Background
Colon adenocarcinoma is the third most common cancer in the world [1]. The most common presenting symptoms are changes in bowel habits, rectal bleeding, abdominal mass, and iron deficiency anemia [2]. Colon adenocarcinoma presenting as terminal ileitis and abscess formation are rare entities that are estimated to be 2% [3,4] and 0.3%-4% [5], respectively. The differential diagnosis of terminal ileitis mostly encompasses inflammatory, infectious, and rarely malignancy causes [6]. Given the broad differential diagnosis, identification of the underlying etiology is essential to the proper treatment [7]. Here, we present a case of recurrent terminal ileitis with abscess formation that revealed a cecal adenocarcinoma with extension into the terminal ileum.
Case Presentation
An 83-year-old female with a history of appendectomy, ascending colon tubular adenoma, and osteoarthritis on naproxen, presented with 7 days of the right lower quadrant (RLQ) abdominal pain, fever, and leukocytosis to 13.4 k/ul (77% segmented neutrophils). The patient had no medical or family history of colon cancer or inflammatory bowel disease (IBD). A contrasted computerized tomography (CT) study of the abdomen and pelvis revealed an abscess (Figure 1) and thick-walled terminal ileum with inflammatory fat stranding. Percutaneous drainage of the abscess was performed with culture-growing Streptococcus anginosus, Escherichia coli, and Haemophilus parainfluenzae. The patient was treated with intravenous piperacillin/tazobactam followed by oral ciprofloxacin and metronidazole for a total of 14 days. A subsequent colonoscopy 3 months after presentation revealed mild ileitis with a biopsy showing normal mucosa in the cecum and the terminal ileum. The etiology of terminal ileitis was thought to be non-steroidal anti-inflammatory drugs (NSAIDs) use, due to thick-wall terminal ileum, mild inflammation from colonoscopy, history of naproxen use for osteoarthritis, and exclusion of other causes. It was unclear why the biopsy was unrevealing, but it could be due to sampling error. She was advised to avoid NSAIDs.
The patient remained asymptomatic for 2 years after this episode. She then presented with 3 days of RLQ abdominal pain, fever, and intentional weight loss of 30 lbs. The patient denied NSAIDs use, melena, hematochezia, or change in bowel habits. Laboratory evidence was remarkable for leukocytosis to 10.9 k/ul (88% segmented neutrophils), lactate of 1.5 mmol/l (0.5-2.2 mmol/l), and CRP of 189 mg/l (0-10 mg/l). A CT study of the abdomen and pelvis with contrast revealed a fluid collection (Figure 2a), thickened wall, and fatty infiltration of the terminal ileum (Figure 2b). A diagnosis of recurrent terminal ileitis complicated by abscess formation was made. The initial suspected diagnosis was Crohn’s disease (CD), so the patient was treated with intravenous piperacillin/tazobactam and methylprednisolone. A subsequent colonoscopy 2 days after presentation revealed a submucosal mass (Figure 3) located adjacent to the ileocecal valve. Additional laboratory evidence showed carbohydrate antigen (CA) 19-9 levels elevated to 65 U/ml (0-35 U/ml), normal carcinoembryonic antigen (CEA) levels, and fecal calprotectin levels of 100 ug/g (<49 ug/g). Biopsy revealed moderately differentiated adenocarcinoma (Figure 4). The patient underwent a robotic right colectomy. Grossly, the tumor was a circumferential 7.5 × 4.5 cm mass involving the ileum and cecum. The tumor invaded through the muscularis propria into pericolonic tissue. All surgical margins were negative. Four of 53 lymph nodes were positive for metastasis. Given the concern of inflammation, abscess, and tumor perforation around the cecum and terminal ileum, biopsy of the right pelvic wall was performed. The biopsy showed fibrous tissue with inflammation and foreign body-type giant cell reaction to luminal contents, consistent with tumor perforation. Final pathology revealed a moderately differentiated grade, pT3N2a stage adenocarcinoma of the cecum and terminal ileum. The postoperative course was uneventful. The patient elected to receive adjuvant capecitabine and had a resolution of her abdominal pain after the antibiotic and tumor excision.
Discussion
Here, we presented a case of cecal and ileal adenocarcinoma presenting as terminal ileitis with abscess formation. The differential diagnosis of terminal ileitis is very broad, including IBD, Meckel’s diverticulum, NSAIDs, vascular conditions, infection, lymphoid nodular hyperplasia, malignant diseases, and infiltrative diseases [8]. Infective diseases, such as tuberculosis and Yersinia enterocolitica, are the most common cause of terminal ileitis in developing countries [4]; IBD, specifically CD, is more common in developed countries [9]. Yet, terminal ileitis is a rare presentation of colon cancer, as demonstrated in this case report. A prospective study of 55 patients found that only 2% of patients with ileal and/or cecal wall thickening had adenocarcinoma [4]. It is thought that terminal ileum wall thickening is due to tumor extension (69%) or a nontumorous process (31%) such as congestion and edema [3]. Therefore, clinicians should have a high degree of suspicion for malignancy when presenting a case of terminal ileitis.
