Background
Cystic abdominal tumors are extremely common and are diagnosed more frequently and earlier due to the use of ultrasonography (USG) as a primary modality for a pelvic examination. It is very rare for simple ovarian cysts to grow immensely because of the routine USG scanning. However, in developing country such as India, in the lower socio-economic setting, even a large simple follicular cyst can be detected because of late presentation.
Very few cases of giant ovarian cysts have been sporadically reported in the literature. [1]. Ovarian cysts are very common in the adolescent. The terms “ovarian cyst” and “ovarian follicular cyst” are often used interchangeably. These two terms describe lesions > 3 cm, and it is important to differentiate them from an “ovarian follicle” which is < 3 cm [2]. If ovulation does not occur, these follicular cysts can continue to grow under hormonal stimulation, occasionally to sizes as large as 8 cm [3].
The most common symptoms of ovarian cysts are pelvic pressure or pain; however, many can remain asymptomatic. Most of the girls with follicular cysts present with abdominal pain and will often report irregular menses as well. Few cases can also go unnoticed due to the lack of any symptoms. Ovarian cancer risk increases in a linear fashion between the ages 30 and 50, with this risk continuing to increase, although at a slower rate, after the age of 50. While age is the largest risk factor for ovarian cancer, the combined history and physical findings dictate whether an ovarian mass can be expectantly managed with close follow-up or surgical management [4].
Case Report
A 20-year-old adult unmarried female referred to the radiology department with abdominal discomfort for 6 months aggravated for 15 days. On examination, her weight and height were 48 kg and 140 cm (body mass index: 23.4), respectively. Vital parameters were stable. There was no pallor, icterus, edema, or lymph node enlargement. The abdomen was grossly distended. On palpation, a large cystic non-tender mass seen in the abdominopelvic region reaching up to the epigastric quadrant.
Hemoglobin was 10.8 g/dl, and the total and differential white blood cell count was within normal limits. Carcinogenic antigen-125 (CA-125) was mildly elevated, with absolute value of 65 IU/ml (normal < 35 IU/ml). The patient was then referred to the radiology department for further evaluation.
Image findings
A frontal chest radiograph conducted for screening appears normal.
Ultrasound was performed using 3-5 MHz sectoral probe, which showed a large anechoic cyst in the abdominopelvic region reaching up to the epigastric region. The cyst shows a thin isoechoic wall with no internal septations or soft tissue components. The lesion was seen compressing and displacing stomach posterior superiorly and bowel loops posteriorly. Right mild hydroureteronephrosis is seen due to compression by the mass lesion along its right lateral aspect. There were no internal calcification/fluid-fluid levels seen.
On the Doppler study, there was no significant internal vascularity noted within the lesion.
Based on ultrasound imaging, the diagnosis of cystic ovarian mass of epithelial origin is made and further advised for contrast-enhanced magnetic resonance (MR) imaging (MRI) abdomen pelvis.
On the MR study, a large abdominopelvic mass lesion is seen extending superiorly up to the epigastric region showing hypointensity on T1 weighted imaging and hyperintensity on T2W/STIR imaging. No internal soft tissue enhancement is seen on the contrast study. A thin minimally enhancing wall is noted. No internal septation/ calcifications was seen.
We considered a diagnosis of serous cystadenomas in view of the size and MR signal characteristics. The right ovary could be distinctly visualized. Right mild hydroureteronephrosis has seen due to mild compression over the lower ureter.
A histopathological examination is suggested as the CA-125 is marginally elevated to look for underlying mitotic etiology.
Discussion
Small ovarian cysts are found incidentally clinically on ultrasound scanning; however, a large follicular cyst is very rare in literature. We have gone through few literature works which described a giant simple cystic abdominopelvic ovarian masses described by Spohn who reported 148.6 kg (328 lb), Symmonds [5] who reported 79.4 kg (175 lb), and Zamora et al. [6] who reported 72 kg ovarian cyst, and Farinetti et al. [7] reported excision of 23 kg ovarian cyst.
The patient may remain asymptomatic due to the absence of any pressure symptoms till late stage. They may present as vague abdominal pain with dragging sensation, and in few, they may have a history of irregular menses. In this case, the patient presented with abdominal pain only. Initially, at the physical examination, the surgeons derived the provisional differential diagnosis of liver mass or mesenteric mass. On USG, a large cystic mass is seen in the abdomen and pelvic area, extending into the epigastric region in its superior extension. Subsequent laboratory investigation showed a mildly elevated CA-125. Serous/ mucinous cystadenomas are very close differentials, in which serious type is the most common type of epithelial neoplasms encountered with benign cystadenoma about 75%, and mucinous cystadenomas were 25% [8]. Simple ovarian cysts up to 10 cm in a patient of any age are highly likely to be benign, with the malignancy rates of less than 1% [9].
