Background
Calcinosis cutis, a rare disease first described in 1985, implies pathological deposition of calcium in the skin and subcutaneous tissue. The exact pathological mechanism pertaining to disease presentation remains unclear however local inflammation may have a role in the development of the disease process. Its presentation has been linked to various diseases; however, it has not been demonstrated as a severe COVID-19 infection-related manifestation.
Our case denotes the combination of metastatic and iatrogenic calcification where severe COVID-19 infection resulted in acute renal failure and hypocalcemia requiring calcium administration and consequently the development of calcinosis cutis. Clinically, it commonly manifests as a firm to hard, whitish, or yellowish isolated or multiple lesions. However, in the case described below it was an uncommon, atypical fleshy appearance initially that was not diagnostic of calcinosis cutis and hence was not included in our list of differentials diagnosis until histologically proven.
Case Presentation
A 55-year-old gentleman with a known history of asthma and chronic migraine was admitted to the intensive care unit (ICU) for invasive ventilation with severe COVID-19 infection. Regular medications included amitriptyline and inhalers. His ICU stay was complicated by acute renal failure requiring hemodialysis, staphylococcal bacteremia, and spontaneous splenic rupture. He was treated with dexamethasone, linezolid, and erythromycin. During the course of his illness, he developed hypocalcemia of 2.08 mmol/l (normal range: 2.2-2.6 mmol/l). Both oral calcium and intravenous calcium gluconate were administered to replace calcium deficiency for approximately 2 weeks. Four weeks later, he developed a tender lesion on the medial left ankle. It was fleshy in appearance initially; therefore, calcinosis cutis was the unlikely differential due to examination findings. It later developed into a 5-cm well-circumscribed yellowish indurated plaque with areas of ulceration and a few satellite lesions were also present (Figure 1).
The lesion was not entirely diagnostic, and the list of differential diagnoses included hypertrophic lichen planus, fungal infection, and impetigo. Metabolic screening demonstrated an elevated adjusted serum calcium of 2.97 mmol/l and phosphate of 1.86 mmol/l. Alkaline phosphatase was mildly elevated at 164 U/l (normal range: 30-130 U/l) with reactive hypoparathyroidism of 0.9 mmol/l (normal range 1.6-6.9 mmol/l). Serum creatinine was significantly elevated at 540 umol/l initially but reduced to 269 umol/l following the hemodialysis, suggestive of acute renal failure. Serum inflammatory markers were moderately elevated with C-reactive protein (CRP) 50 mmol/l and WCC 12.3 × 1012/l. Serum pH was normal, 7.39. The auto-immune profile for connective tissue disease screening was negative. A Computer tomography (CT) chest demonstrated COVID pneumonitis.
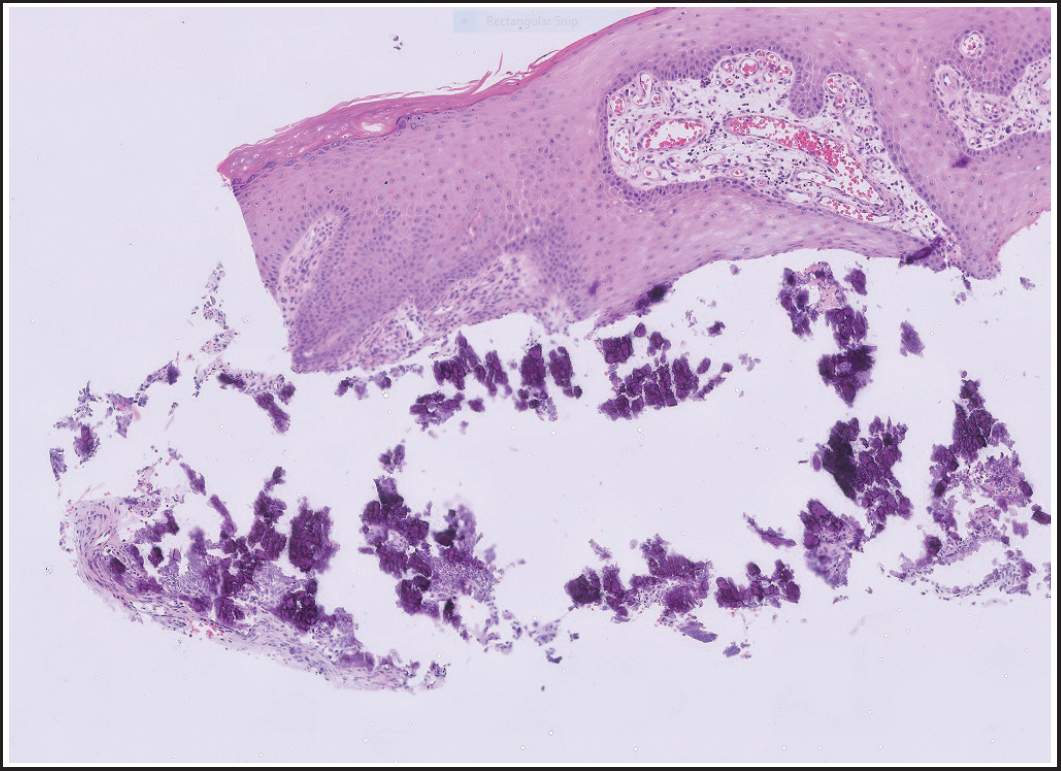
Surface parakeratosis with calcification in the superficial dermis and around blood vessels (original magnification ×10).
