Background
Gastric volvulus occurs when the stomach twists over its axis, leading to variable degrees of obstruction. It should be considered as a possible diagnosis in adult patients presenting with non-specific symptoms such as abdominal pain, vomiting, dysphagia, and heartburn, especially in patients having secondary risk factors such as hiatal hernia. In the acute presentation, a nasogastric tube should be passed to decompress the stomach and prevent ischemia [1,2]. If a tube cannot be passed at the bedside, the nasogastric tube should be placed via esophagogastroduodenoscopy (EGD), preferably with endotracheal intubation under anesthesia to prevent the aspiration of gastric contents. EGD also helps to diagnose the presence of hiatal hernias which is a common predisposing factor for a gastric volvulus. Apart from being a diagnostic tool, it can also be used as a means to reduce the volvulus to relieve the symptoms temporarily, especially in patients with comorbidities who are not good surgical candidates.
Case Presentation
A 78-year-old female, with a medical history of chronic obstructive pulmonary disease, pulmonary embolism, and atrial fibrillation treated with a Watchman device, presented with dysphagia and early satiety for 3 weeks. She had an acute episode of nausea and vomiting, associated with severe upper abdominal and mid-chest pain radiating to her back 3 weeks ago. The pain improved after a few hours, but the upper abdominal tightness and discomfort persisted. Her symptoms were worsened on eating food and associated with a sensation of food sticking in the chest. She also complained of recurrent hiccups and intermittent difficulty in eructation. To evaluate the cause of her symptoms, an EGD was performed under conscious sedation, and a hiatal hernia filled with debris, pills, and food particles was found (Figure 1). On further advancement, the endoscope could not pass the proximal stomach due to what appeared to be a gastric volvulus. Further attempts at the intubation of the stomach resulted in severe patient distress and gagging. To evaluate further, a computed tomography (CT) scan of the abdomen was done, which showed a “large redundant hiatal hernia” concerning for volvulus (Figure 2). Laboratory tests including a complete blood count, basic metabolic panel, and lactate were within normal limits.
A trial to reduce the gastric volvulus was undertaking using these steps: (1) a repeat EGD was undertaken, this time with monitored anesthesia care and endotracheal intubation. (2) During the EGD, the scope was retroflexed in the sac of the hiatal hernia, which appeared turned in the distal end. This helped in visualizing the volvulus (Figure 3). (3) Torsion was applied at this point to reduce(de-rotate) the volvulus. (4) This allowed us to traverse the gastric constriction and led to the entry of the scope in the main body of the stomach, which had notable erythema (5). The scope was advanced further into the duodenum, which appeared normal (6). The scope was then retracted up to the esophagus and re-advanced into the stomach. This time, however, re-entry into the stomach was achieved without difficulty, and previously identified area of volvulus was no longer present (Figure 4).
Along with being a diagnostic procedure, EGD proved to be an effective way to reduce the volvulus in this patient, providing immediate resolution of her acute symptoms, without any adverse effects. After reduction of the volvulus, the patient was referred for surgical fixation which was performed later that month.
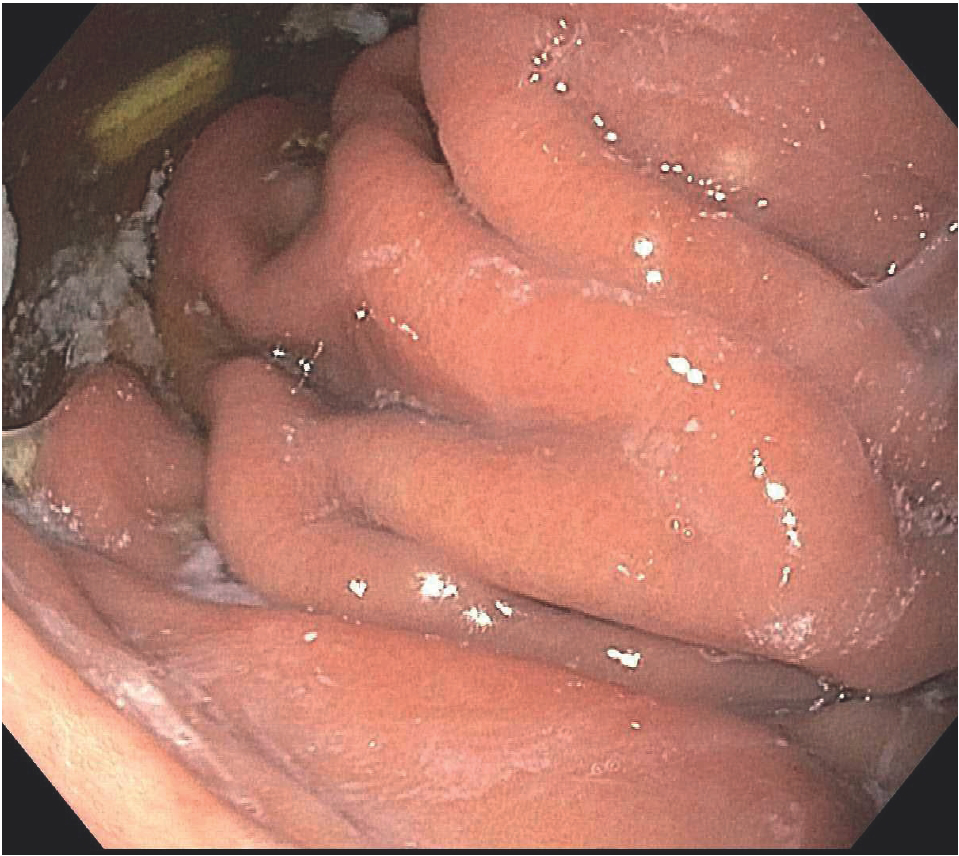
Esophagogastroduodenoscopy showing hiatal hernia with retention of food particles and pills in its sac.
