Background
Psychiatric history
We describe a case of late onset organic (secondary) psychosis that could be conflated with primary (functional) psychosis. The former, however, has prominent positive psychotic symptoms that are associated with warm and unrestricted affect and commonly not associated with family history of mental illness. In contrast, primary psychosis can be associated with positive and negative symptoms, patients may endorse blunted affect and follow the treatment resistant trajectory. There are similarities in the primary and secondary nature of psychosis that may conflate the diagnosis and hinder timely treatment; hence, early recognition of the etiology of the psychosis would be of paramount importance to reduce suffering and prevent chronicity of such patients as demonstrated in this case report.
This is a case of a 52-year-old female who presented with first episode psychosis to psychiatric services in 2018 at the age of 48 which resulted in admission under the Involuntary Psychiatric Treatment Act. Although she was not known to psychiatric services before this episode, three years prior to her admission she had become preoccupied with the notion of spirits. She believed that these “spirits” entered her home via electrical outlets, and family members witnessed her talking to them (spirits). She also believed that the electrical wiring and television in her house were bugged, which drove her to cover several appliances with tinfoil to stop what she described as “waves from roaming around”.
A few months prior to the patient’s admission into acute care, her psychosis became polymorphic in nature comprising auditory second and third-person, commentary auditory hallucinations, and visual hallucinations of people being attacked, to whom she was calling out to save. She also developed persecutory delusions in which her ex-husband was incorporated. In this, she accused him of having access to her house through a “portal” of electrical wiring and a “stingray” gun that she could feel in her body (tactile hallucinations and somatic delusion). Consequently, she covered her windows and electrical appliances with tinfoil and bags, attempting to reduce these perceived incursions. She also endorsed grandiose delusions of predicting the future, sensing energy in people, having premonitions, and being able to see future events before they are reported on the news.
Furthermore, she was switching off the main electricity breaker to stop the “persecutors” from getting into her home via the electrical outlets. This resulted in food spoilage and molds developing in her fridge-freezer. She was noted to be neglecting her personal hygiene and was reported on occasions to scream in the middle of the night. She was also hiding a wooden stick underneath her bed for “self-defense”. Her sleep pattern and appetite became subsequently erratic.
During the initial assessment, she was pressured and disorganized in speech, she was wearing protective gear that included a hat embroiled with tinfoil, an eye shield, and had tissue paper inserted in her ears that she claimed was protecting her from “contaminants”. She dismissed concerns expressed by her father and described the whole psychotic experience as being magical with eutonia (a sense of physical well-being) and a prevailing mood of serenity. She did not demonstrate negative symptoms and she has no family history of mental illness.
Cognitively, she scored 26/30 on the Montreal Cognitive Assessment, MoCA [1]; she lost 3 points on delayed recall and 1 point on language. Functional occupational therapy (OT) assessment revealed difficulty with problem solving but she was deemed safe to live independently.
Olanzapine treatment was initiated and titrated up to 30 mg daily prior to her discharge in January 2018, which gradually ameliorated her psychosis. However, because of poor compliance with her psychotropic medication, she eventually relapsed and was readmitted within 6 months of her discharge (June 2018). Olanzapine was then reinstated, and she hence improved during her second admission. Her cognitive functions were reassessed utilizing Mini-Mental State Examination and MoCA in which she scored 29/30 and 24/30, respectively. On the latter, she lost 2 points on language, 3 points on recall, and 1 point on drawing a clock-face.
Following the second discharge from acute service, the patient continued to comply poorly with her oral antipsychotic medication which resulted in ongoing psychosis. This impeded her ability to develop insight into her MS condition and allow follow-up with neurology for management. Hence, Long Acting Injectable Antipsychotic medication was considered, to which the patient reluctantly agreed to trial. In February 2019, she was switched to Zuclopenthixol decanoate depot that was gradually titrated to 250 mg intramuscular (IM) fortnightly; this resulted in remarkable eradication of her psychosis.
Neurological history
The patient was formally diagnosed by a neurologist with relapsing and remitting multiple sclerosis (RRMS) in 2001, at the age of 32, but she had exhibited symptoms of demyelination 2 years earlier that spontaneously cleared. She was followed up by a neurologist until 2017 but had, against medical advice, discontinued MS treatment in 2007.
