Background
Multiple myeloma (MM) and non-Hodgkin’s lymphoma (NHL) are lymphoproliferative disorders. The simultaneous presentation of both MM and NHL is a rare association of lymphoproliferative disorders [1]. In this case report, a patient who presented with both disorders is discussed. Clinical presentations and features of MM and NHL are variable. The coexistence of MM and NHL can be defined with several different possible pathogenic mechanisms [2]. Pathological studies and immunohistochemistry staining studies were conducted to diagnose NHL B-cell lymphoma. Multiple myeloma was documented with bone marrow biopsy. In 1994, Geun Chan Lee et al. [2] described a patient presenting with petechiae, melena, and weight loss, which was later identified as coincidental MM and NHL.
Case Presentation
A 69-year-old man with a history of hypertension and Benign prostatic hyperplasia (BPH) presented with abdominal pain, weight loss, and melena during the last 7 months. Abdominal pain was general and without radiation. Nausea and vomiting during abdominal pain were reported. There was no fever, skin rash, lymphadenopathy, and hepatosplenomegaly on examination. On examination, he appeared ill, pale, and cachectic. Complete blood count showed hemoglobin 8.6 g/dl, WBC 9.4 × 103/ μl, RBC 4.37 × 106/μl, Hematocrit (HCT) 29.5%, Mean corpuscular volume (MCV) 67.51 μl, Mean corpuscular hemoglobin (MCH) 19.68 pg, Mean corpuscular hemoglobin concentration (MCHC) 29.15 g/dl, and Platelet (PLT) 183 × 103/μl. Other lab studies showed albumin 4 g/dl, creatinine 1.2 mg/dl, Lactic Acid Dehydrogenase (LDH) 428U/l, Erythrocyte sedimentation rate (ESR) 40 mm/hour, and Ca 9 mg/dl.
There was no significant endoscopic finding in esophagogastroduodenoscopy. The colonoscopy report was normal too. Computed tomography scan (CT-scan) indicated a long, rigid, narrow loop with irregularities bound in the distal of the jejunum. The filling defect of the jejunum was compressive-induced because of the extreme increase in thickness. The CT scan findings suggested an infiltrative mass or lymphoma in the small intestine (Figure 1).
To conduct pathological studies, imaging-guided core needle biopsy was done. The specimen consisted of two thread-like fragments of soft white tissues, totally measuring about 20 × 0.1 cm. Microscopic studies demonstrated fragments of a neoplasm composed of large pleomorphic rather than discohesive cells. Immunohistochemistry studies showed the diffuse positive immunostaining of tumor cells by Leukocyte Common Antigen (LCA), CD20, PAX5, CD10, Bcl6, and Ki67(about 95%), scattered positive reaction with MUM1 and Bcl2, and negative staining with CD3, PanCK, and ALK1. According to these studies, a malignant non-Hodgkin B-cell-type lymphoma was diagnosed. Because of continuous complaints of melena, the patient was admitted for small bowel segmental resection. Another pathological study was conducted after resection. The specimen consisted of two portions of the small intestine (M: 23 × 4 and 10 × 2 cm). The external surface of a large portion in the middle area of the meso showed a tumoral mass (M: 8 × 4 × 3 cm). One section of the tumor was in the submucosa with fish-flashy consistency and it had invaded the total intestinal wall. Microscopic findings in pathological studies suggested that the neoplastic tissue consisted of solid sheets of medium-sized lymphoid-like cells with vesicular nuclei, prominent nucleoli, and scanty eosinophilic to clear cytoplasm. Immunohistochemistry staining studies indicated negativity for Creatine kinase (CK) and vimentin and positivity for CD45 and CD20. CD3 was positive in some cells. The small bowel segmental resection was considered as the treatment plan for this patient. Rituximab in combination with cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP) chemotherapy was prescribed for six sessions for preventing the relapse of NHL [3].
