Background
Kaposi’s sarcoma (KS) was first described in 1872 by Moritz Kaposi as a highly aggressive form of sarcoma with a series of 5 cases [1]. While it was rare until the 1980s, its frequency gradually increased after the discovery of the human immunodeficiency virus (HIV) and its becoming epidemic [2]. KS was reported to be associated with Human Herpes Virus-8 (HHV-8) in 1994 [3]. Although it is frequently seen in the lower extremities associated with HIV, it can also occur in any cutaneous area or visceral organs [4]. In the systemic disease stage of acquired immunodeficiency syndrome (AIDS), caused by HIV, organ involvement may occur in 20% of the patients. However, only 2%-3% of these patients have isolated primary KS [5]. Therefore, isolated primary penile KS in an HIV sero-negative patient is an extremely rare condition in the literature [6].
In this study, we aimed to present a case of isolated primary penile KS unrelated to HIV and to review the management of the disease.
Case Presentation
A 65-year-old man, with no history of homosexual or bisexual activity, presented with reddish nodules on penis. These lesions, he noticed 3 months ago, did not grow over time. They were painless. There was no urethral discharge. Past medical history included only hypothyroidism. There was no history of sexually transmitted disease or multiple sexual partners. He was circumcised and physical examination revealed 2 pigmented, raised on the surface, nodular lesions, approximately 3 mm in diameter on the ventral site of the glans penis and foreskin (Figure 1). No other lesions were found in the genital area, oral cavity or other cutaneous areas. There were no enlarged inguinal lymph nodes.
Serum creatinine, prostate specific antigen (PSA), and urine analysis were within normal limits. Serological tests for HIV, hepatitis, and syphilis were negative. Biopsy was recommended to the patient for definitive diagnosis. Excisional biopsies taken from the glans penis and foreskin, measuring 1.1 × 0.7 × 0.3 cm and 0.5 × 0.4 × 0.3 cm, respectively, were sent to pathology. Histopathological examination revealed that the nodule located in the upper dermis was composed of monomorphic spindle tumor cells with fascicular pattern accompanied by frequent mitoses and erythrocytes (Figure 2). The tumor cells displayed nuclear positivity with HHV-8 antibody (Figure 2). Thus, the case was diagnosed as classical type KS nodular stage (Figure 3). Surgical margins were negative. Subsequently, thoracoabdominal computed tomography was performed to exclude disseminated disease. No distant metastases or lesions were detected.
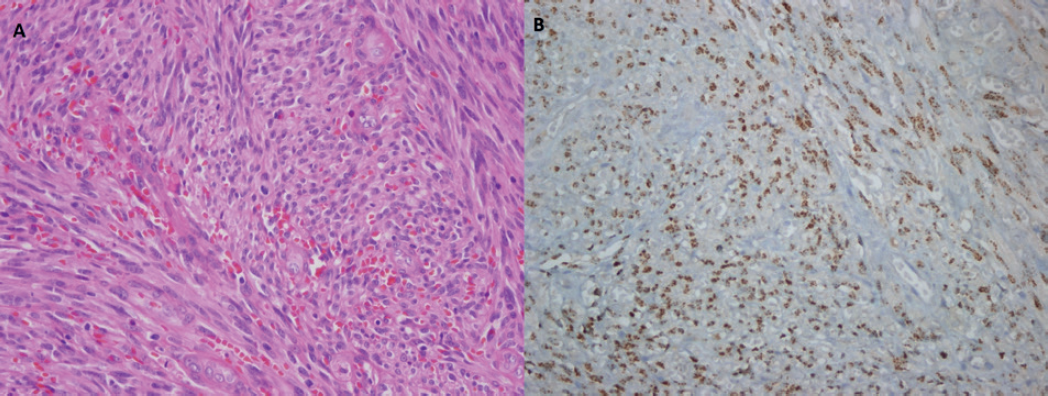
(A) Spindle neoplastic cells and frequent mitoses, 400× magnification. (B) Nuclear HHV-8 positivity in spindle neoplastic cells, 400× magnification.
The patient was consulted with medical oncology. It was decided that there was no need for additional treatment because all lesions were excised with negative surgical margins. No recurrence or disease progression was detected during the 4-year follow-up.
Discussion
KS is a multifocal, angioproliferative malignant lesion originating from lymphatic endothelial cells [7]. It was first described by Moritz Kaposi in 1872, and until the 1980s it was extremely rare [1]. With the spread of HIV in the 1980s, the incidence of KS has gradually increased. It is the most common malignancy in the patients diagnosed with AIDS. The association between KS and HHV-8, also known as Kaposi Sarcoma-associated Herpes Virus (KSHV) was first reported in 1994 [3].