Because of the relapsing nature of her MS, she presented to the neurology clinic with a myriad of protean symptoms e.g., migraines, fatigue, dizziness, and vertigo associated with ringing in her right ear; numbness affecting both feet and spreading to her waist, weakness in her right leg, migratory paresthesia affecting all limbs, intermittent double vision with horizontal separation of images, and urinary frequency with no incontinence.
She was previously treated with Interferon Beta 1A IM (Avonex) but discontinued it due to poor tolerability. Subsequently, she was offered, but continued to decline, other disease modifying therapy (DMT) since 2007; for example, Copaxone, Teriflunomide, Tecfidera, and Mavenclad. She chose instead to take Vitamin D, Omega 3-6-9, flax seed oil, and other natural supplements until the eruption of her psychosis in 2018.
With psychosocial education and persuasion, the patient agreed to receive a neurology consultation in 2018. She was restarted on a DMT (Mavenclad) in November 2019, which was 9 months after commencing her antipsychotic depot treatment. In combination, these therapies halted the progression of her MS lesions, and stabilized her mental status. Eventually, there was full and remarkable resolution of her psychosis that allowed gradual dose reduction of the antipsychotic medication without re-emergence of psychosis.
In November 2020, the patient received her second round of Mavenclad with no reported issues. There has been no further progression of her brain demyelination since November 2019 and her antipsychotic medication was subsequently reduced and then discontinued, with the maintenance of recovery.
Family history was remarkable of the patient’s mother having Parkinson’s disease and multiple malignancies including various second-degree relatives who died from cancer of either the liver, thyroid, colon, or stomach. There was no history of mental illness in her bloodline reported.
Special investigations
January 2010 magnetic resonance imaging (MRI) brain scan
January 2010 MRI Brain Scan revealed progression of MS with the emergence of new T2 lesions and enlargement of old lesions. MS lesions were seen in mid-pons, floor of the 4th ventricle, right side, superior cerebellar peduncle, and at the peripheral in the cerebellum. Small lesions were more prominent intracranially on the left compared with the right side, in addition to focal cord expansion at the level of C3. This indicated Recurrent and Relapsing MS (patient was off Interferon).
June 2013 MRI brain scan
(Brainstem relapse) Abnormal high T2 and fluid-attenuated inversion recovery (FLAIR) signal lesions were demonstrated in the left cerebellum that were more conspicuous when compared with the MRI from 2010. Bilateral lesions were seen in the pons and multiple white matter lesions in the cerebrum were enlarged compared to the 2010 study. Several new lesions were also seen in the left cerebral peduncle, left thalamus, periventricular white matter, and the corpus callosum.
January 2018 MRI brain scan
(Concomitant with emergence of severe psychosis that led to acute psychiatric hospitalization):
White matter black holes were seen on T1 weighting. Some of these were new compared to the prior scan. T2 hyperintensities were seen paraventricularly and within the centrum semiovale and involving U fibers throughout. Lesions were seen within the corpus callosum, pons on both sides and beneath the floor of the 4th ventricle, and within the cerebellar hemispheres on both sides. When compared to the prior examination multiple new lesions were seen. None had a mass effect. There was no restricted diffusion, no hydrocephalus, and no cerebral atrophy. (Figure 1)
Impression
Diffuse white matter T2 hyperintensities are seen compatible with the diagnosis of MS. In the interval from the prior examination in July 2013 multiple new lesions have appeared.
