Background
Psychotic disorders secondary to organic pathologies affecting the central nervous system are due to a general medical condition. Organic causes include central nervous system infections, space-occupying lesions, metabolic and immune diseases, and intoxications [1]. The secondary causes should be considered especially in cases with atypical symptoms, no previous psychiatric or family history, atypical onset (e.g., advanced age), accompanied by neurological symptoms, or suspected imaging or laboratory findings [2]. However, secondary causes are infrequent (3%) in patients with first-episode psychotic symptoms, and the presence of more than one secondary cause might make it difficult to recognize the clinical condition [3]. In that case, there may be significant disruptions in the treatment of the patient. Herein, we present an acute and transient psychotic disorder with multiple secondary causes affecting the central nervous system at the same time.
Case Presentation
Mr. A, a 55-year-old male patient, married. The patient was brought to the emergency department by his relatives because of his thoughts that he would be abused and his relatives would kill him, and his aggressive behavior. These complaints were going on for 3 days. His first complaints started after loss of consciousness and an epileptic seizure in June 2010 and Mr. A was hospitalized in a neurology clinic with a pre-diagnosis of meningitis, encephalitis, and epilepsy. He had visual hallucinations within 1-month treatment. Although the hallucinations of the patient who received antiepileptic treatment regressed, focal or generalized seizures continued for at least once a month. In December 2010, status epilepticus developed and he was readmitted to a neurology clinic. After the seizures, violent verbal and physical behaviors, forgetfulness, and paranoia had begun and thyroid autoantibody elevation was detected during the follow-up, and the patient was diagnosed with Hashimoto’s encephalopathy. He was treated with levetiracetam, levothyroxine, and methylprednisolone. The patient’s psychiatric complaints completely improved at discharge. He did not have any complaints for about 8 years, but then fatigue and forgetfulness began and lasted for 3 years (these complaints are either directly compatible with the finding of Hashimato’s encephalitis or may have arisen secondary to depression related to a general medical condition. No medical evaluation has been made with regard to these complaints). Ten months before his present admission, he had complaints of unhappiness, despair, inability to enjoy life, and feelings of guilt after a psychosocial stressor. However, there is no history of psychiatric/medical evaluation or treatment for these complaints. While these complaints continued, focal seizures started and the patient was brought to the emergency room. In the first neurological examination carried out in the emergency department, no emergency neurological pathology was considered and the patient was admitted to the psychiatry clinic. In the mental state examination; confusion, deterioration in place and time orientation, decreased spontaneous and voluntary attention, short-term and long-term memory pathologies, agitation, insomnia, paranoia, and persecution delusions were detected. The patient’s insight, abstraction, and evaluation of reality were partially damaged. There were no motor deficits or reflex pathologies. The patient was hospitalized with a preliminary diagnosis of acute and transient psychotic disorder; it was decided to reinvestigate the secondary causes due to the presence of confusion and disorientation. For agitation and violent behaviors, haloperidol 5 mg/days was given to the patient. The patient’s medical history revealed Hashimoto’s thyroiditis and type 2 diabetes mellitus. In the laboratory examination, blood count, sedimentation, vitamin B12, fasting blood glucose, and C-reactive protein levels were within normal limits. In the thyroid function tests, free T3 was 2.16 pg/ml, free T4 was 1.42 pg/ml, thyroid-stimulating hormone was 1.743 uIU/ml, anti-thyroglobulin (anti-Tg) antibodies were 10,450 U/ml, and anti-thyroid peroxidase (anti-TPO) antibodies were 33,180 U/ml. The patient’s EEG examination was reported as “a slowing of ground activity with slow waves in theta rhythm, more prominent in the frontal region, but no active epileptiform activity.” Cranial magnetic resonance imaging (MRI) showed, in T2A sequences, nonspecific focal hyperintensities in the bilateral cerebral hemisphere, periventricular and supraventricular white matter, and aberrant vascular structure with regular calibration at the hippocampal sulcus level, causing a slight indentation in the hippocampus. Cortical sulcus and fissures deepened at the vertex level and cerebellar foils appeared to be prominent. On diffusion-weighted sequences, there was no restricted diffusion (Figure 1). With all these findings, Hashimoto’s encephalopathy was considered as a preliminary diagnosis and consulted endocrinology, neurology, and infectious diseases departments. To exclude infectious causes, the patient underwent lumbar puncture. In cerebrospinal fluid (CSF) examination, CSF appearance was clear, 120 erythrocytes were observed on microscopy, leukocytes and bacteria were not seen, CSF glucose was 74 mg/dl, and total protein was 1,007 mg/l. There was no growth in CSF culture. Empirically, intravenous acyclovir treatment was initiated. The patient was started on methylprednisolone (1,000 mg/days) for a preliminary diagnosis of Hashimoto’s encephalopathy. The patient responded well to this treatment and an improvement was observed in the general psychiatric condition. Particularly, agitation and paranoid delusions decreased. On day 5 of treatment, herpes polymerase chain reaction (PCR) results were “herpes simplex virus (HSV) type1 DNA positive, HSV type 2 DNA negative”. After that, methylprednisolone treatment was discontinued and dexamethasone treatment was started for anti-edema treatment and intravenous acyclovir treatment was continued. During follow-up, confusion, orientation, attention, and memory disturbances improved. Agitation regressed and haloperidol treatment was gradually discontinued on the ninth day of hospitalization. There was no psychotic finding.
