Background
Brucellosis, also known as “undulant fever,” “malta fever,” is a zoonotic disease caused by intracellular bacteria of genus Brucella, with primary hosts as camel, sheep, and goats. Humans are the secondary hosts. It presents as a systemic disease with nonspecific symptoms, such as fever, headache, weight loss, night sweats, and varying musculoskeletal manifestations, such as polyarthralgias, myalgias, sacroiliitis, lumbar spondylitis, spondylodiscitis, and peripheral arthritis. Spinal brucellosis may be seen as a presentation in the elderly; however, diagnosis is difficult as it may mimic other diseases of the spine such as tuberculosis (TB), pyogenic osteomyelitis, and malignancy [1]. The occurrence of an associated psoas abscess in spinal brucellosis is extremely rare [2] and may misguide the clinician to an alternative diagnosis such as TB.
Serological testing, culture of blood, tissue if available, and computed tomography/magnetic resonance imaging help in making an accurate diagnosis. Once diagnosed, treatment must be adequate to control infection and prevent relapse. Antibiotic regimens including doxycycline and rifampicin for 3-6 months with an initial combination with an aminoglycoside such as gentamycin or streptomy-cin for 3 weeks are recommended [3].
The following case points out the importance of considering brucellosis as a plausible diagnosis even in the occurrence of a psoas abscess given the relevant occupational history in an endemic setting.
Case Presentation