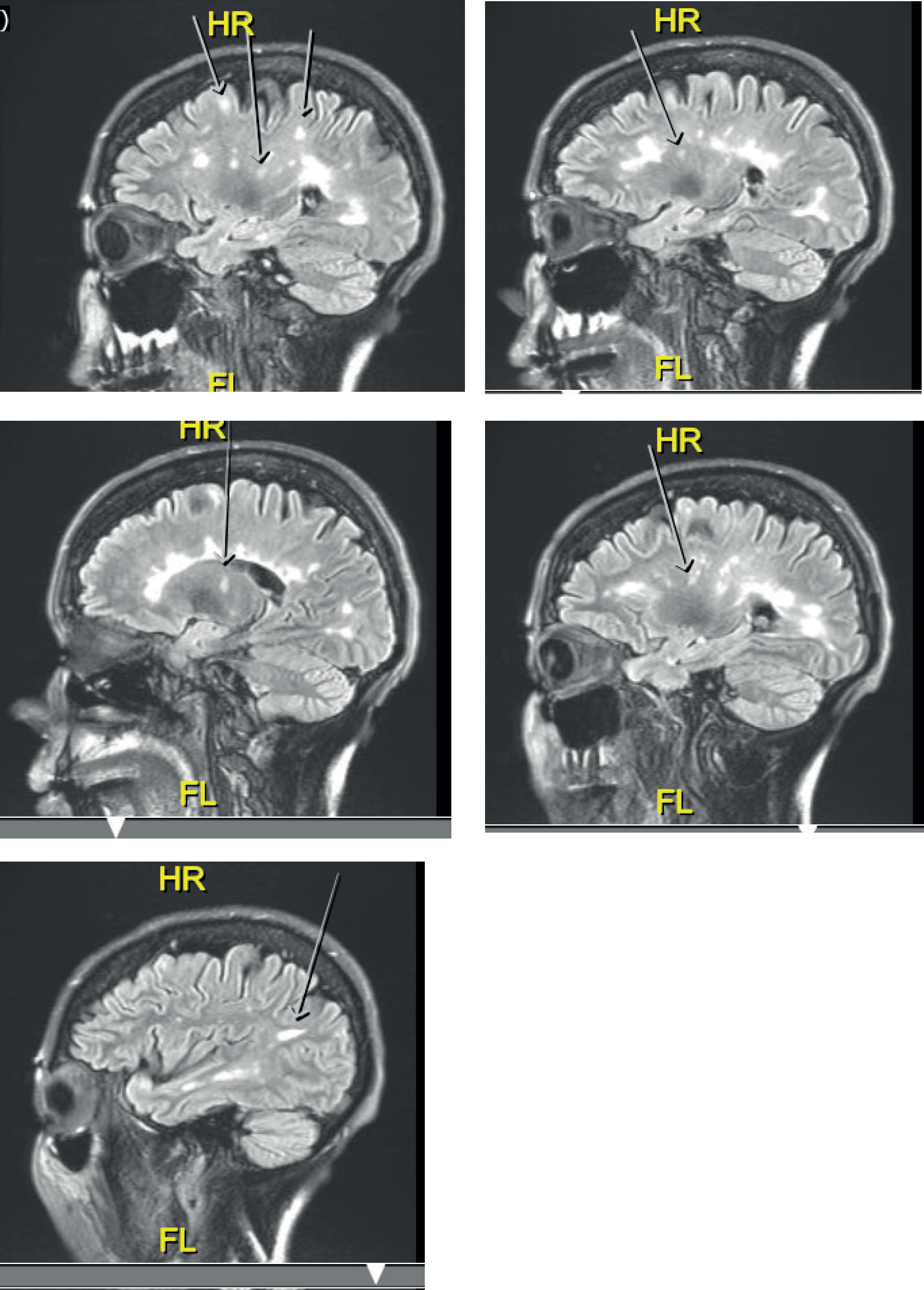
MRI brain scan performed in January 2018 demonstrating multiple new lesions of demyelination concomitant with the emergence of psychosis.
July 2018 brain MRI and spinal cord scan
Showed stable MS lesions with no new lesions noted. MRI Cervical/thoracic/lumber in July 2018 demonstrated short segment eccentric T2 hyperintensities in the Cervical and Thoracic cord consistent with demyelination.
May 2020 brain MRI scan (after DMT)
Showed stable white matter lesions. There was no increased cerebral atrophy or ventricular size. Some lesions were less distinct from prior ones. No new lesions were seen when compared to prior.
June 2021 brain MRI
Showed stable white matter lesions compatible with demyelination with no emergence of new lesions.
Laboratory investigations
To exclude other possible causes of organicity, the patient had extensive laboratory investigations that included full routine chemistry panels, complete blood picture, iron studies, a full endocrine panel, serology for hepatitis B and C, rubella, measles, HIV, and immune-serological tests. Apart from raised prolactin (secondary to psychotropic medication) and a positive Scl-70 autoantibody test, all other results were unremarkable. Patients positive for Scl-70 are at high risk of developing the autoimmune condition scleroderma (70% of those who are positive) [2,3].
EEG in 2018 revealed nonspecific dysrhythmia grade 1 in the left temporal lobe, with no epileptiform interictal abnormalities identified.