A punch biopsy of the skin lesion was performed to clarify an uncertain diagnosis. The histopathology at 10× magnification showed surface parakeratosis with dense calcification within the superficial dermis and calcification around blood vessels, consistent with calcinosis cutis (Figure 2).
The lesion was treated with a topical super-potent corticosteroid that resulted in significant improvement.
Discussion
Our case demonstrates the novel aspect of skin manifestation in a COVID case [1]. Although, calcinosis cutis has been described in chronic renal failure [2,3], however, the appearance of atypical isolated skin lesions of uncertain significance and subsequently diagnosed as calcinosis cutis in the context of COVID and COVID-related acute renal failure has not been described previously. Calcinosis cutis is the abnormal deposition of calcium salts in the skin and subcutaneous tissue. There are four main etiologies: dystrophic, metastatic, iatrogenic, and idiopathic [4,5]. Dystrophic calcinosis cutis is the commonest type where tissue damage causes a release of phosphate protein which calcifies into subcutaneous tissue [6]. Calcium and phosphate levels are typically normal. The metastatic variant is associated with the abnormal metabolism of calcium and phosphate. Iatrogenic calcinosis cutis can occur by treatment with calcium salts [7], finally, the idiopathic variant occurs in the absence of any known tissue injury or a systemic metabolic defect. The clinical presentation varies from solitary or multiple white-yellow firm papules, nodules, or plaques. Ulceration within a lesion results in pain. Occasionally, a chalky white discharge can be seen on the surface of the lesions. A diagnostic skin biopsy demonstrates abnormal calcium deposits in the specimen with stain dark blue with hematoxylin and eosin and black with Von Kossa stain [8].
Treatment is focused on the underlying cause. Topical sodium thiosulphate is utilized to increase the solubility of calcium [9]. Oral diltiazem, intralesional and topical corticosteroids, probenecid, bisphosphonates, and surgical excision have also been described to varying levels of success. Carbon dioxide laser has also been proven effective in treating some lesions [10].
This case demonstrates a combination of metastatic and iatrogenic calcinosis cutis [11,12]. Severe COVID-19 infection progressing to acute renal insufficiency and causing abnormal calcium metabolism is the most likely explanation of metastatic calcification in this case which was further complicated by administering calcium during his admission. This case corroborates that calcinosis cutis can be a differential diagnosis, especially in a patient with acute renal failure with the recent administration of calcium salts. It further highlights the importance of cautious administration of calcium in patients with severe COVID-19 disease and related renal impairment.
Conclusion
This interesting case describes a presentation of calcinosis cutis in a patient with severe COVID-19 infection in the background of acute renal failure and calcium replacement. The development of organ failure carries the worst prognosis and denotes severe COVID-19 infection. Various cutaneous manifestations of COVID-19 have become known. However, this is a manifestation of an atypical clinical presentation of calcinosis cutis in the context of severe SARS-COV-2 infection that has not been reported previously. Once diagnosed, calcinosis cutis should be managed according to the underlying etiologies which include dystrophic, metastatic, idiopathic, and iatrogenic.
What is new?
This interesting case describes a presentation of calcinosis cutis in a patient with severe COVID-19 infection in the background of acute renal failure and calcium replacement. The development of organ failure carries the worst prognosis and denotes severe COVID-19 infection. Various cutaneous manifestations of COVID-19 have become known. However, this is a manifestation of an atypical clinical presentation of calcinosis cutis in the context of severe SARS-COV-2 infection that has not been reported previously.