An increased CA-125 raises the suspicion of mitotic etiology by the pathologist. However, the minimally elevated CA-125 can also be seen in benign etiology with the risk of cancer increases depending on size, wall morphology, and internal components [10]. These simple cysts are either nonneoplastic cysts (including physiologic cysts, periovarian or paratubal cysts, and small hydrosalpinxes) or benign neoplastic cysts (including serous and mucinous cystadenomas) [11]. Small mural nodules may be missed at the US in seemingly simple cysts larger than 7.5cm, where MRI plays a key role to detect soft tissue signal intensity.
Subsequent evaluation with the MR study revealed no significant soft tissue component/septation, which further suggests benign etiology. We derived the diagnosis of serous cystadenoma on the basis of radiological manifestations. However, the differentiation of giant follicular cyst with benign epithelial neoplasm is difficult on imaging modality solely.
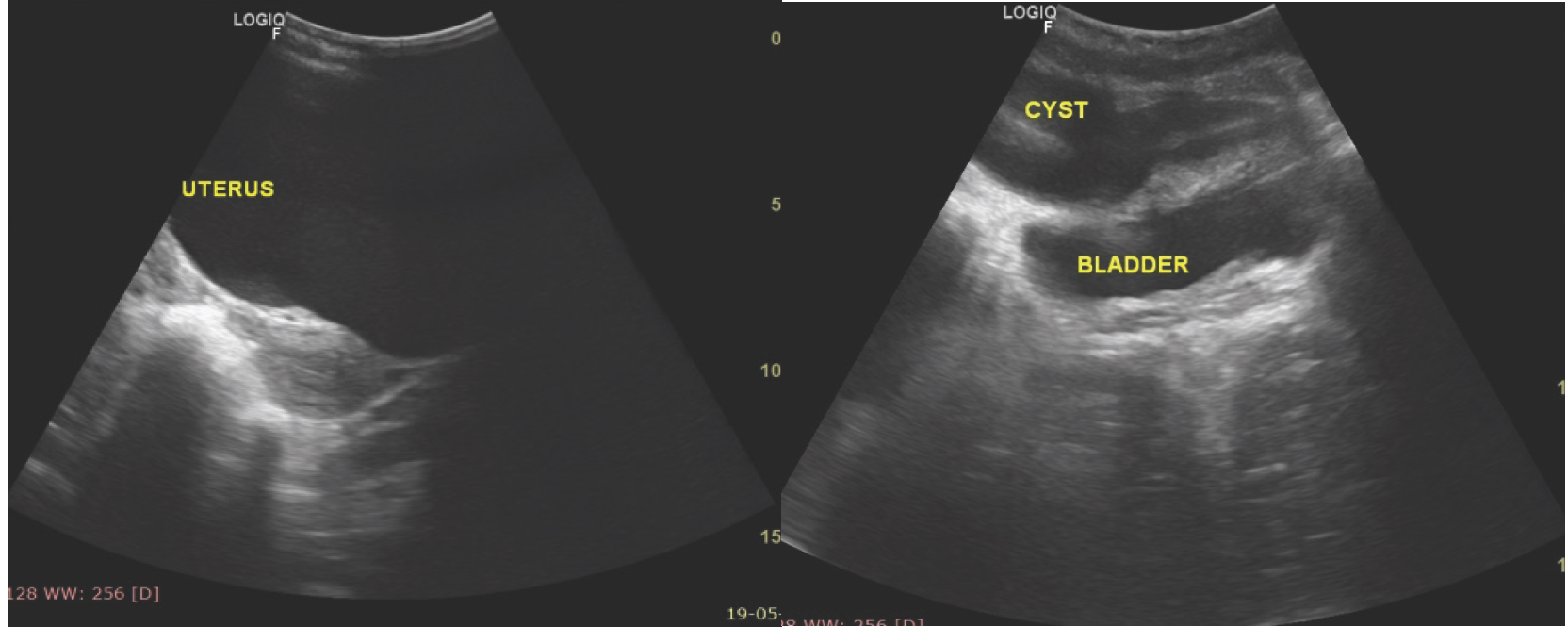
Gray-scale USG of the pelvis in the longitudinal section shows (a) a large anechoic cystic area in midline compressing the anterior wall of the uterus (b). Cyst is also seen indenting the anterosuperior margin of the bladder wall. No internal septations/soft tissue echogenicity seen.
