Background
The classical features of dengue fever are fever, arthralgia, myalgia, leukopenia, and thrombocytopenia [1]. The diagnosis of dengue fever in the endemic area can usually be made with the presentation of classical symptoms and serology testing [2]. One of the laboratory tests to confirm the diagnosis is specific Immunoglobulin M (IgM) serology testing by enzyme-linked immunosorbent assay, which has a sensitivity and specificity of approximately 90% and 98%, respectively, after 5 days of illness [3]. However, the false positive of this serology test remains a challenge in diagnosing dengue fever due to cross-reactivity with other circulating flaviviruses [3,4]. Hence, a clinician should remain vigilant in diagnosing dengue fever even in an endemic area. To the best of our knowledge, we did not identify any reported case of cross-reactivity of dengue IgM serology with a confirmed case of Salmonella typhi infection up to the date that this case report was done. We present a case of typhoid fever with hemophagocytic lymphohistiocytosis mimicking as dengue fever with encephalitis due to the presence of cytopenias and hepatitis, and dengue IgM serology was positive.
Case Presentation
A previously healthy 30-year-old gentleman was initially presented with a fever for the duration of 4 days accompanied by myalgia, arthralgia, nausea, and diarrhea. The physical examination was unremarkable, and his vital signs were stable.
His initial laboratory findings showed bicytopenia with white cell count of 3.2 × 109/l and platelet count of 89 × 109/l. His hemoglobin is normal with 13.7 g/dl and hematocrit of 37.1%. Aspartate aminotransferase and alanine aminotransferase are raised with the value of 216 and 87 μ/l, respectively. Otherwise, his renal profile is normal. Qualitative Rapid Test Kit for both dengue IgM and Immunoglobulin G showed a positive result. However, nonstructural protein 1 antigen test was negative. This prompted the diagnosis of dengue fever as it is endemic in Malaysia. He remained febrile at day 6, and an empirical antibiotic (ceftriaxone 1 g once a day) was started. However, at day 8 of illness, he became delirious.
Computer tomography (CT) of the brain was normal. Cerebrospinal fluid (CSF) analysis was clear, colorless, and acellular and yields no organism. CSF protein was raised with 0.75 g/l and glucose level of 2.5 mmol/l (43% of blood glucose). Herpes simplex virus 1 and 2 dengue polymerase chain reaction (PCR) from CSF was negative as well.
Dengue IgM by enzyme-linked immunosorbent assay method was detected in serum, but dengue PCR was not detected in both the serum and CSF. Other investigations including Surface antigen of the hepatitis B virus, anti-Hepatitis C virus, and anti-human immunodeficiency virus were all nonreactive. Serum ferritin was significantly raised with a level of 45193.47 μg/l. Serum fibrinogen and serum triglyceride were 220 mg/dl and 2.48 mmol/l, respectively. The c-reactive protein was 138.2 mg/l. Peripheral blood film did not show any significant findings.
It is when blood culture yielded S. typhi, the diagnosis was revised to typhoid fever with secondary hemophagocytic lymphohistiocytosis (HLH). Bone marrow aspirate and trephine (BMAT) showed normocellular marrow with evidence of histiocytes and hemophagocytic activity, which confirmed the diagnosis of HLH (Figure 1).
He was treated with intravenous immunoglobulin (IVIG) [0.4 g/kg once a day (OD)] for 3 days, together with a total of 2 weeks of IV ceftriaxone (60–75 mg/ kg OD). He became afebrile the next day, and delirium resolved. After 2 weeks of treatment, all blood parameters were normalized, and eventually, he was discharged well.
Discussions
Dengue fever classically presents with fever, arthralgia, myalgia, leukopenia, and thrombocytopenia [1]. The specific IgM serology testing by enzyme-linked immunosorbent assay for dengue fever has a sensitivity and specificity of approximately 90% and 98%, respectively, after 5 days of illness [3]. The patient had these classical features, and the presence of specific IgM resulted in the diagnosis of the dengue fever earlier. However, the persistent fever and delirium that he suffered later prompted us to investigate further, e.g., dengue encephalitis and secondary HLH.
Although rare, HLH is a potentially fatal complication of dengue fever [5]. The diagnostic criteria based on HLH-2004 trial [6] require the presence of five out of eight criteria: fever (≥38.5°C), splenomegaly, peripheral blood cytopenia (with at least two of the following: hemoglobin <9 g/dl, platelets <100 × 109/l, and absolute neutrophil count <1.0 × 109/l), hypertriglyceridemia (fasting triglycerides >2.99 mmol/l) or/and hypofibrinogenemia (fibrinogen < 150 mg/dl), hemophagocytosis, low or absent NK cell activity, ferritin >500 μg/l, and elevated soluble CD25 2SD above age-adjusted laboratory-specific norms. However, such criteria were designed originally for clinical trials and may be difficult to apply in clinical practice. A proposed modified HLH diagnostic criteria [7] were introduced to aid the diagnosis of HLH, which requires three of four clinical criteria (fever, splenomegaly, cytopenias, and hepatitis) and one of four immune markers (hemophagocytosis, increased ferritin, hypofibrinogenemia, and absent or very decreased NK cell function). The patient met the latter proposed criteria; fever, hepatitis, encephalitis, cytopenias, increased ferritin, and bone marrow showed evidence of HLH activity.
The absence of dengue PCR in both serum and CSF and the presence of S. typhi in blood culture hypothesized that the secondary HLH is due to S. typhi infection.
