Background
A brain abscess is a rare but serious complication of sinusitis. It mainly involves male teenagers. It is characterized by a heterogeneous clinical picture (fever, headache, pain in the frontal region, neurological symptoms, and ocular symptoms). The pathogenic organism mainly involved belongs to the Streptococcus milleri group (Streptococcus intermedius, Streptococcus constellatus, and Streptococcus anginosus). The diagnosis is clinical with the support of imaging. Treatment can be conservative with antibiotic therapy alone (4-8 weeks), or it can be surgical. Long-term sequelae occur in 40% of cases, and mortality is around 10%. We describe a case of a 16-year-old boy affected by a sinusitis-induced brain abscess.
Case Presentation
A 16-year-old apparently healthy boy came to the emergency room (ER) for the onset of a swelling of the upper right eyelid and photophobia. He reported that, from about 10 days, he had an evening-onset fever, mucous-purulent rhinorrhea, nasal obstruction, and frontal headache. On physical examination, he was found to be in generally good condition with tenderness on palpation of the right frontal and supraorbital region. Endoscopic examination of the right nasal cavity showed a purulent discharge.
Laboratory data showed neutrophilic leukocytosis and a moderate increase in C-reactive protein (CRP) (19.6 mg/ dl). He was discharged from ER with the diagnosis of a right frontal sinus disease and a prescription for a 10-day antimicrobial therapy with amoxicillin (50 mg/kg/day).
A period of clinical well-being followed with only occasional headache; after 2 months, the boy returned to the ER for a new appearance of swelling in the upper right eyelid accompanied by rhinitis, fever, headache, sleep disturbances, and several episodes of vomiting. Physical examination revealed painless unilateral proptosis in the absence of cutaneous hyperemia, conjunctivitis, and diplopia, and the pupils were bilaterally isochoric, isocyclic, and reactive to light, painful palpitation of maxillary sinuses bilaterally. Neurological observations were normal. Examination of the ocular fundus of both eyes revealed bilateral papilledema. A computed tomography (CT) scan of the brain and orbit found a 5-cm right orbitofrontal and frontal expansive lesion surrounded by vasogenic edema, an extra axial homolateral orbitofrontal collection, a subfalcine herniation, a 7-mm midline shift, and a phlogistic inflammatory tissue in orbital roof and paranasal sinus (Figure 1a).
Laboratory data showed neutrophilic leukocytosis and a slight increase in CRP (3 mg/dl), and procalcitonin was negative. Fiberoptic examination of the nasal cavity and nasopharynx showed a purulent discharge from the right ostiomeatal complex.
We started a wide-spectrum antimicrobial therapy (ceftriaxone 2 g/day) and osmotherapy (mannitol 18% [0.8 g/ kg/day]) and glucocorticoids (dexamethasone [0.3 mg/kg/ day]) to reduce vasogenic brain.
After 24 hours from hospitalization, a magnetic resonance imaging (MRI) with gadolinium enhancement was performed. Frontal lesion had a characteristic enhancement pattern of a brain abscess, and the images confirmed CT results (Figure 1b).
A conservative approach with broad-spectrum antibiotics (ceftriaxone 2 g/day, amphotericin B
3 mg/kg/day, and rifampicin 10 mg/kg/day) was suggested by neurosurgery department that would have performed surgery if there had been no response to antibiotic therapy.
After 4 days of conservative therapy and due to the clinical deterioration of the patient, another MRI was performed. The images showed an increase in the brain abscess and the subfalcine herniation size.
A combined neurosurgery and otolaryngology procedure had to be performed. Neurosurgery performed a craniotomy and drained a large amount of purulent fluid. The day after surgery, a CT was performed. It showed a slight decrease in the midline shift from left to right and an initial re-expansion of the frontal horn of the right lateral ventricle.
After surgical procedure, empiric antibiotic therapy has been continued with ceftriaxone, rifampicin, amphotericin B, and vancomycin.
