Background
The superior mesenteric artery syndrome (SMAS), also known as Wilkie’s syndrome (WS), is a rare pathological condition that involves the horizontal part of the duodenum which is compressed between the superior mesenteric artery (SMA) and abdominal aorta, there can be spine involves in the compression in some cases, which leads to the hindrance for the passage of chyme in the duodenum, creating a mechanical obstruction, causes widening and destruction of intestine and stomach. The SMA supplies the horizontal part of the duodenum, jejunum, ileum, pancreas, and two-third of the transverse colon. The causes of developing SMAS are mostly rapid and excessive weight loss, resulting in the loss of the duodenal fat pad [1-7]. The reduction of the fat pad, therefore, leads to the changes in angle between the abdominal aorta and the SMA, or aorto-mesenteric angle and distance, causing intestinal obstruction. The classic symptoms of acute SMAS include postprandial abdominal pain, nausea, and vomiting. It can be congenital or acquired [7, 8].
The literature data on the frequency of occurrence of WS is widely different and is estimated at 0.1%-0.78% in various studies [9-11]. Various authors write that it is detected in 3%-17% of cases among the causes of chronic ileus and in 0.013%-0.30% of cases with radiological studies of the upper gastrointestinal tract [6, 8, 12]. The combination of chronic ileus with stomach ulcer disease is observed in 25%-75%, with a duodenal ulcer in 31%-39%, with a biliary disease of 8.9%-87.4%, and hyperchlorhydria up to 50% [8, 13, 14]. The ratio of women suffering from WS is two times greater than that of men. In up to 75% of cases, the disease is detected in the age group of 10-30 years. However, this syndrome can be seen in older patients. This pathology is not only a rare disease, but also a frequently unfamiliar situation for many surgeons because the patients can develop life-threatening complications that can lead them to death by up to 33% [8, 11, 15].
Case Presentation
Patient G, a 28-year-old man, was admitted to the surgical department of the Bashkir State Medical University clinic on October 11, 2021, with complaints of postprandial abdominal pain in the epigastric region, which was radiating to his lower back, with belching, bloating, and nausea. He complained of difficulty in breathing and periodic pain behind the sternum associated with meals. The patient also noted progressive weight loss and had a history of Osteochondrosis, left-sided scoliosis, no history of smoking or alcohol, and no allergic reactions. The symptoms of WS first appeared in 2018 and afterward worsened day by day.
The results of the inspection during admission: the height of the patient was 173 cm, weight was recorded 60 kg, the body mass index (BMI) 20 kg/m2, and the body temperature was 36.7°C. Heart rate was 74 beats per minute. Blood pressure was 120/75 mmHg. The abdomen was soft during palpation and moderately painful in the epigastric region, and no symptoms of peritoneal irritation were seen. During the auscultation of bowel sounds, the intestinal peristalsis was heard. The kidney punch test was negative. Diuresis was normal.
Diagnosis
Esophagogastroduodenoscopy in dynamics shows hypertrophic and superficial gastritis and gastroduodenal reflux. Therapy was carried out with proton pump inhibitors, after 2 weeks, the signs of aggravation of gastritis went, but the pain persisted. The ultrasound shows increased pneumatization in the intestine. X-ray shows R-signs of gastritis. Echocardiography and Electrocardiography were normal. magnetic resonance imaging of the thoracic vertebra: signs of initial manifestations of degenerative changes in the thoracic spine. Left-sided spondylarthrosis Th4-Th9. The Computed tomography (CT) scan of the abdomen shows a decrease in the aorta-mesenteric angle to 14° (normal 35°-65°) (Figure 1); the distance between these vessels at the origin was 6 mm. (Figure 2a and b). There was a compression of the left renal vein between these vessels: the diameter at the compression level was 0.2-0.3 cm, and the diameter of the veins present more proximally to the origin of the SMA was 1.2 cm. Moderate compression of the lower horizontal part of the duodenum.
These findings show the patient was suffering from SMAS WS with moderate compression of the duodenum and the left renal vein (Nutcracker syndrome).
Course of operation
Laparoscopic Strong operation was performed as it has minimal invasion and with less complications as compared to others, the anastomosis done by laparotomy. As a preoperative preparation, the patient had been given antibiotics for the prevention of postoperative infections, and compression stockings were tied to prevent thromboembolic complications; the compression linen was applied 30 minutes before the operation. A planned operation was carried out under endotracheal anesthesia. Laparocentesis was performed with a paraumbilical trocar of 10 mm. CO2 insufflation was done at 10-12 mmHg. Under visual control, a laparoscope was introduced, as well as two 5 mm and one 10 mm trocars. During the inspection, there was compression of the duodenum by the SMA. The horizontal part of the duodenum was expanded to 5-6 cm below the ligament of Treitz; the diameter of the small intestine was around 2 cm. The procedure of the Strong operation was performed by mobilizing the horizontal part, by dividing the ligament of Treitz, preparing for the imposition of an anastomosis. A mini laparotomy was performed over an anastomosis overlay area, after which the duodenojejunostomy was done and the compressed portion of the duodenum was released. Hemostasis was controlled. A tubular drain was installed in the abdominal cavity; the abdominal wall was stitched layer by layer, and aseptic dressings were applied. The postoperative period was without complications. Symptomatic drug therapy was carried out; everyday dressing of the postoperative wound with antiseptics was performed. Postoperative ultrasound was done to check free fluid and to know if the symptoms were relieved or not, the intestinal loops were expanded or not; the patient noted an improvement in the state and the relief of pain in the epigastrium; there were no complaints about nausea and vomiting. He was discharged after 9 days of hospitalization in satisfactory condition and advised to have an x-ray of the abdomen after a month, as follow-up routine checkup to see if the symptoms would reoccur. During the inspection, there were no complaints of pain or discomfort, and no clinical signs were seen that were present before the operation. After 1 month weight gain was noted up to 61 kg. No anorexia, no signs of postprandial pain, or epigastric tenderness.
