Background
Malignant mesothelioma is a rare malignancy arising from mesothelial cells in serosal membranes. It often occurs in the peritoneum (30%), pleura (60%-70%), and other sites (<1%) [1]. Currently, the standards of care are cytoreductive surgery (CRS) with hyperthermic intraperitoneal chemotherapy (HIPEC) [1,2]. The optimal management of recurrent disease and particularly extra-abdominal recurrence remains unknown. This case report details the surgical management of a patient with recurrent malignant mesothelioma in the chest wall.
Case Presentation
A 34-year-old otherwise well female known to the peritonectomy unit for ongoing follow-up of malignant peritoneal mesothelioma was found to have recurrent chest wall disease. She first presented to the unit 3 years earlier and was managed with CRS and HIPEC. A full CRS was achieved with high volume disease peritoneal cancer index 31 and completeness of cytoreduction score 0. The sites of larger volume disease were in the lower ileum and the right iliac region. She received regular follow-up and imaging scans. At her 15-month follow-up, she developed abdominal wall recurrence in the left hypochondrium without intraperitoneal disease and underwent excision of the abdominal wall mass, re-do peritonectomy, and HIPEC. In both surgeries, HIPEC involved mitomycin C and cisplatin for 90 minutes at 41.5°C. Histopathology in both instances confirmed epithelioid-type malignant mesothelioma. Formal nodal status was not calculated, as the standard staging for peritoneal mesothelioma remains the PCI. In the first surgery, nodes from the gall bladder and small bowel/right colon mesentery showed reactive changes only. In the second surgery, peritoneal nodes again showed reactive changes only.
At 26 months after her second peritonectomy, the patient developed a left chest wall lesion. Tumor markers such as CEA, CA 19.9, and CA 125 were normal. A computed tomography of the chest, abdomen, and pelvis showed the recurrence of disease in the left anterior chest wall (7.2 × 1 × 1.3cm), which was confirmed with ultrasound-guided biopsies.
The patient was discussed at the multidisciplinary meeting (MDT) and was planned for a re-do peritonectomy and HIPEC, with excision of the left chest wall lesion, followed by postoperative radiotherapy. Intraoperatively, the chest wall lesion was found to be superior to the previous left hypochondrium site of disease and extended to the left anterior abdominal wall, splenic flexure, and lower ribs (Figure 1). The tumor was resected en bloc with the lower ribs, a portion of the left external oblique muscle, and the splenic flexure colon (Figure 2). Furthermore, tumor deposits were found in the right iliac region and retroperitoneum, which were resected. Left hemicolectomy was performed. HIPEC was administered for 90 minutes with mitomycin-C and cisplatin at 41.5°C. The abdominal wall was closed primarily. Her recovery was uncomplicated, and she was discharged 12 days postoperatively. Histopathology of the chest wall lesion confirmed the deposits of epithelioid mesothelioma involving skeletal muscle, abutting the hyaline cartilage likely originating from the rib. Three of five retroperitoneal lymph nodes were positive for epithelioid mesothelioma; the remaining lymph nodes from the splenic flexure and pericolic nodes showed reactive change only.
Discussion
Malignant peritoneal mesothelioma is a rare disease with an incidence of only 300-400 cases per year in the United States [1]. Without treatment, the disease is universally fatal with a median overall survival of 6-12 months [2]. With the advent of aggressive treatments such as CRS and HIPEC, the median survival has improved significantly to 34-92 months [3], with a reported median disease-free survival of 38.5 months after optimal cytoreduction and HIPEC [4].
In the event of peritoneal recurrence, the current standard of treatment is for repeated CRS and HIPEC [4,5]. There is no evidence of efficacy for systemic chemotherapy or radiotherapy for such disease [5]. Recurrence has also been reported in the abdominal wall at old laparoscopy or biopsy sites, likely due to surgical trauma or seeding of malignant cells to the abdominal wall [6,7]. However, the patient had an unusual recurrence in the chest wall, which was found to originate from the ribs rather than extending from a primary peritoneal lesion. The potential of the chest wall lesion representing a new primary such as pleural mesothelioma was considered; however, histopathology of the chest wall lesion demonstrated epithelioid mesothelioma identical to the biopsies taken from the original surgery, during which disease was confined to the peritoneum. Therefore, this patient was found to have an unusual extraperitoneal recurrence of her primary peritoneal mesothelioma. There is currently no documented literature on the management of such recurrences. Aside from surgical trauma and seeding of malignant cells, it is unclear why extraperitoneal recurrences occur. The genetic studies of patients with peritoneal mesothelioma have demonstrated mutations in NF2, BAP1, and CDKN2A; however, the significance of these mutations for recurrent disease is unclear, and thus, genetic testing is yet to become a standard clinical practice [8]. The patient had no family history of neurofibromatosis and did not undergo karyotyping during her treatment.