A 57-year-old gentleman, presented with history of intermittent fever with chills for 1 month, lower abdominal discomfort and lower back ache for 1 week. On examination, he had diffuse tenderness over the lower abdomen, along with point tenderness at the level of L1-L2 lumbar spine with normal neuromotor examination.
Laboratory investigations showed normal hemogram except for thrombocytopenia (platelet count - 80,000/ mm3), mild transaminitis [Alanine aminotransferase - 32 U/l, aspartate aminotransferase - 116 U/l) with raised alkaline phosphatase (900 U/l) and gamma glutamyl transpeptidase (140 U/l). Mantoux test was negative. Blood cultures showed no bacterial growth.
In view of the spine tenderness, an magnetic resonance imaging (MRI) of the dorsolumbar spine was done and Coronal short tau inversion recovery (STIR) image (Figure 1) showed hyperintensity at L1 and L2 vertebral bodies and intervening disc consistent with spondylodiscitis and associated large left psoas abscess (Figures 1 and 2). Mild hepato-splenomegaly was also evident. Given these MRI findings and the high incidence and prevalence of TB in India, it was the first considered differential diagnosis.
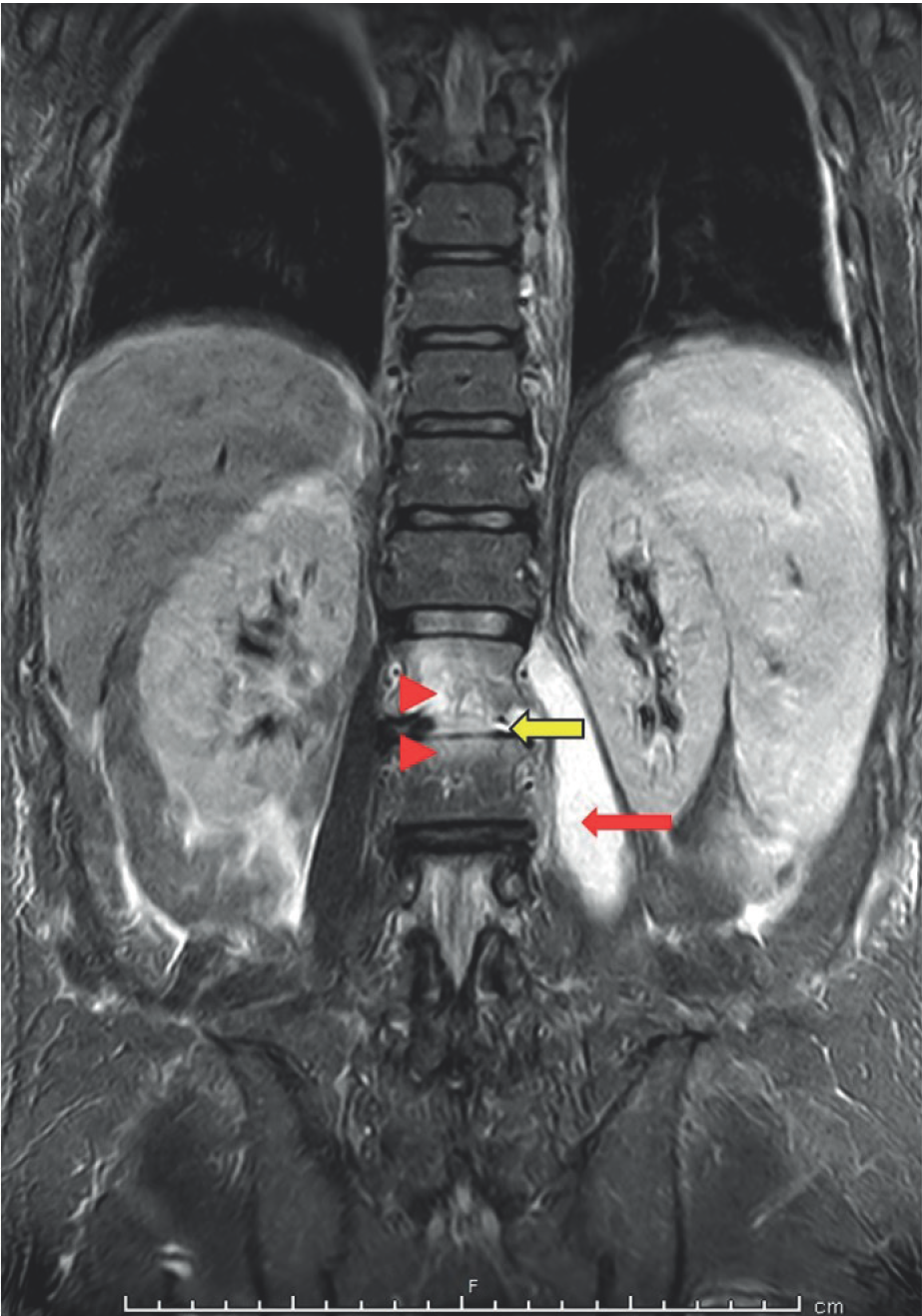
MRI dorsolumbar sine - Coronal STIR image: hyperintensity at L1 and L2 vertebal bodies (red arrowheads) including the intervening disc (yellow arrow) and associated large left sided psoas abscess (red arrow).
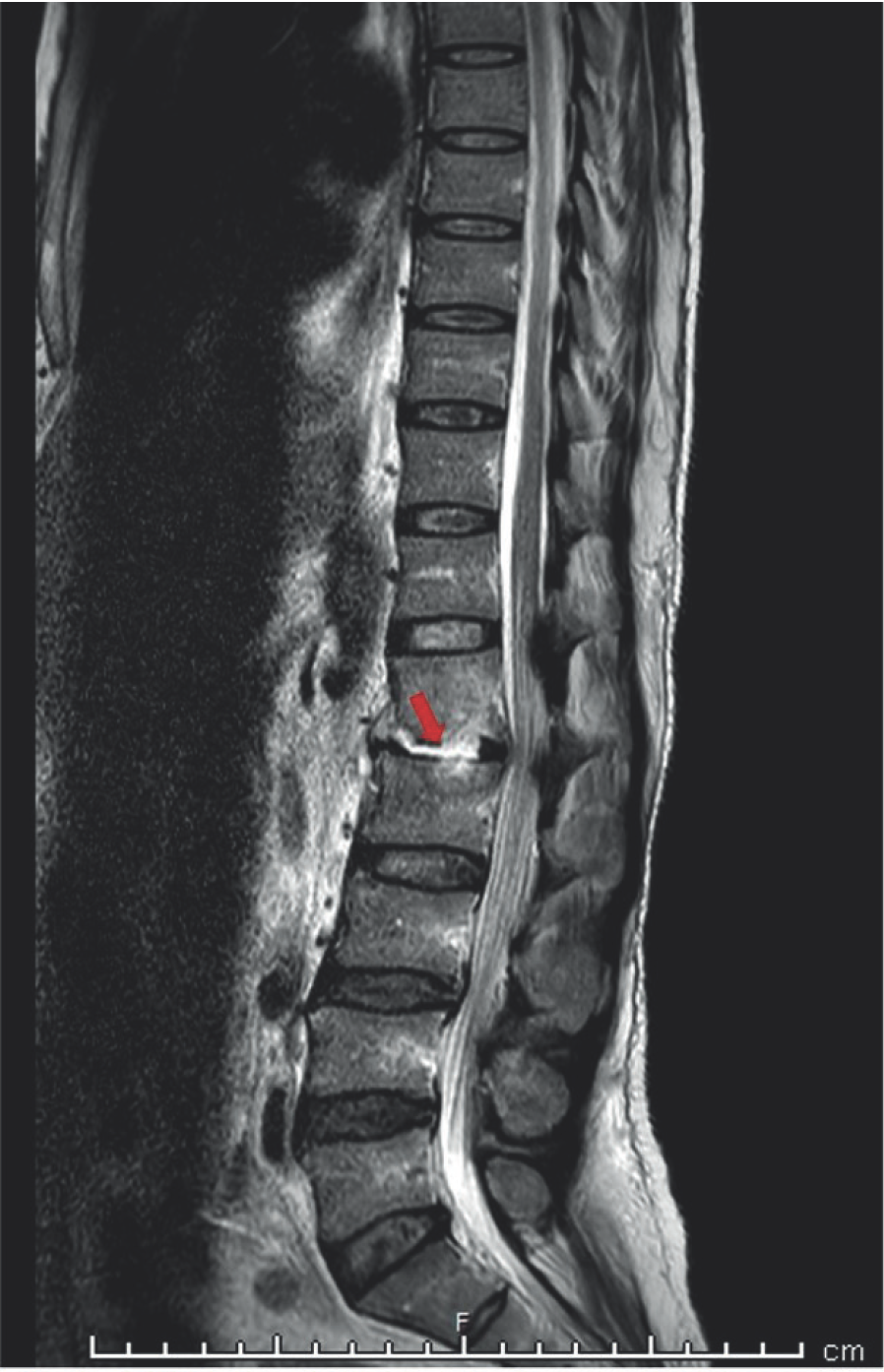
MRI dorsolumbar spine - Saggital T2w image: hyper-intensity in intervening disc between L1 and L2 vertebrae (red arrow).
