Background
Post-traumatic vestibular stenosis has functional and aesthetic implications. It is caused by deformed compromised anatomy of vestibular wall, which is comprised multiple anatomical defects, such as anterior septal deviation or caudal dislocation or prominent soft tissue of columella, disfiguration or misalignment of lateral cartilaginous support, and soft tissue stenosis secondary to excessive scarring. A thorough nasal examination is a part of the essential procedure in determining and establishing the cause of nasal stenosis. For this reason, failure to visualize the nasal cavity during the examination warrants at least a radiographic imaging to visualize the anatomy of nasal cavity as a part of diagnostic modality and also for surgical planning, if needed.
The treatment of nasal vestibular stenosis is challenging and difficult, particularly when dealing with soft tissue scarring as another insult to correct the abnormality may further predispose to more scarring, leading to re-stenosis [1]. Surgical repair requires resection of the scar tissue [2] and post-operative care should be intense to prevent the risk of re-stenosis [3]. This report highlights a novel post-operative care strategy to maintain a patent and functional vestibular opening using a glue gun stick to dilate the nasal opening, thus preventing re-stenosis.
Case Presentation
We report a case of a 26-year-old male who had allegedly involved in a motor vehicle accident sustaining a laceration wound over the left alar nasal sulcus requiring toileting and suturing in the outpatient department. A month post-trauma, he complained of persistent left nose blockage and was reviewed by our team. On examination, there was a well-healed scar over the left alar nasal sulcus. Anterior rhinoscopy revealed a narrowed right vestibular opening and pin-point opening of the left nostril (Figure 1). Minimal misting was observed on the right nostril and absence of misting over the left side upon cold spatula test. Rigid nasoendoscopy showed hypertrophy of right inferior turbinate with no other abnormalities. However, the rigid 25 mm diameter 0-degree scope was unable to be introduced into left nostril due to stenosis at the vestibular region. Computed tomography of paranasal sinuses showed a patent nasal cavity posterior to the stenosis. He later underwent a series of dilatation of the left nostril using Hegar dilators and resection of fibrous tissue using jumping-man Z-plasty technique under general anaesthesia.
A week post-operatively, the patient was instructed to perform daily nasal dilatation using a glue gun stick. The glue gun stick is a solid cylindrical stick of varying diameters designed to be applied with a hot glue gun for use in the application of the adhesive. In our patient, the glue stick of 7.0 mm diameter was used. For the purpose of dilating the nostril, the distal end of the stick was trimmed into a cone shape in order to ease introduction into the