Background
Paraduodenal hernia (PDH) is a rare cause of internal hernias presenting with intestinal obstruction. It constitutes <1% of all cases of intestinal obstruction [1]. However, 53% of the internal hernias are PDH [1]. Among the cases of PDH, left PDH accounts for 75% and right PDH for 25% [1]. Undiagnosed cases of PDH can increase the mortality rate up to 20% [2]. CT scan of the abdomen should be done in doubtful situations [3]. At surgery, the hernial defect can either be marsupialized or suture closed primarily with or without mesh reinforcement [4].
Case Presentation
A 29-year-old female with no comorbidities presented with acute abdominal pain radiating to the back, nausea, bilious vomiting, abdominal distention, and obstipation since 2 days. She had undergone full-term normal delivery 4 days prior. She did not give any history of per rectal bleed. She was stable hemodynamically.
Per abdominal examination revealed mild abdominal distension with slight tenderness in the upper abdomen and hyperperistalsis in the central abdomen. Per-rectal examination revealed an empty rectum.
The laboratory reports were unremarkable, except for leukocytosis (15,230 per high power field).
Radiological examination
(A) Erect abdominal X-ray revealed multiple air fluid levels (Figure 1A).
(B) Ultrasonography of the abdomen showed dilated small bowel loops and minimal inter-bowel free fluid.
(C) Contrast-enhanced abdominal computed tomography (CECT) showed small intestinal loops to the right of superior mesenteric artery (SMA) suggestive of mal-rotation of midgut and a transition point beyond which contrast did not move into distal bowel loops (Figure 1B). On axial section, small bowel loops were seen posterior to ascending colon (Figure 1C). This gave an impression of completely obstructed right PDH.
At laparoscopy, a long stretch of small bowel loops was seen going into a recess present posterior to ascending colon (Figure 2A). These entrapped loops could not be reduced by gentle taxis (Figure 2B). Hence, lateral attachments of ascending colon were divided (Figure 2C). Waldeyer’s fossa was then laid open and marsupialized with the general peritoneal cavity by incising the sac in a progressively cephalad direction (Figure 2D). Contents of the hernial sac were reduced. The entrapped small bowel was not devitalized. After peritoneal toilet, ample quantity of normal saline was instilled into the peritoneal cavity to reduce the chances of postoperative adhesions.
Follow-up and outcome
Postoperative recovery was uneventful. She was kept nil by mouth for 1 day. On postoperative day 2, she was given liquids orally which she tolerated well. On postoperative day 3, she was given soft diet which was again tolerated well. Over the ensuing 6 months, she continues to be symptom-free. A brief timeline of events is summarised in (Table 1).
Discussion
Internal hernias are abnormal protrusions of part or whole of viscera through defects in the mesentery or peritoneum contained within abdominal cavity [1]. They constitute less than 2% of all cases of intestinal obstruction [5]. Neubauer was the first to describe paraduodenal hernia in 1786 [6]. Paraduodenal hernia is defined as abnormal protrusion of part or whole of viscera into paraduodenal fossa. PDH constitutes less than 1% of all cases of small intestinal obstruction [1]. 53% of internal hernias are PDH [1]. Of all cases of PDH, left PDH constitutes 75% and right PDH constitutes 25% [1]. PDH occurs due to an error in rotation of the midgut during embryonic developmental phase. Embryological development of right paraduodenal hernia consists of non-rotation of pre-arterial segment of midgut after initial 90 degree counterclockwise rotation with continued rotation of post-arterial segment of mid-gut which leads to entrapment of small bowel (pre-arte-rial segment) behind large bowel (post-arterial segment) mesentery (Figure 4) in a recess called Waldeyer’s fossa (Figure 3) which lies posterior to ileo-colic, right colic, middle colic vessels, and anterior to posterior parietal peritoneum [7].
