Background
The prevalence of blood culture-negative infective endocarditis (BCNIE) is up to 31% in all cases of infective endocarditis (IE) [1]. It often poses a challenge to a physician in terms of diagnosis and therapeutic antibiotic choice. It carries a high risk of morbidity and mortality due to multiorgan failure secondary to severe sepsis, decompensated cardiac failure, and thromboembolic phenomena in the brain and other parts of the body [2]. The thromboembolic mechanism is from the dislodged portions of the platelet-fibrin matrix of vegetation which travel to the distal arteries, lodging in a vascular bed, and propagate to occlude the affected vessels [3]. The importance of early recognition of thromboembolic phenomenon is crucial and a multidisciplinary approach may be required in handling the complication.
Case Presentation
A previously healthy 33-year-old Asian gentleman who is a nonsmoker, nonintravenous drug user came with chronic fever and lassitude. He had several visits to the local clinic and was given a short course of oral cefuroxime. On presentation, he was alert but hemodynamically unstable, had a high-grade fever and cardiac assessment revealed a pansystolic murmur on the mitral area which radiates to the axilla suggestive of mitral regurgitation. He had immunological manifestation in which there was a presence of Roth spots on fundoscopy and microscopic hematuria during urine examination. He had a poor denture which needed dentist attention for the cleaning procedure.
The inflammatory markers (white blood cell count and C-reactive protein) were elevated, 28.5 × 103/ul and 109 mg/l, respectively. However, no causative microorganism growth despite three sets of blood cultures. The other relevant atypical infection workups for culture-negative IE based on our locality such as Brucella species serology and serum mycoplasma serology were tested negative. The autoimmune and thrombophilia screening were tested negative. He also tested negative for the retroviral disease, hepatitis B and C infection.
Trans-thoracic echocardiography revealed a large vegetation size of 2.81 cm2, the presence of a flip-flop appearance of the anterior leaflet of the mitral valve, and severe mitral regurgitation (Figure 1a and b). The patient was diagnosed with BCNIE and treated with intravenous (IV) ceftriaxone and gentamicin after a consensus between a cardiologist and an infectious disease specialist.
On day 10 of antibiotics, he experienced severe resting pain and weakness of the bilateral lower limb. Physical examination noted coldness from knee downward, bluish discoloration of the toes, prolonged capillary refilling test, nonpalpable pulses and absence of Doppler signal from femoral downward, paresthesia of the leg and foot and reduced muscle power to 4/5 distally.
An urgent computed tomography angiography (CTA) of bilateral lower limbs was performed and showed multilevel bilateral lower limb thrombosis involving bilateral common iliac arteries down to the dorsalis pedis artery and posterior tibialis artery (Figure 2a and b).
Immediately after the diagnosis of bilateral acute lower limb ischemia, he underwent emergency bilateral open femoral embolectomy and right profundaplasty. The indication of the operation was to prevent the threatened limb from becoming gangrenous and nonsalvageable.
It was intra-operatively noted the vessel walls were not calcified and the clot evacuated from both common femoral arteries down to the superficial femoral artery, small caliber right superficial femoral artery, and proximal right profunda artery. Fogarty catheter sizes 3Fr, 4Fr, and 5Fr were used to evacuate blood clots proximally and distally and noted good inflow postprocedure. Right profundaplasty with a vascular patch and left common femoral arteriotomy patch repair were performed to ensure good distal blood flow and prevent vessel stenosis (Figure 3a and b). The clot was sent for culture and sensitivity, but no microorganism growth was seen. He made a good recovery postoperatively with good distal circulation characterized by palpable distal pulses and biphasic Doppler signal. In less than a week, he was able to ambulate without support, but the left foot drop persisted. The surgical wound healed in 2 weeks postoperatively. The indication of mitral valve replacement was clearly mentioned to the patient, but he insisted on getting a second opinion at the other center. He was discharged after completing 6-week course of IV antibiotics.
