Background
99mTc-Methylene diphosphonate (MDP) bone scan demonstrates the uptake in areas of abnormal bone turn over; therefore, it is used worldwide to image skeletal metastasis and various inflammatory pathologies, including avascular necrosis (AVN) of head of femur [1]. As there is increased uptake in the head of femur during the remodeling phase of AVN and metastasis, it can be misinterpreted as a metastatic lesion [2]. Different imaging modalities are used for the diagnosis of AVN, e.g. plain radiographs, magnetic resonance imaging (MRI), and 99mTc-MDP bone scintigraphy (BS) etc. MRI is considered a gold standard for diagnosis of AVN and can help in differentiation between AVN & skeletal metastasis [3]. We are reporting a case in which skeletal metastasis mimicked AVN on 99mTc-MDP BS.
Case Presentation
A 40-year-old female patient with right breast carcinoma was referred to the Nuclear Medicine Department of our hospital for 99mTc-MDP BS. She underwent right mastectomy, followed by chemotherapy and radiotherapy 4 years ago. She was on a wheel chair, unable to walk with primary complaint of pain in the left hip for the last 4 weeks. On general physical examination, her blood pressure was 110/70 mmHg, pulse rate was 78/minute, no fever, and chest was clear on auscultation. During routine work-up, her blood tests showed hemoglobin of 12.8 gm/ dl (normal 12-16 gm/dl), Total Leukocyte Count (TLC) of 7,500, blood sugar of 84 mg/dl, urea of 31 mg/dl (n = 10-50 mg/dl), creatinine of 0.6 mg/dl (n = 0.6-1.3 mg/dl), non-reactive HbsAg/anti-HCV, and normal Liver Function Tests (LFTs). Her chest X-ray was normal with normal abdominal ultrasound. Her left screening mammography was normal. She had her Dual Energy X-rays Absorptiometry scan done 1 year ago, which showed osteoporosis (T-score = −2.7). Her previous bone scan done 1 year ago was negative for skeletal metastasis. A 99mTc-MDP bone scan was conducted with Infinia dual head gamma camera equipped with low-energy high-resolution collimators at 140 Kev peak with a 20% energy window. It showed a focal increased uptake in the head of left femur and suspicion of AVN in the left head of femur was raised (Figure 1). She was advised MRI of hip joints by the treating physician, which showed hyper-intense signals with marrow changes in the head of left femur and acetabulum, suggestive of skeletal metastatic lesion (Figure 2). Follow-up bone scan after 1 year showed an abnormal increased uptake in the right parietal region of the skull, few ribs, and uptake in left head of femur, extending up to the trochanteric region with findings compatible with skeletal metastasis (Figure 3).
Discussion
AVN was first reported by Munro in 1,738 people, with poorly understood pathogenesis [4]. Extravascular pressure on small arteries and intravascular thrombosis are regarded as the common proposed pathogenesis [5]. Common sites involved head of femur, humerus, mandible, scaphoid, and talus bones. The head of femur is the most common site of AVN [6]. AVN of the head of femur is believed to be a leading causing of hip replacements, accounting for almost 10% of all hip replacements [7]. Non-traumatic causes of AVN are usually underappreciated, mostly involving young patients due to prolonged use of high dose steroids and cancer chemotherapeutic drugs [8,9]. Thrombosis in the arteries is commonly seen in cancer patients and may lead to AVN in the long run if there is involvement of the feeding vessel to the head of femur [10]. AVN may be asymptomatic, although it predominantly presents as local discomfort in the relevant joint, then progressing to painful restrictions of movements causing functional disability [11].
