Background
Brugada syndrome (BrS) is a rare autosomal dominant inherited disorder associated with ventricular arrhythmia and sudden cardiac death (SCD) caused by mutation of the SCN5A gene that encodes for alpha-subunit of the sodium channel [1]. Brugada phenotype (BrPh) is an acquired form of Brugada resembling electrocardiographic (ECG) pattern associated with an identifiable stressor that is transient and disappears with resolution of the stressor [2]. The typical ECG findings may occur spontaneously, after provocative drug testing or with stressors. The literature has often elaborated certain modulating factors, such as bradycardia, vagal tone, fever, and certain medications, that unmask or exacerbate BrS [3]. However, its existence in the setting of HTN is not described. We report a case of a 28-year-old male who manifested as typical type 1 ECG finding of Brugada pattern in the setting of uncontrolled hypertension and atypical chest pain.
Case Presentation
A 28-year-old African-American male presented to the emergency department (ED) with a complaint of sudden onset, sharp, intermittent, localized anterior chest pain rated as 3/10 in intensity that started a few hours prior to his ED visit. His chest pain was non-exertional, non-pleuritic, and non-radiating with associated dyspnea. The remainder of his review of symptoms was negative, including palpitation, syncope, presyncope, nausea, or vomiting. His past medical history was significant for hypertension and hyperlipidemia. No family history of SCD and premature cardiac disease was reported. The patient’s home medication included hydrochlorothiazide 25 mg and pravastatin 20 mg, once a day. However, he was not compliant with his medications. His physical examination was significant for elevated blood pressure at 204/102 mmHg. Cardiovascular and pulmonary examinations were normal without any tenderness of the chest wall. ECG upon admission showed right bundle branch block (RBBB) with down sloping of the ST segment with T-wave inversions in V1 and V2 consistent with type 1 Brugada pattern as shown in Figure 1. Admission lab work revealed normal electrolytes, serial troponin less than <0.03 ng/ml (normal), and erythrocyte sedimentation rate 8 mm/hour (normal). Urine toxicology and blood alcohol level were negative. A computed tomography ruled out pulmonary embolism. Labetalol 10 mg was administered intravenously and home hydrochlorothiazide was restarted. His blood pressure gradually lowered to 132/76 mmHg within 24 hours and his chest pain resolved as well. Subsequent ECG revealed type 3 Brugada pattern as shown in Figure 2. On further reviewing the patient’s outpatient records, he recently had an abnormal ECG showing type 3 Brugada pattern when his blood pressure was 119/77 mmHg as shown in Figure 3. His treadmill stress test was negative for ischemia. Similarly, a transthoracic echocardiogram demonstrated an ejection fraction of 59% and normal RV systolic function. Moreover, a 30-day event monitor revealed sinus rhythm. He declined provocative testing as well as genetic testing for the SCN5A gene mutation. Nonetheless, since BrPh was seen on ECG after lowering his blood pressure, he was discharged from hospital without any sequel. His hospital course is shown in Figure 4.
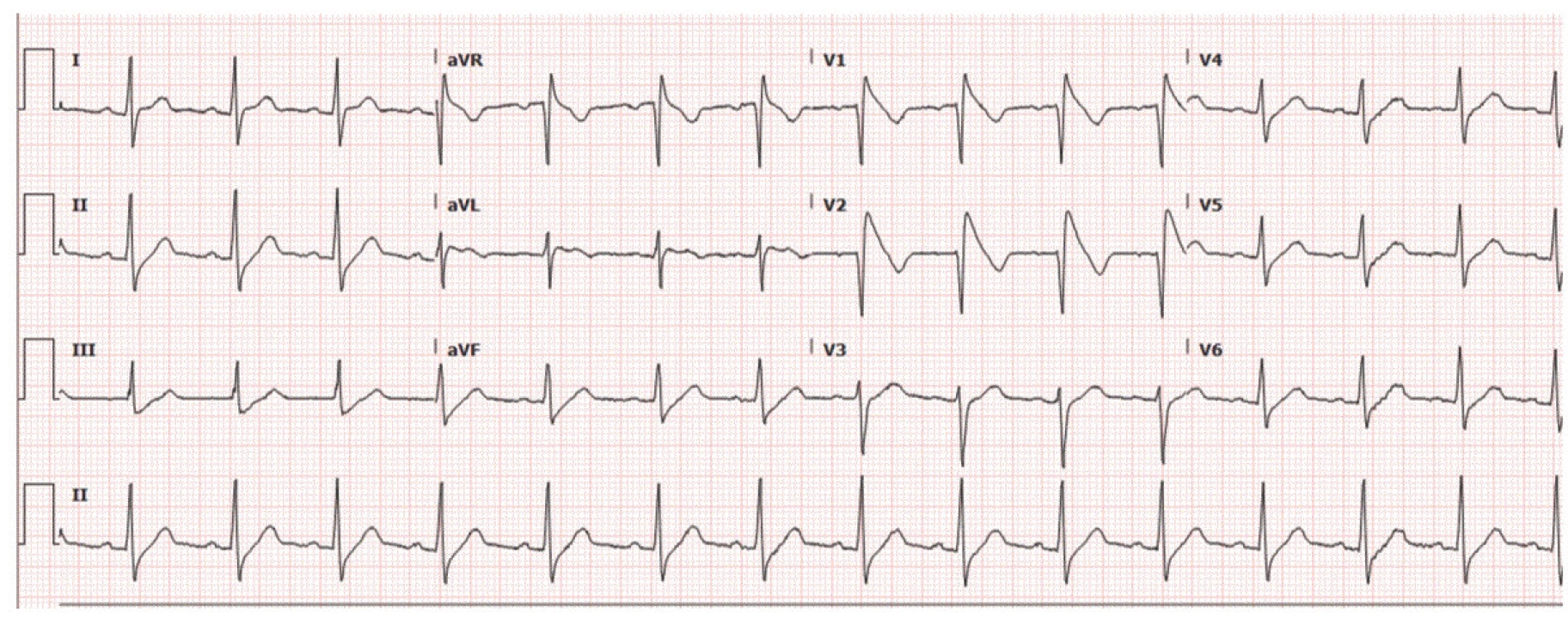
Type 1 Brugada pattern on ECG strip of patient upon presentation; BP upon presentation: 204/102 mmHg
Discussion