| Day | Event |
|---|---|
| 0 | Patient presented with pain in abdomen and diagnosed with right PDH |
| 1 | Patient underwent laparoscopic repair of right PDH |
| 2 | Patient passed flatus and started on liquids which were tolerated |
| 3 | Patient started on soft diet |
| 4 | Patient had her first bowel movement |
| 5 | Patient was discharged |
| 10 | On first follow-up, patient was asymptomatic |
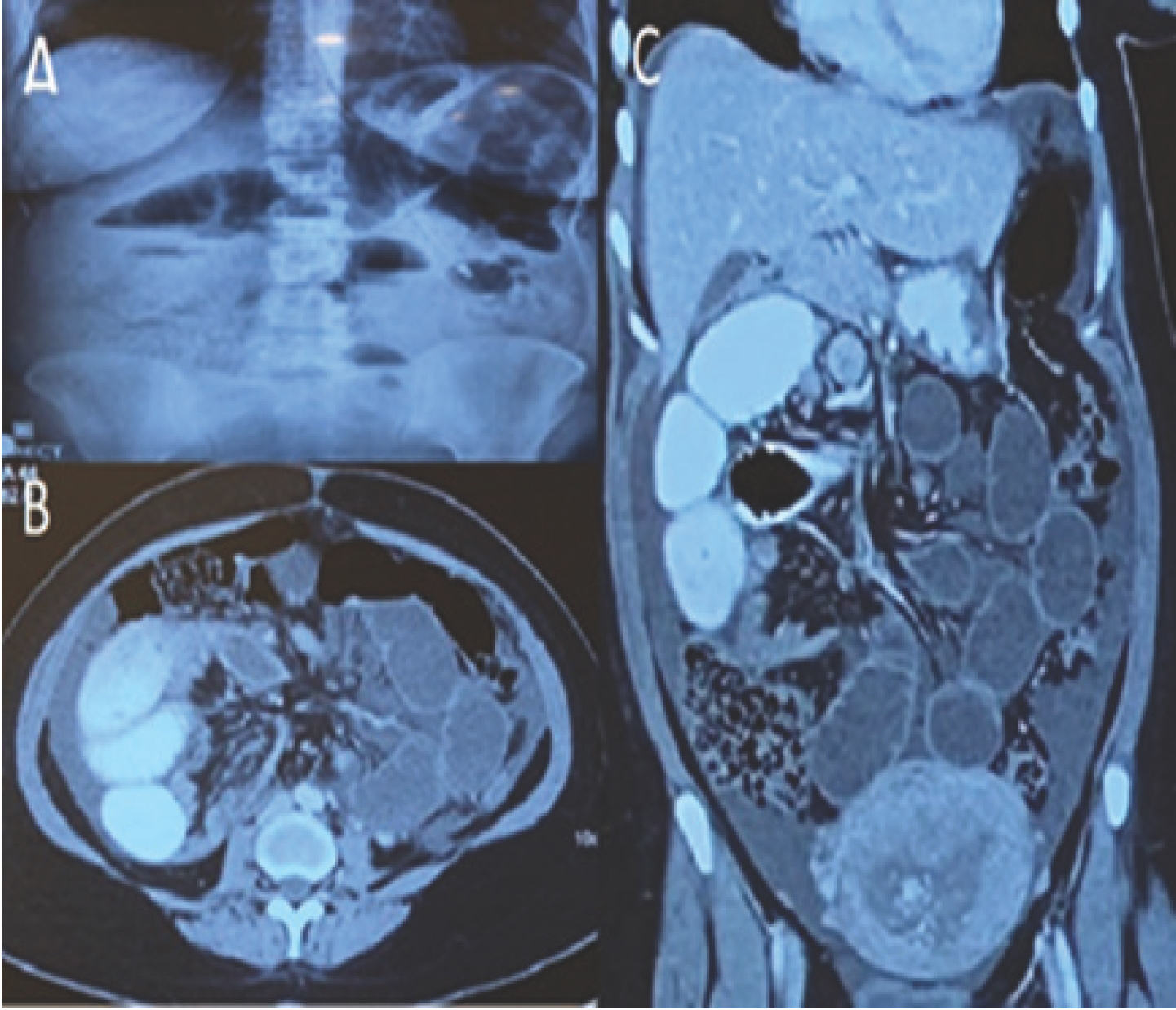
(A) X-ray abdomen showing multiple air-fluid levels. (B) CECT abdomen and pelvis [axial view] showing small bowel loops behind ascending colon. (C) CECT abdomen and pelvis [coronal view] showing small bowel loops to the right of SMA and transition point beyond which contrast is not seen going into distal bowel loops.
