Background
Periosteal reaction occurs in response to any insult to the cortical bone showing abnormal increased uptake on bone scan (BS). It can appear in various patterns depending on the type, severity, and duration of insult [1]. It is seen as a periosteal elevation from the cortex [2]. It is more common and aggressive in children as the periosteum is loosely adherent to cortical bone in pediatric age group [3]. The periosteal reaction in children can result from physiological periostitis (PP), infection, trauma, prosta-glandins administration, infantile cortical hyperostosis (ICH), hyper-vitaminosis A and D, and scurvy [4]. The PP is a periosteal reaction without any inflammatory conditions. It symmetrically involves long bones. However, it can present asymmetrically at times, hence it can easily be misinterpreted for a pathological process [5]. Prompt differentiation is important as PP is a self-limiting process without any active management. Different imaging modalities are used for diagnosis of PP, e.g., plain radiographs, computerized tomography, and magnetic resonance imaging. A 99mTc-methylene diphosphonate (MDP) BS demonstrates increased radiotracer accumulation in areas of increased bone metabolism. It has high sensitivity to delineate any such area [6]. We report a case in which PP presented with features and simulations of osteomyelitis on 99mTc-MDP bone scintigraphy.
Case Report
A 1-month-old male child was referred to the nuclear medicine department for bone scintigraphy with a history of swelling in the right hip joint for 2 weeks. The referring physician was suspecting infective process involving right hip joint. The guardian of the patient gave a history of swelling and reduced right leg movement along with irritability of the child. There was no history of fever or trauma. On examination, there was mild swelling and mild discoloration of the skin in the right proximal thigh with restricted extension. His complete blood counts, erythrocyte sedimentation rate, and C-reactive protein were within normal limits. A 99mTc-MDP three-phase BS was carried out with Infinia dual-head gamma camera equipped with low-energy high-resolution collimators at 140Kev peak with a 20% energy window. It showed abnormal increased perfusion with pool activity in region of right proximal femur (Figure 1). Delayed phase showed increased radiotracer uptake in proximal and distal ends of right femur along with increased uptake in proximal right humerus (Figure 2). Correlative X-ray images of right femur and humerus showed periosteal reaction at diaphyseal ends of respective long bones (Figure 3). Keeping in view the normal biochemical profile of the child, a detailed history of no evidence of antibiotics, vitamins, or other treatment was present. The case was also discussed with the referring physician and local radiologist, but no clue of any infective pathology could be elucidated. Keeping in view the clinical and radiological findings, PP was suspected. The patient was given symptomatic treatment i.e., non-steroidal anti-inflammatory drugs (NSAIDs) by the treating physician and improvement in patient’s condition was observed, subsequently confirming our diagnosis.