vestibular region until the vestibule was able to be dilated to the original diameter of the stick (Figure 2). In addition, lignocaine 2% gel was used to lubricate and ease the insertion of the stick as well as prevention of friction which could potentially add injury to the nasal mucosa. Regular daily dilatation of nasal vestibular opening was continuously advised for three consecutive months. At 3-month review in our clinic, he was able to introduce a 7-mm-standard size diameter of glue gun stick into both nostrils easily (Figure 3).
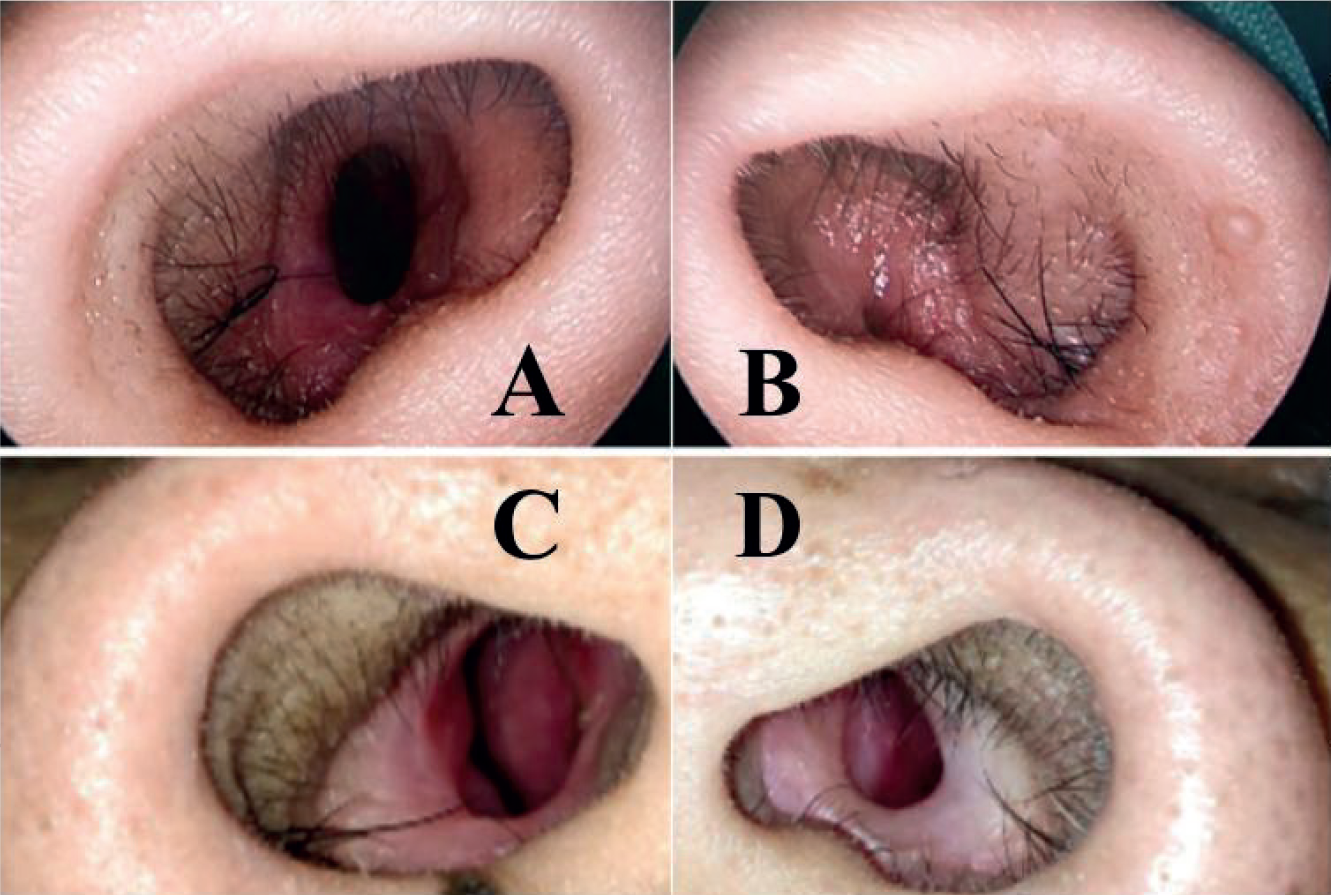
A right narrowed vestibular opening (A) and pin-point opening of the left vestibule (B) and the post dilatation opening of right (C) and left vestibule (D).
Discussion
Post-traumatic vestibular stenosis is not only disrupting its functional status and causing aesthetic concern for the patient, but also pose as a management challenge to the attending medical personnel.
The diagnosis of nasal stenosis is mainly clinical [4]; therefore, proper history and physical examination are crucial to ensure appropriate management. Patients with nasal vestibular stenosis often complain of perpetual unilateral or bilateral nasal blockage. However, unilaterality of nasal symptoms is the single most important historical factor that suggests a potentially dangerous nasal obstructive disorders [5]. Therefore, a thorough physical examination, including observation, anterior rhinoscopy, and nasal endoscopy are crucial to evaluate the nasal septum, the mucosa, the turbinates, and the entire length of nasal cavity up to the nasopharynx looking for any obstructive pathology [5].
Moreover, other factors that need to be assessed prior to vestibular repair include the width of the obstruction, the condition of the surrounding lining tissue, and the severity of external deformity [6]. However, limitation in visualizing the entire nasal cavity requires imaging study. In this case, computed tomography is the radiological diagnostic modality of choice though it is not routinely performed in clear cut cases of nasal vestibular compromise.
The spectrum of nasal stenosis may span from mild stenosis or narrowing to complete atresia [7]. Adamson et al. [4] categorize the degree of nasal stenosis into mild (10%–20% narrowing), moderate (20%–50% narrowing), and severe (>50% narrowing), which were determined based on physical examination. Despite the arbitrary of the classification system, it provides a crude assessment of the condition and assists in the description of the degree of stenosis present. Apart from that, a more detailed assessment proposed by Menger et al. [3] defined a three-level assessment of severity of nasal stenosis that is based on physical examination, photography and symptoms. The various classifications present in practice serve as a clinical aid in describing the pathology as there is limited literatures discussing specifically on the degree and severity of nasal narrowing.
