Background
Uterine artery embolization (UAE) is an effective and minimally invasive approach to treating symptomatic uterine fibroids in a certain cohort of patients [1]. Since the publication of the first series of bilateral uterine artery embolization for fibroids in 1995, this approach has been widely utilized, and there is now level 1 evidence to this as a low cost yet effective treatment with symptom control even up to 5 years after treatment [2,3].
Aortic dissection is a potentially life-threatening vascular event with an estimated incidence of 5 in 100,000 [4]. Intimal tear leads to blood flow into a false channel within the inner and outer layers of the aortic media, which may result in critical occlusion of branches of the aorta, or rupture. Approximately, 18% of cases are associated with underlying connective tissue disease (CTD), such as Marfan’s Syndrome and Ehlers–Danos [5]. Though not formally contra-indicated, interventional arteriography, including uterine artery embolization is considered high risk in patients with CTD [6]. This is due to the perceived increase risk of vascular complications, such as dissection and rupture associated with CTD, both within the target and transient vasculature, but also at the arteriotomy. To the author’s knowledge, there are no reported cases of uterine artery embolization in the setting of aortic dissection or CTD.
Case Presentation
A 44-year-old female was referred from an external institution for consideration of uterine artery embolization in the setting of known large uterine fundal fibroid. The fibroid was associated with menorrhagia, pelvic pain, and urinary frequency. Ultrasound demonstrated increase in the dominant fibroid size (444 to 684cc) over 6 months. The patient had been considered for a total abdominal hysterectomy; however, she was deemed high risk for surgery in view of Stanford type B thoracic aortic dissection 10 months prior (Figure 1a–c) and morbid obesity.
MRI aortogram demonstrated the aortic intimal flap with luminal patency in the renal and visceral branches. The true lumen was stenotic in the lower abdominal aorta (Figure 2), and the intimal flap extended to the right common iliac artery (Figure 1c), with no flow from the true lumen beyond this, and the false lumen supplying flow to the remainder of the right leg. The flap did not extend to the left internal iliac artery, and thus the left leg flow was from the true lumen. The dissection had been treated conservatively and remained stable at serial imaging over a period of 9 months. Other relevant medical history included: morbid obesity (Body Mass Index 37); pregnancy 2 years prior complicated by pre-eclampsia and gestational diabetes mellitus, emergency Caesarian section, and post-partum hemorrhage; past history of vesicoureteric reflux complicated by recurrent urinary tract infections and renal calculi. Additionally, the patient reported an allergy to contrast associated with angioedema, including facial and tongue swelling occurring after the initial CT imaging during her acute aortic presentation (necessitating MRI for follow-up).
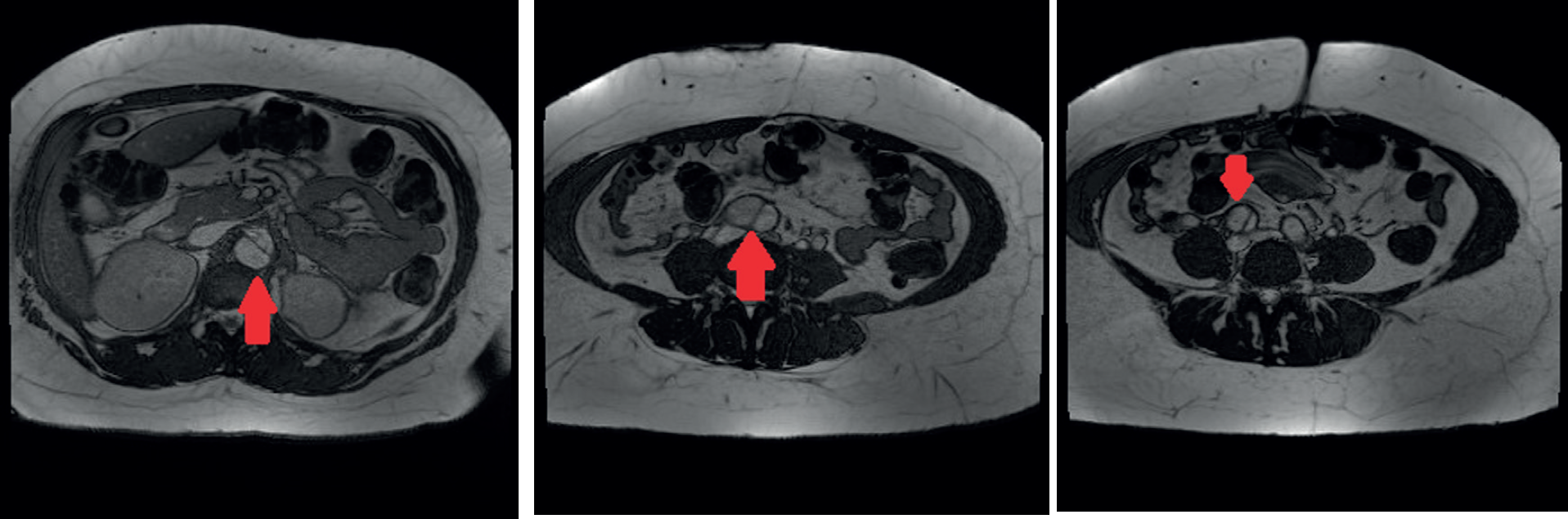
Axial T2-weighted MRI showing type b dissection flap (arrow) in the visceral abdominal aorta (a), aorta at its bifurcation (b), and in the right common iliac artery (c).