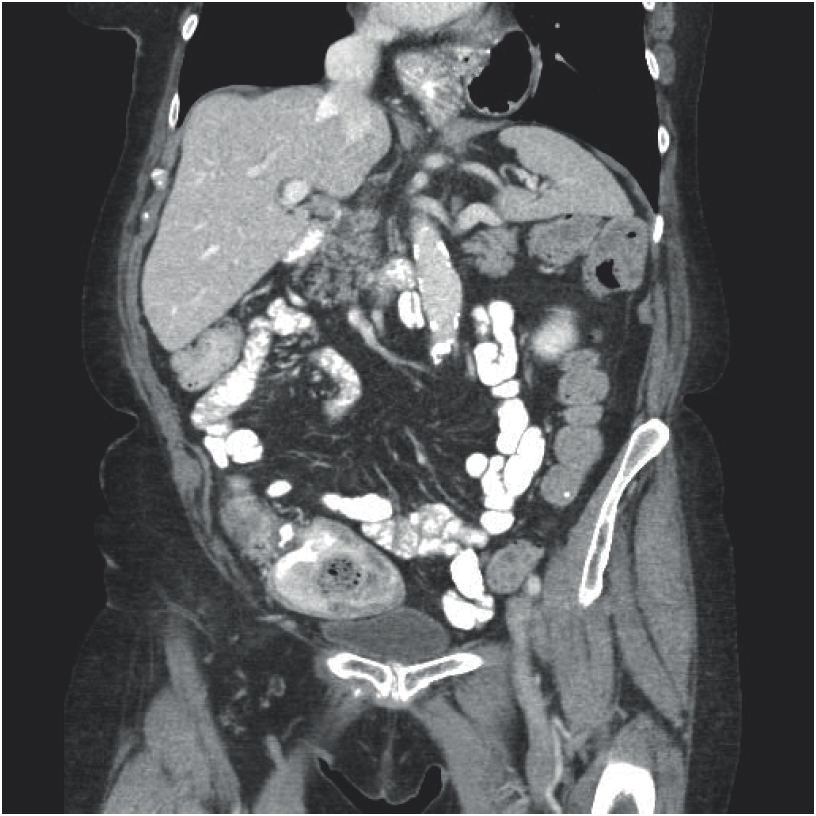
Coronal section of the CT scan of the abdomen showing the presence of part of the stomach above the diaphragm, in the thoracic cavity.
Discussion
Gastric volvulus is common in adults with age greater than 50 years and with risk factors which include diaphragmatic abnormalities such as hiatal hernia, para-esophageal hernia, diaphragmatic eventration, phrenic nerve paralysis, gastric or splenic abnormalities, and even kyphoscoliosis [1]. Gastric volvulus can present either acutely or may be a chronic condition secondary to other pathologies. In case of an acute gastric volvulus, the patient presents with three major symptoms that constitute Borchardt’s triad: abdominal or lower chest pain, vomiting, and inability to pass a nasogastric tube. This triad is present in almost 70% of the patients with an acute gastric volvulus [2]. Gastric volvulus, though rare, is more common in adults after their fifth decade, constituting 80%-90% of cases [3]. Symptoms of chronic gastric volvulus can be non-specific, ranging from mild abdominal discomfort, dysphagia, bloating, and heartburn. The physical examination in these patients is relatively normal. Acute gastric volvulus is usually diagnosed on plain abdomen X-rays which show a single large spherical gas bubble located in the upper abdomen or chest, along with air-fluid level [4]. CT scan is preferred over barium studies if radiographs prove to be inconclusive, as CT scan also picks up the anatomic abnormalities in case of a secondary gastric volvulus.
Often, patients presenting with these symptoms also undergo EGD as a part of their diagnostic evaluation. If a gastric volvulus is found, treatment measures in terms of nasogastric tube placement, reduction of the volvulus, and placing a percutaneous endoscopic gastrostomy (PEG) tube can be done in the same endoscopy. The endoscope is guided through the stomach beyond the twist and manipulated within the stomach [5,6]. If the stomach de-rotates, the endoscope should be guided into the duodenum, ensuring that the stomach is fully de-rotated. PEG tubes are used to prevent future rotation and are left for several weeks before they are removed to allow enough time for the formation of adhesions between the stomach and abdominal wall. It is important to note that anesthesia helps to relax the muscles, which aids in easy manipulation of the scope beyond the obstruction. The scope should follow the twist of the volvulus while advancing and should be manipulated in the opposite direction while retracting, to reduce the volvulus. The ease of re-advancement of scope back into the stomach can help to predict the scale of success of the procedure. This procedure is relatively safe and easy to perform, having the same side effects as that of any other EGD, with aspiration being a significant one. Hence, we recommend performing this procedure under general anesthesia.
Esophagogastroduodenoscopy (EGD) needs to be encouraged as not only a diagnostic but also a therapeutic method for the reduction of gastric volvulus. For this, we still need studies at a larger scale documenting the risk-benefit ratio of this procedure.
In a study of patients with chronic volvulus who were conservatively managed, 64% of patients had recurrent symptoms [7]. This makes surgical management more preferable in patients without co-morbidities, who are good surgical candidates. Recurrent symptoms, however, were not associated with any serious complications [7]. This gives us hope that surgical procedures can be avoided if appropriate steps are followed to reduce a gastric volvulus endoscopically, leading to the lower rates of morbidity.



