Background
Sarcomatoid carcinoma (SC), also known as spindle cell carcinoma and polypoid squamous cell carcinoma, is a rare variant of squamous cell carcinoma characterized by dysplastic surface squamous epithelium along with an invasive spindle cell element [1]. It can occur at any age from 20 to 90 years with a definite male predilection. The clinical presentation is mostly exophytic and polypoid, but the nodular or endophytic appearance has also been described [1]. SC shows a biphasic histologic appearance with epithelial changes varying from dysplasia to invasive carcinoma and stromal component composed of fusiform or spindle-shaped cells. SC is an extremely rare tumor of the sinonasal tract with only 13 cases reported since 1957 in the literature [2,7].
Case Presentation
A 79-year-old male reported to the oncology department with the complaint of soft tissue growth in the left side of the oral cavity for 1 year which was painless but increasing rapidly in size (Figure 1). It was associated with dysphagia. The biopsy showed it as SC. The patient had Eastern Cooperative Oncology Group (ECOG) performance status three on presentation with the bulging left cheek. The patient was nonsmoker, non-diabetic, or hypertensive.
The patient was investigated with contrast-enhanced Computer Tomography (CT) face and neck that showed a well-lobulated heterogeneously enhancing soft tissue density mass infiltrating left maxillary antrum with the destruction of inferior, anterior, medial, and lateral maxillary wall with the involvement of left-sided hard palate as well as maxillary alveolus (Figure 2). the incidental finding of a mass lesion at the point of confluence of the right and left hepatic ducts with dilated right and left hepatic ducts was made on quadruple-phase CT scan which is highly suspicious for Klatskin’s tumor. Furthermore, biopsy and histopathological confirmation of this lesion was not possible due to the patient’s condition. A biopsy of mass from the oral cavity was done, which showed malignant spindle cell neoplasm. The location of tumor and focal cytokeratin positivity favored SC. The bone scan showed the foci of abnormal radiotracer uptake in manubrium and multiple ribs bilaterally—compatible with skeletal metastases (Figure 3). The rest of the metastatic workup was unremarkable. Hence, the patient was diagnosed as SC of the maxillary sinus with skeletal metastasis.
The case was discussed in a multidisciplinary meeting, and the patient was referred to an orofacial surgeon, but the surgeon refused surgical resection due to the age and performance status of the patient.
The patient was given palliative radiotherapy 50G/20fx. Six months post-radiotherapy, patient’s quality of life is better, and he is doing well.
Discussion
SC is a rare variant of squamous cell carcinoma characterized by dysplastic surface squamous epithelium along with an invasive spindle cell element [1]. Different authors have different views regarding the histogenesis of SC and have used various terms to describe it. Virchow (1864) first reported it and labeled it as carcinosarcoma, suggesting that it may be a “collision tumor” between carcinoma and sarcoma [3]. Krompecher (1900) proposed an epithelial origin with “dedifferentiation” to a spindle cell morphology and used the term “SC” to describe it. Lane (1957) proposed the term “pseudocarcinoma,” suggesting that it may be a squamous cell carcinoma with an atypical reactive stroma. This multiplicity in nomenclature indicates the complexity of its histogenesis [1].
It has a wide age of occurrence ranging from 2nd to 9th decade and a mean age during the 5th decade with a predominant male predilection [7]. Although most tumors in the head and neck region occur in the larynx, in the oral cavity, it has a site predilection for the lower lip, tongue, and alveolar ridge or gingiva. Vishwanathan et al., in their study of 103 cases of SC, reported an incidence of 17.5% in the larynx and 63.1% in the oral cavity [4]. In the larynx, true cords and the supraglottic areas are the predominant sites of occurrence with the subglottic area being an unusual location. Pyriform sinuses are the preferred site in the pharynx as are nasal cavity and maxillary antrum in the sinonasal tract [9].
Because of its rarity, tumor histogenesis, clinical course, and resulting prognosis, its management is debatable [10]. The treatment of choice is radical surgery [4–6]. Prognosis has been better in patients treated with surgery and adjuvant radiation therapy [6]. Radiotherapy might be administered for the postsurgical palliation of local recurrence. Carcinosarcoma at the maxillary sinus confers a poor survival rate and a high local recurrence rate.
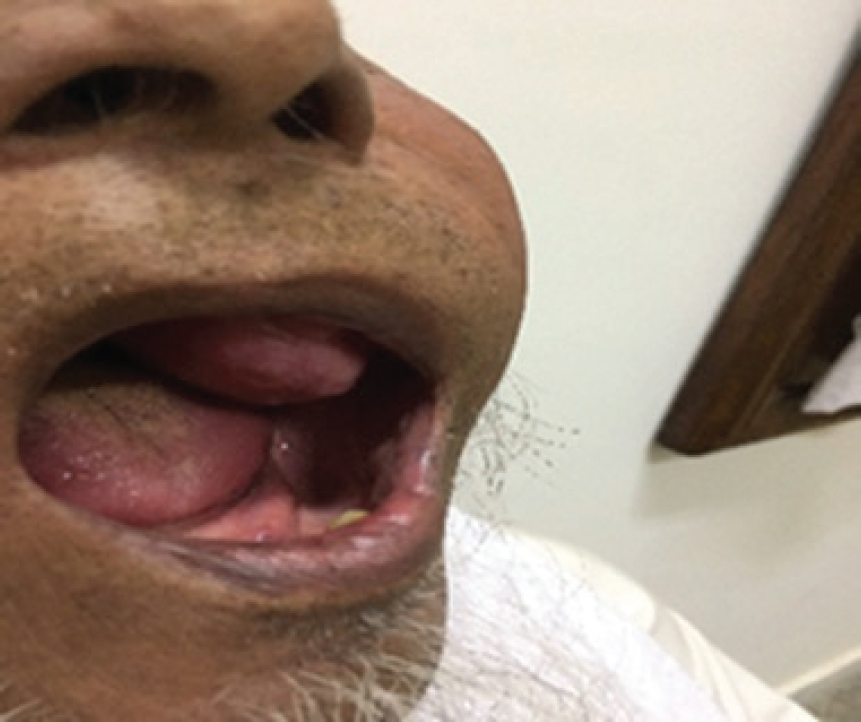
Clinical presentation of the patient. A polypoidal growth hanging into the left side of the oral cavity.
