Background
The incidence of myoma in pregnancy is approximately 2%, and only one-tenth of these presents with some complication [1]. Myoma in pregnancy commonly complicates as pain, spontaneous abortion, preterm labor, preterm rupture of membranes, or abruptio placentae, but pyogenic inflammation is rare. Infections may arise through ascending infection of the lower genital tract, endometritis, contiguous extrauterine pelvic infection, hematogenous, or lymphatic spread of any distant infection [2]. The clinical diagnosis is often missed or delayed as it mimics the syndrome of “painful myomas,” which is mostly thought as red degeneration or hemorrhagic infarction. A thorough search of the literature shows only a few cases during pregnancy, and most of them presented with fever and leukocytosis and led to abortion or iatrogenic preterm delivery [3]. Although mild hydronephrosis is physiological in pregnancy, the literature shows the cases of obstructive uropathy and renal dysfunction in association with comorbidities such as twin gestation, polyhydramnios, and some renal anomalies or rarely with uterine leiomyoma [4]. However, to the best of authors’ knowledge, this patient is the first case, where pyomyoma manifested as deranged renal function with acute kidney injury due to obstructive uropathy in pregnancy. The patient was managed with a lower segment cesarean section along with drainage and enucleation of pyomyoma.
Case Report
A 30-year-old female, second gravida presented to the emergency room at 33 weeks’ gestation with 10 days of abdominal pain, fever, and vomiting. The pain was continuous and localized to the lower abdomen and bilateral flanks. The perception of fetal movements was adequate with no history of bleeding or leaking per vagina. On examination, moderate pallor was noted along with tachycardia. Abdominal examination showed distended tensed uterus with fundal height corresponding to 36 weeks’ size. The uterus was relaxed but tender. The fetus was in cephalic presentation with a normal fetal heart rate. Blood pressure and urinalysis were normal. Initial laboratory test results detected anemia (hemoglobin 8.0 g/dl), normal white blood cell (WBC) count, and liver function test. The renal function test had a marked derangement with blood urea nitrogen (BUN) being 76 mg/dl and serum creatinine of 2.6 mg/dl, with normal electrolytic values. An abdominopelvic sonogram revealed normal fetal biometry and amniotic fluid for gestational age. An ill-defined heterogeneous soft tissue was noticed in the pelvic cavity, causing mass effect over the posterior wall of the uterus, which was not seen separately. Bilateral hydroureteronephrosis was also noted. Magnetic resonance imaging pelvis revealed an abdominopelvic mass of approximately 18 × 11 cm with peripheral T1 hyperintensity and diffusion restriction and bilateral hydroureteronephrosis with extension (Figure 1). On the basis of symptoms, laboratory tests, and imaging studies, a large degenerating myoma with obstructive uropathy was clinically suspected. The patient was treated with adequate hydration with supportive antibiotic and analgesic medications avoiding nephro-toxic drugs. Blood, urine, and vaginal swab cultures were obtained. The detail investigations to look for the cause of fever were done. Temperature and output records were maintained. All culture reports were negative. No definitive cause of fever was found. The patient was kept on expectant management, but her subsequent laboratory tests showed a marked ascendency of WBC counts (27,000/ml deterioration of RFT with BUN −104 mg/dl and serum creatinine of 3.6 mg/dl. Her general condition worsened over 3–4 days despite aggressive supportive therapy. In view of acute kidney injury with the worsening condition due to mass effect of myoma, the decision for emergency laparotomy with cesarean section was taken after appropriate counseling and informed consent.
Laparotomy was performed with midline vertical infraumbilical incision, and a fetus weighing 1,700 g was delivered by the lower segment cesarean section. On pre-operative examination, the posterior surface of the uterus was covered with flakes of mucopus and adhered to bowel loops which were released. There was an irregular ragged mass of approximately 16 × 10 cm extending from the posterior surface of the uterus to the right side broad ligament. It had friable degenerated tissues with purulent collection within it, which was spontaneously draining suggestive of ruptured pyomyoma (Figures 2 and 3). Around 50 ml of pus collection was seen in the pelvic cavity which was drained. The right tube and ovary were edematous and covered with mucopus, whereas the left tube and ovary were normal. The pyomyoma was enucleated, and optimum hemostasis was ensured. Peritoneal lavage was done followed by intraperitoneal drain insertion.