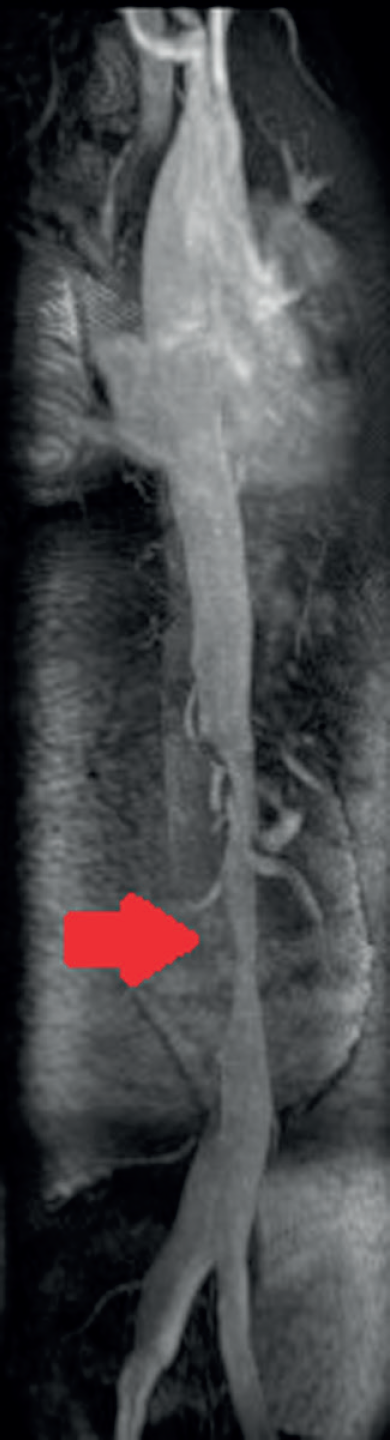
Coronal T2-weighted MRI showing true lumen associated with the Stanford type B dissection, and the area of infrarenal aortic stenosis (arrow).
Although the patient was not aware of any formal connective tissue disease diagnosis, it was suspected that an underlying connective tissue disease was likely in view of the combination of aortic dissection and urinary reflux, and the patient was referred for further genetic investigations which are still pending.
The patient was seen in the Interventional Radiology Outpatient Clinic, anesthetics pre-admission clinic for preparation, and pre-medicated with oral prednisolone 50 mg, two doses prior to the procedure, and oral cetirizine 10 mg, for contrast allergy. This is in line with our hospital protocol for contrast allergy pre-medication.
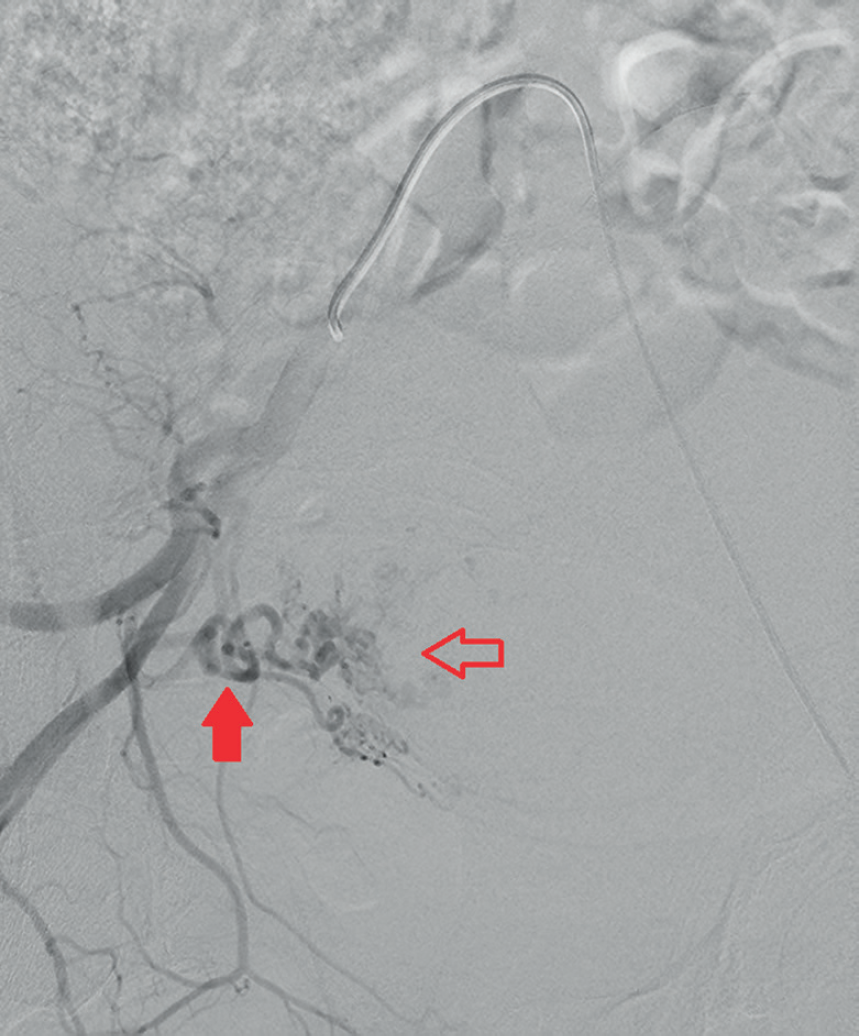
Overhill right internal iliac angiogram showing enlarged right uterine artery (arrow) and filling of the large uterine fibroid (open arrow).