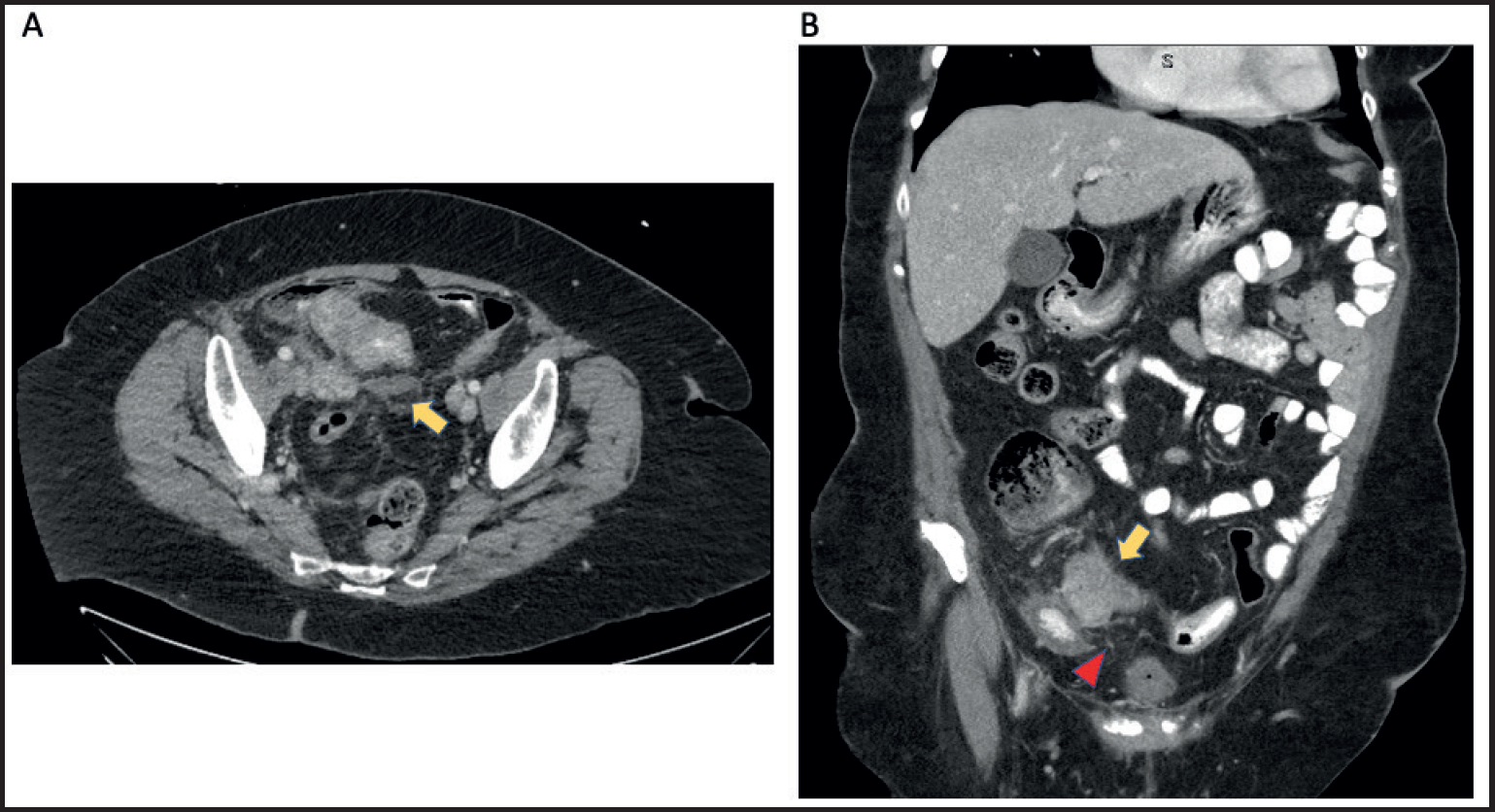
Contrasted CT scan of the abdomen and pelvis (a) A 3.5 × 1.1 cm lenticular fluid collection (yellow arrow) suggestive of an early abscess formation. (b) Thickened terminal ileal wall (yellow arrow) and area of fatty infiltration (red arrowhead).