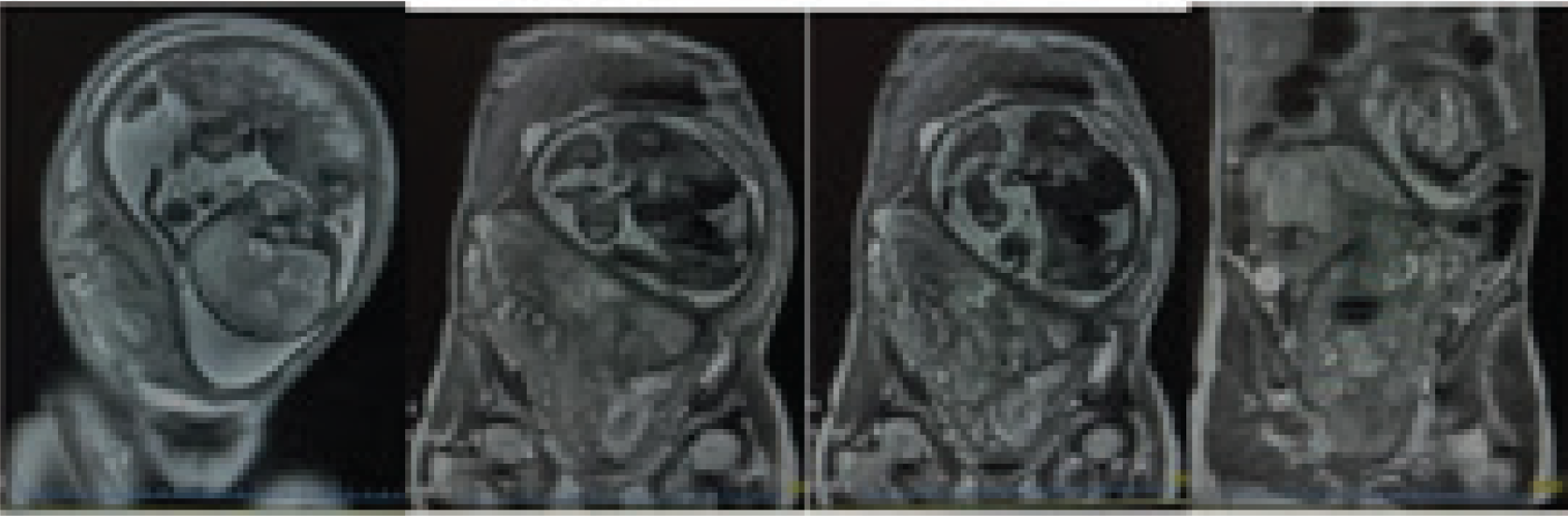
MRI abdomen and pelvis: Ill-defined abdominal mass with peripheral T1 hyperintensity, diffusion restriction, and fibroid red degeneration.