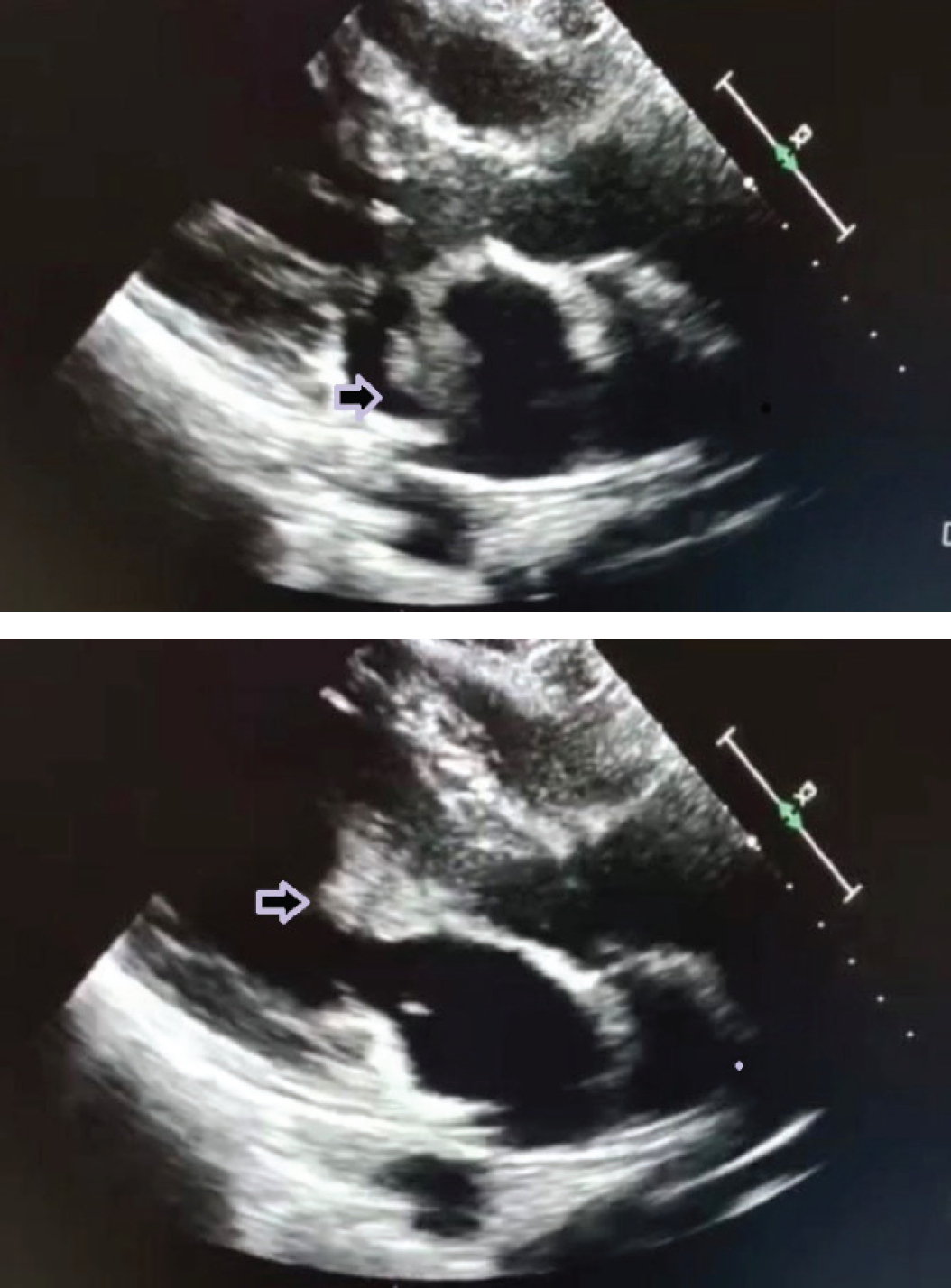
(a and b) 2D trans-thoracic echocardiogram parasternal long-axis view shows the presence of a hyperechoic lesion at the anterior leaflet of the mitral valve (arrow). This lesion is suggestive of vegetation at the mitral valve.