Left paraduodenal hernia generally affects the male population. Its development consists of normal rotation of gut and abnormal fixation of the descending mesocolon to the posterior abdominal wall, which leads to formation of an unsupported area and herniation of contents into Landzert’s fossa which lies lateral to the fourth part of the duodenum, posterior to the inferior mesenteric vein (IMV), the ascending branch of the ascending left colic artery (LCA), and anterior to posterior parietal peritoneum [7].
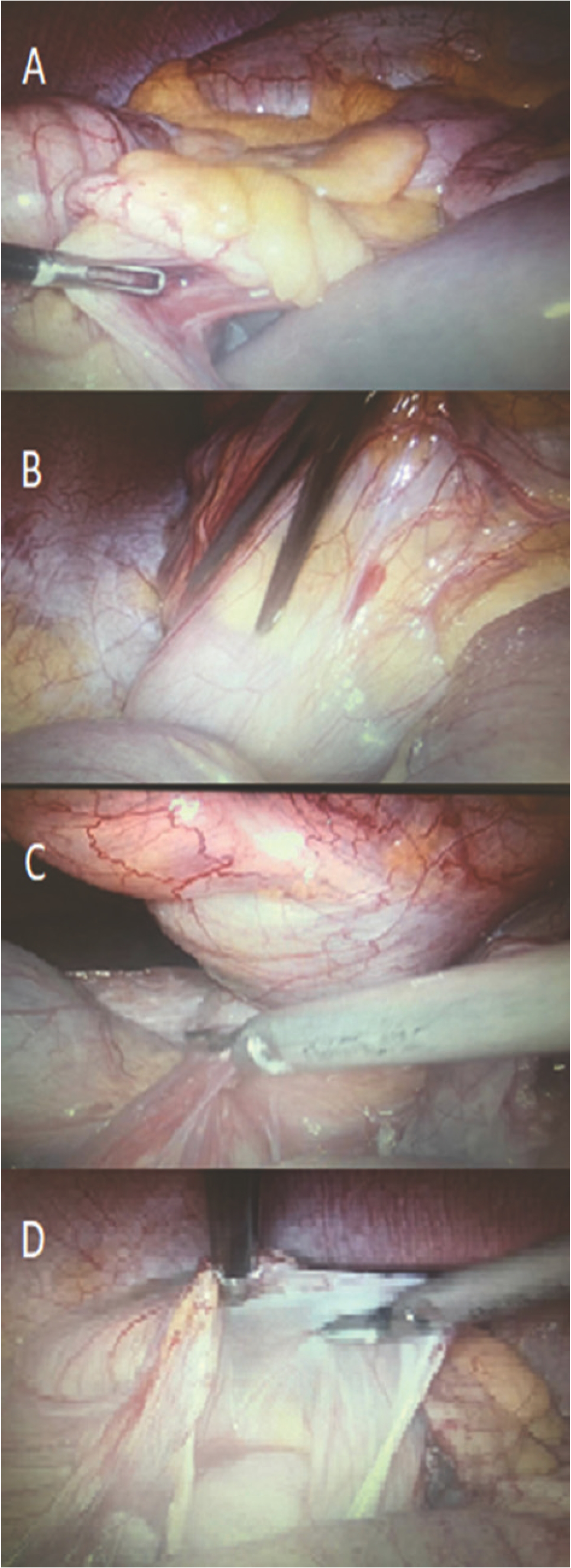
(A) Small bowel loops seen going into Waldeyer’s fossa. (B) Attempted but failed reduction of hernial contents by gentle taxis. (C) Division of lateral attachments of ascending colon and marsupialization of sac. (D) Whole hernia sac is merged with the peritoneal cavity.