USG-guided aspiration of cystic fluid was performed for the fluid cytology of the cyst. The cytology of the fluid showed a few benign epithelial cells and no malignant cells. No normal ovarian tissue could be identified, and the patient underwent surgery. A histopathological examination of the excised cyst wall was reported as a juvenile solitary follicular cyst with no evidence of malignancy.
There was no evidence of hydroureteronephrosis seen on the right side on follow-up ultrasound.
Differential diagnosis
Differential diagnosis of the large abdominal cystic lesion includes functional cysts and serous cystadenomas (common), cyst adenofibromas and mucinous cystadenomas (less common), and mesenteric cysts.
Final diagnosis
A giant follicular cyst was seen on the ovary.
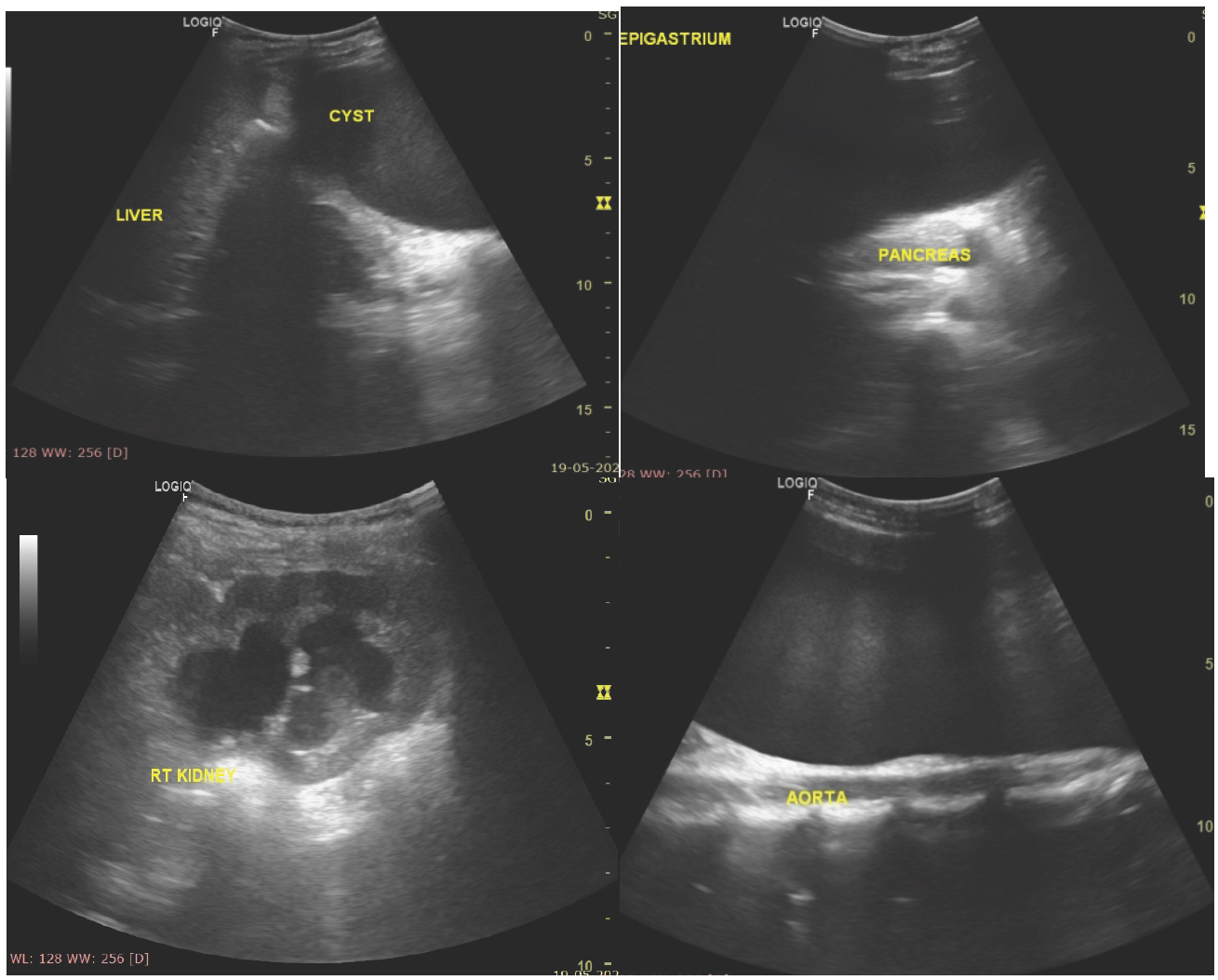
A large cystic anechoic pelvic mass (Figure 1) seen extending (a) in the epigastric region abutting the lesser curvature of the stomach. (b) Causing mild compression of the pancreatic head and proximal body. (c) The mass is slightly right parasagittal in location causing into compression over the right lower ureter, resulting in moderate right hydroureteronephrosis. (d) In its posterior extension, it is seen indenting the retroperitoneal organs such as the aorta.
