Background
Idiopathic Atrophoderma of Pasini and Pierini (IAPP) is a rare dermatological disease with histopathological and epidemiological differences from morphea and linear atrophoderma of Moulin. Although Morphea has been rarely described to have extra-cutaneous manifestations, IAPP is a disease limited to the dermis. This case report presents a 14-year-old African-American male with congenital IAPP and systemic vascular aneurysms.
Case Presentation
A 14-year-old African-American male with a significant past medical history for IAPP presented with 1 day of abdominal pain.
The pain was located in the right lower quadrant, specifically over the area of the rash, and was described as “bruise-like” in character. The patient described the pain as constant, with an intensity of “8 out of 10”, radiating linearly over the skin from the right lower quadrant to the right back. The pain would increase with the movement of his right arm and leg and was relieved only by lying still in bed. No over-the-counter medication was tried at home before presentation.
On review of systems, the patient reported a 12-pound weight loss in the last month due to decreased appetite. He denied night sweats and fevers. His mother noted that the rash appeared more sunken. The patient did not report of any headaches, throat pain, nausea, episodes of vomiting, diarrhea, or constipation. The patient had a prior workup done to rule out systemic sclerosis at the age of 8 years. This workup included serum testing for Scl-70 antibody, IgA and celiac panel, and negative biopsies from esophagogastroduodenoscopy and colonoscopy. Additionally, multiple abdominal ultrasounds were obtained to rule out fibrotic changes in the internal organs, such as that of spleen and liver.
His physical examination showed normal vital signs for his age. He was on the 90th percentile for weight and had a body mass index of 27.24 kg/m2. He was in mild distress due to his abdominal pain. The area of pain was along with the distribution of rash shown (Figure 1). There was no guarding or rebound tenderness. There was no hepatosplenomegaly. Other signs of appendicitis, such as Rovsing’s sign, Psoas sign, and Obturator sign, were negative. Testicles were normal bilaterally. The rest of his examination was unremarkable other than his skin rash.
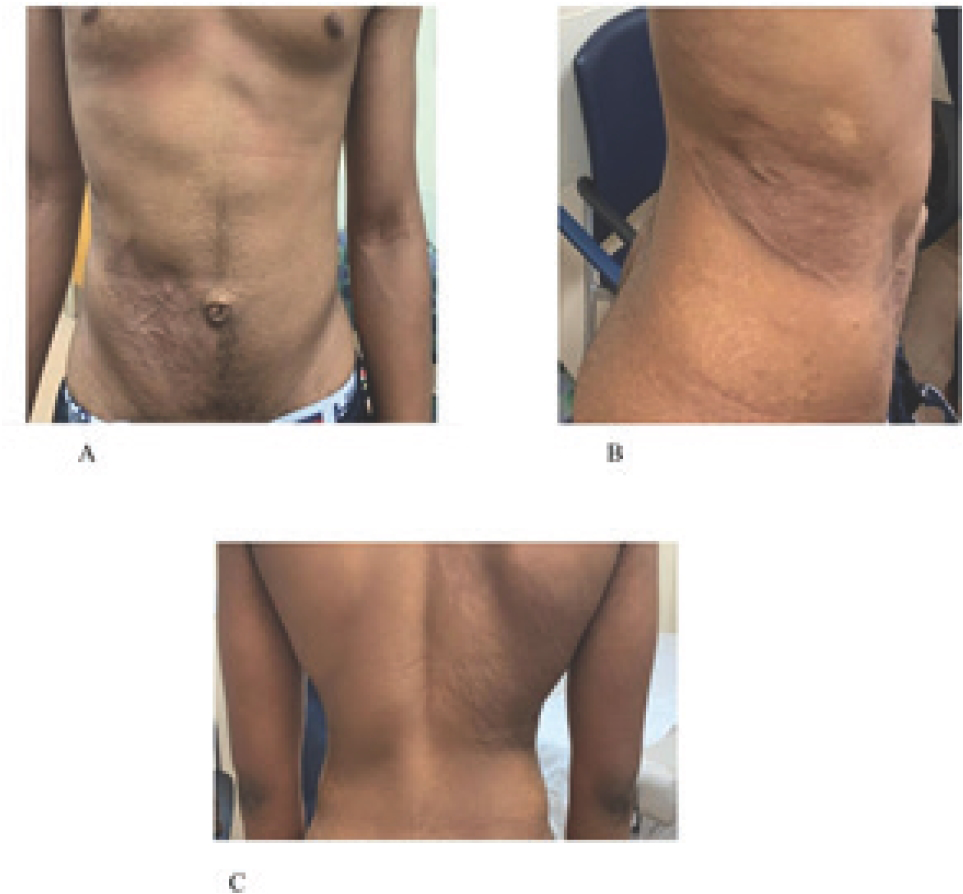
(A) Abdominal right lower quadrant rash. (B) Extension of rash into the right flank and (C). Right back.