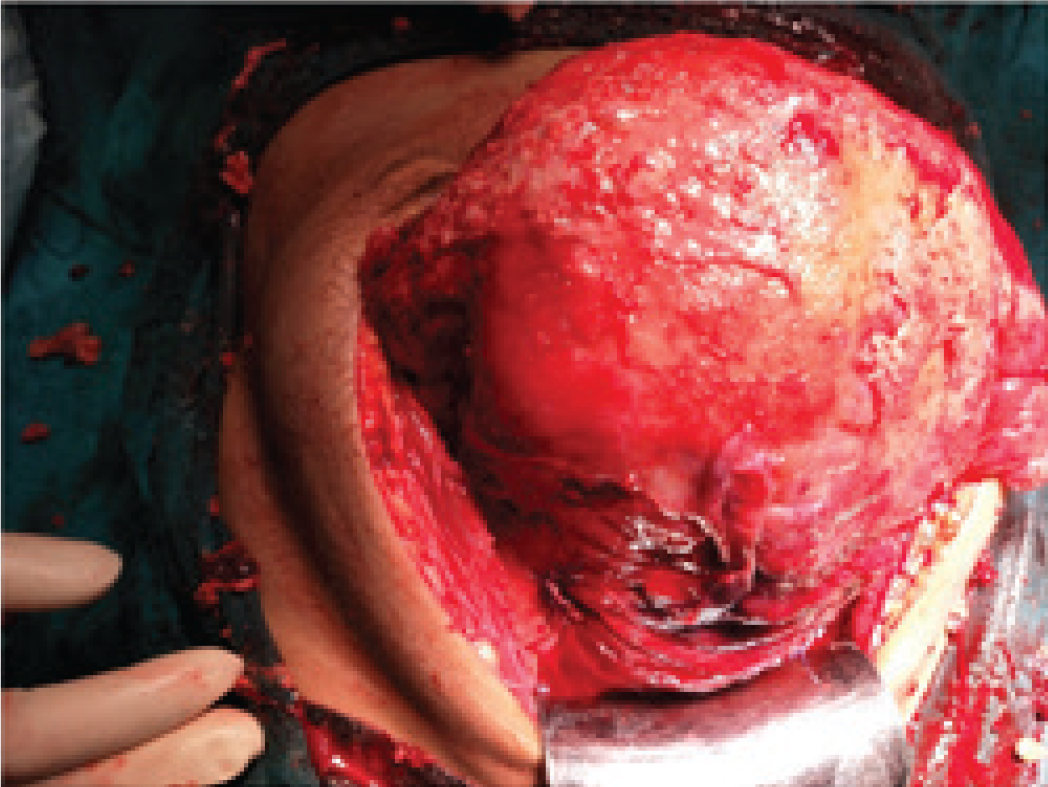
Intraoperative picture showing the posterior irregular surface of the uterus and pus flakes.
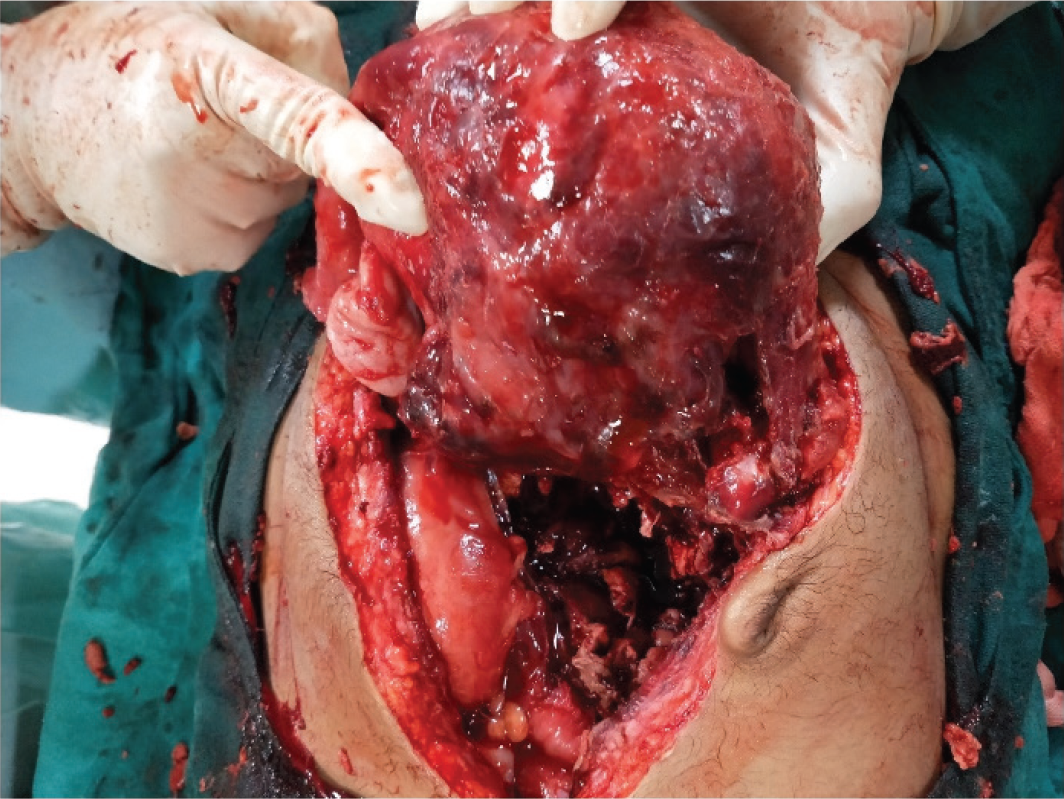
Intraoperative picture showing the posterior irregular surface of the uterus after drainage of pyomyoma.