We presented a rare case of typical type 1 Brugada pattern in ECG in a young man who presented with uncontrolled hypertension and atypical chest pain. ECG findings remarkably changed to type 3 Brugada pattern when the blood pressure was normalized. BrS is an inherited arrhythmic disorder which develops secondary to the SCN5A gene mutation, and which encodes for the cardiac sodium channel [1]. Such channelopathy can lead to life-threatening arrhythmias and SCD. Sleep deprivation, fever, antiarrhythmic drugs, tricyclic antidepressants, alcohol and cocaine use, and electrolyte abnormalities, including hypokalemia, hyperkalemia, and hypercalcemia, are some of the common triggers known to incite SCD in patients with BrS [4-6]. Three ECG patterns can be noted in patients with BrS. Classic Brugada ECG (type 1), also referred to as a “coved type” ECG, is described as a RBBB, prominent ST segment elevation (≥2 mm) with inverted T-wave in precordial leads V1 and V2 with little to no interruption of the isoelectric line, which is our patient’s ECG results [3]. Type 2 Brugada ECG, also known as “saddle back” pattern, has RBBB with ST elevation and biphasic T-wave configuration in the precordial leads. Type 3 Brugada ECG has a similar ECG pattern to that of type 2, the only difference being ST segment is elevated by 1 mm or more in the type 2 pattern and less than 1 mm in the type 3 pattern [3,7]. Furthermore, it is crucial to recognize the conditions that can induce BrPh without the presence of true BrS since BrPh is not associated with life-threatening arrhythmia and SCD [8]. In our patient’s case, we believe he had BrPh, which was modulated by his uncontrolled hypertension. A good history is essential to differentiate BrS from BrPh. It is equally important to exclude other causes of ST-segment elevation. In the absence of electrolyte abnormality, ischemic, or structural heart disease, our patient’s ECG during sinus rhythm revealed RBBB, normal QT interval, and persistent ST-segment elevation in precordial leads V1 and V2 during the episodes of elevated blood pressure, followed by resolution of the ECG pattern upon resolution of elevated blood pressure. Since the patient had evidence of type 1 Brugada pattern captured on a 12-lead ECG with no known history of documented ventricular fibrillation, polymorphic ventricular tachycardia, a family history of SCD at <45 years old, coved-type ECGs in family members, syncope, or nocturnal agonal respiration, we concluded that his ECG changes could be a manifestation of BrPh rather than BrS [7]. For similar reasons, an electrophysiology study was not performed to establish a diagnosis. To the best of our knowledge, this is the first case reporting hypertension-induced classical type 1 BrPh. Our case emphasizes the importance of recognizing the Brugada pattern in ECGs in young adults so that the inciting agents could be identified earlier and managed accordingly. While few medications, including quinidine and hydroquinidine, are known to offer some benefit to patients with BrS, the presence of spontaneous Brugada type 1 ECG pattern in the occurrence of symptoms warrants an implantable cardioverter-defibrillator [9]. In conclusion, early recognition and prompt intervention are of utmost importance in patients who demonstrate a Brugada pattern on ECG as it might be the first sign of impending SCD. The management of BrPh, on the other hand, lies in treating the underlying stress leading to the ECG change.
Conclusion
BrPh is an acquired form of BrS that can resemble Brugada-like ECG pattern in the presence of an underlying stressor. This is the first case reporting a suspected BrPh as a result of uncontrolled hypertension in which ECG tracing transforms from type 1 Brugada pattern to type 3 Brugada pattern with management of underlying stressors of hypertension.
What is new?
BrPh is an acquired form of BrS that can resemble Brugadalike ECG pattern in the presence of an underlying stressor. This is the first case reporting a suspected BrPh as a result of uncontrolled hypertension in which ECG tracing is transformed from type 1 Brugada pattern to type 3 Brugada pattern with management of underlying stressors of hypertension.