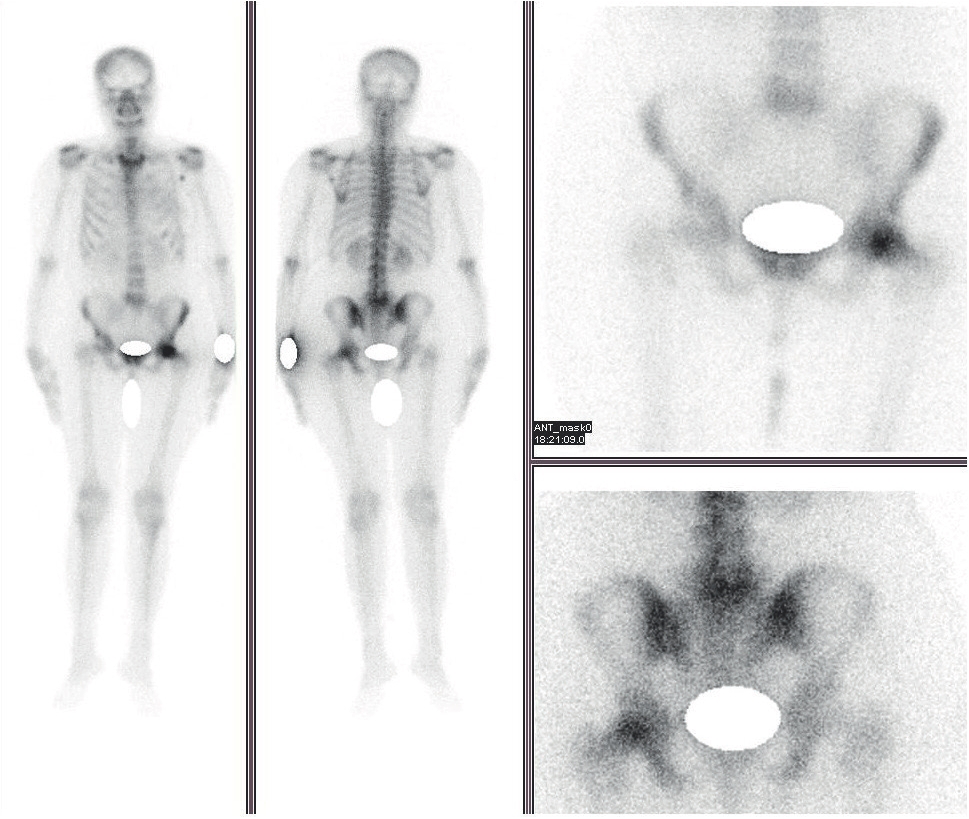
99mTc-MDP Bone scintigraphy showing focal increased uptake in the head of left femur with suspicion of AVN left head of femur.
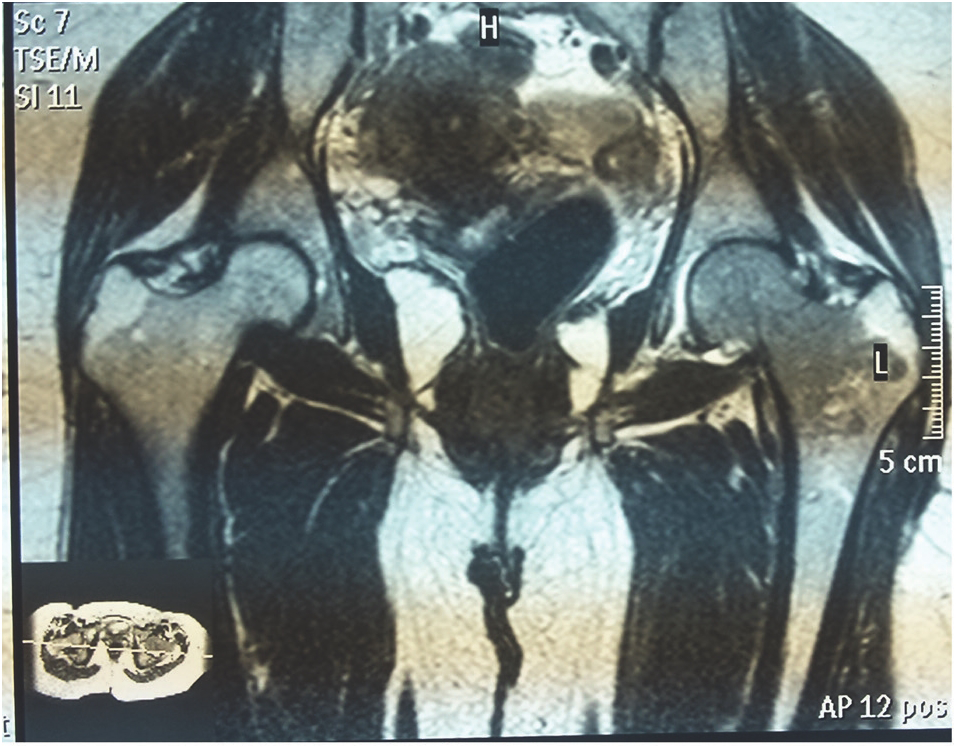
MRI (T1) of the bone and hip joints showing marrow signal changes in the head of left femur suggestive of a skeletal metastatic lesion.
Diagnosis of AVN is usually done with routine plain radiographs, 99mTc-MDP BS, Single Photon Emission computed tomography coupled with low dose CT scan (SPECT/CT) and magnetic resonance imaging (MRI). MRI is usually regarded as the gold standard for diagnosis of AVN, while BS is regarded as a primary tool for skeletal survey for skeletal metastasis in patients with malignant disorders [2,12].
Plain radiographs may not be helpful in the diagnosis of early AVN. In the advance stages of AVN, the plain radiograph may show mild demineralization to degeneration/flattening of the femoral head. SPECT/CT hybrid imaging can also be helpful in diagnosis of AVN. SPECT images may show avascular focus involving femoral head later replaced by increased activity in remodeling phase, with CT scan showing sub-chondral lucencies and sclerosis during the remodeling phase, before collapse of femoral head [13].