In post-operative period, her fever subsided within 48 hours. RFT started to improve and became normal within a week of surgery. The mother and baby were discharged in satisfactory condition on 11th post-operative day. The histopathology report showed the areas of coagulated necrosis, hemorrhage, and fibrinous exudate confirming degenerated pyomyoma (Figures 4 and 5). Pus and placental culture report detected Coagulase-negative staphylococcus as a causative agent of infection confirming a possible spread of infection from the endometrium.
Discussion
Pyomyoma is a pyogenic infection of leiomyoma due to infarction and subsequent infection in myoma. It is unusual and associated with high morbidity and maternal mortality if diagnosis or treatment is delayed. The patient was promptly treated which led to optimum clinical outcome. Around 50 cases of pyomyoma have been reported to date with mortality rate of approximately 11% [5]. Pyomyoma has been seen in both reproductive and postmenopausal women, but most of the cases are linked to pregnancy, which highlights an increased tendency of suppurative myoma during pregnancy. The onset of symptoms is insidious and often presents in postdelivery or post-abortal period as fever, pain, or sepsis. Prahlow et al. reported pyomyoma at 12 weeks of gestation in a woman with intravenous drug abuse. Exploratory laparotomy was performed for suspected adnexal torsion or tubo-ovarian abscess, where perforated pyomyoma was demonstrated [6]. Only four cases of pyomyoma have been reported as being diagnosed during pregnancy, and only one case has been reported till date by Kobayashi et al. with successful myomectomy in the second trimester and continuation of pregnancy till term [7]. Grune et al. could diagnose pyomyoma during pregnancy at 26 weeks of gestation by ultrasound-guided puncture of myoma which showed the growth of pathogenic organism. The patient underwent a cesarean section with subsequent myomectomy as sepsis did not respond to conservative management [8]. Ruch et al. performed an emergency laparotomy at postpartum day 1 for suspected acute appendicitis which revealed ruptured pyomyoma [9]. Kobayashi et al. managed a case of leiomyoma with high-grade fever and suspicion of peritonitis at 21 weeks of pregnancy by performing laparotomy which revealed pyomyoma. Myomectomy was done which led to the conservation of pregnancy till term. Hence, in all cases, diagnosis and treatment necessitated surgical intervention.
The triad of leiomyoma, pain, and fever of unknown origin points toward a high probability of infected myoma, but, sometimes, unusual presentation delays its diagnosis. The imaging studies may not characteristically differentiate it with other pelvic masses. The management of suspected pyomyoma must be individualized considering the maternal condition and gestational age. Early surgical intervention along with antibiotic therapy might improve obstetric outcome. Fertility preserving surgery involving myomectomy or pyomyoma drainage are reasonable options in early trimester [10]. In the present case, deteriorating renal function with sepsis led to an emergency cesarean section which revealed perforated pyogenous myoma. The fetus could be salvaged as it was mature enough for delivery.
To conclude, pyomyoma is unusual, and diagnosis is mostly missed in pregnancy due to vague and nonspecific symptoms. Definitive diagnosis and treatment are possible with surgery, pathological examination, and bacterial culture growth. Although the administration of antibiotic forms cornerstone in management, surgical therapy is essential for the complete cure of pyomyoma. Further studies are needed to establish guidelines for early diagnosis and treatment in case of suspected pyomyoma during pregnancy.