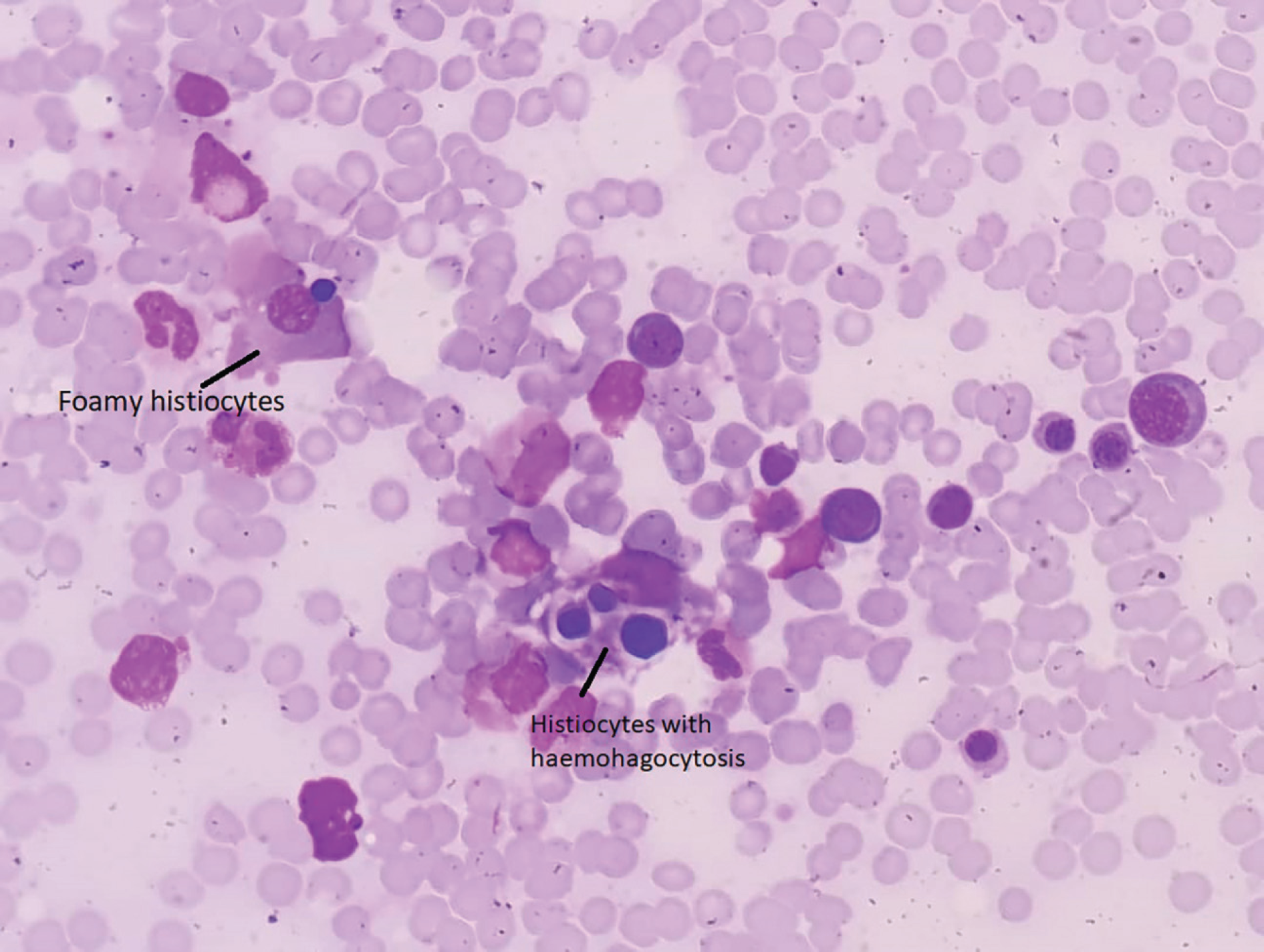
Bone marrow histology of normocellular marrow with evidence of histiocytes and hemophagocytic activity.
Hence, the central nervous system manifestation, cytopenias, and hepatitis for which initially thought to be dengue fever complicated encephalitis were mimicked by a typhoid fever with secondary HLH. However, it is important to know that a negative PCR result does not necessarily exclude the diagnosis of dengue, especially, if the test is performed after the period of viremia [8]. There is a possibility that the patient might have a coinfection with dengue fever as the serology suggested. A positive dengue IgM serology could also represent cross-reactivity or a recent infection [9]. In addition, dengue encephalitis usually occurs during the early phase of infection coinciding with viremic phase [10,11]. Hence, in the absence of direct evidence of dengue virus, encephalitis at the later course of the illness, and isolation of S. typhi from blood culture, the overall presentation leans toward the diagnosis of typhoid fever with HLH.
Several case reports discussed the similar association between S. typhi and HLH, which resolved with antibiotic (with or without intravenous immunoglobulin) [12–14]. Interestingly, these case reports all have negative dengue IgM serology. It is known that dengue IgM serology cross-reacts with other circulating flaviviruses, even leptospirosis and malaria [3]; however, to the best of our knowledge, we did not identify any reported case of cross-reactivity of dengue IgM serology with a confirmed case of S. typhi infection up to the date that this case report was done.
Conclusion
We report a case of typhoid fever with hemophagocytic lymphohistiocytosis mimicking as dengue fever due to cytopenias and hepatitis, and dengue IgM serology was positive. Although rare, a high index of suspicion is required for early diagnosis and treatment. A 2 weeks’ course of ceftriaxone (60–75 mg/kg/day) and IVIG (0.4g/kg OD) for 3 days resulted in complete resolution of his illness.
What is new?
To the best of our knowledge, we did not identify any reported case of cross-reactivity of dengue Immunoglobulin M (IgM) serology with a confirmed case of Salmonella typhi infection up to the date that this case report was done. We present a case of typhoid fever with hemophagocytic lymphohistiocytosis mimicking an IgM serology-positive dengue fever with encephalitis.