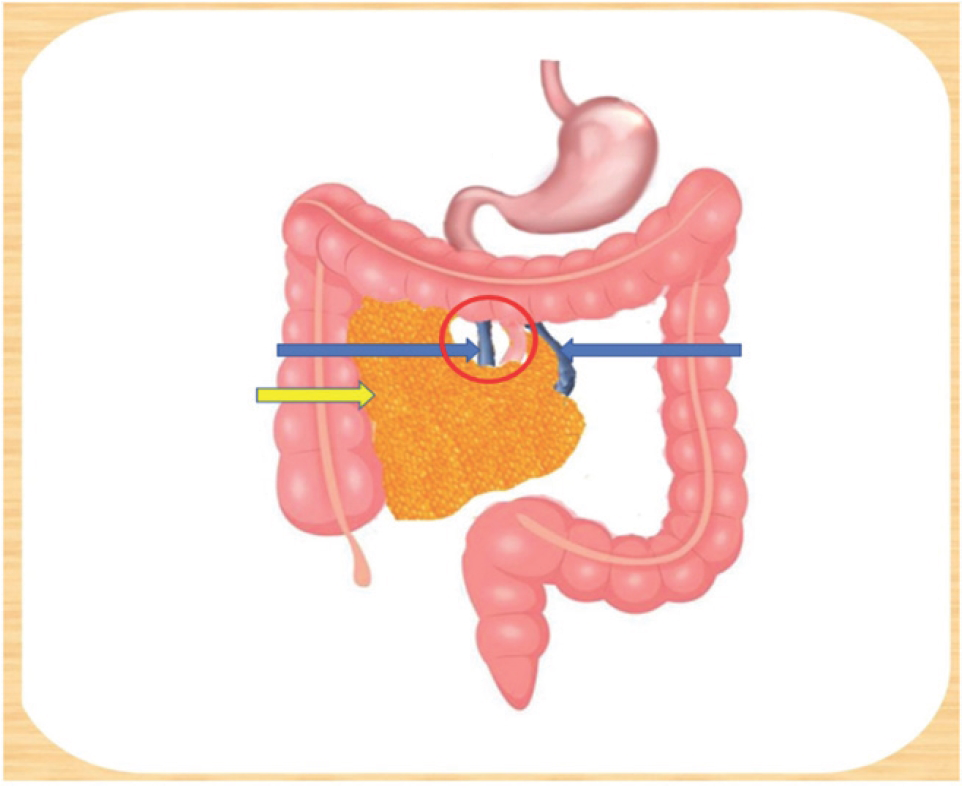
Yellow arrow depicts the hernial sac in the fossa of Waldeyer behind the ascending mesocolon, left blue arrow depicts the SMV, right blue arrow depicts the IMV, red circle depicts the hernial orifice.