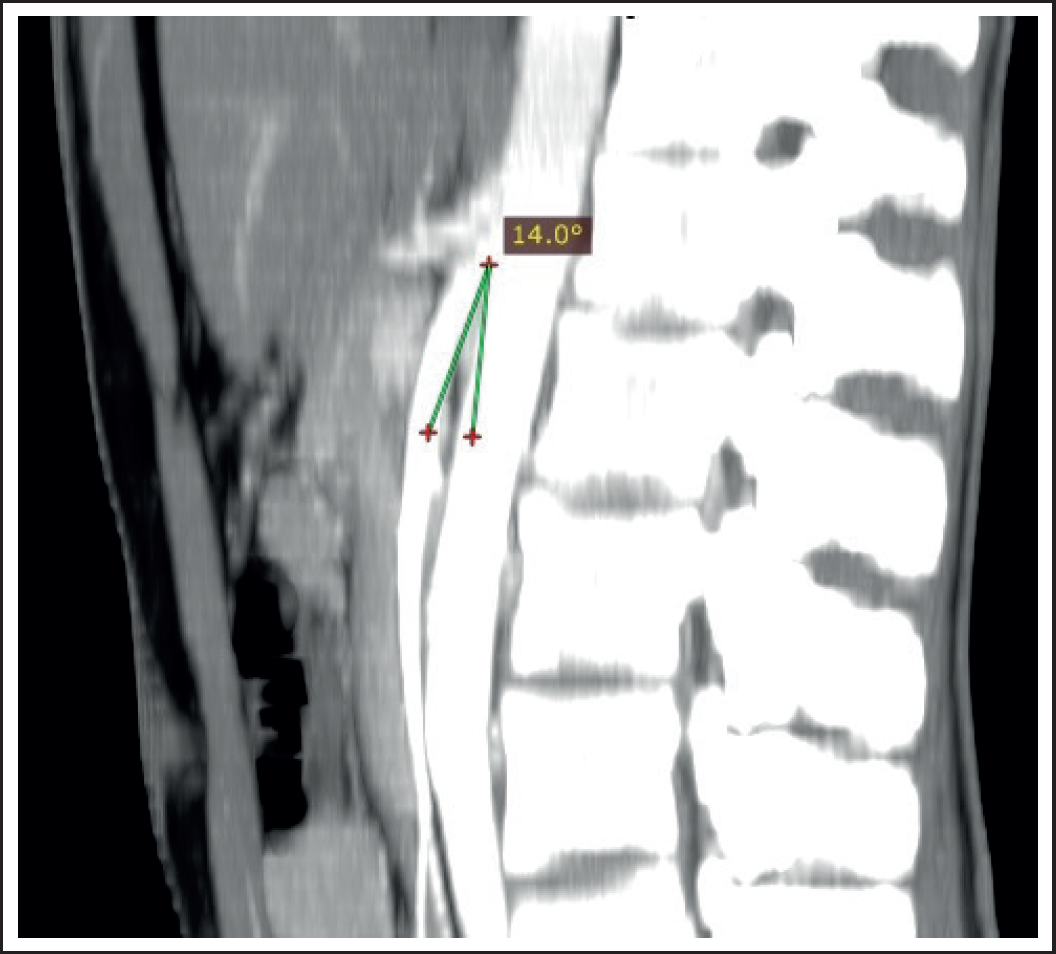
Sagittal section of CT-scan with a contrast of the abdomen (peritoneum and retroperitoneal space) showing a narrowed Aorto-mesenteric angle of 14°.

(a) Axial section of CT-scan with a contrast of the abdomen (peritoneum and retroperitoneal space) showing a narrowed aorto-mesenteric distance of 6.0 mm. (b) Sagittal section of CT-scan with a contrast of the abdomen (peritoneum and retroperitoneal space) showing a narrowed aorto-mesenteric distance of 6.0 mm.
Discussion
This pathology is not only a rare disease, but also a frequently unfamiliar situation for many surgeons because patients can develop life-threatening complications, and also this pathological condition is underdiagnosed, proper and high clinical diagnosis is of utmost importance [1-3]. The decrease in distance and the aorto-mesenteric angle can develop not only duodenal hypertension but also renal vein compression, which leads to renal fornical hemorrhage and varicocele, which can lead to reproductive pathologies [4-6]. It can be hard to diagnose at once, but with proper clinical investigations, the diagnosis can be made as in the case above. The treatment of Strong’s operation is the surgery of choice done for WS to relieve the obstruction huge success rate of up to 90%, this procedure was chosen because the obstruction was huge and couldn’t be managed by conservative treatment, so after the operation there was a reduction in symptoms and pain, and the patient gained weight and increase in BMI by diet change. Conservative therapy or management can be used in acute cases including weight gain, which can be achieved orally or parenterally by focusing the main aim on reconstructing the mesenteric fat pad and increasing the aorto-mesenteric angle. Thus, timely treatment can save the time and life of the patient [3-7]. This case report presents a case of WS followed by Nutcracker syndrome, which gives the medical peer group an open review to treat and diagnose the situation; the diagnosis was done by CT-scan with the combination contrast. The surgical treatment included the Strong’s operation with symptomatic therapy; as a result, the patient gained weight, and no signs and symptoms were seen after 1 month, a follow-up routine checkup for the symptoms of the disease.

