Background
As newborn babies have an open fontanelle and sutures, any increased intracranial pressure can usually be accommodated to some degree [1,2]. Therefore, in the immediate newborn period, it is an exceptionally rare event for the pressure to be sufficient to cause the brain to herniate. Typically, this would happen in a downward direction, through the foramen magnum, as has been reported in the context of hypoxia with diffuse brain edema [3-5] or secondary to an antenatally diagnosed frontal lobe tumor [6]. In these cases, there has generally been some point-of-care imaging performed prior to a definitive diagnosis being reached through Computerized Tomography (CT) or (Magnetic Resonance Imaging) (MRI) scanning [3,4,6]. Given the rarity and variety of underlying causes of these events, information regarding the outcome cannot easily be ascertained. However, it is notable from this literature search that the majority of neonates with cerebral or cerebellar herniation do not survive active treatment [6,7]; or are considered for palliative care [3-5].
An acute or rapidly expanding cerebellar hemorrhage would cause some pressure effect and has been reported to press the cerebellum upward [5,7], but has not been shown to cause upward herniation through the opening in the tentorium cerebelli prior to this case. Where the cerebellum has been affected, there is the potential for clinical signs relating to coordination and eye movements [1]. It is recognized that in childhood, vertical nystagmus is strongly correlated with significant intracranial pathology [8].
Case Presentation
A male infant was born via forceps-assisted vaginal delivery at 38 weeks gestation in a district general hospital in the United Kingdom. There was an antenatal history of reduced fetal movements in the previous 48 hours, and suspicion of chorioamnionitis. Prior to this, there had been standard antenatal care with normal scans. The only medication used in pregnancy was labetalol for maternal hypertension.
No resuscitation was needed at delivery and the birth weight was on the 91st centile. Cefotaxime was started empirically due to chorioamnionitis, and the baby remained with its mother in the postnatal ward.
At 17 hours of age, he collapsed with pallor, bradycardia, and respiratory distress. He was admitted to the neonatal unit and was intubated and ventilated. A full neurological assessment was abnormal, with little spontaneous movement, reduced tone both centrally and peripherally, with reduced suck and gag reflexes. At 20 hours of age, there was a clinical seizure with extensor posturing, lip smacking, and vertical nystagmus. This was treated with a loading dose of phenobarbitone, and empirical acyclovir was added to cover for viral infection.
The baby was then transferred to the tertiary neonatal unit where the neurological examination remained severely abnormal with lower limb hypotonia and increased tone in the upper limbs; minimal response to suck and gag stimuli and limited withdrawal responses. There was no respiratory effort on the ventilator. Cerebral function analysis monitoring showed a discontinuous normal voltage trace. There was one further episode of possible seizure with stiffening of the right arm with lip-smacking and hiccups. This was treated with a second dose of phenobarbitone alongside levetiracetam. Initial blood tests were unremarkable, other than mild hyponatremia and a raised c-reactive protein at 20 mg/l.
A cranial ultrasound was completed, which showed a large hyperechoic region around the thalamus, with an extension toward the brainstem. There was no evidence of intraventricular hemorrhage and the right and left ventricular indices were 16.4 and 17.1 mm, respectively (both 97th centile). The subsequent MRI showed an acute cerebellar hematoma (Figure 1) with a mass effect obliterating the posterior fossa cisterns. There was upward herniation of the right cerebellar hemisphere through the tentorium cerebelli with the displacement of the midbrain structures and associated edema.
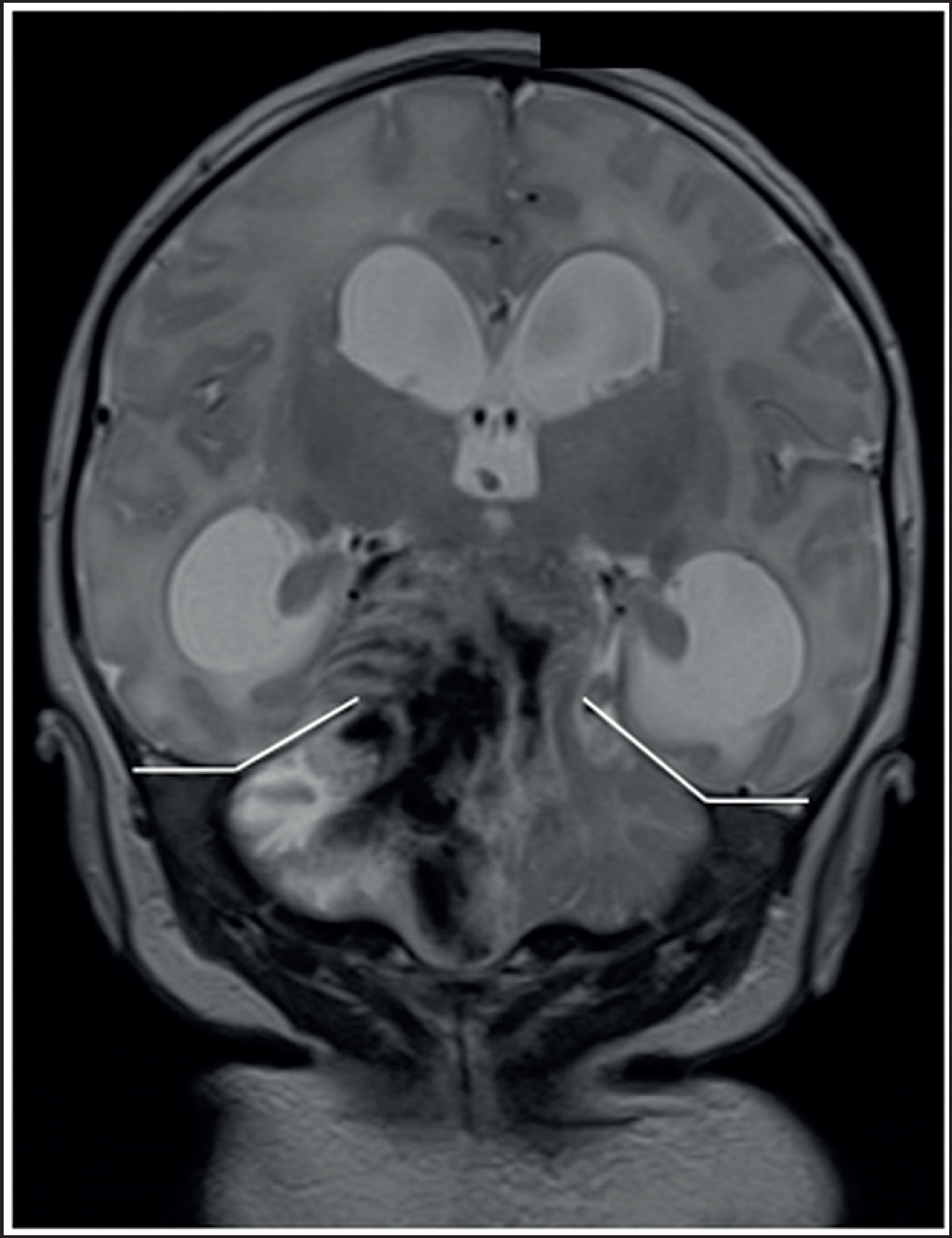