Vestibular stenosis is typically due to an obstructive scar tissue that occurs as a consequence of excessive wound healing leading to an abnormal fibrotic scar formation. This results from the overproduction of fibroblast, collagen, elastin, and proteoglycans during the healing proses. This circumferential growth of scar tissue in the nasal vestibular region causes stenosis. Generally, the excision of the scar tissue alone is inadequate as the scarring process resulting from the excision will always show a tendency to reocclusion [2].
Z-plasty is a surgical technique performed to improve nasal vestibular stenosis, functional status, and the cosmetic appearance of scars [8]. Z-plasty involves the formation of two triangular flaps of equal dimensions that are then transposed to break the circular scar and redirect it into better alignment with the natural skin fold or in the lines with least skin tension [9]. The jumping man Z-plasty is a variation of the double-opposing Z-plasty that allows skin lengthening to be achieved in areas of limited adjacent skin laxity within scar contracture.
Other techniques used to surgically repair nasal stenosis secondary to cicatrix are split skin graft, full-thickness skin graft, and composite grafts [10]. However, Salvado and Wang [7] have reported a case of nasal vestibular stenosis treated by dilating the stenosis using Hegar dilators followed by the application of mitomycin C and the placement of stent. Mitomycin C is known to inhibit fibroblast proliferation and prevent collagen synthesis, which is one of the preventive measures used together with the stent placement.
Apart from that, vestibular stenosis has a high recurrence rate after surgical repair due to contracture during wound healing [3]. Postoperative scar contracture may occur in any surgical site due to a cascade of events present in wound healing and maturation. Excessive scar contracture may be caused by inherent problems in the physiological wound healing process, including the abnormalities in cell migration and proliferation, synthesis and secretion of extracellular matrix proteins and inflammatory cytokines, and the injury precipitated by the remodeling process [11]. Furthermore, the inward movement of the intact edges of the injured tissue which occurs during wound healing further adds to the tendency for the injured vestibule to contract, leading to stenosis. This is further exacerbated by the constant negative pressure generated by inspiratory forces on the nostril.
The use of the vestibular devices in post-operative management of vestibular stenosis has been described in many literatures for the prevention of re-stenosis, including the use of nasopharyngeal airway tubes, custom-made acrylic nasal stent, and silicone suction tube [12]. These devices are intranasal stent that have to be worn by patient at an interval period of time to ensure favourable outcome. These stents have shown satisfactory prevention of re-stenosis. However, they are not immediately available to cater for situation of a non-fitting device due to postoperative swelling, or a device that is too large or damaged, thus causing interruption to the patients’ rehabilitation period post-operatively [13].
In our case, we decided to use a glue gun stick, which is a form of thermoplastic adhesive that is commonly retailed as solid cylindrical sticks of varying diameters. It is readily available at local groceries with the standard size of 7.0 mm diameter and 11.0 mm diameter. As it is a readily available item coupled with its affordability, makes it an excellent alternative to the conventional devices to maintain post-operative nasal patency.
In our patient, rather than using the intranasal stent, we used this solid cylindrical glue gun stick in post-operative care for the prevention of recurrence of stenosis. Apart from its easy access, availability, and cost-effectiveness, we based on the principle that in vestibular stenosis, the need for continuous dilatation of the nasal vestibule in post-operative period is vital to properly mold the surrounding tissue at the stenotic region.
Our patient was not attached to any intranasal device which might otherwise decreased the mobility of the patient. Furthermore, the patient’s compliance with the daily routine of nasal dilatation using glue gun stick was excellent and this is very crucial in preventing the high incidence of re-stenosis.
As a result, our patient experienced marked improvement in his nasal blockage post-surgery and did not experience recurrence of nasal stenosis. The appearance of the left nostril, although appeared slightly smaller than the other side, was still satisfactory with no obvious functional problem. There was also better aesthetic outcome seen in our patient.
Conclusion
Post-traumatic nasal vestibular stenosis provides a demanding functional and aesthetic value that requires surgical intervention to correct the stenosis. However, it is equally important to maintain post-operative nasal dilatation to prevent re-stenosis. In our report, the use of glue gun sticks in post-operative care has shown benefits in the prevention of re-stenosis. Therefore, we also recommend for glue gun stick to be used as a prophylaxis in nasal laceration specifically in cases involving the inner musoca or nostril after toilet and suturing.
What is new?
Care and rehabilitation following surgical repair of post-traumatic vestibular stenosis with scarring tissue should be intense and meticulous as treatment failure and risk of re-stenosis is high. This report highlights a novel and cost-effective post-operative care using glue gun stick to maintain a patent and functional vestibular opening.



