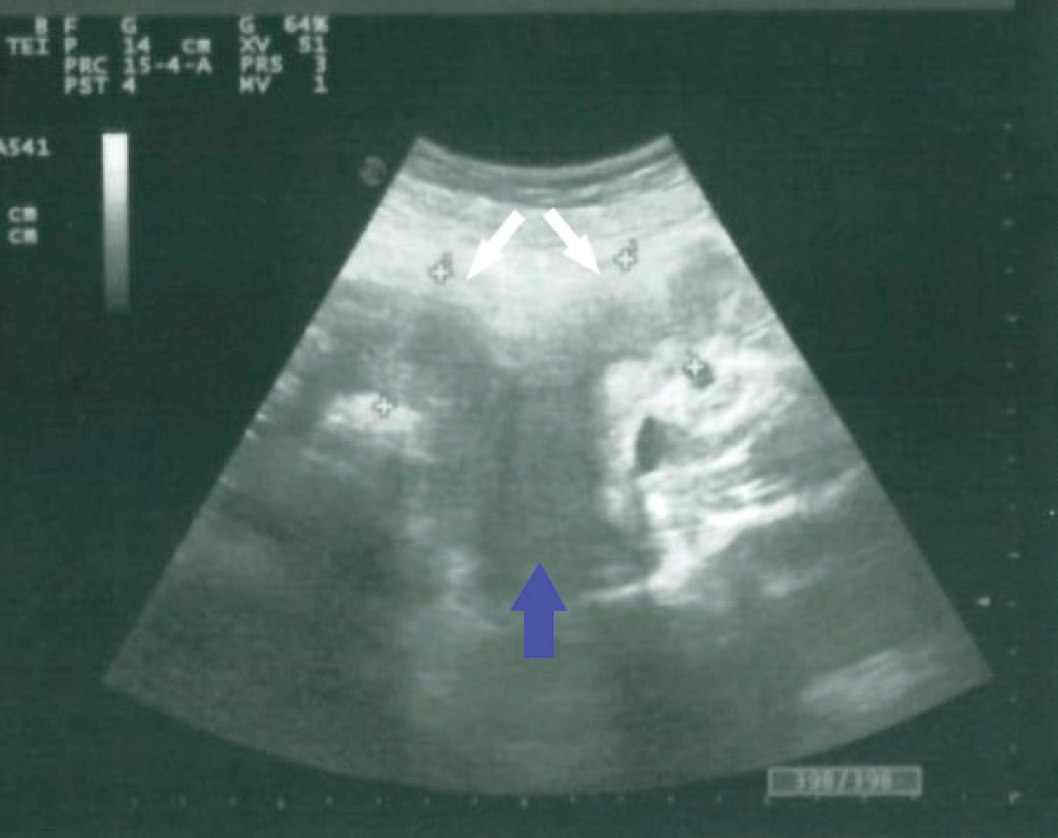
Transabdominal ultrasonography. Longitudinal scan shows two separate uterine cavities with hematometra indicated with white arrows and the upper vagina distended by hematocolpos (blue arrow).
These findings were compatible with vaginal atresia in a patient with uterus didelphys complicated with hematometracolpos. At our institution, a multidisciplinary team of gynecologists, radiologists, and surgeons discussed this clinical case. A vaginoplasty was recommended.
Discussion
Vaginal atresia is a rare congenital female tract anomaly that affects one out of 4,000 women, it appears as complete or partial vaginal agenesis. The partial atresia is further classified as distal and proximal. [4].
During embryogenesis, a midline fusion of the Mullerian ducts and later septum reabsorption processes produce the proximal two-thirds of the vagina, cervix, and uterus. The urogenital sinus develops into the caudal portion of the Müllerian ducts, forming the vaginal plate. Reabsorption of that central part forms the lower vagina and hymen [3,5]. Anomalies of development can occur at any point of the fusion or canalization process.
There are many classifications of uterine anomalies. One of the most successfully adopted is the American Fertility Society classification system which divides uterine malformations into seven classes. This system ignores vaginal anomalies and some combined anomalies. The European Society of Human Reproduction and Embryology (ESHRE), in collaboration with the European Society for Gynecological Endoscopy (ESGE), has introduced a new classification based on Müllerian development processes, which cover additionally uterine, cervical, and vaginal anomalies [1].