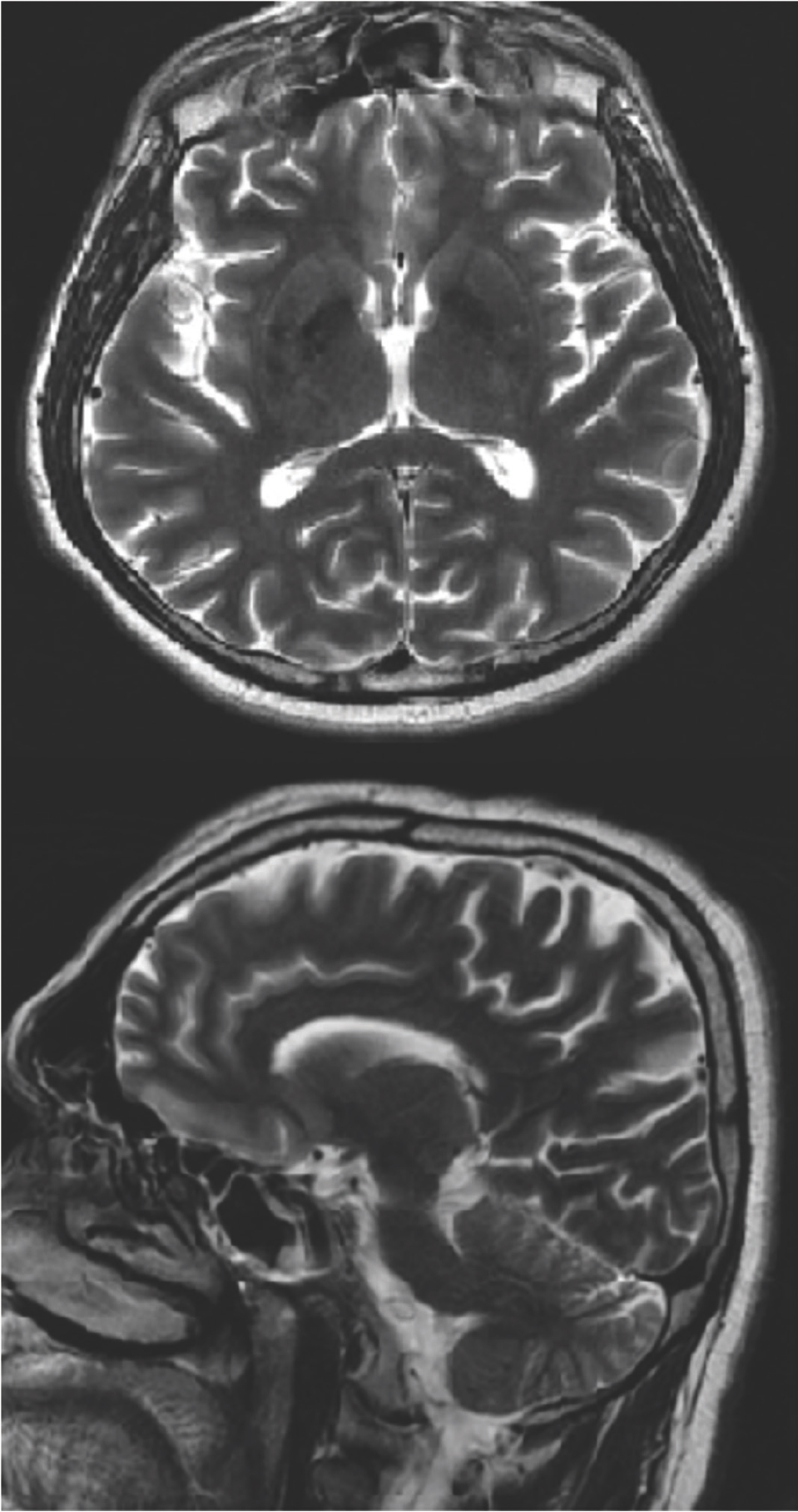
Cranial MRI showed that in T2A sequences, nonspecific focal hyperintensities in bilateral cerebral hemisphere, periventricular and supraventricular white matter, and aberrant vascular structure with regular calibration at the hippocampal sulcus level but causing a slight indentation in the hippocampus. Cortical sulcus and fissures deepened at the vertex level, and cerebellar foils appear prominent.