A T2 weighted MRI image in the coronal plane showing upward herniation of the cerebellum with associated mass effect causing obstructive hydrocephalus. The cerebellar tentorium is marked with white lines.
After extensive discussion in a multidisciplinary format including the neonatal and neurosurgical teams, the consensus was reached not to offer surgical intervention, but rather to focus on palliation, which was jointly agreed with the family. After extubation on compassionate grounds, there was an unexpected period of clinical stability and improving neurological status. A repeat MRI after 72 hours showed partial resolution of the hematoma and mass effect. The baby was transferred to the neurology ward for ongoing observation and consideration of surgical intervention. He has recovered sufficiently to be discharged home and remains under active surveillance.
At 3 months of age, he has made developmental progress with no evidence of raised intracranial pressure. There is reduced variation in spontaneous movements with some upper limb asymmetry with an imbalance in muscular tone. A further MRI scan at 13 months showed a normal myelination pattern, with some atrophy of the right cerebellar hemisphere and cortical white matter. At this age, he has normal gross motor development, with left-hand dominance and no pincer grasp as yet. The “Ages and Stages 3” questionnaire completed by the family reports age-appropriate communication, problem-solving, and social skills.
Discussion
There is a large list of differential diagnoses for a postnatal collapse, with definitive treatment being directed by the underlying pathology. This baby had suffered a significant intracranial event, which was responsible for the severe neurological abnormalities and the collapse. In this case, the intracranial abnormalities were first seen on cranial ultrasound scanning, confirming it is a useful point of care investigation which can detect a problem, even if more sophisticated modalities are necessary in due course.
This case illustrates that although a very rare event, cerebellar herniation secondary to massive hematoma is a possible cause of postnatal collapse and may present with neurological signs. As with older children, the presence of vertical nystagmus is a significant clinical sign in the immediate neonatal period. The significant distortion to the cerebellar anatomy is the likely cause for the nystagmus, but it is unclear about the timing of the expansion of the hematoma, given the interval between the initial collapse and the subsequent seizures.
Any neurosurgical intervention was felt to be exceptionally high risk in the multidisciplinary discussion, and it was uncertain regarding the long-term outcome even if surgery were to be successful. This was based on expert neurosurgical, neurological, and neonatal opinions. The period of clinical stability and improvement was unexpected and shows the importance of regular review of the direction of care in a palliative setting.
Follow-up is undoubtedly an important feature in this case as the literature review identified a very small cohort of similar patients, none of whom survived through to discharge. Therefore, there is no data suggesting the level of neurological impact that a surviving baby may experience, and this information could help to inform decision-making in other cases, acknowledging that this outcome is out of keeping with most cases. The resultant cerebellar atrophy is likely to be due to the mass effect of the initial hemorrhage, but the relatively mild clinical findings represent the plasticity and potential for the neonatal brain to recover from a significant and life-threatening insult, such as this.
Conclusion
Herniation of the neonatal brain is a rare cause of collapse in the newborn. It can present with focal signs, such as nystagmus when the cerebellum is implicated and can occur in an upward direction through the cerebellar tentorium. Definitive diagnosis can be made with MRI scanning, with suggestive features on bedside cranial ultrasound scan. In this instance, the patient survived to discharge and has mildly impaired neurological assessment at 14 months of age.