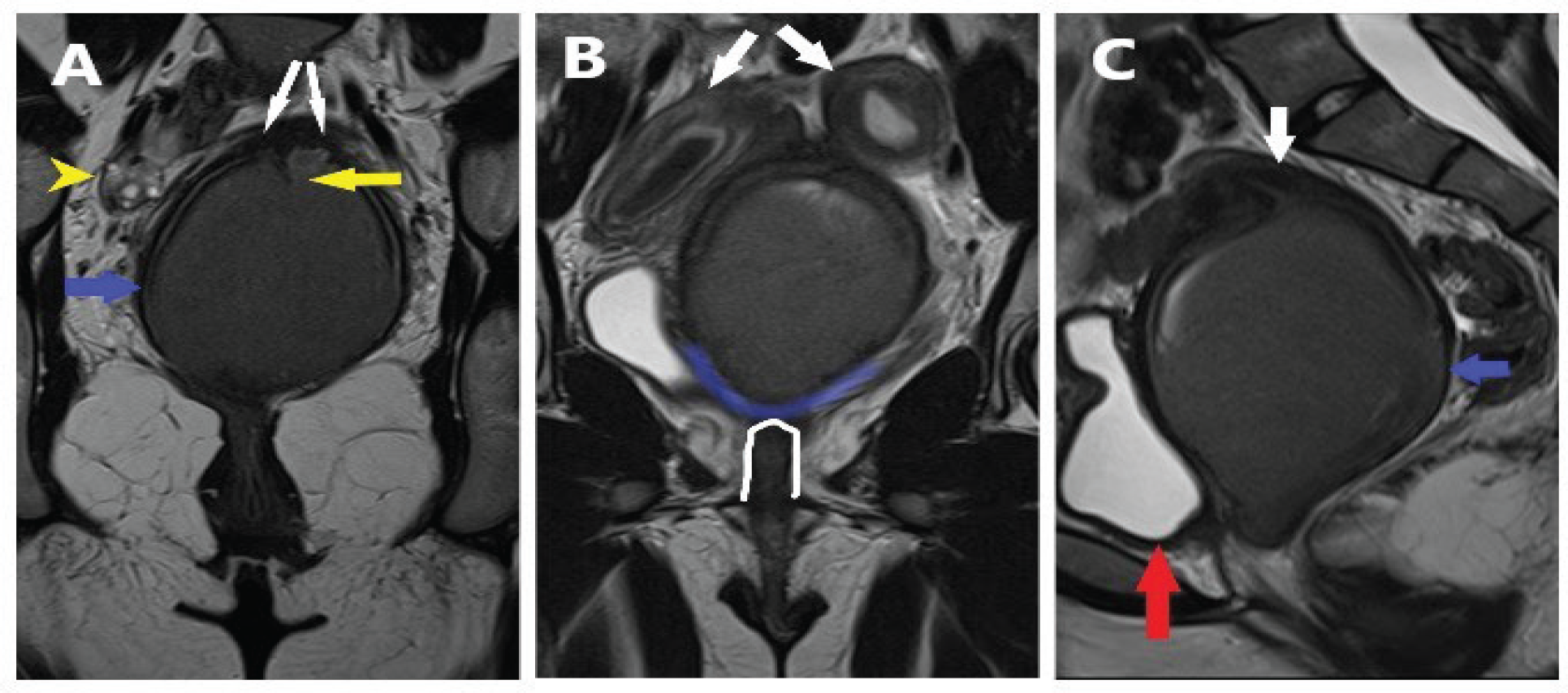
MRI T2-weighted coronal (a,b) and sagittal (c) images: (a) the upper vagina distended by hematocolpos (blue arrow), a short longitudinal vagina septum (yellow arrow) and the terminal part of two distinct cervixes (white arrows) are noted. The right ovary with small follicles (yellow arrowhead); (b) this scan demonstrates two separate uterine cavities with hematometra indicated with white arrows, the rectum is occasionally noted (white outline); (c) sagittal T2-weighted image shows distended blind-ending upper vagina (blue arrow) behind the urinary bladder (red arrow). In communication with the upper vagina, the right cervix is noted (white arrow).