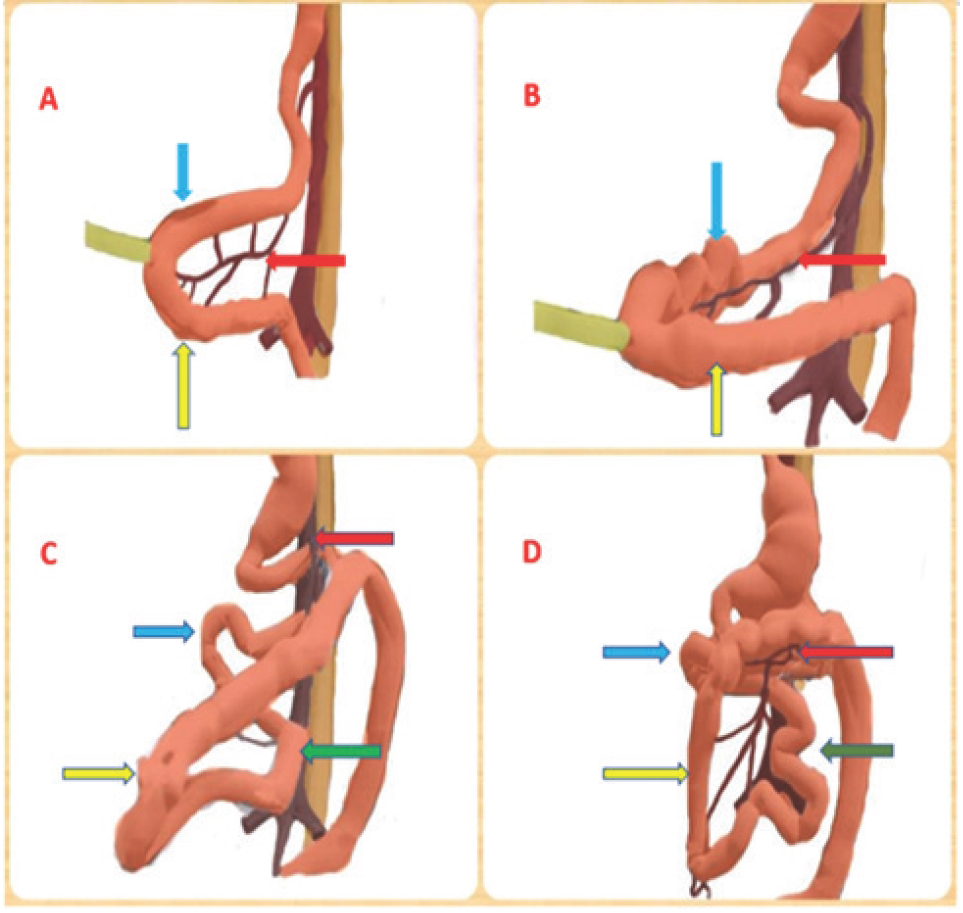
A&B: blue arrows: pre-arterial segment, yellow arrows: post-arterial segment, red arrows: SMA. C&D: blue arrows: proximal pre-arterial seg, green arrows: distal pre-arterial segment, yellow arrows: post-arterial segment, red arrows: SMA. (A) Herniation of midgut, (B) Initial 90° rotation of midgut, (C) Non-rotation of pre-arterial segment with continued rotation of post-arterial segment, (D) Entrapment of pre-arterial segment behind post-arterial segment.
The most common presentation of PDH is in the fourth and fifth decade of life, with male to female ratio being 3:1 [8]. Patients may present with non-specific symptoms such as nausea, vomiting, or dull aching long-term abdominal pain. However, it may also present with features of bowel obstruction such as vomiting, abdominal distention, sluggish bowel movements, constipation, or obstipation. PDH can also present with lump in abdomen. PDH can also be an incidental discovery during operation or radiological imaging [7]. The gold standard preoperative diagnostic investigation for PDH is contrast-enhanced computed tomography of the abdomen (CECT). In right PDH, the CECT abdomen may identify clumped small bowel loops along the right side of the abdomen with features of non-rotation of midgut. SMA lies anterior to clumped small bowel. Caecum remains in the normal position. Sometimes SMA, ileocolic artery and right colic vein lie in the anterior margin of the neck of the sac [3]. However, CECT of left PDH may reveal clumped small bowel loops seen between stomach and transverse colon anteriorly and pancreas or left adrenal gland posteriorly. IMV and ascending branch of LCA lie in the anterior or medial border of the sac [3].