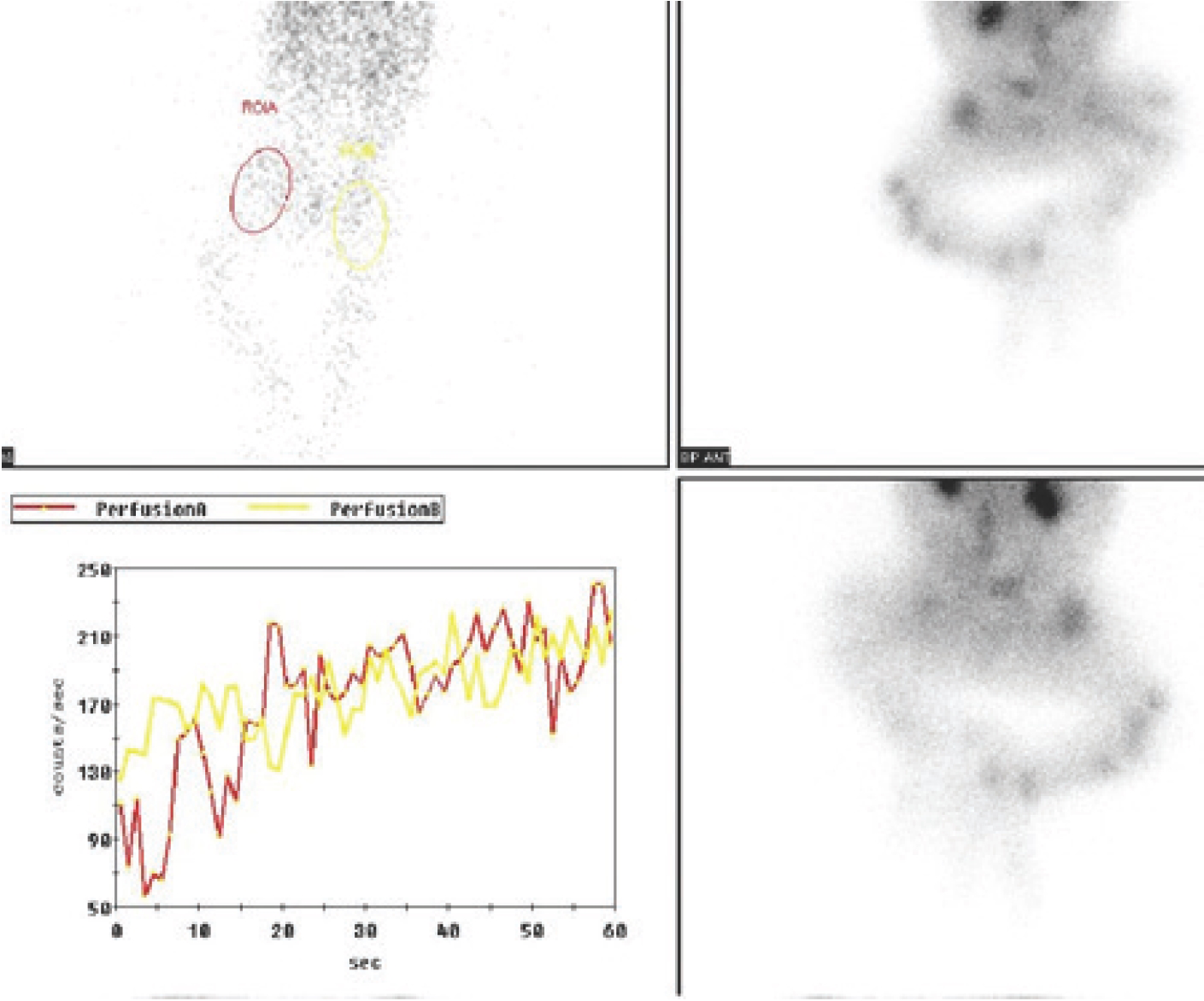
99mTc-MDP bone scintigraphy (early dynamic sum images) focused on pelvis/femoral regions showing increased perfusion and blood pool activity in the proximal right femur.
Discussion
PP is a periosteal reaction without any inflammatory condition and a well-documented pediatric radiological finding. It can present in infants up to 6 months of age with majority of cases reporting between 1 and 4 months of age with no gender preponderance [5]. The exact incidence and etiology are unclear. The loosely adherent periosteum and rapid bony growth in children may be the reasons for this finding. It is usually bilateral and symmetrical in distribution. It commonly involves the long bones, mostly femur and tibia. Occasionally, it may be asymmetrical and more prominent on one side, leading to diagnostic dilemma. It has been observed that if on first examination only one bone is involved then uninvolved ones may become evident in subsequent examination [7]. It can be suspected in case of normal physical examination and laboratory investigations as the condition is benign and self-limiting. Accurate diagnosis of this condition will eliminate the need for further rigorous testing and management of the child. BS is a sensitive tool to point out any focus of increased osteoblastic activity. It can augment the clinical suspicion to reach the diagnosis in most of the cases [8]. In this case, however, its finding was misleading. A unilateral periosteal reaction may lead to misdiagnosis of child abuse or infection [9]. The periosteal reaction due to trauma can be bilateral and multiple, but usually there is evidence of fracture and hematoma. Additionally appearance of new bone will be irregular so it can help in excluding the child abuse [10]. The osteomyelitis of bone will not involve multiple bones symmetrically, also presenting symptoms and laboratory investigations can help in excluding this common cause [11]. ICH occurs in same age group, but it is usually genetic and most commonly involves flat bones with involvement of mandible in 75%80% of the cases, which may cause failure to thrive due to difficulty in eating [12,13]. PP, on the other hand, is a benign finding involving children of 1-6 months of age. It can be suspected in case of normal biochemical investigations and radiological finding of periosteal reaction involving diaphysis of multiple long bones. The condition is self-limiting, needs no surgical or aggressive pharmacological treatment, and has excellent prognosis [5]. Therefore, it is important that the knowledge of this condition should be kept in mind before subjecting the child to long and laborious procedures and treatments.