Streptococcus intermedius has been isolated from wound and wound drainage cultures. Blood culture was negative. As a result of the antibiogram, the antimicrobial therapy with ceftriaxone and rifampicin was continued.
The boy has been discharged from hospital after 14 days of intravenous antibiotic therapy.
At home, he had to continue an oral antimicrobial therapy with amoxicillin/clavulanic acid and rifampicin.
He was hospitalized after 1 week again suffering from photophobia, daily frontal headaches, and proptosis on the right side. Laboratory data were normal. Examination of the ocular fundus of both eyes revealed bilateral papilledema and peripapillary hemorrhages. An MRI showed a vasogenic brain edema around the right frontal lesion of the abscess, a midline shift of 14 mm, and compressed frontal horns of lateral ventricles (Figure 1c). The intravenous antimicrobial (ceftriaxone [4 g/day] and rifampicin [10 mg/kg/day]) and anti edema therapy was administered (dexamethasone and furosemide).
The MRI performed on days 7, 15, and 30 (Figure 2a, b, c) from hospital admission showed a progressive decrease of the residual abscess, of the edema and an initial midline recovery.
The boy was discharged after 30 days of intravenous antimicrobial therapy and dexamethasone.
At home, he had to continue an oral antimicrobial therapy with rifampicin for 3 weeks and steroids in decreasing doses.
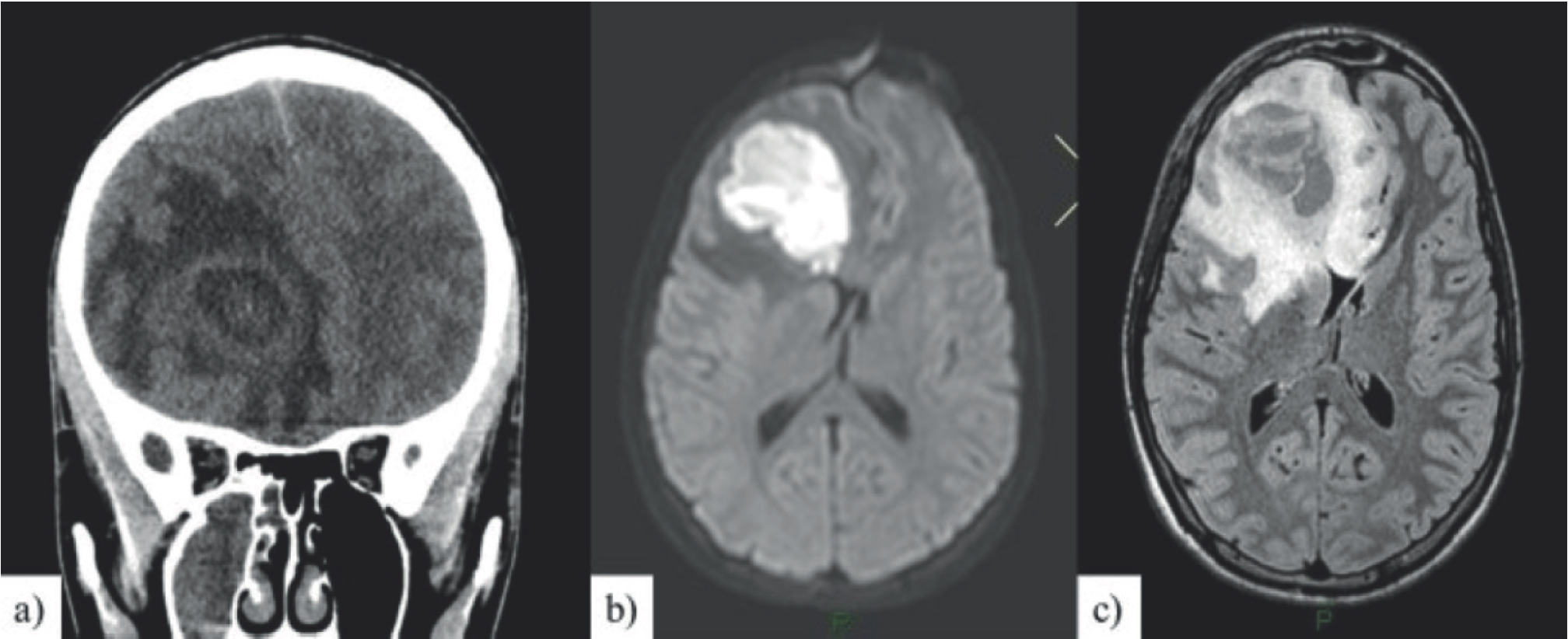
a) Coronal section CT: non-homogeneous expansive formation in the orbito-frontal and anterior frontal right region, delimited by edema with shift of the median structures; b) axial DWI MRI: restriction of lesional diffusion with abscess appearance; c) MRI FLAIR 3D axial MPR: greater extension of the edema adjacent to the known right frontal abscess lesion, with compression on the anterior areas of the lateral ventricles and shift towards the left of the midline structures.