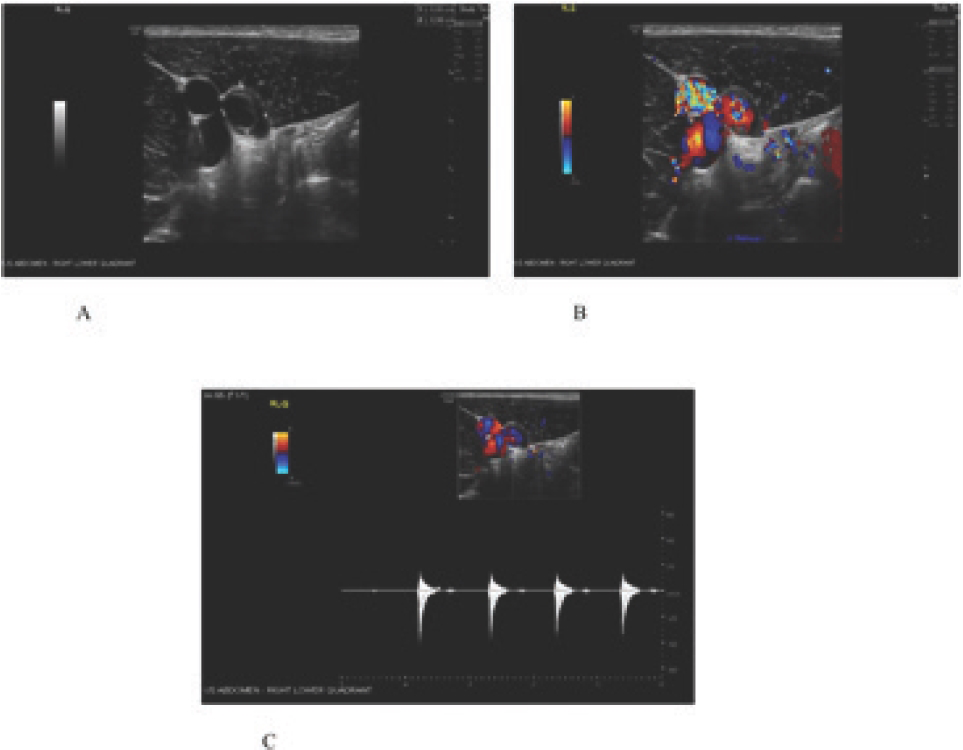
Ultrasound of the right lower quadrant region. (A) 1 × 1 cm thick-walled vascular structure appearing to communicate with the medial aspect of the right external iliac artery through a narrow neck (B) and (C) irregular flow with arterial spectral waveform, concerning pseudoaneurysm.