| 1. | Patient (gender, age) | 29-year-old female |
| 2. | Final diagnosis | Obstructed right PDH |
| 3. | Symptoms | Pain in abdomen radiating to back, nausea, bilious vomiting, abdominal distension, and obstipation |
| 4. | Medications | IV fluids, antibiotics, analgesics, antacids, and anti-emetics |
| 5. | Clinical procedure | Laparoscopic repair of right PDH |
| 6. | Specialty | General and laparoscopic surgery |
| Serial no. | Title | Journal (Year of publication) | Author/s | Age/Sex | Presentation | Mode of surgery | Comments | Reference No. |
|---|---|---|---|---|---|---|---|---|
| 1. | A rare case of small bowel obstruction due to PDH | The American journal of case reports (2019) | Rahaf Suhail Al Otaibi et al. | 24y/F | Acute | Open | 2 weeks Post partum, Left PDH | [1] |
| 2. | Laparoscopic re- pair of a right PDH | Surgery Jour- nal,N.Y. (2018) | John Matthew Manipadam et al. | 31y/F | 2 months history | Laparo- scopic | Right PDH | [10] |
| 3. | Laparoscopic re- pair of a right-sided PDH | Journal of Surgical case reports (2019) | Stephanie Walker et al. | 37y/M | Acute | Laparo- scopic | Right PDH | [11] |
| 4. | Right PDH with midgut malrotation | Journal of the Belgian society of Radiology (2019) | Joon Ho Cho et al. | 30y/M | 1year history of intermittent pain & 4 months history of vomiting | Not known | Right PDH | [12] |
| 5. | Bowel obstruction due to a right PDH with midgut malro- tation | Journal of Visceral surgery (2020) | N Peru et al. | Young adult | Acute | Open | Right PDH | [13] |
| 6. | Laparoscopic repair of right PDH in adult patients: case report and literature review | Case reports in Surgery (2018) | Tomoko Takag- ishi et al. | 56y/F | Acute | Laparo- scopic | Right PDH | [14] |
| 7. | Case of strangulat- ed right paraduo- denal fossa hernia in a malrotated gut | BMJ case reports(2017) | Michelle Ong et al. | 53y/F | Acute | Open | Right PDH | [15] |
PDH can be treated by laparoscopic or open surgery. The basic principles of the surgery are:
(1) Reduction of the hernial contents with or without sac excision
(2) Suture-closure of the defect with or without meshplasty or
(3) Marsupialization, if the size of the defect is large
In our case, the defect was laid open and sac was marsupialized.
Topographic anatomical knowledge of the hernial borders is of clinical significance, as one can damage major vessels (SMA in right PDH or IMV in left PDH) during the repair of the hernia. However, it has been noted that in a case of left PDH, in order to get an access into the hernial orifice one may sacrifice the IMV [9]. We were able to manage our case totally laparoscopically. Laparoscopy has the well-known advantage of magnified view, less morbidity, shorter hospital stays, and early recovery [4]. A review of literature of recently published PDH cases over last 3 years is summarized in Table 3.
Conclusion
Rarity and nonspecific symptoms are the two factors causing difficulty in clinical diagnosis of PDH. However, early diagnosis can avoid ischemia of the bowel, with less mortality.
This case is particularly interesting for the following reasons:
(A) Our patient was a young female in her early postpartum period (post-full-term normal delivery) with no history of previous abdominal surgery.
(B) The symptoms started on day 4 after the full-term normal delivery of baby. This implies that during the latter part of her pregnancy, the increased intra-abdominal pressure must have had a role in pushing more and more small bowel loops through the congenital defect into her Waldeyer’s fossa, thereby resulting in entrapment and obstruction.
Thus, it is evident that in cases of intestinal obstruction, in the early postpartum period, PDH should be one of the differentials and can be managed laparoscopically. A summary of our case is given in (Table 2).

