Background
Chronic myelomonocytic leukemia (CMML) is a rare and heterogeneous malignant myeloid disorder that shares features of myelodysplastic syndromes and myeloproliferative neoplasms [1-3]. Patients present with a variety of symptoms, including splenomegaly in about 30% that results from extramedullary hematopoiesis [3,4].
The variable clinical course, advanced age, and disappointing long-term efficacy of currently available treatment alternatives complicate treatment choice [2] and give it a relatively poor prognosis, with a median overall survival of 2-3 years [3]. The allogeneic hematopoietic cell transplantation is the only curative option, resulting in long-term remission in up to 40%, but applies to a minority of patients [2]. Other therapeutic measures commonly used include the use of erythropoiesis-stimulating agents, cytoreductive chemotherapy, and hypomethylating agents, but only palliate the symptoms [3]. Although the current therapeutic options can improve patient’s quality of life, they barely modify disease evolution [4].
Splenomegaly is a debilitating complication that presents in many other lymphoproliferative disorders and can present with abdominal discomfort or tenderness, pain, early satiety, fatigue, cachexia, and cytopenia secondary to sequestration [5]. Approaches directly targeting the spleen include splenectomy or splenic irradiation (SI). Although splenectomy is efficacious for select patients, 36% of those experience significant complications, with a high rate of postoperative mortality. SI may be an ideal alternative for patients who have a poor response to systemic therapy and/or are not surgical candidates [5,6].
In this article, we present a case report of a patient with CMML who received SI. As far as we are aware, this is the first case report of SI for symptomatic splenomegaly on a patient with CMML.
Case Presentation
A 71-year-old man with no relevant medical history presented with abdominal pain and left hypochondrium distension, a recent weight loss of 10 kg, and leukocytosis with monocytosis (5,040 cells/μL); the abdominal ultrasound revealed a massive enlargement of the spleen and liver, and the bone marrow biopsy revealed hypercellularity, with an increase in the number of elements in the granulocytic series and marked dysmegakaryopoiesis. The diagnosis of CMML was made. The man started treatment with hydroxyurea, initially with splenic, clinical, and analytical responses. About 10 months later, he reported of clinical worsening and started methylprednisolone and mercaptopurine, with a new sustained response for 1 year. Due to the new analytical worsening (leukocytosis with monocytosis plus thrombocytosis) and expressive splenic growth, the patient was proposed for splenic radiation therapy (RT).
The patient underwent palliative RT to the spleen with volumetric-modulated arc therapy, with a 6-MV photon beam. The planning target volume (PTV) included the spleen with a 2 mm margin. The dosimetric plan was to administer a total dose of 7.5 Gy to the PTV in 5 × 0.25Gy and 10 × 0.50 Gy per each fraction (Figure 1A and B). Initially, the patient was started with 0.25 Gy fractions every other day, to evaluate clinical and hematological response. After four fractions (cumulative dose of 1 Gy), the treatment was suspended due to thrombocytopenia (Figure 2). After 4 weeks, the treatment was resumed, but due to thrombocytopenia and anemia, it was suspended again after 4 × 0.25 Gy fractions (total dose of 2 Gy). The man maintained the analytical changes and no objective clinical or imagological response was observed (Figure 3), so the treatment was given as concluded and the patient was discharged. The patient was kept in palliative care and died 6 weeks after RT was completed.
Discussion
SI has been widely used in palliative treatment of symptomatic splenomegaly in patients with lymphoid and myeloid malignancies [7,8]. First carried out in 1903, SI is well recognized among radiation oncologists as an effective, low toxic, and cost-effective alternative to splenectomy, although non-radiation oncologists may be unaware of its efficacy [5,6]. The main purpose is the palliation of symptoms, like abdominal pain, anemia, and thrombopenia.