Discussion
The reported patient developed her first episode psychosis at age 48. Her psychosis was protean and was initially refractory to treatment, even though, it was of late onset, and she did not have family history of mental illness. The main markers for organic (secondary) versus functional (primary) psychosis was that it was of late onset, mainly protean positive psychotic symptoms, the patient maintained warm and unrestricted affect, and did not experience negative symptoms. The patient achieved a remarkable recovery from her psychotic symptoms after she received antipsychotic medication and treatment for her MS. The organic nature of this patient’s psychosis has been confirmed further after discontinuation of her antipsychotic medication and her steadfastly maintaining recovery from psychosis after her MS was treated.
MS is an immune-mediated demyelinating neurological disorder that can be associated with psychiatric sequelae. It is estimated to affect 2.5 million people worldwide with a preponderance in women and in white populations living in northern latitudes [4]. The mean age of onset is 30 years, and female: male ratio is 3:1.
The disease commonly emerges as a clinically isolated syndrome (CIS) presenting with e.g., optic neuritis and brain stem involvement as demonstrated in this case report. MS patients often follow an RRMS within 5 years from the CIS. Permanent disability occurs when there is incomplete recovery from relapses or when the disease becomes secondary progressive which usually takes 15-20 years from its onset. Some patients may follow a benign course with little disability, while around 15% may follow a primary progressive course from the onset. Overall MS reduces life expectancy by a median of 7 years [4].
The patient we present here developed her first MS symptoms in 1999 around the age of 30 years but was formally diagnosed within 2 years with an RRMS. Her psychiatric manifestations emerged 15 years later, and she had her first psychiatric admission following an acute psychotic episode, at the age of 48 years.
Psychiatric manifestations secondary to MS were reported previously by Charcot in 1877 [4]. Cottrell studied 100 cases of MS and reported depression, euphoria, lability of affect, and eutonia in patients with an established diagnosis of MS [5]. Marrie et al. [6] performed a systematic review of 118 population-based studies that had shown several psychiatric co-morbidities with the highest prevalence of depression 23.7%, followed by anxiety 22%, alcohol misuse 15%, bipolar disorder 6%, psychosis 4.3%, and substance misuse 2.5% [6].
The prevalence of psychosis is higher in MS patients compared to the general population at 4% versus 0.5%, respectively, in those aged between 15 and 25 years with no significant difference in those aged 65 or above [4,6]. Feinstein et al. [7] compared 10 MS patients who had psychosis with an age, gender, and disability-matched MS group who did not have psychosis. The lesion burden on MRI brain scan was greater in the psychosis group, particularly around the temporal horns. The mean age of onset of psychosis was 39.6 years (our patient developed psychosis around the age of 45 years), later than the age expected for a primary psychotic illness (schizophrenia). Feinstein indicated that in 9 out of 10 patients neurological symptoms preceded psychosis by an average of 8.5 years. The onset of psychosis coincided with MS relapse in four patients. Symptoms mimicked those of schizophrenic positive symptoms, with persecutory delusions being the most common (70%), followed by passivity phenomena (30%), thought disorder (20%), and third-person auditory hallucinations in 20%. Similar to Feinstein’s [7] study, our patient’s symptoms improved in response to antipsychotic medication. However, her compliance on oral antipsychotic medication (Olanzapine 30 mg) was erratic, and she improved dramatically when switched to Zuclopenthixol decanoate depot IM.
Gilberthorpe et al. [8] studied the spectrum of psychosis in MS in a clinical case series of 15 patients with a concomitant diagnosis of psychotic disorder. Those patients either had a definitive diagnosis of MS or MRI evidence of demyelination in the absence of neurological symptoms, known as radiologically isolated syndrome (RIS). He subdivided his case series into three subgroups, the first subgroup was those with progressive MS; where neurological symptoms predated the onset of first episode psychotic symptoms with a diagnosis of organic schizophrenia-like psychosis (9 patients). This group represented the majority (60%) of patients who had progressive MS and neurological symptoms for several years before the emergence of psychosis. They also had cognitive impairment and their brain MRI showed significant lesions of demyelination similar to those seen in our patient. In the second subgroup (3 patients), first episode psychotic symptoms predated the diagnosis of MS or an RIS. Those patients received an ICD-10 diagnosis of schizophrenia several years before they were diagnosed with MS with a latency of 7-12 years between the emergence of psychosis and the MS diagnosis. The third group consisted of three patients whose first episode psychosis was diagnosed within the same year of MS being detected. Gilberthorpe noted in his case series that the onset of psychosis in MS was at a later age compared to the general population. Males with MS had a preponderance to develop psychosis when compared to females in that study; however, this gender disparity was not found in a large Canadian study [9]. Gilberthorpe also commented that a high percentage (73%) of patients in his cohort showed mild or moderate cognitive impairment [8].
