Background
Hamartomas are rare benign lesions that have been reported throughout the body. They usually develop in adulthood. This suggests that they represent benign neoplasms, a contention supported by some molecular studies [1].
Seromucinous hamartoma (SH) was first described in 1974 by Baillie and Batsakis, but only in the past few years that it has clearly characterized [1]. In the sinonasal cavity, hamartomas have been designated as epithelial, mesenchymal, and mixed. Each of these characteristic features will show overlapping features of multiple types [1]. Herein, we report two additional cases of SH that partly expand their histologic spectrum and review the typical histologic features, differential diagnosis, and literature pertaining to these interesting lesions.
Case Presentation
Written informed consent was obtained from the patient, as well as Institutional Board Review approval. A 50-yearold man, with a personal history of heart attack, high blood pressure, dyslipidemia, pancreatitis, and cholecystectomy, presented with a progressive nasal obstruction at the right side and hyposmia for the last 10 years, which worsened for the last 2 years. The patient denied epistaxis, drainage, enlarging mass of the neck, or facial pain. He also denied visual loss or diplopia.
Flexible endoscopic evaluation revealed a large pedunculated mass that was inserted into the posterior wall of the right nasal fossa (Figure 1A). A preoperative CT scan was obtained and revealed a 4.5 × 4.4 × 2.5 cm, heterogeneously enhancing mass in the right nasal cavity, apparently attached to the middle meatus, with no bone remodeling (Figure 1B–E).
In July 2018, the patient underwent an endoscopic nasal cavity exploration under general anesthesia (informed consent form was obtained), a large pedunculated mass inserted above the choana was completely removed and submitted for pathologic examination.
Grossly, the tumor was a firm pedunculated mass with a lobular surface and glistening containing a few visible cysts (Figure 1F). The microscopic study revealed multiple lobules covered by ciliated columnar epithelium and contains, in the subepithelial area, multiple cysts covered by cubic epithelium, as well as small ductal structures covered by columnar epithelium in the middle of the fibrous stroma (Figure 2). The ductal epithelial cells were flattened and cuboidal without atypical characteristics. These findings support the diagnosis of seromucinous hamartoma.
Patient was discharged at the same day, and postoperative course was uneventful, with no wound complications, and no recurrence at the 6-month follow-up examination.
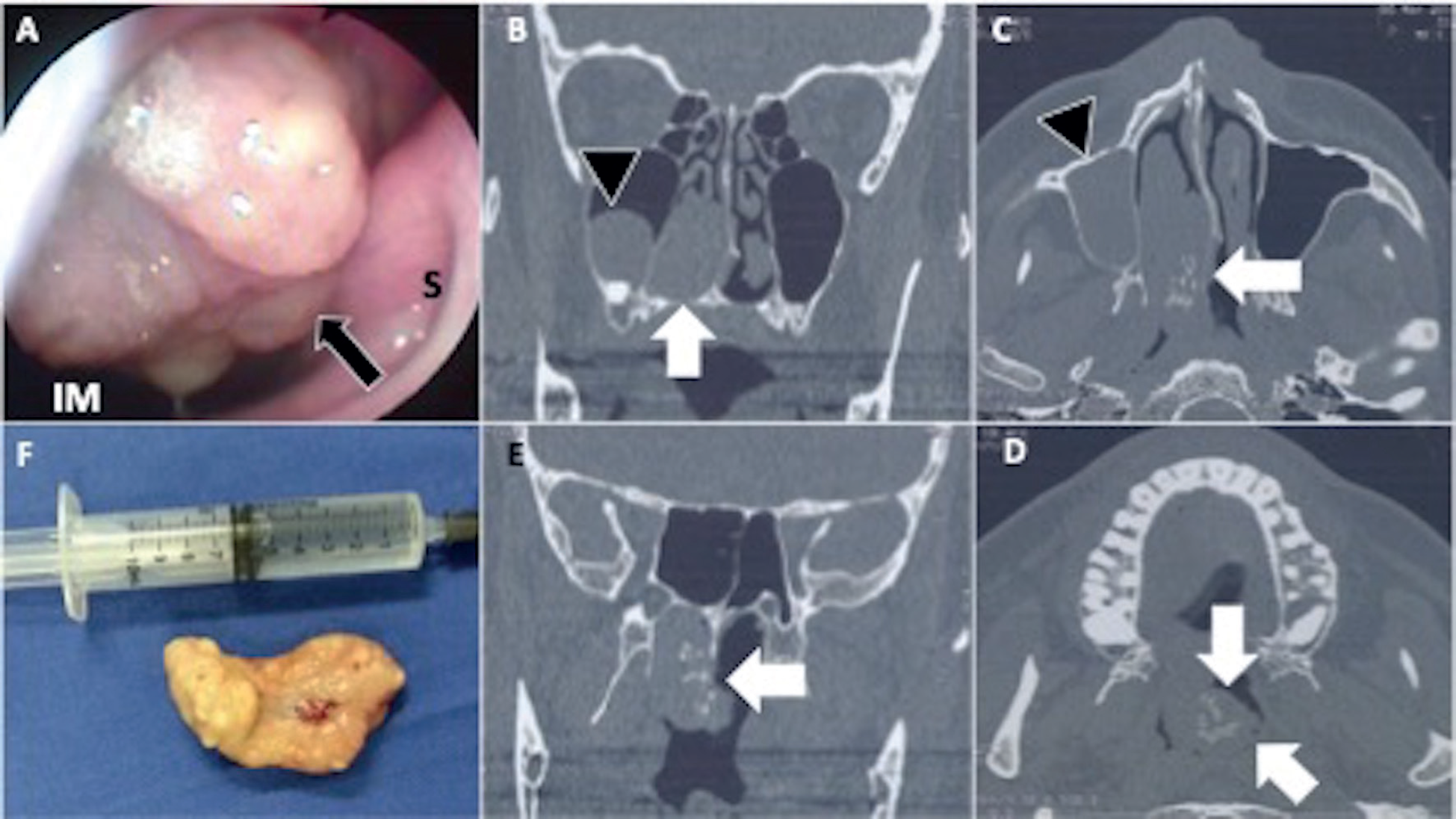
(A) Endoscopic view of a right nasal fossa. Arrow points to the pedunculated lesion with a lobular surface arising from the middle meatus. (B) and (E) CT scan in a coronal view, from anterior (B) to posterior (E). Arrow points a hypodense, well circumscribed lesion attached to the middle meatus, with hyperdense content. Arrowhead points to a round and well-circumscribed lesion inside the maxillary sinus. (C) and (D) CT scan in an axial view. Arrow points to the lesion that reaches the rhinopharynx at the left side. (F) Lesion removed from the right nasal fossa. IM = inferior meatus; S = septum.