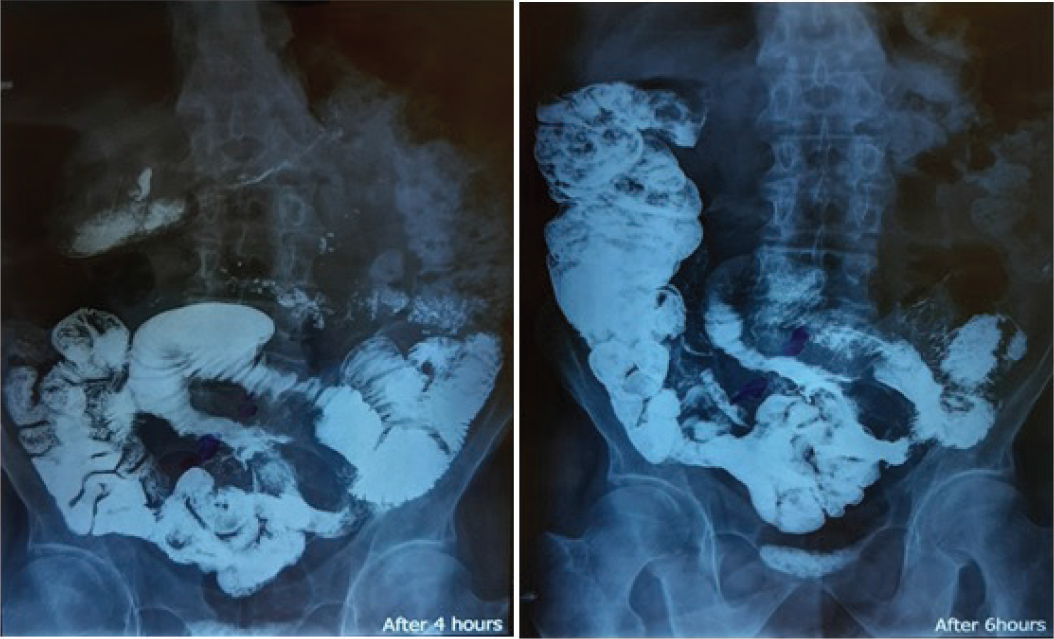
CT scan indicated a long, rigid, narrow loop with irregularities bound to the distal of the jejunum.
Bone marrow biopsy, bone marrow aspiration, and peripheral blood smear were conducted for NHL staging. Bone marrow aspiration smear revealed 1% myoblast and 35%–40% plasma cells. Myeloid maturation was shifted to the left and megakaryocytes were decreased (Figures 2–4). According to the classification system of NHL, the subtype of NHL in this case report was diffuse large B-cell lymphoma (DLBCL). Based on the staging system for NHL, which is known as the Lugano modification of the Ann Arbor staging system, this case was stage IE NHL. Bone marrow biopsy showed that 30% of cellularity consisted of trilineage hematopoietic cells. Many areas of the plasma cell sheets and aggregations were identified. According to these findings, a diagnosis of MM was made.
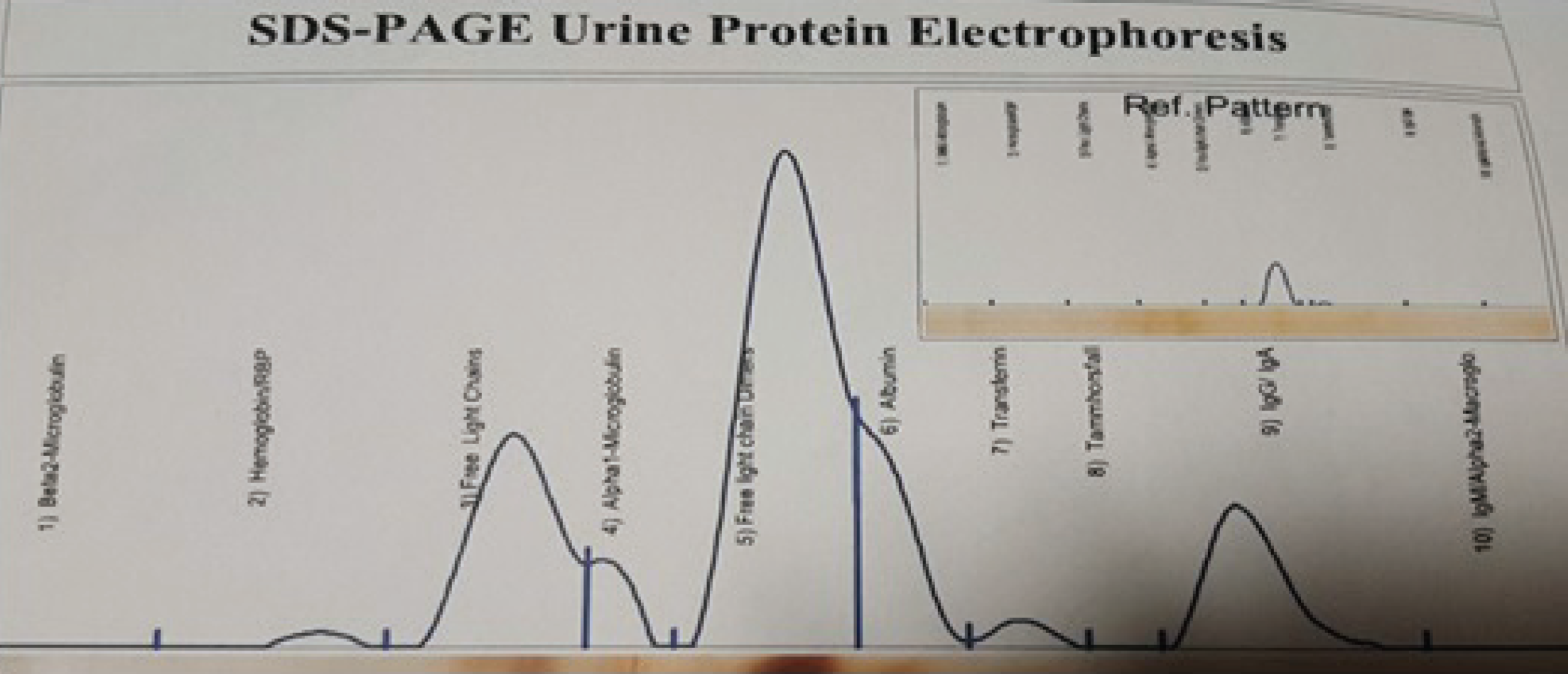
SDS-PAGE urine protein electrophoresis showing the presence of a monoclonal free light chain protein.
With regard to MM, according to these initial results, Sodium dodecyl sulfate page (SDS-PAGE) urine protein electrophoresis showed the presence of a monoclonal free light chain protein (12.3 mg/dl; Figure 5). Serum protein electrophoresis was normal. Although there was no clinical sign or symptom leading to MM and the patient did not mention any skeletal pain, a whole body bone scan was carried out as a workup for MM and it reported to be normal.
Treatment was directed toward NHL because of intestinal bleeding, which is a life-threatening condition. The patient tolerated the treatment well, melena was treated due to the surgical resection, and Hb was in the normal range.