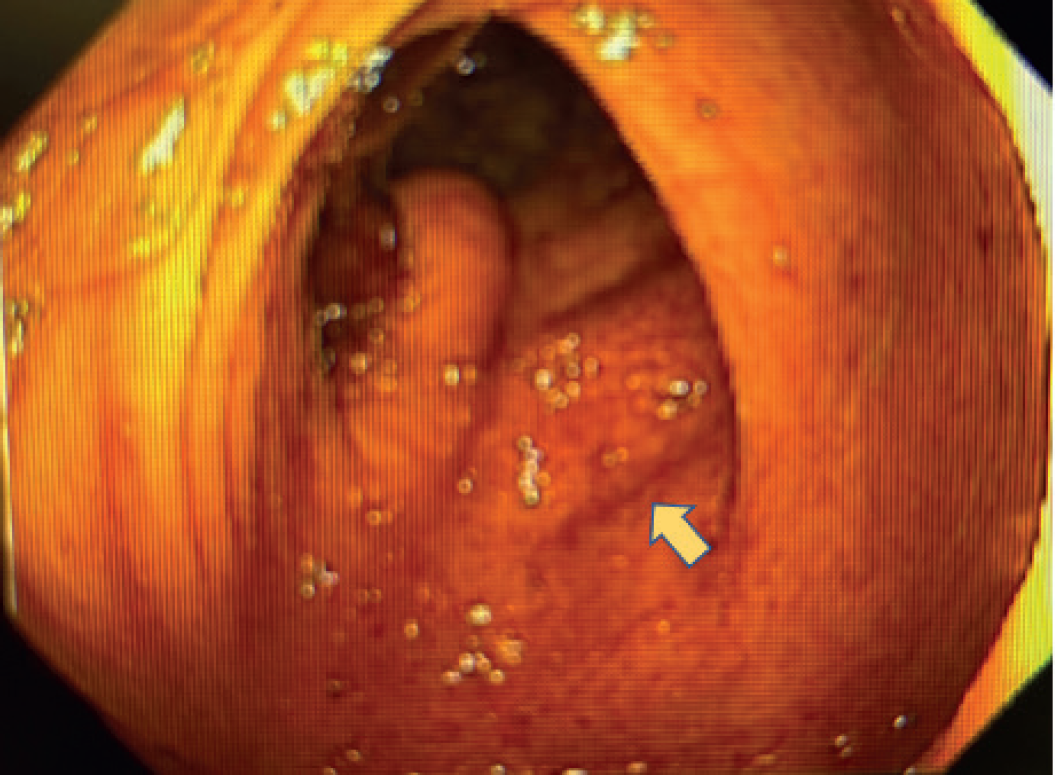
Endoscopic image of a firm submucosal mass (yellow arrow) located adjacent to the ileocecal valve from colonoscopy.
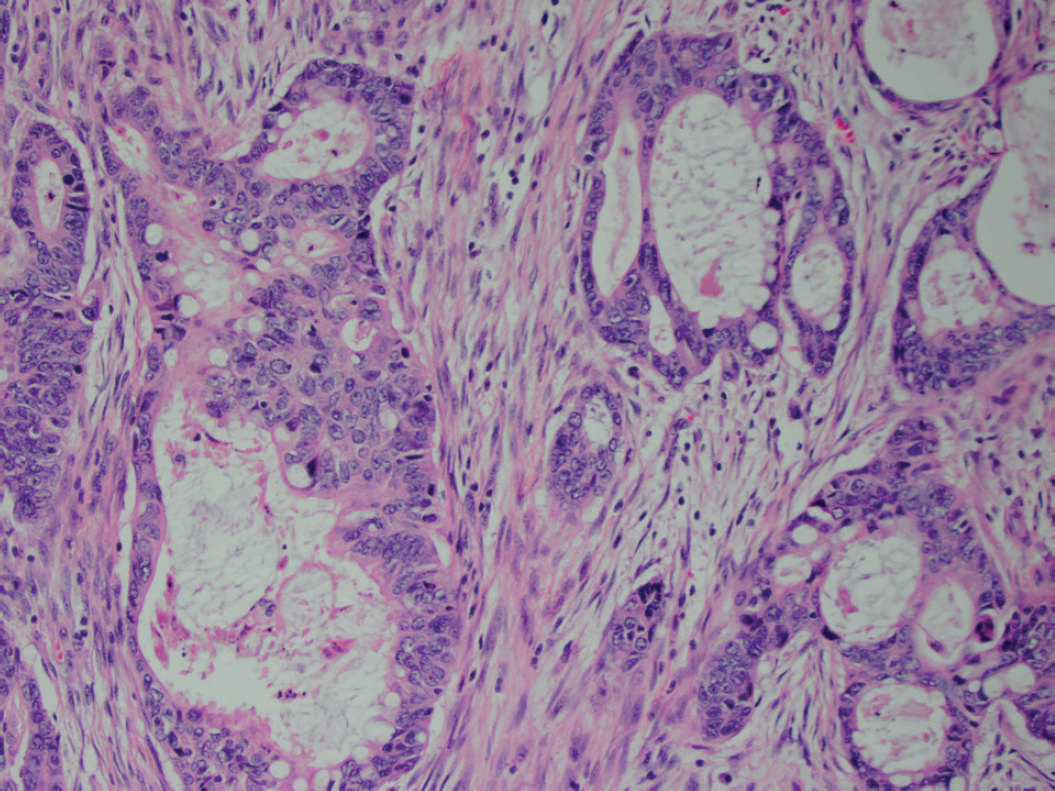
H&E staining of the mass demonstrated a malignant gland-forming neoplasm composed of angulated glands within a desmoplastic stroma. The cells had enlarged, round elongated nuclei with irregular nuclear membranes. These findings are suggestive of moderately differentiated adenocarcinoma (20×).