(a) Axial T2-weighted image through the pelvis shows the upper vagina distended by hematocolpos (blue arrow) situated between the urinary bladder (red arrow) and rectum (white arrow); (b) axial T1-weighted image through the pelvis on the perineal level demonstrates the urethra (yellow arrow) and anal canal (white arrow). The vaginal introitus is absent.
In the case of vaginal atresia, the uterus and cervix may be normal or may demonstrate fusion or reabsorption defects. If vaginal agenesis is associated with the presence of a functioning uterus, these patients present with cyclical progressively worsening abdominal pain resulting from the accumulation of menstrual blood in the uterus o vaginal cavity (hematometra or hematocolpos). Endometriosis frequently coexists. Patients may have difficulties in their sexual life and reproductive problems.
An abdominal mass can be palpated. Upon rectal exam, a bulge is sometimes defined at a variable distance from the perineum. On vaginal exam, the hymen appears normal and the vaginal introitus is absent [2].
In young patients, US is the preferred method for evaluating acute pain because it is readily available, quick, does not require ionizing radiation, and allows for evaluation of the renal system. Pelvic US may illustrate a haematocolpos e/or hematometra but has some limitations as a smaller field of view than MRI, it can fail to encompass the external contour and uterine cavity in a single volume and it is difficult to assess the level of obstruction and the relationships with the rectum and bladder [6].
Currently, MRI remains the imaging standard of reference for MDA because it is a non-invasive ionizing radiation-free exam that allows an optimal field of view and multiplanar reformation. Evaluating the uterus in its proper coronal plane is critical for uterine malformation classification. Whereas vaginal aplasia is best evidenced in transverse images. T1w Fat Sat sequences permit more accurate detection of blood products to determine the presence of hematometra, hematocolpos, or endometriosis. Dixon technique is also widely used. Routinely performance of T2w ultrafast spin-eco technique Half-Fourier-Acquired Single-shot Turbo spin Echo coronal and sagittal planes is required for the detection of kidney and ectopic ovaries [7].
During differential diagnosis procedures, other congenital genital tract anomalies can be considered. An imperforate hymen is the most common obstructive anomaly, occurring in 1/2,000 girls. It can present with a very similar appearance to vaginal atresia symptoms of cyclical pain and amenorrhea. The diagnosis is based on the presence of a bulging bluish hymenal membrane and normal uterus, vagina, and ovaries. This may be confirmed with a pelvic US and MRI that shows collections in the distended vaginal cavity and thicker inferiorly bulged imperforate hymen. A transverse vaginal septum is a much rarer condition. The obstruction can occur most commonly in the upper third of the vagina. The vaginal septum may be thin or thick, partial, or complete. The clinical presentation will depend on the partial or complete septum. In the case of the complete septum, cyclic abdominopelvic pain with enlarging pelvic mass is present. US and MRI exams demonstrate the distention of the vagina superior to the septum with hematometrocolpos. Axial T2W image centered at the vagina shows the separation of the right and left vaginal fornices by a fibrous band [2,3].
Prompt management of obstructed outflow genital tract anomalies is essential due to severe cyclical pelvic pain, the risk of pelvic inflammatory disease, hematosalpinx, and endometriosis. A multidisciplinary team of pediatric surgeons, physicians, and pediatric gynecologists manages the most complex cases. Hormonal suppression can be provided while obtaining an accurate diagnosis whilst planning surgery. Surgery of vaginal outlet obstruction depends on the local anatomy. Simple incision, excision, or vaginoplasty can be performed [8].
Conclusion
The rarity and its variable presentation of congenital genital tract anomalies can lead to delayed diagnosis and erroneous management. A careful and detailed assessment is needed to reach the appropriate diagnosis and ensure treatment maximizes the future potential for sexual function and reproduction. MRI provides precise anatomic details of the internal uterine cavity, the external contour, and the cervicovaginal tract [2,3,7].