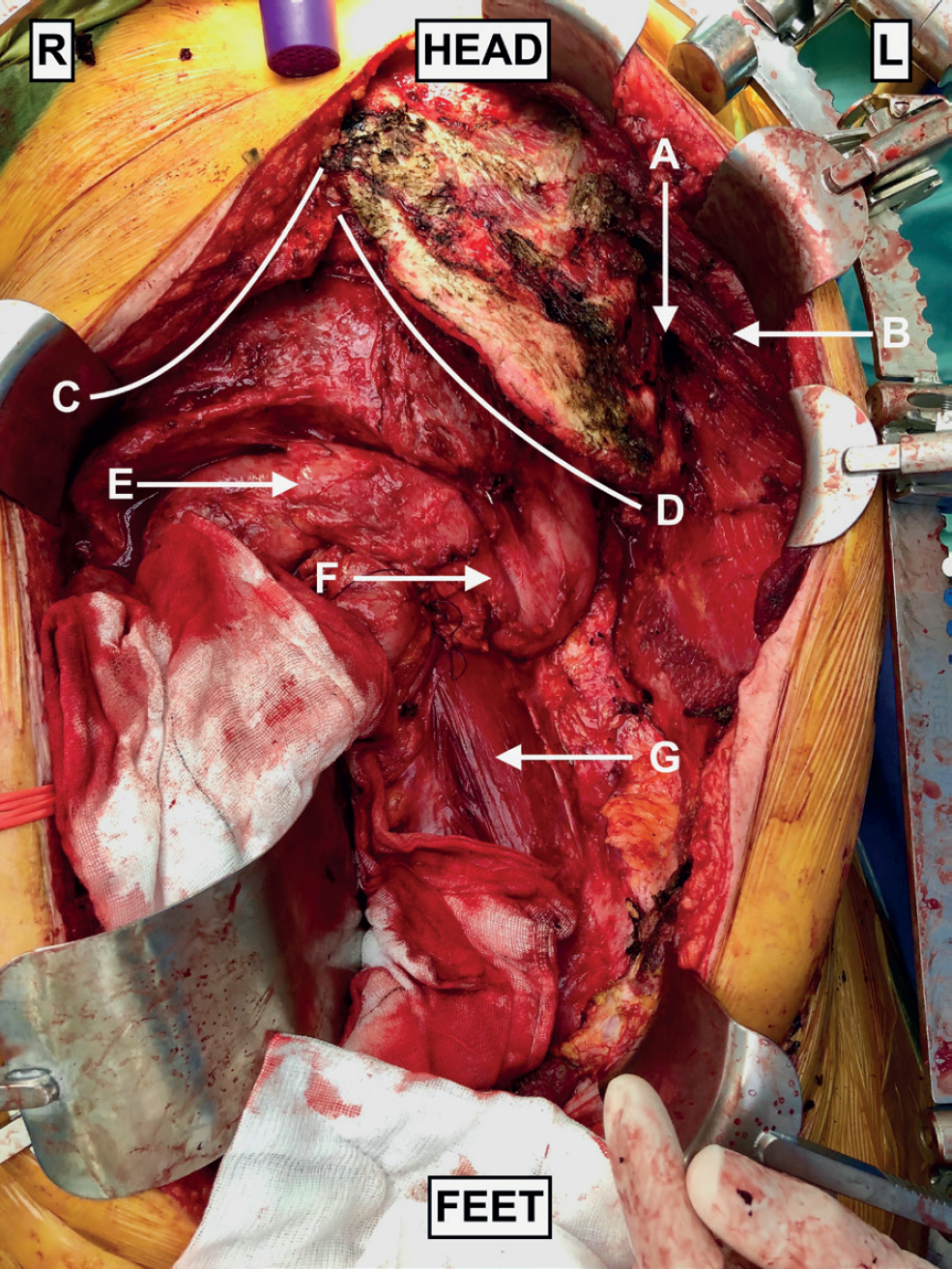
Post-excision of tumor. (A) Tumor excised. (B) Left external oblique muscle retracted laterally. (C) Right costal margin. (D) Left costal margin. (E) Transverse colon. (F) Stomach. (G) Left psoas.
The surgery enables complete excision of tumor deposits, but it increases the risk of ventral hernias particularly with the excision of abdominal wall musculature. With disease originating from the ribs, excision carries a high operative risk due to injury to the lung, intercostal muscles, and diaphragm during resection. External beam radiotherapy may be an option but is limited by its adverse effects such as radiation pneumonitis, radiation enteritis, and chest wall excoriation [9]. The efficacy of systemic or intraperitoneal chemotherapy in cases of mesothelioma recurrence is known to be limited even in peritoneal recurrence [5]. A trimodal approach of surgery, followed by adjuvant chemotherapy and radiotherapy, has been described as a potential treatment for recurrent pleural mesothelioma in the chest wall; however, this approach to treatment is considered experimental and yet to be evaluated in large scale trials or peritoneal origin disease [9].
The patient did not receive adjuvant systemic chemotherapy or radiotherapy with her initial two surgeries. The main reasons for this were the lack of evidence for systemic chemotherapy or radiotherapy and the use of intraoperative HIPEC. Radiotherapy was initially considered as an adjuvant option after her second operation given the recurrent disease; however, due to the risks of radiation enteritis, the decision was made not to proceed. Radiotherapy was considered after the third operation again. As this represented the patient’s second recurrence of disease, the decision was made to undertake radiotherapy. However, there is no evidence for or against radiotherapy in this rare situation, and the treatment decision was made based on the peritonectomy unit’s multidisciplinary team (MDT) meeting’s expert advice and discussion with the patient.
Conclusion
Extra-abdominal recurrence of peritoneal mesothelioma remains a rare and unusual site of disease. The peritonectomy unit utilizes an MDT approach to tailor an individualized treatment plan for such complex peritoneal mesothelioma cases. This patient was discussed at the MDT meeting, and a decision was made for redo-peritonectomy with HIPEC and post-operative radiotherapy to the chest wall to reduce recurrences. We suggest that an MDT approach remains the standard of care in such patients given the paucity of data and lack of standardized approaches to the management of these rare cases.
What is new?
Little is known regarding the management of extra-peritoneal recurrence of peritoneal mesothelioma. The case report details the management of chest wall recurrence of peritoneal mesothelioma with surgery and adjuvant radiotherapy within an MDT setting. There are no other known reports of such a clinical case.