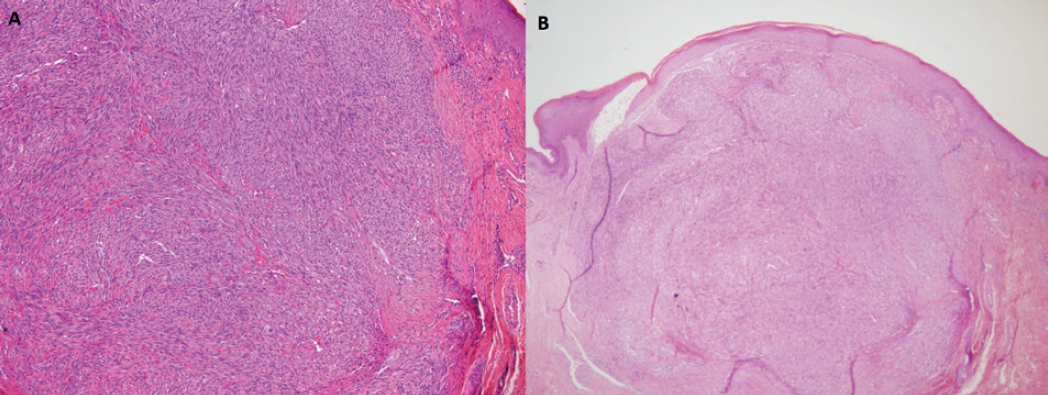
(A) Erythrocytes between fascicles composed of monomorphic spindle cells, 100× magnification. (B) Kaposi sarcoma nodular stage, 40× magnification.
KS is more common in men than women. There are 5 epidemiological and clinical subtypes of KS; classical (sporadic) type, AIDS-related (epidemic) type, iatrogenic type (seen in patients using immunosuppressant drugs as in solid organ transplantation patients), endemic type (often seen in HIV sero-negative individuals living in Africa) and non-epidemic (men having sex with men, without immunosuppression and HIV infection) type [7].
The seroprevalence of KSHV worldwide is estimated to be 5%-20%. The highest prevalence rate is observed in Africa (>50%), North America, and Asia have the lowest rates (<5%). A moderate prevalence is observed in the Mediterranean and Eastern Europe (5%-20%). Similarly, the incidence of KS is higher in Africa and Mediterranean regions compared to Asia and North America [7].
The epidemiology of the disease and the discovery of the role of KSHV in the pathogenesis indicates that KS develops independently from HIV. The main role of HIV is to cause an increase in KSHV infections. With the definition of combined antiretroviral therapies, a significant decrease has been achieved in the incidence of AIDS-related KSHV [8].
Disease presentation may range from a single cutaneous lesion to extensive visceral involvement [4]. Cutaneous lesions are usually multiple, pigmented, painless, flat or raised, nodules or plaques. In our case, 2 pigmented, painless, raised, nodular lesions were detected. KS limited to the penis is rare and often occurs in association with AIDS. While genital involvement is observed in approximately 20% of HIV sero-positive patients, isolated penile KS is detected in only 2%-3% of these patients [5]. Isolated penile KS is extremely rare in HIV sero-negative patients [6]. We considered our case as a very rare condition because of the patient had a isolated primary penile KS without HIV and any other risk factors.
The involvement sites and prognosis of the subtypes are usually different. Classical subtype is frequently observed in the Mediterranean regions and while the lesions usually occur in the lower extremities, visceral involvement is less common. Our case was diagnosed as classical KS and considered as a rare condition because the lesion appeared in an unusual location. In endemic subtype, typically observed in African children and the disease has an aggressive clinical course. It usually presents with multiple lymph nodes and lymphedema, and there is extensive visceral involvement. AIDS-related subtype is characterized by multiple cutaneous lesions on the extremities, trunk, and face. Visceral involvement is observed in 15% of the patients. In iatrogenic and non-epidemic subtype multiple cutaneous lesions are frequently observed but visceral involvement is rare [9].
Pyogenic granuloma, condyloma acuminata, glomus tumor, and molluscum contagiosum should be considered in the differential diagnosis. As in our case, histopathological examination of the resected tissue is required for differential diagnosis. Characteristic histological features are spindle-shaped tumor cells, extravasated erythrocytes, abnormally proliferated vascular structures and inflammatory cell infiltration. Spindle cells are actually differentiated, proliferating endothelial cells infected by KSHV. Detection of KSHV antigens in spindle cells by immunohistochemical staining is diagnostic [10].
There is no defined standard treatment for KS. The management should be based on the clinical and immunological features of the patient. Since KSHV eradication is not possible, the main purpose of the treatment is to reduce the symptoms, number and size of the lesions, and prevent disease progression [11].
Surgical excision is recommended for small and solitary lesions. Local recurrence is rarely observed in patients with complete excision of the primary tumor [6]. In our case, the lesions were excised with a negative surgical margin and no recurrence was observed in the 4-year follow-up. Radiotherapy is recommended for large and multiple lesions, but the risk of tissue fibrosis in the penis and associated erectile dysfunction development should be considered [11]. In addition, cryotherapy was also reported for local treatment and a success rate of 85% was mentioned, but its effectiveness was only shown in small lesions. It may cause hypopigmentation and scar formation [12]. In a recent study, 151 patients, who are treated with intralesional vincristine injection for local lesions, were prospectively investigated. Complete response was observed in 76.1% of the patients, and the total success rate was reported as 98.7% [13]. Laser ablation techniques were also reported for the treatment of local lesions [14].
Conclusion
Isolated primary penile KS is rare and often occurs in HIV sero-positive patients. It is extremely rare in HIV sero-negative patients but it should be kept in mind in the differential diagnosis of pigmented and nodular lesions in the penis. Excisional biopsy and histopathological evaluation are required for definitive diagnosis. Although there is no defined standard treatment, excision of lesions with negative surgical margins has a high success and very low complication rate, as in our case.