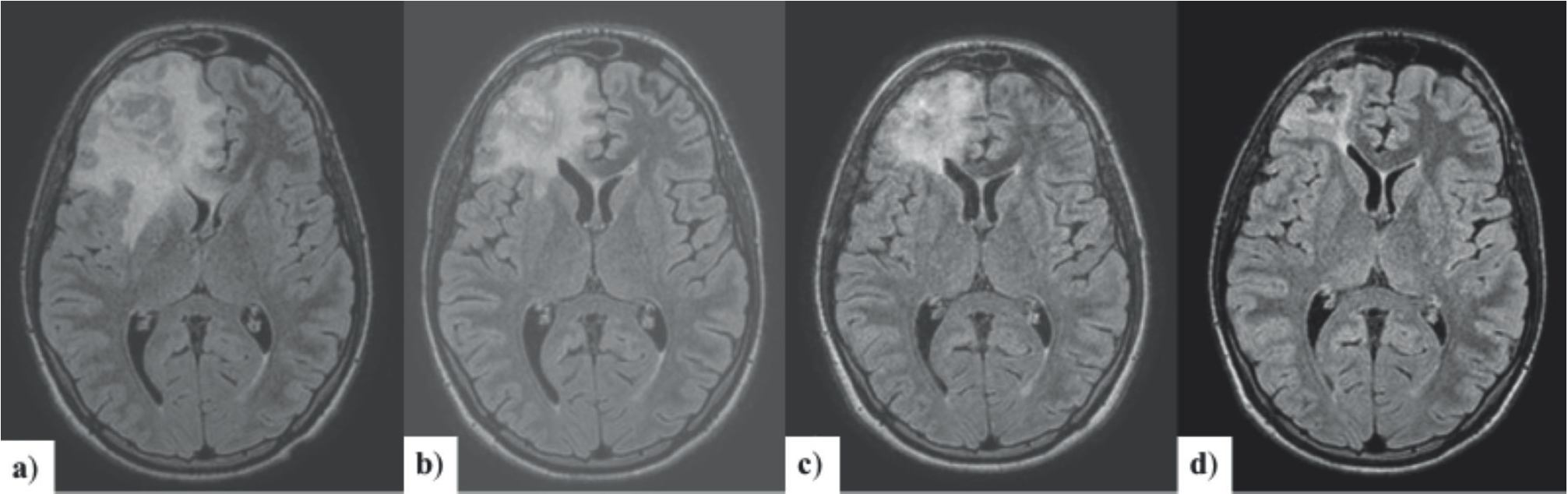
MRI FLAIR 3D axial MPR : a) RMN performed 7 days later, b) 15 days, c) 30 days, and d) 5 months after entering the ward; progressive reduction of the abscess residue, edema, and hypoexpansion of the frontal horn of the ipsilateral ventricle and convolutions.
MRI follow-up after 5 months (Figure 2d) revealed that everything was almost within the normal standard. The boy is in good health and has no sequelae.