The mechanism of psychosis in MS was attributed, by Andreassen et al. [10] to a shared genomic risk locus within the major histocompatibility complex region of chromosome 6. This region is common to MS and schizophrenia but not to bipolar disorder; suggesting that abnormal myelination may be the shared basis for both conditions [10].
Moreover, autoimmunity has been suggested as a shared risk factor between schizophrenia and MS. Schizophrenia is associated with a 50% increase in life-time prevalence of autoimmune disease and there is an increased familial association between autoimmune disease and schizophrenia [2]. Titulaer et al. [3] described 23 out of 691 patients with autoimmune encephalitis (anti-N-methyl-D-aspartate receptor or anti-NMDAR encephalitis). He suggested that the latter could cause psychosis in patients with MS and other demyelinating diseases which could be overlooked, with subsequent delay in therapy with immunosuppressants [3]. Notably, our reported patient was positive for Scl-70 autoantibody test which represents a high risk of developing an autoimmune condition of scleroderma.
Impaired cognitive function has been considered as an added burden compounding disability from MS, limiting independence, ability to work, and treatment concordance. Cognitive impairment is present in 40%-70% of patients with MS in cross-sectional studies and its severity increases in progressive MS. This impairment may present differently in MS patients e.g., decreased intelligence quotient from the premorbid state, slower processing, impaired learning, executive function, and social cognition but preserved simple attention and basic language skills [4]. Our patient scored 24/30 on MoCA [1], losing 2 points on language, 3 points on recall, and 1 point on drawing a clock-face. Functional OT assessment revealed difficulty with problem solving but she was deemed safe to live independently. White and grey matter lesions and abnormalities in Normal Appearing Brain Tissue cause disconnection in widespread networks relevant to cognition. Indeed, our patient’s MRI brain scan in 2018 showed several new and deep lesions affecting multiple areas in her brain that were concomitant with the development of severe psychosis and cognitive impairment.
The patient reported here, has a significant family history of cancer, mainly in second-degree relatives. In the study by Bahmanyar et al. [11] they used the Swedish general population register data to examine the cancer risk among 20,276 patients with MS and 203,951 individuals without MS (control). Similar analysis was conducted among the parents of the MS and control groups. There was an overall reduced risk of cancer among the MS group but there was increased risk of brain tumors and urinary organ cancer. The parents of patients with MS did not have an increased or decreased risk of cancer. The author commented that the overall reduced risk of cancer in the MS patients could be related to behavioral changes, treatment, and better anti-tumor surveillance. Nevertheless, MS increases the risk of brain and urinary organ cancer.
MS is a disabling neurological disorder that can be compounded by a co-morbidity of psychosis that may be sharing the same etiological and pathophysiological trajectory. This would understandably be an added burden that undermines the patient’s ability to insightfully deal with the primary illness (MS). Hence, early detection and treatment of such a condition are of paramount importance to enable recovery.
The emergence of psychosis prior to the neurological manifestations of MS could confound the clinical picture, delay the important diagnosis of MS, and label the patient with a primary psychotic condition. Hence, it is crucial to raise awareness amongst both psychiatrists and neurologists of the implications of missing either of the diagnoses when they co-occur. Suspicions should be high of organicity in general, especially when psychosis is late onset, polymorphic, treatment resistant and associated with an intact/warm affect.
We hope by sharing this case report with the scientific community that we shed light on the nature of organic/secondary psychosis associated with MS, the relevant neuropathology, and the conundrum surrounding its diagnosis and management.
What is new?
Multiple sclerosis (MS) is a disabling neurological disorder that can be compounded by a co-morbidity of psychosis and other psychopathology that may be polymorphic in nature. This would understandably be an added burden that undermines the patient’s ability to insightfully deal with the primary illness (MS). Hence, early detection and treatment of such a condition are of paramount importance to enable recovery.