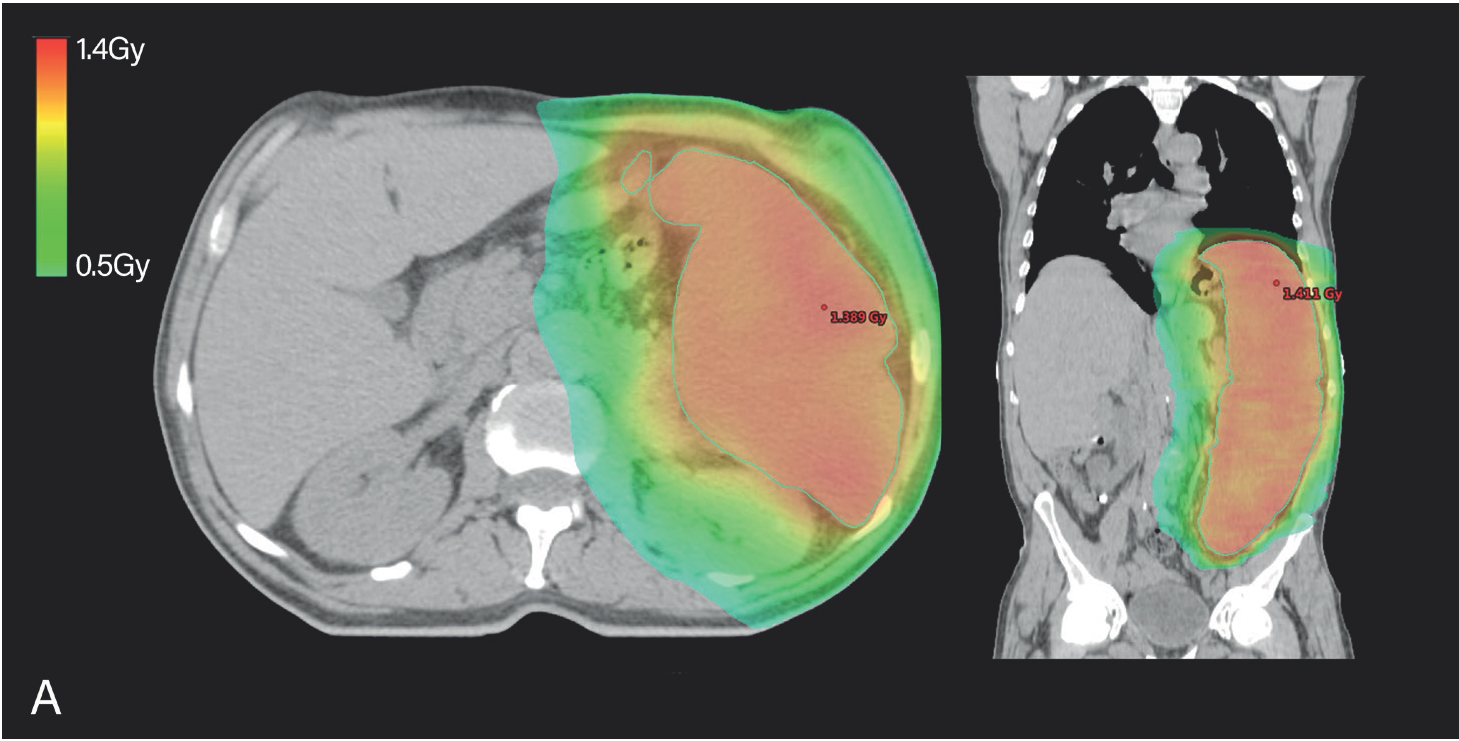
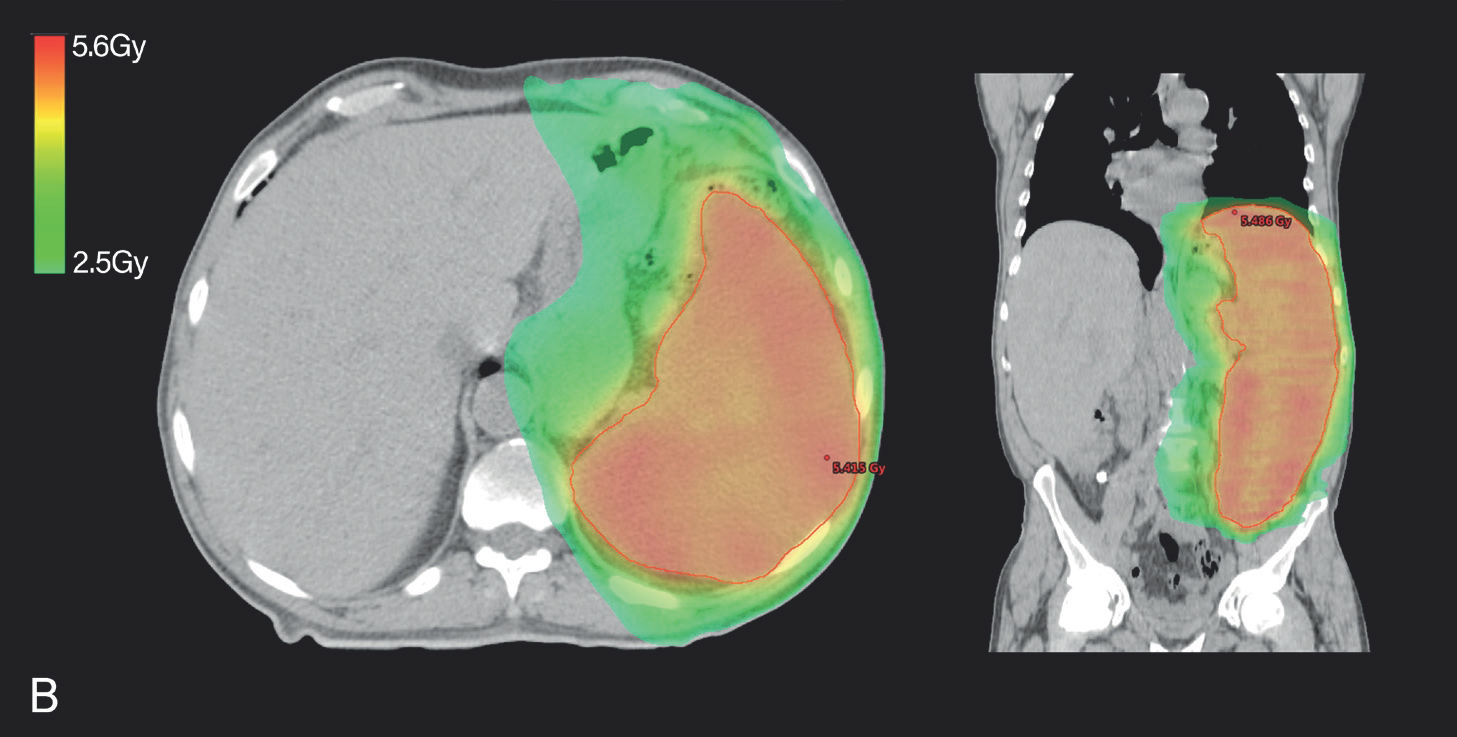
Dose color wash showing the prescribed dose in axial and coronal planes. A: 5x0,25Gy; B: 10x0,50Gy.
Irradiation induces a broad range of local and systemic effects, which may result in systemic remissions besides local palliation, but the underlying mechanisms are not yet fully understood [6].
There are several articles in the literature corroborating the effectiveness of SI for the palliative management of symptomatic splenomegaly. In the available literature, outcomes are assessed by using several endpoints, such as pain relief, reduction in size of the enlarged spleen, and improvement of cytopenias and symptoms associated with splenomegaly. Given the number of patients referred for SI is low and the significant heterogeneity in patient characteristics, there is no consensus on optimal dose-fractionation schemes; so, both efficacy and toxicity outcomes reported show considerable diversity. As far as the role of SI for patients with CMML, we found no reports in the literature concerning patients with this diagnosis. However, the published articles show some interesting results that can be used for these patients.
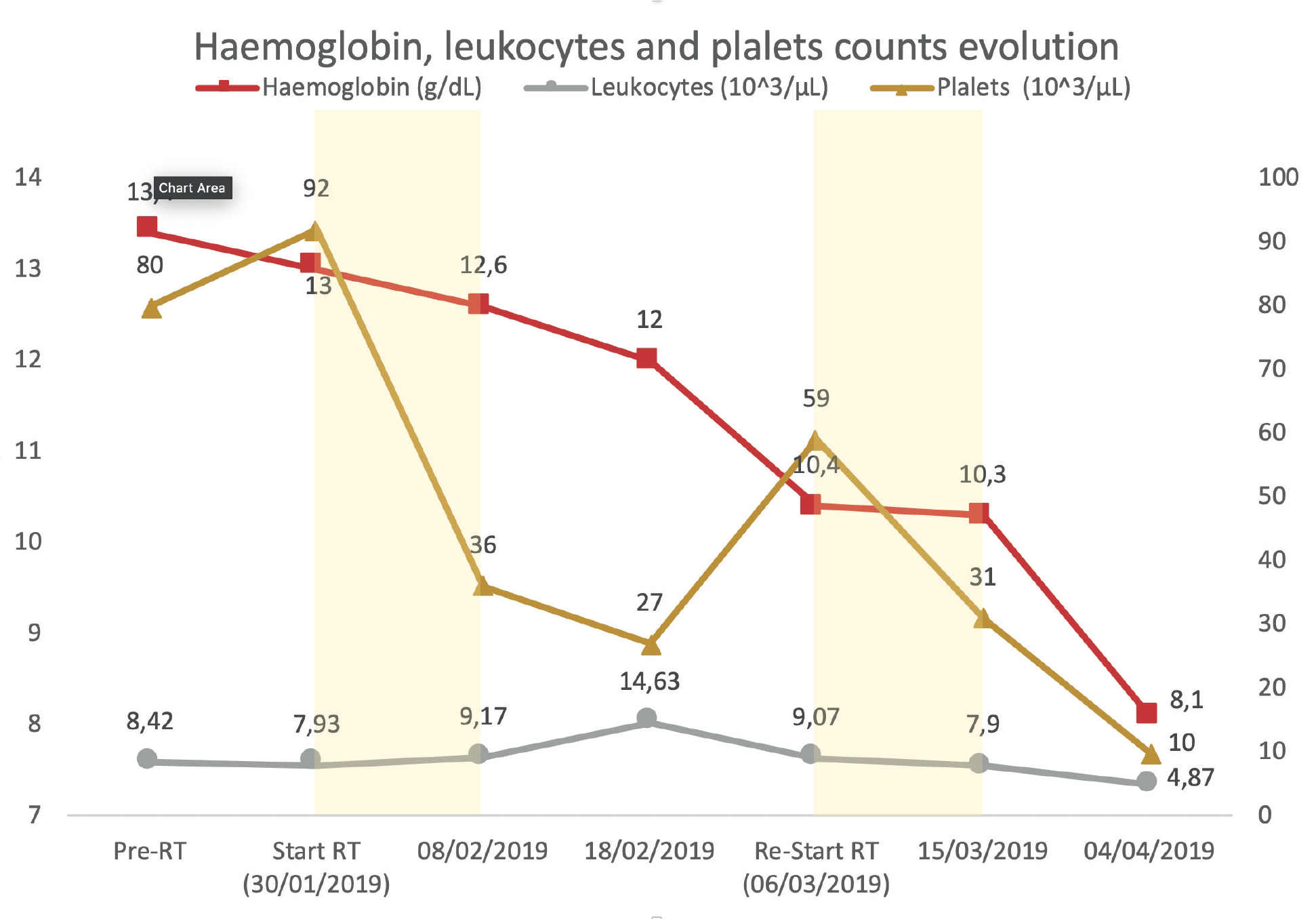