Discussion
A brain abscess is a rare but severe infection of the brain parenchyma. The mortality decreased from 30% to 60% in the 1970s to less than 10% in the past few years through imaging techniques and the use of antibiotic therapy [1]. Common predisposing factors include hematogenous dissemination, contiguous infection (sinusitis, otitis, mastoiditis, and meningitis), and penetrating head injuries; in 15%-30% of the cases, the cause is unknown [2]. In about 6%-8% of the cases, sinusitis complications can occur. The patient will then develop a brain abscess. The frontal lobe is more affected because of its rich network of diploic veins and the frequency of frontal and anterior ethmoid sinusitis. The abscesses secondary to sinusitis affect not only the temporal but also the frontal lobe. Adolescents are particularly affected by the rapid growth of the frontal sinuses and their blood supply; moreover, the male sex is mostly affected by this.
The clinical presentation may be deceptive and/or heterogeneous with fever, headache, pain in the frontal region, neurological symptoms, and ocular symptoms. Large abscesses cause a mass effect by compression of the surrounding tissues, causing an increase in intracranial pressure, herniation, and neurological deficits depending on the area involved.
Brain abscess patients typically have symptoms that last for about 10 days [3]; in this case, the symptomatology persisted for 2 months even if attenuated. Probably, the first antibiotic therapy with amoxicillin for sinusitis had only been partially effective so that, after a while, the infection was spreading again allowing the abscess to grow further causing intracranial hypertension and cerebral herniation due to mass effect.
Blood tests generally show a neutrophilic leukocytosis with increased CRP; the blood culture is positive only in a small percentage of patients, and the isolated germ is the same as the purulent material present in the abscess [4], and the species of Streptococcus (53%) predominate of which the S. milleri group (S. intermedius, S. constellatus, and S. anginosus) is the most common [3,5], followed by Staphylococci. In immunocompromised patients, the fungi dominate. Sterile pus cultures are found in 30% of the cases.
Neuroimaging techniques, such as CT or MRI, will determine the diagnosis, but, in urgent cases, the examination that is preferable is the CT due to the rapid execution times. MRI is useful in the follow-up due to the absence of ionizing radiation and greater specificity.
Treatment may be conservative with only antibiotic therapy or may be surgical. The therapeutic choice depends on the immunological and neurological status of the patient, the position of the abscess, and the number and size of the abscesses. The conservative approach is reserved for cases of small abscesses that do not cause neurological deficits or in the case of multiple abscesses. Surgery is used in case of resistance to an antibiotic therapy. Intravenous empirical antibiotic therapy is combined with vancomycin, a third-generation cephalosporin, rifampicin, and metronidazole. The duration of the treatment is not standardized, but, from the data in the literature, it is considered useful to keep it intravenous until the completion of 4-8 weeks [4,5].
Long-term sequelae occur in approximately 40% of cases (epilepsy, focal motor deficits, visual or hearing impairment, hydrocephalus, speech problems, learning, or behavioral disorders), and this depends on the presence of neurological deficits at the onset and the duration of the antibiotic therapy [3,4].
In this case, after finishing the antibiotic and antiedema therapy, a medical examination revealed that the boy was in good condition without sequelae.
Conclusion
The clinical case of the patient is interesting because, in the literature, there are few described cases of brain abscess secondary to sinusitis. A simple airway infection, such as sinusitis, in the 6%-8% of cases can cause this serious complication with high morbidity and mortality. An immediate antibiotic therapy and/or surgical intervention are necessary to guarantee a more rapid healing of the patient.
A multidisciplinary approach of neuroradiology, neurosurgery, pediatricians, and otorhinolaryngologist is necessary for an adequate treatment of the patient.
What is new?
We describe the case of a brain abscess caused by Streptococcus intermedius secondary to sinusitis in 16-year-old adolescents. The case is very interesting because, in developed countries, brain abscesses are relatively low in children, but the morbidity and the mortality rates are high. The images could help pediatricians to early recognize this infection and start the antibiotic therapy and/or surgery as soon as possible. Searching the literature, the cases described are not many.