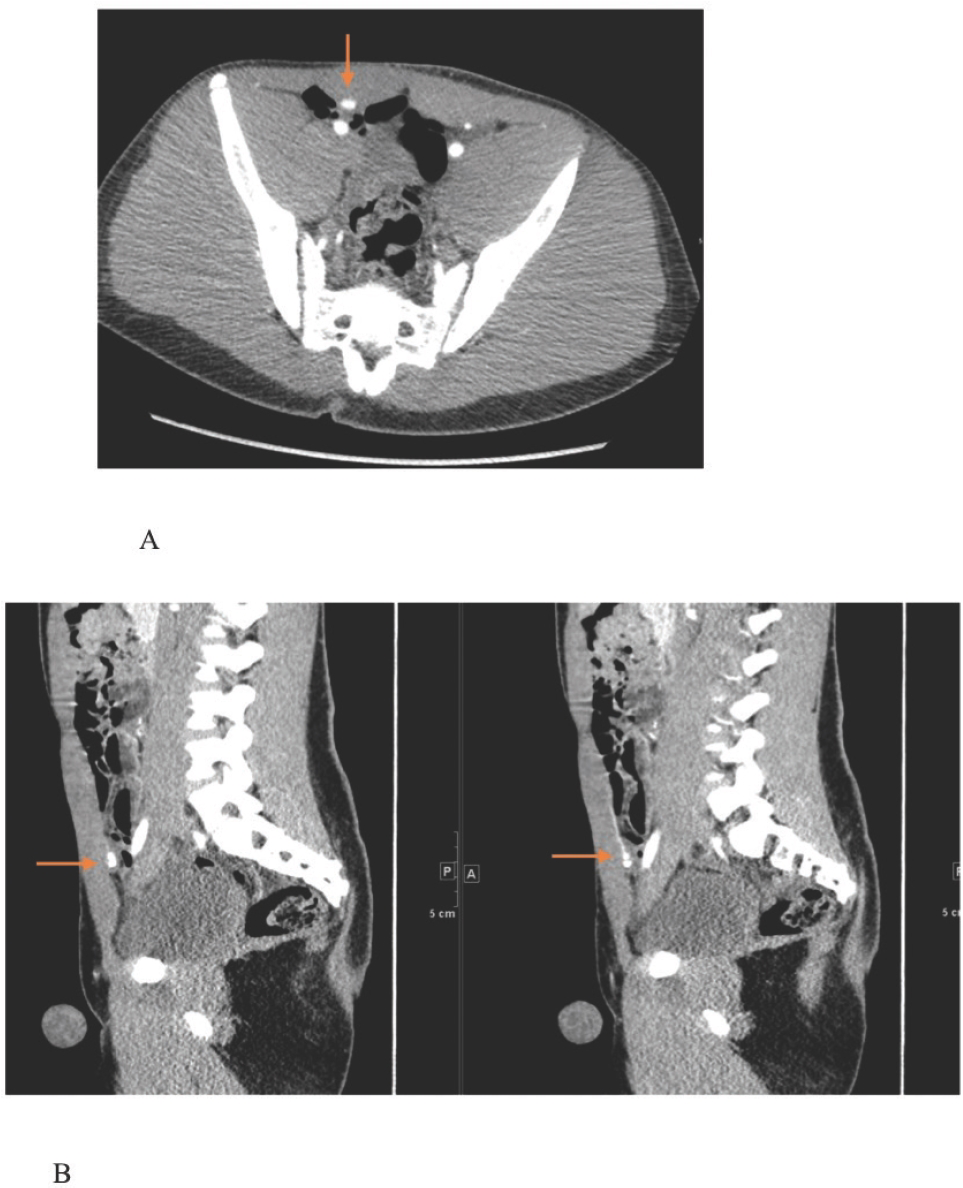
CT angiogram of the abdomen and pelvis. Small multilobulated outpouching of contrast arising from the medial aspect of the right inferior epigastric artery, which measures approximately 1 × 0.9 cm transverse × 0.8 cm AP, and likely represents a pseudoaneurysm, with possible internal areas of clot. (A) Cross-sectional view (B) Transverse plane.
His pain was assessed to be secondary to worsening IAPP in the emergency department. However, given the location of the pain, acute appendicitis was ruled out by obtaining a right lower quadrant ultrasound. The ultrasound showed a 1 × 1 cm thick-walled vascular structure that appeared to communicate with the medial aspect of the right external iliac artery. There was irregular arterial flow (Figure 2). Consequently, a computed tomography angiography of the abdomen and pelvis (CTAP) was carried out to rule out multiple aneurysms. CTAP revealed a small aneurysm of the right inferior epigastric artery (Figure 3).