The procedure was performed under intravenous conscious sedation provided by an anesthetist. Given the altered flow dynamics to the right leg, the left common femoral artery was accessed using a modified Seldinger technique and a 5-French sheath inserted. Overhill access to the right internal iliac artery was obtained with an 0.038″ catheter (Rim, Merit Medical, USA) (Figure 3), followed by super selection of the uterine artery with a microcatheter (Progreat 135 cm 2.7 Fr, Terumo, Japan) and embolization with 355–500 micrometer PVA particles, in the standard manner for uterine fibroid embolisation. Given the stenotic lower abdominal aorta, a Waltman loop was felt to be difficult to perform and the rim catheter did not provide enough stability to facilitate an ipsilateral internal iliac artery approach. The catheter was, thus, changed for a dedicated uterine artery catheter (UAC2, Merit Medical, USA). Although the true lumen stenosis made this a challenge, this was able to be formed in the lower aorta and passed into the internal iliac artery (Figure 4). The ipsilateral left uterine artery was then super selected with the microcatheter and also treated with PVA particles.
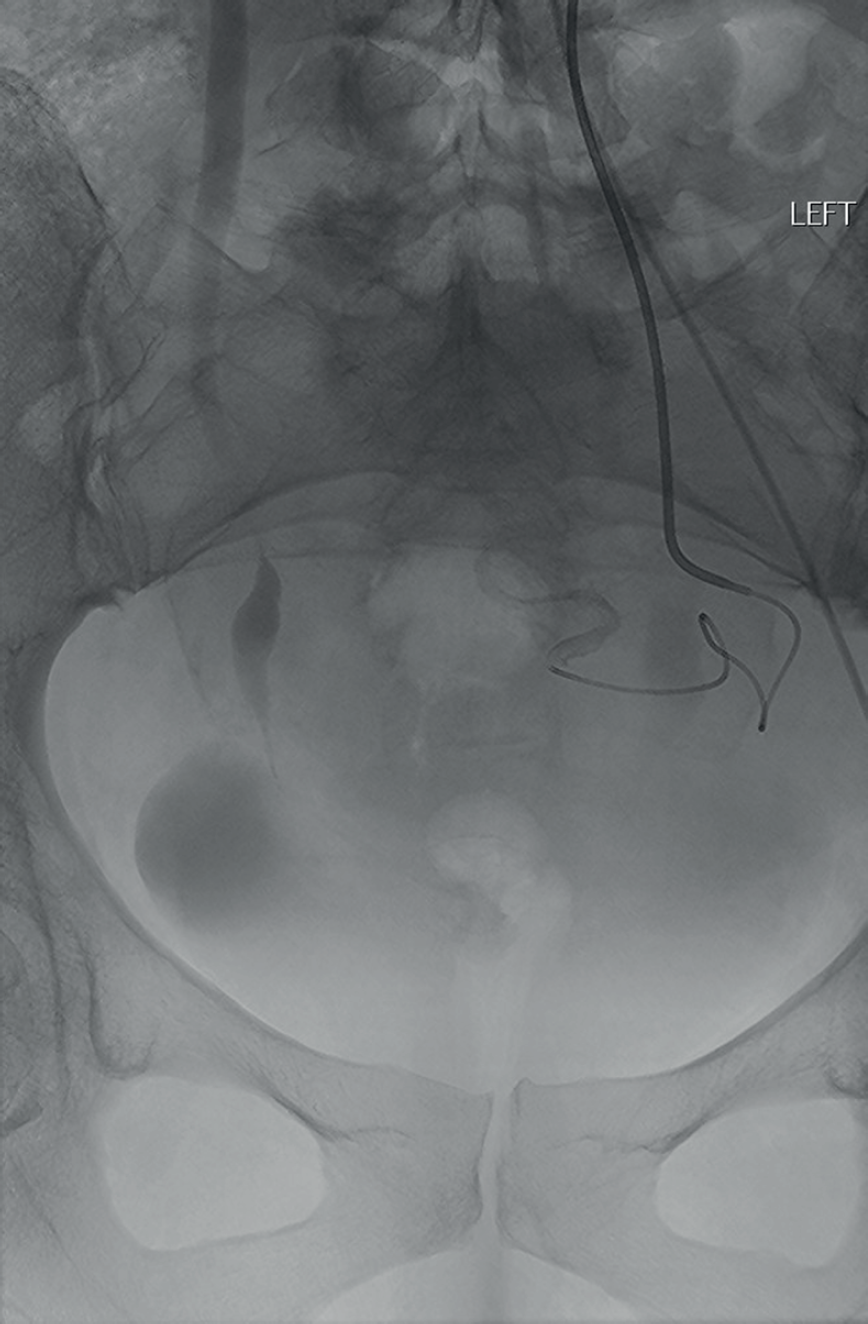
Ipsilateral left internal iliac artery access using UAC2 catheter (Merit Medical) and microcatheter to the uterine artery.
An Angio-Seal closure device (Terumo, Japan) was used at the conclusion to close the arteriotomy and was deployed without complication (confirmed with on-table ultrasound after deployment). The patient was discharged on day 1 post-operative with mild post-embolization syndrome [2]. At 6-week clinical follow-up, the fibroid remained avascular on transabdominal ultrasound and the patient reports improvement in menorrhagia. The patient otherwise remains clinically silent to any further vascular abnormalities.
Discussion
Patients with a history of aortic dissection are a challenging population for the endovascular proceduralist. Frequently, interventional angiography, including UAE is considered relatively unsuitable in patients with CTD [7,8]. However, there is a lack of evidence to guide treatment approach to symptomatic uterine fibroid in this population. Indeed, to our knowledge, no prior case reports describing UAE in a patient with CTD are available and we acknowledge that treatment via open (hysterectomy or myomectomy) or endovascular approaches in this complex patient presented a risk with either approach.
In the general population, UAE offers a safe, effective, and economical alternative to medical or surgical management in the treatment of symptomatic uterine fibroids with similar improvement in quality of life at 5 years after treatment in either surgical or UAE groups, and with fewer major complications. This is offset by more minor complications and a greater need for re-intervention at 10 years after treatment [1,2,8,9].