Given that CD is common in the North America and malignancy can mimic CD presentation, especially when the tumor encircles the bowel and narrows the lumen [5], it is important to distinguish malignancy from CD to guide proper management [7]. If an elderly patient presents with RLQ mass with anorexia, weight loss, and anemia, malignancy should be considered [7]. Radiographic features that favor malignancy include short length (<5 cm), irregular, asymmetric wall thickening (>3 cm), homogenous or mixed attenuation, and absence of perienteric fat stranding [10]. CT findings of perienteric fat stranding, when disproportionally more severe than the degree of wall thickening, can help differentiate CD from malignancy [10]. However, abscess formation, as shown in our patient, is a rare complication of colon cancer that occurs in 0.3%-4% of patients yet is the second most common presentation of perforative lesions [5]. It can present with a CT finding of severe pericolic fat stranding, mimicking CD and leading to diagnostic uncertainty [11]. In this situation, the endoscopic finding of polypoidal or ulcerated proliferative mass with the abnormal glandular pattern on pathology and elevated CEA and CA 19-9 are highly suggestive of a malignancy [7].
Treatment for terminal ileitis should be tailored to its specific etiology; however, terminal ileitis often does not have an obvious cause and 91.2% of cases remain indeterminate despite biopsies [5,12,13]. A study suggested that most patients were treated with antibiotics after diagnosis of terminal ileitis without determination of the exact etiology [14]. Like our case, our patient’s first presentation of terminal ileitis was attributable to NSAID use, despite an unrevealing biopsy in the cecum and terminal ileum, but she later experienced recurrent terminal ileitis with biopsy showing cecal adenocarcinoma with extension into the terminal ileum, a site distinct from her history of tubular adenoma in the ascending colon. It is possible that malignancy caused secondary terminal ileitis in the initial presentation [5]. On the other hand, chronic inflammatory changes could hypothetically lead to dysplasia, ultimately leading to neoplasia in our patient, although it is very unlikely for this advanced malignancy to develop in the span of only 2 years. Regardless of the cause, we recommend close follow-up with repeat colonoscopy with biopsies for symptomatic terminal ileitis of unclear cause [13]. Overall, clinicians should have a high degree of suspicion for malignancy in those patients presenting with terminal ileitis and abscess formation.
Conclusion
The differential diagnosis of terminal ileitis is very broad, mostly encompasses inflammatory, infectious, and rarely malignancy causes. Colon adenocarcinoma presenting as terminal ileitis and abscess formation are rare entities which are estimated to be 2% and 0.3%-4%, respectively. CD is common in the North America and malignancy can mimic CD presentation, especially when tumor encircles the bowel and narrows the lumen, so it is important to distinguish malignancy from CD to guide proper management. Terminal ileitis often does not have an obvious cause and most cases remain indeterminate despite biopsies. Therefore, we recommend close follow-up with repeat colonoscopy with biopsies for symptomatic terminal ileitis of unclear cause. Finally, clinicians should have a high degree of suspicion for malignancy in those patients presenting with terminal ileitis and abscess formation.
What is new?
Colon adenocarcinoma presenting as terminal ileitis and abscess formation are rare entities which are estimated to be 2% and 0.3%-4%, respectively. The CD is common in the North America and malignancy can mimic CD presentation, especially when tumor encircles the bowel and narrows the lumen. Therefore, it is important to distinguish malignancy from CD to guide proper management.