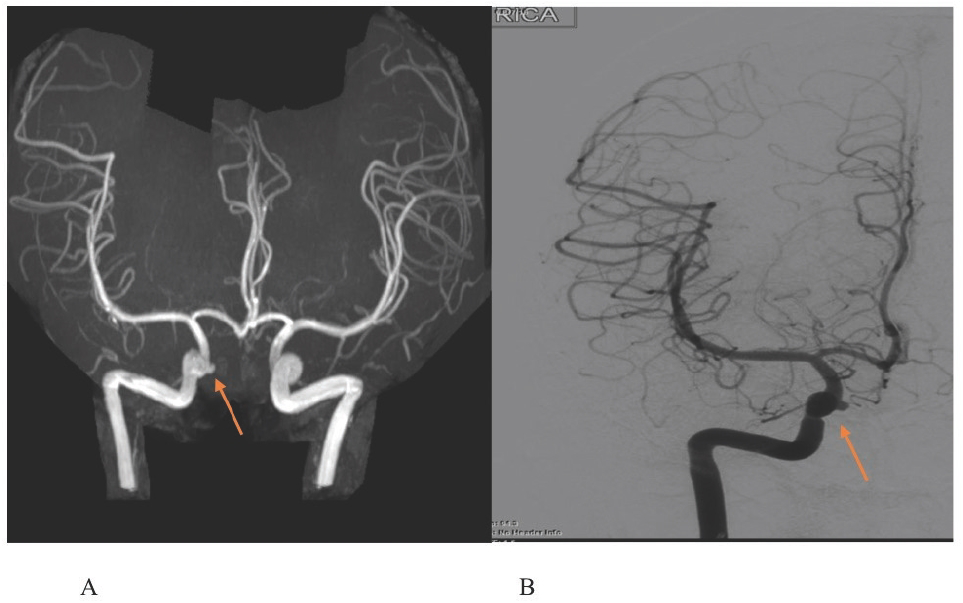
(A) MRA of the head showing 5 mm right superior hypophyseal aneurysm pointing medially (B) Neuro-interventional study defining the dimensions of the aneurysm as 2.43 × 3 mm at the level of the ophthalmic artery pointing medially with a superior hypophyseal segment. The origins of the right internal and external carotid arteries were patent without evidence of ulceration or stenosis.
The patient underwent interventional radiographyguided embolization of the inferior epigastric artery during his inpatient stay. Further workup included lab testing and imaging. Complete blood count, electrolytes, autoimmune workup, and Lyme titers were all within normal limits. Imaging included an echocardiogram, magnetic resonance angiography (MRA) of the head, MRA of the chest, and renal ultrasound with doppler. On his echocardiogram, the patient was found to have a mildly dilated aortic root with trivial aortic regurgitation, while his MRA head revealed a small <5 mm right superior hypophyseal aneurysm (Figure 4A). No aneurysms of the chest cavity or in the renal system were found. Neuro-interventional radiology was further employed to define the cerebral aneurysm (Figure 4B). An ophthalmology exam was negative for uveitis and vasculitis.
Currently, the patient is being followed-up as an outpatient by rheumatology. A trial of topical mometasone, tacrolimus, and calcipotriene has not shown any improvement. The patient is due for a trial of IM methotrexate weekly.
Discussion
IAPP is a rare cutaneous dermatological condition with an unknown etiology and less than 100 cases described in the medical literature. Congenital IAPP is rare but reported [1]. It presents commonly in females, with a male:female ratio of 1:6. These lesions can cause pain, paresthesia, or pruritis.
Some authors consider IAPP on the spectrum of localized scleroderma [1], while others consider it altogether a different entity [2]. Histopathology of IAPP differs from morphea (also known as local scleroderma). IAPP lacks inflammation, has dermal thinning, unaltered appendageal structures, and low disaccharide content (DeltaDi-4S) per skin biopsy. On the other hand, morphea has histopathological features of epidermal atrophy “with” inflammation, alteration in sweat glands, and pilosebaceous glands and increased content of DeltaDi-4S on skin biopsy.
Another entity called “linear atrophoderma of Moulin” (LAM) can present with similar dermatologic findings to IAPP. Lack of inflammation is found in both lesions. However, LAM classically presents earlier in life (between 6 and 20 years of age) and has a unilateral distribution following Blashko’s lines, whereas IAPP presents between ages 20 and 40 years and does not routinely follow Blashko’s lines [2]. In a study comparing multiple modalities of treatments for IAPP, none or minimal improvement was found. These treatments included topical and systemic steroids, oral doxycycline, and oral hydroxychloroquine. One study reported some improvement with Q-switched alexandrite laser, 755 nm at 6-week intervals [2]. Our patient has shown a treatment response similar to patients previously described in the literature. Both IAPP and LAM lack organ involvement. Morphea, however, has been rarely described to involve extracutaneous tissues, but no reports of aneurysms have been found [3].
Conclusion
To our knowledge, this is the first case report describing deep artery aneurysms in a pediatric patient with a dermatological lesion assessed to be IAPP by histopathology; thin collagen bundles arranged parallel to the skin surface throughout the dermis. More longitudinal studies are needed for patients with IAPP to determine if patients with congenital IAPP inherit a risk of developing arterial aneurysms later in life.