Evolution of hemoglobin, leukocytes and platelet counts before, during and after the treatment. Yellow areas represent the period the patient was receiving radiation therapy.
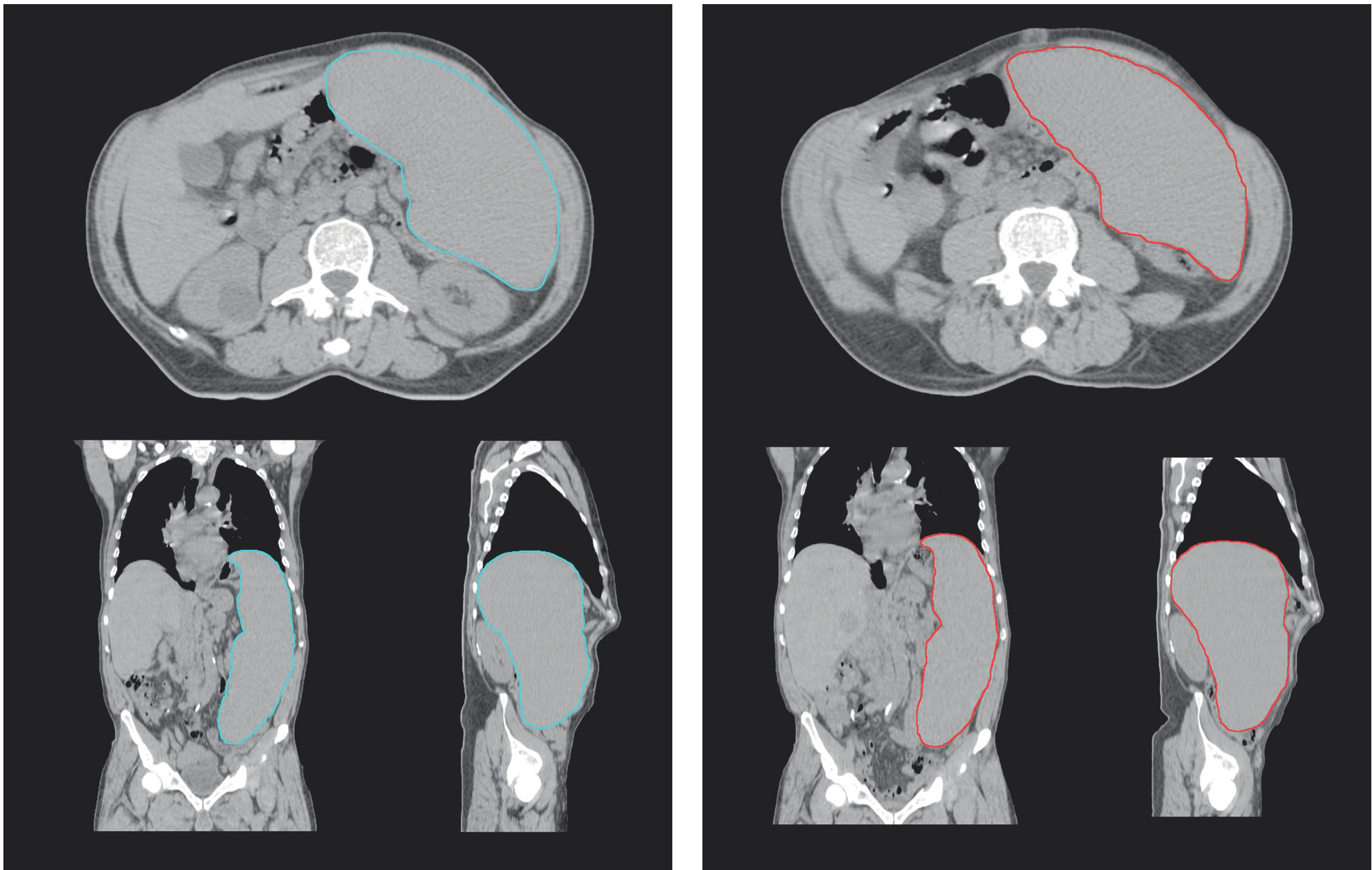
Spleen volume before (left, V=3212cc) and after (right, V=3310cc) the treatment (total dose of 2Gy); Blue and red lines indicates the clinical target volume.
The doses used in the literature show a large interval of values, with a range between 0.15 and 30.5 Gy in fractions of 0.1-2.5 Gy [5]. To avoid toxicity, these doses must be kept at lower levels, which have been supported by several studies.
In the report by Elliott et al. [9] on 23 patients, objective spleen-size reduction and relief of symptoms were observed in 94% and 96%, respectively. In Bouabdallah et al.’s [10] study on 15 patients, 90% of them reported complete resolution of splenic pain and 81% an objective reduction in spleen size. In the analysis with 14 patients, by Kitanaka et al. [11], reduction in spleen size was obtained in 93% and relief of symptoms in 86%. All of the previous studies used a median total dose of less than 10 Gy (2.8 Gy, 9.8 Gy, and 5 Gy, respectively), and it seems to be sufficient to ameliorate splenomegaly and its associated symptoms. A larger study by Kriz et al. [8] confirms these findings. 122 patients were treated with doses from 0.3 to 16 Gy in fractions of 0.1-2 Gy, with pain relief achieved in 74.8% and improvement of hematological parameters in 73.6%.