Both the above diagrams show the reconstructed image of the patient’s CTA bilateral lower limbs done before the operation. (a) Multiple sites of thrombosis were noted; left common iliac including the external and internal iliac till proximal superficial femoral artery, distal tibial till dorsalis pedis artery. (b) Right common iliac artery till origin of the external and internal iliac artery, short segment branch of the internal iliac artery, proximal superficial femoral artery, mid to distal peroneal artery, distal anterior tibial artery till dorsalis pedis, and distal posterior tibial artery.
Discussion
There are several postulations on the possible cause of BCNIE. This includes prior exposure to antibiotics, fastidious fungi, and bacteria or difficult-to-cultivate organisms [1,4,5]. Before antibiotic administration on this patient is the possible cause of negative organism growth. The empirical antibiotic used should target the most likely organism based on the possible source of infection and locality. In this case, a poor denture is the most likely source of infection. The likelihood of infection from Streptococcus viridans is strongly associated with this condition. Thus, IV ceftriaxone and IV gentamicin were given targeting to treat this bacterium. The advantage of these antibiotics’ regimes is their wide spectrum of coverage including Streptococcus, Staphylococcus, Enterococcus, and Haemophilus, Aggregatibacter, Cardiobacterium, Eikenella, Kingella group [1,6].
The incidence of the thromboembolic phenomenon is around 20%-50% of all IE cases [7]. The previous study reported septic embolization commonly affects the brain, 26.3% while to the extremities was rare, 2.2%-5% [1,8]. The presentation of embolization varies from transient ischemia, which is successfully treated with antibiotics and anticoagulant, to or more severe form of acute limb ischemia which requires intervention such as embolectomy and limb amputation [9]. The subtle symptoms of leg pain suggest acute limb ischemia may be missed if not suspected early especially in culture-negative IE in view of the rarity of the systemic emboli complication [5].
