Background
The coronary lesions without signs of severe calcification are usually treated with direct stent implantation. Postdilatation is performed by some operators routinely and the others prefer to postdilate the stent only in case of underexpansion. However, the inability to expand the stent to its nominal diameter is a situation that can be encountered by every operator, especially if predilatation is not accurately performed. Underexpansion of the stents poses a high risk of stent thrombosis and restenosis in the long term. Postdilatation of the stent with a non-compliant (NC) balloon is generally the first maneuver. On the other hand, “what to do next?” is a question that does not have a clear answer as yet. We herein represent the use of a low-speed rotablation in the management of an underexpanded stent.
Case Presentation
A 68-year-old male complaining about shortness of breath was examined in the outpatient clinic. He was a current smoker and underwent treatment for hypertension. He also had a strong family history. Myocardial perfusion scintigraphy revealed ischemia in the inferoposterior region and the patient underwent coronary angiography. Left coronary arteries were normal, but there was a visually severe lesion in the crux of the right coronary artery (RCA) (Figure 1A and B). The fractional flow reserve value was measured to be 0.77 and the procedure proceeded with an implantation of a stent. As the lesion did not seem to be heavily calcified, direct stent implantation was performed without balloon predilatation. The procedure was completed by kissing balloon inflation with 3.0 and 2.5 mm balloons at 16 atm after implantation of a 3.5 × 23 mm drug-eluting stent at 16 atm (Figure 1C and D). Postdilatation was performed with a 3.5 × 8 mm NC balloon at 16 atm and the final appearance was satisfactory (Figure 1E and F). After 9 months, the patient defined same anginal symptoms and the exercise stress testing was positive. Coronary angiography showed restenosis, especially in the underexpanded segment of the stent (Figure 2A). In the intravascular ultrasound (IVUS, Galaxy 2 + Atlantis 40 MHz catheter), the strut-to-strut diameter of the stent in the underexpanded region was measured to be 1.6 mm and was likely to be responsible for restenosis (Figure 2B). High-pressure balloon inflation up to 26 atm was performed many times (Figure 2C-F). Then, a cutting balloon (3.5 × 10 mm) was advanced but failed to cross the lesion. Meanwhile, a dissection occurred in the proximal RCA resulting in no reflow and ST-elevation and then managed with bail-out stenting (Figure 2G and H). The procedure was completed with 3.0 and 3.5 mm kissing balloon inflation at 22 atm (Figure 2I and J). After 4 months following the second procedure, the patient presented with the same symptoms and scintigraphy was again positive in the inferoposterior region. Coronary angiography again revealed restenosis in the same region which was accepted to be underexpanded in the previous angiographies (Figure 3A and B). Balloon inflation again was not a promising therapeutic option in this case since the patient had been exposed to restenosis twice in a short while following intervention. A 1.75 mm rotablator was used cautiously under low speed (150,000 rpm) to ablate the stent struts which prevented adequate expansion and lead to repeating restenosis (Figure 3C). The postdilatation was still not easy but successful this time (Figure 3D). As the flow in the posterior descending artery was thought to be compromised, a 13 × 3.5 mm Drug Eluting Stent (DES) was implanted and the procedure was completed with a final kissing (Figure 3E-H). The patient is free of the symptoms since then.
Discussion
In heavily calcified lesions, almost all operators perform predilatation to provide an adequate expansion area for the subsequent stent. On the other hand, some lesions which are accepted to be non-calcified at the first look are treated with direct stenting. The expansion of the stent can be complicated in such situations. When the hard plaque is covered by underexpanded stent struts, it generally becomes more challenging to have optimal dilatation when compared to predilating a non-stented hard plaque. Postdilatation with NC balloons inflated at maximum recommended pressures (20-30 atm) is applied by all operators in the first step. If this fails, the second step includes very limited options. In the recent years, dedicated super high-pressure NC balloons (OPN NC®; SIS Medical AG, Winterthur, Switzerland), which can be inflated up to 40 atm, were introduced and found to provide an effective and safe alternative strategy when classical NC balloons fail [1,2]. However, these dedicated balloons are not readily available in most laboratories. Actually, rotational atherectomy is often used to reduce plaque rigidity and facilitate dilatation before stent implantation, when aggressive predilatation fails to fully dilate the calcified lesion. However, a few recent case reports presented that rotablation was useful in ablation of underexpanded stent struts and these reports have presented successful overall destruction of the metalic stent components by using imaging modalities such as IVUS or optic coherence tomography [3,4]. The major concern about rotablation when ablating a stent is entrapment and development of slow flow [5]. Fortunately, we did not encounter with such complications in our case just like the other few cases reported [6-8]. Beginning with a small burr size, as well as a low speed, may avoid development of complications.