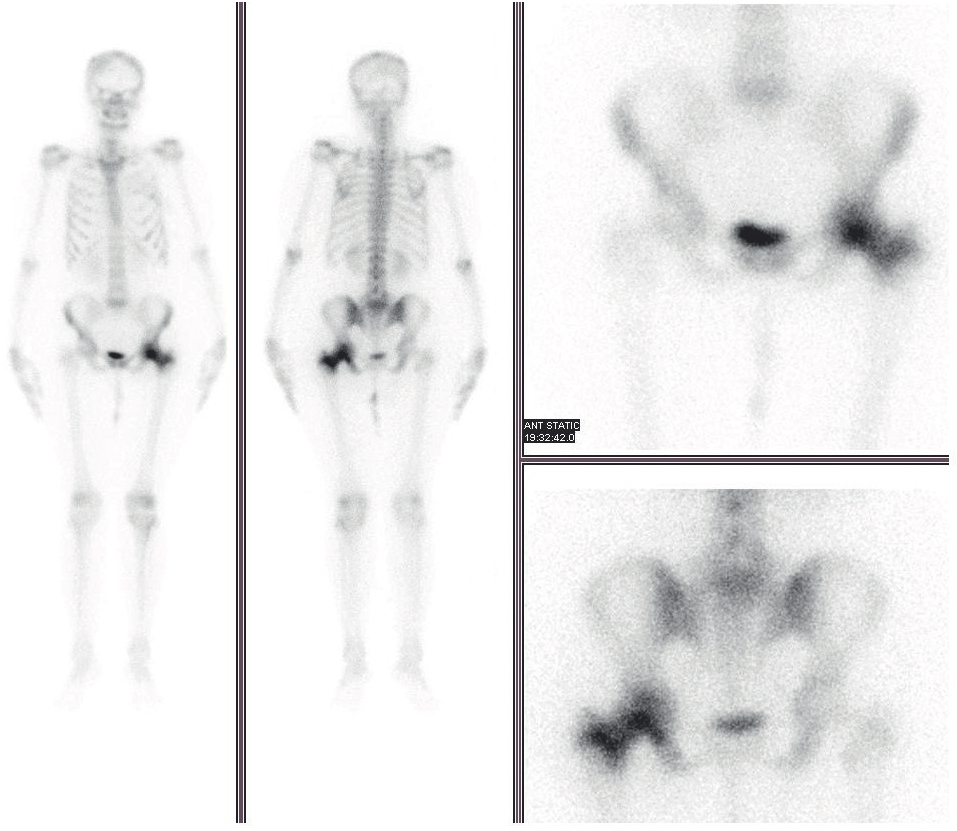
Follow-up 99mTc-MDP bone scintigraphy after 1 year showing an abnormal increased uptake in the right parietal region of skull and few ribs with an uptake in the left head of femur extending up to trochanteric region and compatible with skeletal metastasis.
Skeletal metastatic lesions primarily involve the axial skeleton, with less involvement of appendicular skeleton. The spine, pelvis, rib cage, and ends of long bones are regarded as the common sites of bone metastases due to high content of red marrow [14].
Bone scan is highly sensitive for osteoblastic bony lesions but has inherent low specificity [15]. All pathognomonic processes outlined by bone scan are analyzed by experts, based on experience and imaging atlas in mind. Based on their lifelong learning curves, and history of the patient with patterns, appearance and distribution of the lesions, they label a lesion as metastatic/malignant or non-metastatic/benign in nature. In case of ambiguity, further characterization usually needs correlative radiological imaging or histopathological confirmation. MRI showed hyper-intense signals with marrow changes consistent with a metastatic lesion involving the head and neck of the left femur rather than AVN [16]. This diagnosis was confirmed by longitudinal follow-up. Bone scan done after 1 year confirmed that a lesion in the head of femur was not AVN, i.e., no change in head of femur and hip joint space. Along with this, the appearance of multiple new lesions and extension of the focal lesion in the head of femur to neck/trochanteric region of femur confirmed it to be a skeletal metastatic disease.
Conclusion
A solitary skeletal metastatic lesion in the head of femur is a rare finding. In the presence of local symptoms with focal uptake in femoral head, AVN remains at the top of differential diagnosis. However, probability of skeletal metastatic lesion must always be considered in patients with known history of carcinoma. Bone scan is a primary tool for skeletal metastatic survey due to high sensitivity for osteoblastic response but exhibits low specificity in relation to disease-specific pathognomonic findings. MRI must be considered in such cases as a safe, non-invasive, and easily available option for further characterization of solitary lesions.
What is new?
Both skeletal metastasis and AVN show osteoblastic response when imaged with 99mTc-MDP BS. A solitary osteoblastic lesion in the head of femur on bone scan turning out to be a skeletal metastatic lesion is a very rare finding, making it a unique case not reported in the literature previously. They are totally different pathologies with different lines of treatment, as one is benign and other is malignant. In our case, a solitary osteoblastic lesion in the head of femur with local symptoms favored the AVN head of femur which on further workup with MRI turned out to be a metastatic lesion, causing a total change in the line of management. It shows the importance of correlative imaging for proper diagnosis.