Using lower doses may be important for avoiding excessive radiation-induced toxicity while being an effective palliative treatment option. The biggest systematic review, which included 486 patients, concludes that there was no apparent correlation with improvement in symptoms of doses of 5 Gy versus 10 Gy, suggesting lower doses may be as effective as higher doses. The overall rate of pain relief, improvement of cytopenias, and spleen-size reduction was 59%, 78%, and 72%, respectively [5].
Close monitoring of hematological parameters during the course of SI is critically important for early detection and prompt management of toxicity, which includes thrombopenia, neutropenia, and/or febrile neutropenia or sepsis. The most common toxicities were grades 3 and 4, and developed in 82.5% of the patients [5].
Also, the incorporation of adaptive radiotherapy approaches and image guidance techniques may enhance the accuracy and precision of SI, as the first allows for redesigning the treatment plans concerning for changes in target volume during the radiotherapy course, and the second improves accuracy and precision of radiotherapy by accounting for intrafractional and interfractional uncertainties during the fractionated radiotherapy course.
Conclusion
The literature concerning SI is limited by the significant heterogeneity of patient characteristics, diagnoses, and prognosis, making it difficult to come to a consensus on patient selection and optimal dose-fractionation schemes. This is even worse when it comes to patients with CMML, as none of the small uncontrolled studies available includes this diagnosis. The available data show that SI is an effective palliative treatment option for patients with symptomatic splenomegaly by reducing symptoms and hematological parameters, due to significant reduction of splenic size. Even low doses appear to be equally efficacious. Our patient is an example of the need of close monitoring through RT, as hematological toxicities are common and, sometimes, fatal.
What is new?
The literature concerning SI is limited, making it difficult to come to a consensus on patient selection and optimal dose-fractionation schemes. This is even worse when it comes to patients with CMML, as none of the small-uncontrolled studies available includes this diagnosis. This is the first case report of SI for symptomatic splenomegaly on a patient with CMML. This article can help future physicians to treat and manage symptomatic splenomegaly.