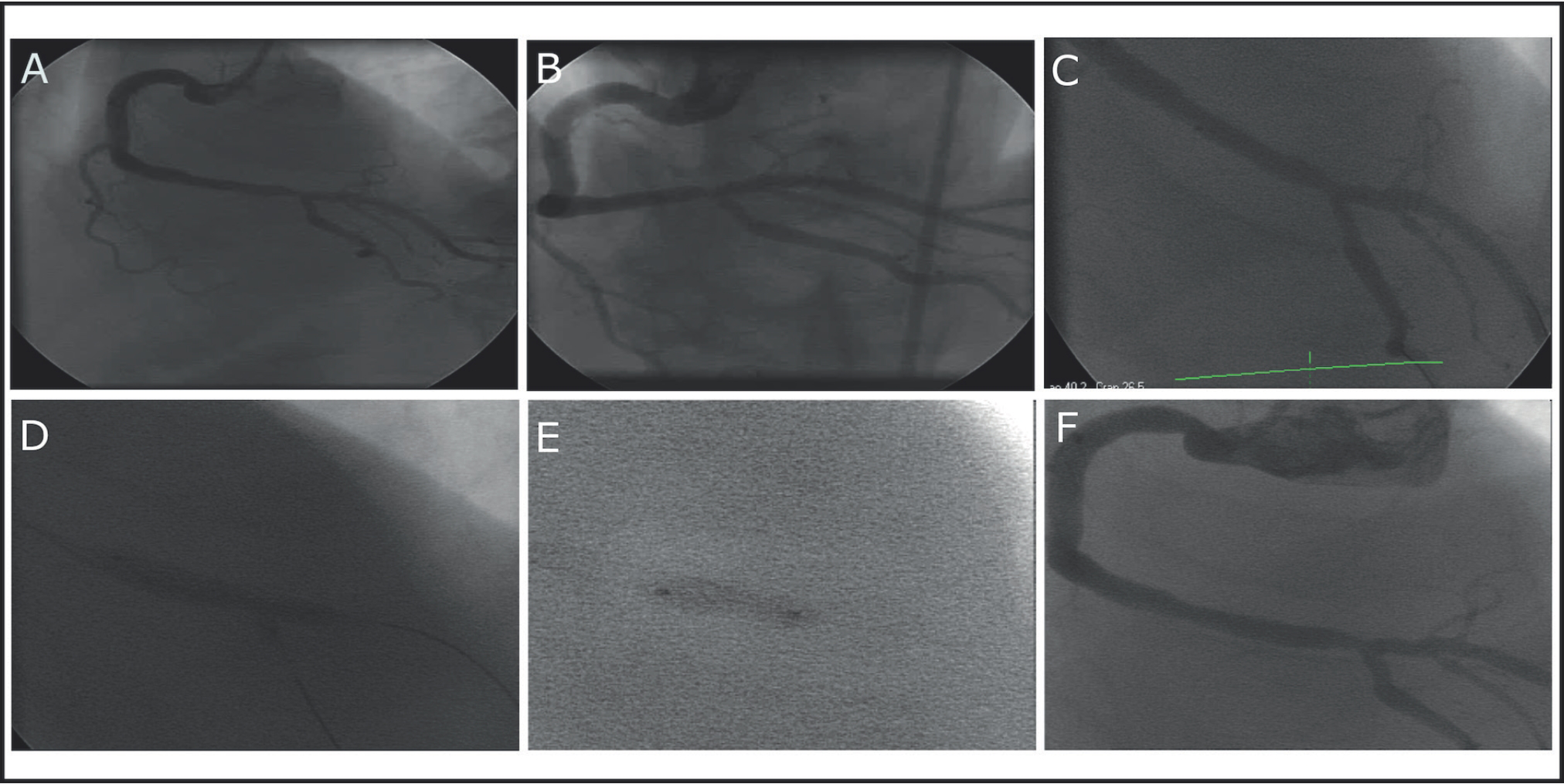
Direct stenting was performed in the crux with subsequent postdilatation. (A,B) Severe lesion in the crux; (C) 3.5 × 23 mm DES; (D) kissing with 3 + 2.5 balloons; (E) postdilatation by 3.5 × 8 mm Powersail balloon at 24 atm; and (F) final appearance at the end of the first procedure.