Despite patients on appropriate antibiotic therapy, the risk of distal embolization is unpreventable. Distal embolization to the bilateral lower limb still occurred possibly due to a bigger size of vegetation, 2.81 cm2 located at the anterior leaflet of the mitral valve, and the event of embolization occurred within the first 2 weeks of antimicrobial therapy. This is consistent with the European Society of Cardiology guideline which states that high predictive risk of the embolic phenomenon if the vegetation size is >10 mm, a higher embolic event during the first 2 weeks of treatment, left-sided IE and involving the anterior leaflet of mitral valve [1]. Thus, surgical debridement and valve replacement must be offered to those who have a high risk of systemic embolization [10].
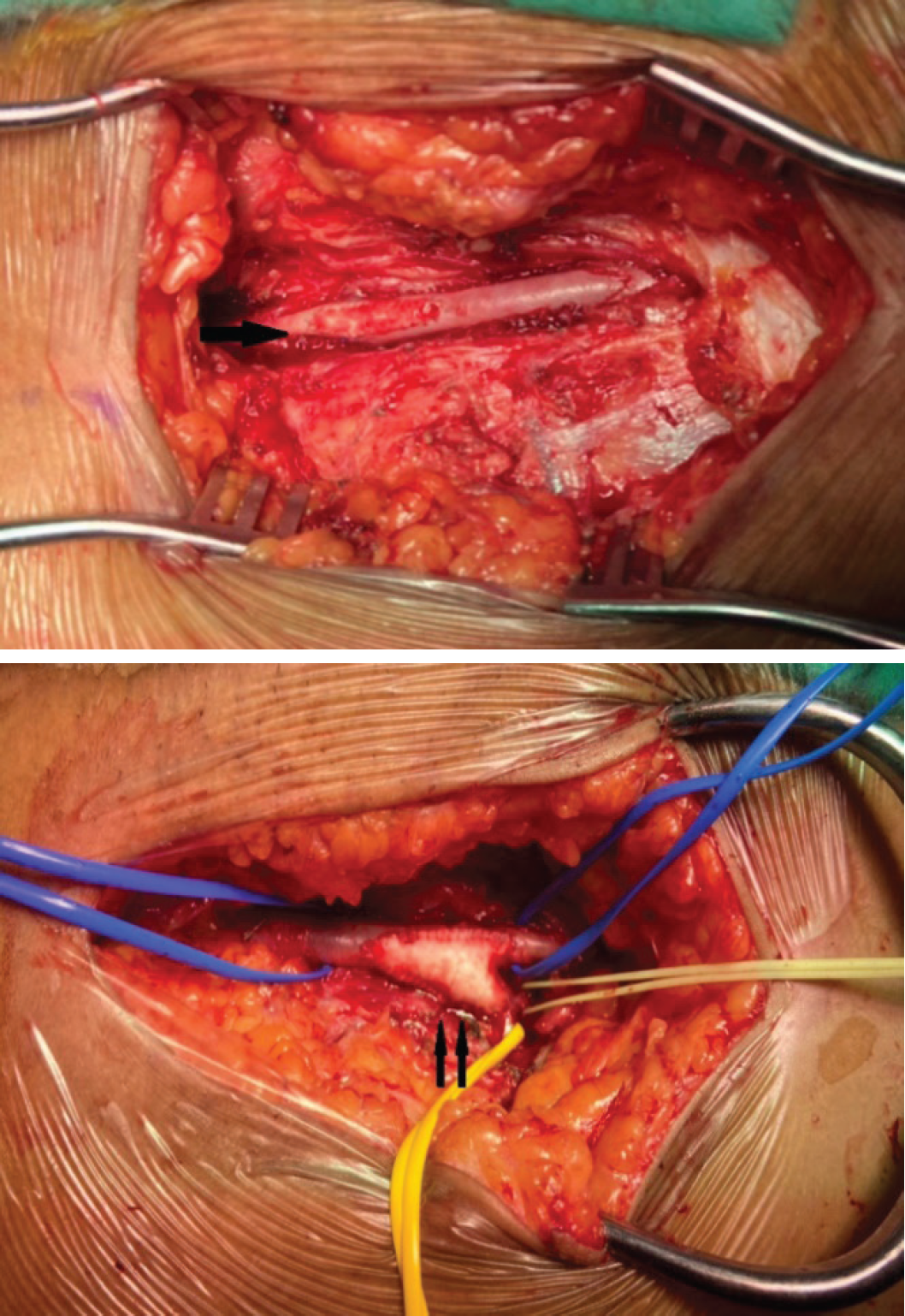
(a) Left common femoral artery bifurcates to the superficial femoral artery and profunda artery which is not visualized in this diagram given it is posteriorly located. Note the single arrow point on the patch repair of the arteriotomy. (b) Right common femoral artery bifurcates to the superficial femoral artery and profunda artery (arrow site). The double arrow pointed to the profundaplasty by using a vascular patch.
In this case, as the circulation of the lower limb was compromised, emergency surgical intervention with bilateral femoral embolectomy and right profundaplasty was performed in a timely manner. This case highlighted that despite the rarity of BCNIE causing limb ischemia, it can still occur due to significant risk factors. The early recognition of acute limb ischemia and prompt treatment are deemed important in saving the threatened limb from being amputated.
Conclusion
BCNIE poses a dilemma in diagnosis and treatment. It requires extensive investigation to prove the existence of the causal organisms through culture and sensitivity, serology testing, or polymerase chain reaction which might not be available in the local setting. Experts’ consensus is mandatory in the treatment of BCNIE. The choice of antibiotic must be based on the local antibiogram and target the most likely source of infection. The thromboembolic phenomenon to the lower limb is rare but should raise suspicion of the treating physician based on the patient’s symptoms and clinical signs. The involvement of vascular surgeons in treating acute thromboembolic phenomena in BCNIE is a must. The intervention may vary according to the affected vessels. Risk stratification of developing distal emboli should be recognized early and the patient may benefit from surgical debridement and valve replacement.