The abscess fluid was drained under ultrasound guidance and it was sent for evaluation. Acid fast bacillus (AFB) staining, cartridge based nucleic acid amplification test, AFB cultures were negative. Bacterial culture of the fluid showed growth of Brucella melitensis after 3 days of incubation. Brucella agglutinin titres sent thereafter were elevated (1:320).
A careful review of history revealed that the patient, a paddy farmer occupation, had significant contact with goats during his daily work on the farm, suggesting the likely source of transmission of disease.
This patient was then started on Rifampicin (600 mg/ day), doxycycline (200 mg/day), and gentamicin (5 mg/kg/ day, advised for 3 weeks), following which he improved clinically. He was discharged after fever subsided and he felt symptomatically better, and was advised to be in close follow up.
Discussion
Brucellosis is a zoonotic disease usually acquired by consumption of unpasteurized dairy products, or close contact with infected animals (camel, sheep, and goats). It is caused by gram negative, intracellular coccobacilli of the genus Brucella, including B. melitensis, Brucella abortus, Brucella suis, Brucella canis, and Brucella ovis [4].
Brucellosis affects multiple organ systems. After entry into the body, the bacteria undergo hematogenous dissemination to the reticulo-endothelial system, rich in mononuclear phagocytes, like the liver, spleen, lymph nodes, and bone marrow [3]. From there, the microorganisms reach the spine by antegrade flow through the nutrient arterioles of the vertebral bodies, or by retrograde flow through the Batson’s venous plexus [1].