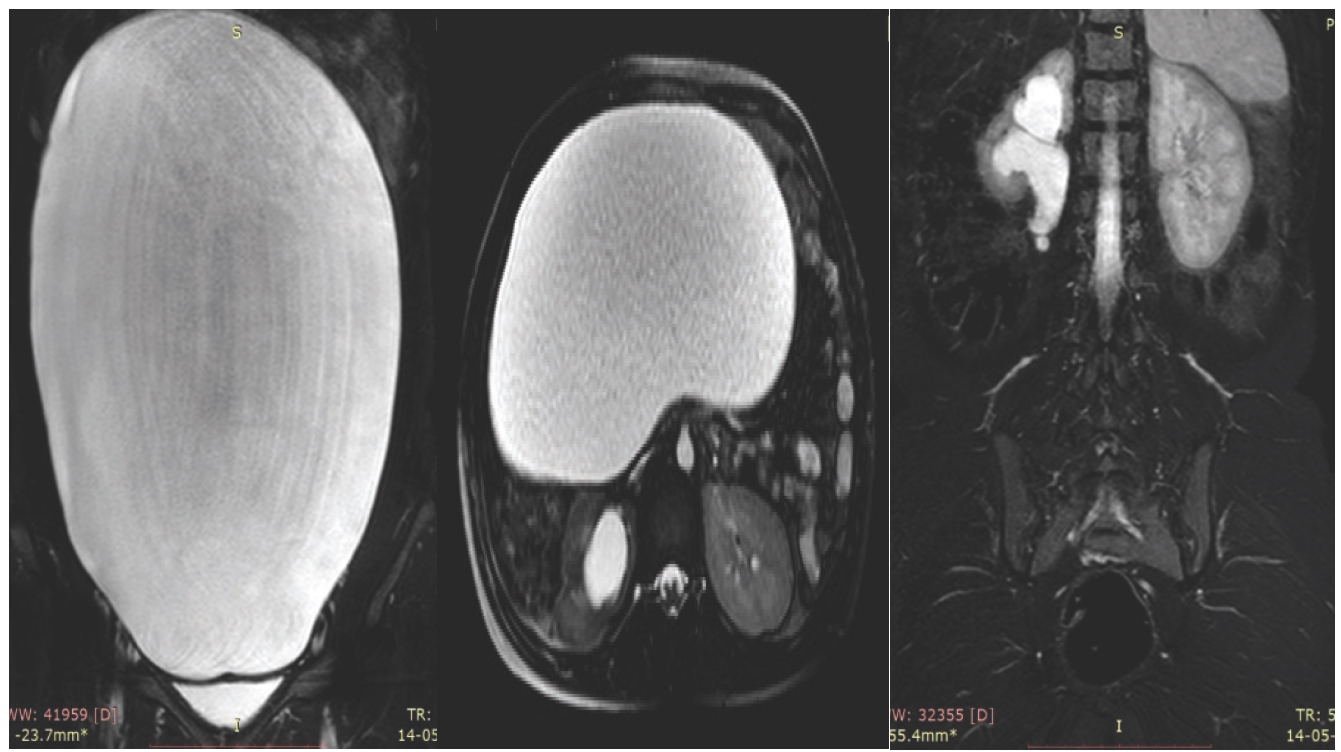
Coronal, axial, and sagittal T2 fat-saturated MR images show (a) a large abdominopelvic cystic mass lesion extending into the epigastric region with slight right parasagittal location causing (b and c) indentation over the retroperitoneal organs and vessels.
Conclusion
An imaging modality collaborated with the histopathological findings leads to the accurate diagnosis of cystic ovarian masses. A giant functional cyst of the ovary may show similar USG and MR appearance and should be further evaluated on histopathological examination. Radiological modalities play a vital role in narrow down the differential diagnosis and further management.
What is new?
Small ovarian cysts are found incidentally clinically on ultrasound scanning; however, a large follicular cyst is very rare in literature. In a developing country such as India, in the lower socioeconomic setting, even a large simple follicular cyst can be detected without any pressure or other clinical symptoms.