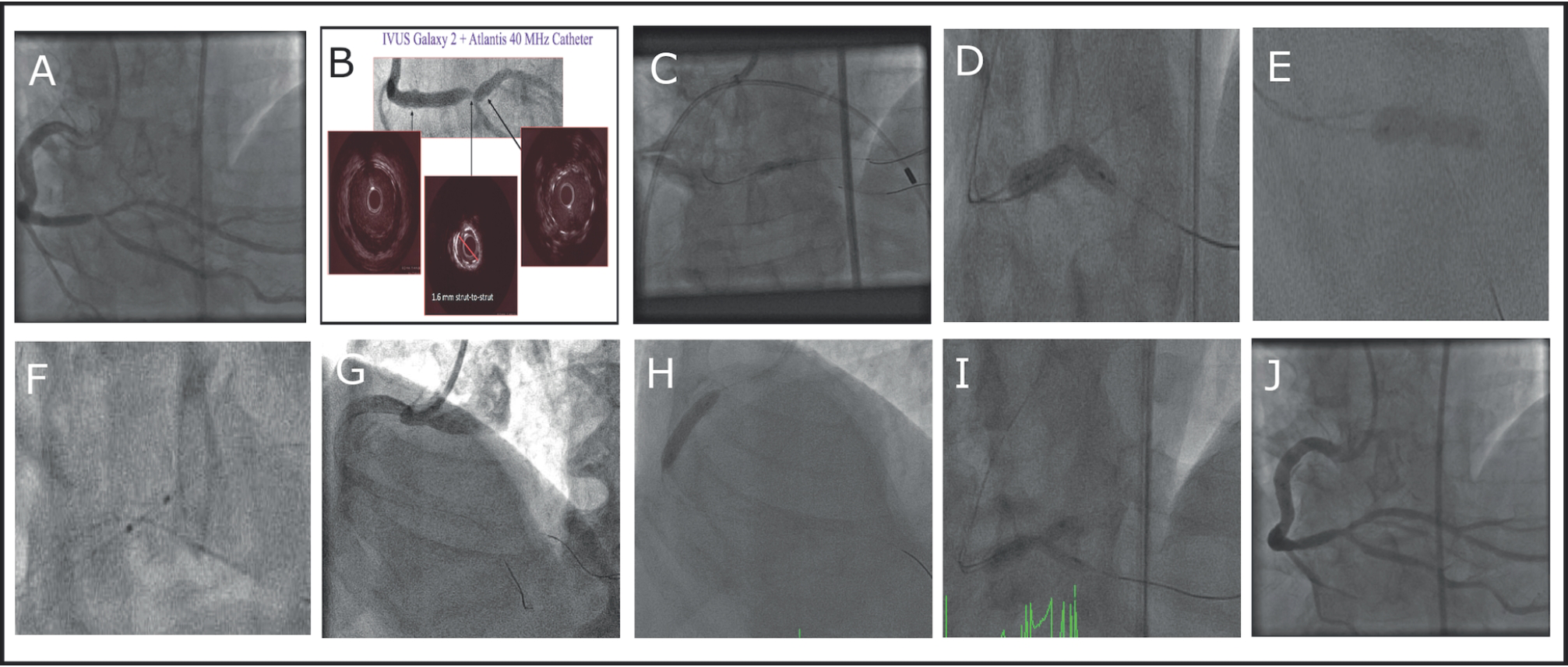
After 9 months following the first intervention, the patient was again complaining about angina. (A) Stent restenosis in the crux; (B) Strut-to-strut diameter was measured to be 1.6 mm via IVUS; (C) repeated balloon inflations; (D) 3.5 × 18 mm Powersail balloon at 20 atm; (E) 3.5 x 18 mm Powersail balloon at 26 atm; (F) 3.5 × 8 mm Powersail balloon at 26 atm; (G) dissection in proximal RCA while advancing the cutting balloon which was not able to cross the lesion; (H) bail-out stenting; (I) kissing with 3.5 + 3.0 mm balloons at 22 atm; and (J) final appearance of the second procedure.