Because the NHL in this case report is extranodal, the treatment response cannot be evaluated and monitored according to the Response Evaluation Criteria in Solid Tumors (RECIST) and Lugano criteria.
Discussion
The non-Hodgkin’s lymphoma is a major category and a diverse group of the lymphatic system’s tumors and neoplasms [1]. DLBCL is the subtype of NHL, diagnosed in this case, which is the most common histologic subtype of NHL [4]. The clinical presentations and features of stage I extranodal DLBCL can be variable due to the involved organs [5].
The principal characteristics of MM are neoplastic proliferation of abnormal plasma cells in the bone marrow and the production of monoclonal immunoglobulin [6]. The clinical presentations of MM are a variable spectrum of features from asymptomatic to severely ill [7].
In this case report, the patient was diagnosed with NHL. Bone marrow biopsy and urine protein electrophoresis fulfilled criteria for MM. In the bone marrow biopsy, there were localized collections of plasma cells and 30% of cellularity consisted of trilineage hematopoietic cells.
The simultaneous coexistence of both MM and NHL as a rare association of malignancies in the patient suggests specific studies about the possible translocations that can define the possible mechanism of this coexistence.
This case also offers additional support for studying more rare cases with regard to the association of lymphoproliferative and hematopoietic malignancies in order to compare the details of clinical presentations and features. Although these cases are rare, comparisons of similar cases can lead to opportunities for understanding proper clinical management and treatment.