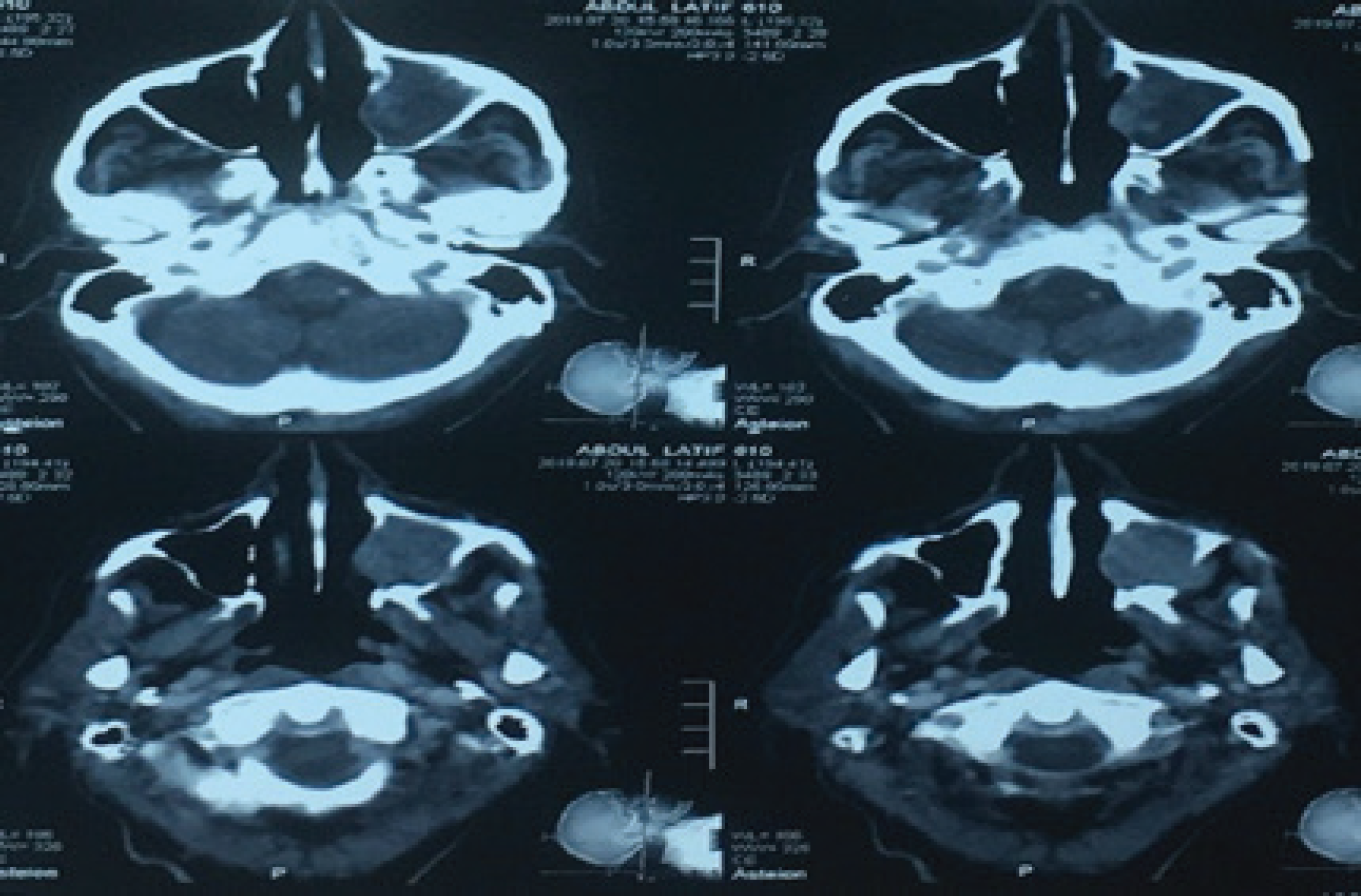
CT manifestation of tumor showing well-lobulated heterogeneously enhancing soft tissue density mass infiltrating left maxillary antrum with the destruction of inferior, anterior, medial, and lateral maxillary wall with the involvement of left-sided hard palate as well as maxillary alveolus.
Conclusion
Carcinosarcoma of maxillary sinus due to its rarity, tumor histogenesis, clinical course, and resulting prognosis is difficult to manage. Ideally, it should be managed in multidisciplinary meetings via surgical resection and radiotherapy according to the performance status of the patient. The patient can benefit from radiotherapy if this tumor is unresectable.
What is new?
SC of the maxillary sinus is a rare tumor with few cases reported, and less is known about its adequate management. Radical surgical resection followed by radiotherapy has been described in the literature as an optimal approach for its management. In the present case, age and poor performance were the factors limiting the optimal management, so radiotherapy alone was delivered to the patient leading to better disease control, quality of life, and manageable adverse effects.