Although there is limited literature on the subject, it is reasonable to assume that both UAE and surgery are associated with higher rates of complications in patients with CTD. Indeed, the HOPEFUL study [1] found that “medical comorbidity” predisposed to post-operative morbidity in both patient groups, though did not investigate the impact of connective tissue disease specifically. Successful surgical management of uterine fibroid in a marfanoid patient has previously been reported [10], but there are no previous case reports of UAE in similar patients.
This case is not without points of limitation to mention. It is reasonable to consider that in this patient, at 10 months after the aortic event, the intimal flap is scarred / fibrous and indeed the catheter feedback supported this during the case with the lower aortic true lumen stenotic but firm to catheter manipulation. It is encouraging to see that catheters can be successfully looped in the aorta even with the inherent stenosis and may have been helped by the iliac-specific catheter used (UAC2, Merit Medical). An ipsilateral approach with a smaller reverse curve catheter may have been an alternative possibility in some patients with appropriate internal iliac artery size and angulation. The risk of dissection associated with femoral access, and the use of a closure device is also a concern but did not materialize in this patient. In this patient, the dissection flap made access from the right common femoral artery difficult and also removed potential for radial access, something that often benefits patients with elevated body mass index. As the flap did not involve the left iliac system, this side remained available for access and both internal iliac and uterine arteries were normal, resulting in otherwise normal delivery of embolic material once the upstream vascular obstacles were negotiated.
This case report describes successful UAE for symptomatic uterine fibroids in the setting of type B dissection and a potential diagnosis of CTD. Connective tissue disease or chronic type B dissection may not need to be a deterrent to offering this or other endovascular treatments in the non-acute setting. In particular, patients who wish to retain their uterus or who are averse to the risks of major surgery should be considered candidates for endovascular uterine treatment with appropriate counselling of the risks and benefits of both approaches.
What is new?
Uterine fibroid embolization is an established treatment for symptomatic uterine fibroids. However, it is recommended to avoid endovascular procedures in those with connective tissue disease or aortic dissection. We describe a successful case of treatment in this setting, discuss reasons, and risks of alternative treatments.