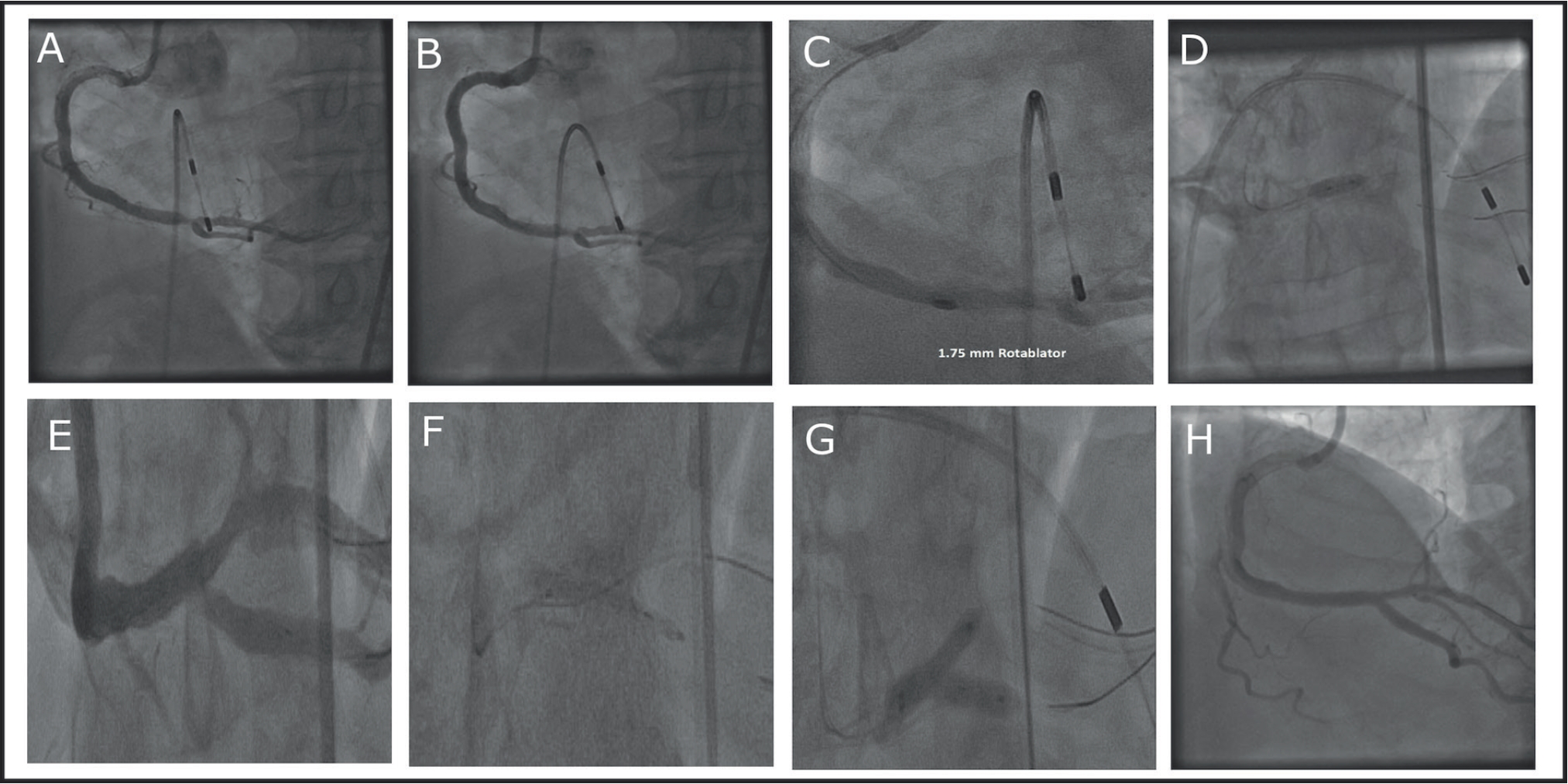
After 4 months following the second intervention, the patient presented with the same anginal symptoms. (A,B) Stent restenosis again, especially in the underexpanded region; (C) rotablation of the underexpanded stent struts with 1.75 mm burr under low speed (150,000 rpm); (D) postexpansion was still not easy; (E) deterioration of flow in the ostium of PDA; (F) 3.5 × 13 mm DES extending along PDA; (G) final kissing; and (h) final appearance
Conclusion
Consequently, given the limited options for treatment of underexpanded stents, rotablation is a reasonably safe and logical approach. Beyond being a bail-out option, by the growing number of cases reported in the literature, rotablation can be considered as an established treatment modality for underexpanded stents when classical and dedicated high-pressure balloons fail.