Discussion
There are two epithelial entities known as hamartomas, the respiratory adenomatoid hamartoma (REAH) and the seromucinous hamartoma. Since its first description in 1974, there were few case reports, but seromucinous hamartoma has been more studied over the last years because of its relationship to REAH and unique immunoprofile [2]. Foci of identical features to REAH and/or seromucinous hamartoma can be seen in cases of chronic rhinosinusitis and nasal polyposis [1].
To date, about 20 cases of seromucinous hamartoma have been published [1]. They typically arise on the posterior nasal septum, but it also has been described on the lateral wall and in the paranasal sinuses. The age at diagnosis varies between 14 and 85 years (which peaks in the late 6th decade), and the male to female ratio is 3:2 [1,3]. The most common presentation is nasal obstruction and epistaxis, although most patients are asymptomatic [3]. Physical examination reveals a polypoid mass without any local invasion, neither bone destruction nor other aggressive features.
Pathology
Seromucinous hamartoma was initially described as a polypoid mass of respiratory-epithelium-lined tissue with submucosal seromucinous glands in a lobular arrangement and a fibrous background [1-4]. Later reports highlighted additional features, such as invaginated respiratory epithelium-lined gland-like structures in a haphazard arrangement; squamous metaplasia; dense lymphoplasmacytic infiltrate; and dense cytoplasmic eosinophilic granules [1]. The stroma is edematous to fibrotic, with patchy chronic inflammation. No atypia, no mitotic activity, and no epithelial proliferation is seen [4]. Mucinous cells are not a common feature despite the name "seromucinous hamartoma". The nuclei are small and there is no evident mitotic activity or necrosis [4].
Immunohistochemistry demonstrates diffuse positivity for cytokeratins 7 and 19, positivity for S100, and no reactivity of myo-epithelial cells among the seromucinous glands [1–3].
Differential Diagnosis
The main differential diagnosis is the low-grade non-intestinal type adenocarcinoma, and possibly with other low-grade adenocarcinomas [2,4]. Seromucinous hamartoma shows no cytological or architectural features of malignancy (such as glandular fusion and invasion) [2].
Treatment and Prognosis
The treatment for sinonasal seromucinous hamartoma is by endoscopic resection. Recurrence is not frequent and malignant transformation has not been reported, to the best of our knowledge.
Conclusion
Seromucinous hamartoma is a rare form of nasal cavity hamartoma characterized by arborizing, polypoid growth pattern lined by respiratory epithelium. The submucosa has a haphazard proliferation of seromucinous glands without atypia. Although a distinct benign entity, it can be easily confused with inflammatory polyps.