There is an incubation period of 1-3 weeks. Brucellosis clinically presents with fever, malaise, night sweats, weight loss, polyarthralgias, and myalgias. Osteoarticular involvement is commonly known in the form of sacro-iliitis, lumbar spondylitis, spondylodiscitis, and peripheral arthritis. In children and young adults, sacroiliac and knee joint involvement is more commonly seen. Spinal involvement is seen in 2%-65% of the cases [1,5], more so in elderly population in endemic areas. It can be focal, confined to the anterior portion of the endplate, or, diffuse, involving the entire vertebral body and adjacent disc, vertebrae, and epidural space [3,6]. Infrequently, extension of the inflammatory process to the epidural space, leads to neurological complications in the form of myelitis, radiculopathy, demyelinating neurpathies [7].
Laboratory investigations may show anemia, thrombocytopenia (as seen in this case), mild elevations of the liver enzymes, elevated eruthrocyte sedimentation rate. These findings are, however, not specific. Standard tube agglutination titres of >1:160 in those with history of animal contact are taken to be positive. Definitive diagnosis is made by isolation of the organism in blood, cerebrospinal fluid, bone marrow, or abscess fluid/pus. Blood cultures may not always give yield because of intermittent bacteremia and probable use of previous antibiotics.
MRI is currently the best modality for assessment of spinal disease. It shows low to intermediate signal intensity of the vertebral bodies and disc, on T1 weighted image and hyperintensity on STIR and T2 weighted images as seen in this case. In 18% of cases, there may appear a small amount of air, entrapped in between the disc and affected superior endplate of the vertebral body, referred to as “peripheral vacuum phenomenon” [8]. Paravertebral abscesses, present in up to 16%-30% cases are also delineated on MRI [1,2,9]. Bone scintigraphy, if done, helps in identifying all the sites of osteoarticular involvement.
The diagnosis of spinal brucellosis, however, is difficult as it may mimic other diseases of the spine such as TB, pyogenic spondylitis, spinal metastasis, plasmacytoma, and actinomycosis. Tubercular spondylitis must always be ruled out. Even with spinal involvement, the occurrence of a psoas abscess, as seen in this case, is rare in brucellosis, unlike in TB. A review by Turgut et al. [4], based in Turkey, endemic to Brucellosis, found the occurrence of a psoas abscess in only 1.2% of cases of spinal brucellosis. TB usually affects the mid thoracic spine as opposed to lower lumbar spine in brucellosis. Tubercular spondylitis also causes extensive vertebral body destruction with collapse and deformity with much larger paraspinal/ psoas abscess formation [1,7].
Treatment of spinal brucellosis requires a least a 6-week course of antibiotics - Rifampicin, Doxycycline, an aminoglycoside may be added for the initial 2-3 weeks, but there are no guidelines for the same [10,11]. Therapeutic failures are known, and in these cases, may require an extended regimen of antibiotics up to 6 months. Surgical intervention is required in cases of cord compression, or vertebral collapse.
Conclusion
Brucellosis has a varied clinical presentation. Spinal involvement often deviates the mind of the clinician towards other differential diagnoses, such as TB, more so, in the presence of a psoas abscess as seen in the above case. History of contact with animals, nonspecific presentation, endemicity, positive serological tests and cultures, with correlating MRI findings help to clinch the diagnosis. The treatment is often prolonged, but when diagnosed early, will change the clinical course of the patient.
What is new?
Brucellosis is a zoonotic infection, commonly presenting with osteoarticular involvement. Spinal brucellosis occurs in up to 65% of affected cases, but the occurrence of a psoas abscess is rare. One Turkish study gave an incidence of psoas abscess as 1.2% cases of spinal brucellosis, still very low, given it is endemic to the disease. This presentation with a psoas abscess as seen in this case report may mislead the clinician to an alternative diagnosis such as TB.