Discussion
The brief psychotic disorder is defined in DSM-5 as the presence of one or more psychotic symptoms with a sudden onset and full remission within 1 month [4]. Although the prevalence varies in studies, it is estimated to be 0.05% [5]. It is mostly observed in stressed groups. It is also more common in women and personality disorders. In the differential diagnosis, psychotic cases related to the general medical condition must be distinguished [6]. In this case, it was planned to reevaluate the secondary causes due to the presence of non-typical confusion and orientation disorders in the dramatic clinical picture of brief psychotic disorder and the patient’s medical history. Although the patient had been evaluated by neurology in the emergency department, it took time for some neurological symptoms to become apparent in some disorders related to CNS and psychiatric symptoms may be in the foreground in the clinical picture. When investigating the secondary causes, side effects related to levetiracetam and carbamazepine treatment were first considered. Various psychiatric symptoms, including psychotic symptoms with levetiracetam, may occur as side effects [7,8]. Secondly, it was thought that psychotic symptoms might have been caused by an epileptic seizure. As a matter of fact, psychosis develops in 2%–7% of epilepsy patients [9]. In the EEG examination, the slowdown in frequency and theta waves supported this view and in consultation with neurology, levetiracetam was discontinued and valproic acid was started to make better the antiepileptic effect and to reduce possible side effects. After hippocampal lesion was detected in MRI examination, it was thought that psychotic symptoms might be secondary to this lesion. Because the relationship between hippocampal abnormalities and psychosis has been shown previously, it has been suggested that these abnormalities might predispose to psychosis, affect the progression of the existing psychotic picture, or occur secondary to psychosis-related environmental factors [10]. However, there was no evidence of how this lesion occurred and its clinical significance. The Department of Neurology and Neurosurgery planned to follow-up the lesion every 6 months with cranial MRI. It was thought that the patient may have had a recurrence of Hashimoto’s encephalopathy due to the presence of psychotic symptoms (36%, reported in Hashimoto’s encephalopathy) [11], a history of epileptic seizures [12], rapid response to the steroids [13], a previous history of Hashimoto’s encephalopathy in the medical history, and especially high autoantibodies [11-13]. Hashimoto’s encephalopathy is a clinical condition characterized by elevated thyroid autoantibodies, stroke-like episodes, seizures, status epilepticus, impaired consciousness, dementia, or psychosis. Autoimmune mechanisms are thought to be involved in its pathogenesis and therefore respond rapidly to steroid treatments [14]. Therefore, steroid treatment was started on the third day of hospitalization. The patient who was consulted for infectious diseases and was started on prophylactic acyclovir was diagnosed with herpes encephalitis on the fifth day of hospitalization. Most encephalitis, including herpes encephalitis, begin with psychiatric symptoms before clear neurological symptoms appear [15]. As in our case, HSV encephalitis characteristically included the temporal lobe, particularly hippocampal lesions [16]. In this case, there were clues based on the clinical status and medical history, suggesting that the symptoms of brief psychotic disorder were secondary causes. However, the presence of acute onset psychotic symptoms, lack of apparent neurological symptoms, inadequate evaluation of the patient due to agitation, or complicated clinical appearance due to overlapping medical reasons led to the overlook of possible medical causes of psychotic symptoms and the patient to be directed to psychiatric treatment. Although secondary causes are rare in acute psychotic conditions, adequate evaluation of these causes and observation of suspected cases in the emergency department for a certain period are recommended. Especially, in cases such as herpes encephalitis, the mortality rate is up to 70% when appropriate treatment is not given, and the importance of this is clear [17].
What is new?
In this case, medical conditions causing acute psychotic symptoms occurred simultaneously (epilepsy, Hashimoto’s encephalopathy, and herpes encephalitis). In addition, the leading symptoms of these three medical conditions were acute and severe psychotic symptoms, suggesting a psychiatric illness rather than a medical condition.

