Background
Amoebiasis is endemic in developing countries, where poor hygiene, overcrowding, and low sanitary standards result in the increased prevalence of the disease [4]. Intestinal manifestations include colitis, whereas liver abscess is the most common extraintestinal manifestation [5]. It is common in adults but rare in children, and only few cases of amoebic liver abscess are reported in the literature [6].
Case Presentation
A 45-days-old male baby presented to the gastroenterology department with an 8-days history of fever and vomiting off and on. His feed intake was less than usual. There were no other systemic symptoms. There was no history of hospital admission, sepsis, or umbilical catheterization. On admission, the temperature was 38°C, he was pink in air, not jaundiced, conscious, and slightly irritable. On abdominal examination, it was soft, non-tender, and not distended. Liver was 3 cm below the costal margin, soft in consistency, and slightly tender. No other viscera were palpable and bowel sounds were normal. Rest of the systemic examination was unremarkable.
Routine labs were conducted along with liver ultrasound and Computed tomography of the abdomen. Complete blood count showed raised white blood cells with predominant neutrophils, Hemoglobin (Hb) was low, and C-reactive protein was raised. Blood culture was negative and enzyme-linked immunosorbent assay (ELISA) test was positive for amoebiasis. (Table 1)
Ultrasound of the abdomen, carried out on the day of admission, showed heterogeneous ill-defined areas in the right lobe of the liver, suggestive of multiple liver abscesses. The largest one measuring 33.6 × 13.2 × 26 mm, with a volume of 6.1 ml, and the other one measuring 20.9 × 14.7 × 17.5 mm, with a volume of 2.8 ml. The smallest one measured was 15.2 × 9.4 × 11.2 mm, with a volume of 0.8 ml (Figures 1 and 2). CT of the abdomen showed multiple heterogeneous density areas with internal cystic spaces in the right lobe of the liver (Figures 3 and 4).
On admission, the child was given triple antibiotic cover with IV fluids and symptomatic treatment. After the blood culture report, the antibiotics were stopped. After the ELISA report, he was started on IV metroni-dazole. The child’s fever settled on the third day, with improvement in the WBC count to normal on the seventh day. The C reactive protein became normal on the tenth day. Follow-up ultrasound was carried out with marked improvement showing the largest lesion of about 2.7 × 4 mm only, while the smallest one was about 2.1 × 1.2 mm. The child was discharged with an oral metronidazole course for 4 weeks and follow-up was given in the clinic. On follow-up, the child was symptom-free, playful, and healthy, having a normal ultrasound.
| TESTS | PATIENTS VALUES | NORMAL VALUES |
|---|---|---|
| Hb | 7.6 g/dl | 9 g/dl |
| WBC | 27,600 × 109/l | 3.5–10.0 × 109/l |
| Neutrophils | 74% | 52% |
| Lymphocytes | 23% | 42% |
| Monocytes | 02% | 04% |
| Eosinophils | 01% | 02% |
| Prothrombin time | 12 seconds | 13 seconds |
| Activated partial thromboplastin time | 30 seconds | 33 seconds |
| Alanine aminotransferase | 46 IU/l | 7–56 IU/l |
| Aspartate aminotransferase | 48 IU/l | 10–40 IU/l |
| Serum albumin | 3 g/dl | 3.5–4.5 g/dl |
| Urea | 25 | 10–25 mg/dl |
| Creatinine | 0.4 | 0.7–1–4 mg/dl |
| Serum IgA | 0.58 g/l | 0.08–0.91 g/l |
| Serum IgG | 8.8 g/l | 2.05–9.48 g/l |
| Serum IgM | 0.91 g/l | 0.17–1.43 g/l |
| ELISA for amoebiasis | positive | |
| Echinococcus antibodies | negative | |
| Blood culture | negative |
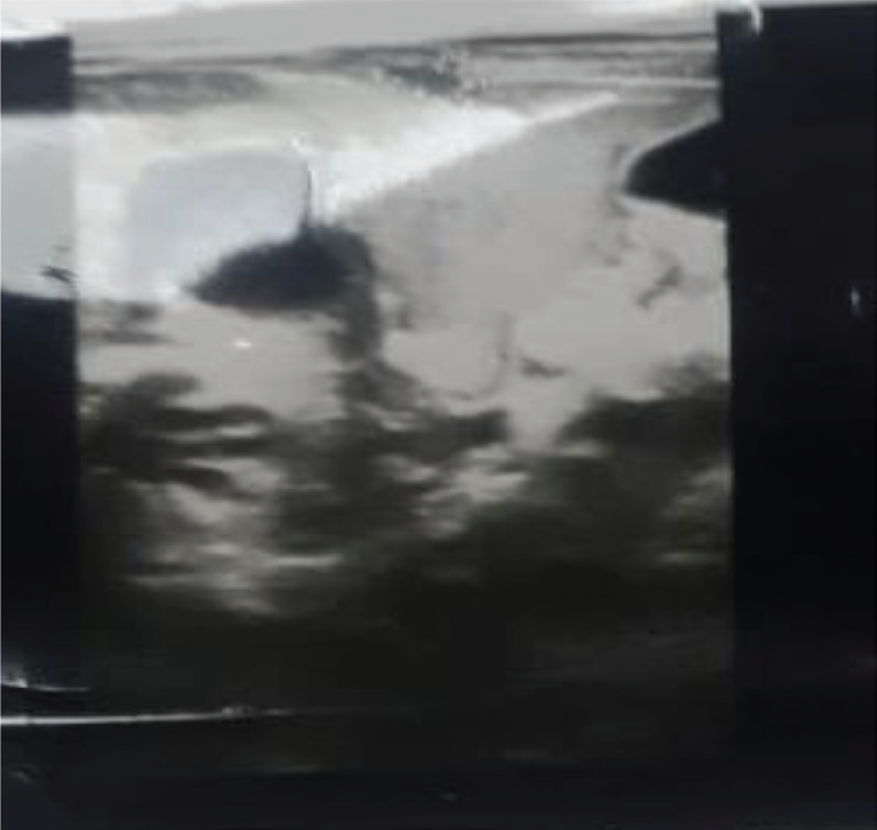
Ultrasound of the abdomen showing heterogeneous ill-defined areas in the right lobe of the liver, suggesting multiple liver abscesses, with the largest one measuring 33.6 × 13.2 × 26 mm, with a volume of 6.1 ml, and the other one measuring 20.9 × 14.7 × 17.5 mm, with a volume of 2.8 ml. The smallest one measured 15.2 × 9.4 × 11.2 mm, with a volume of 0.8 ml.
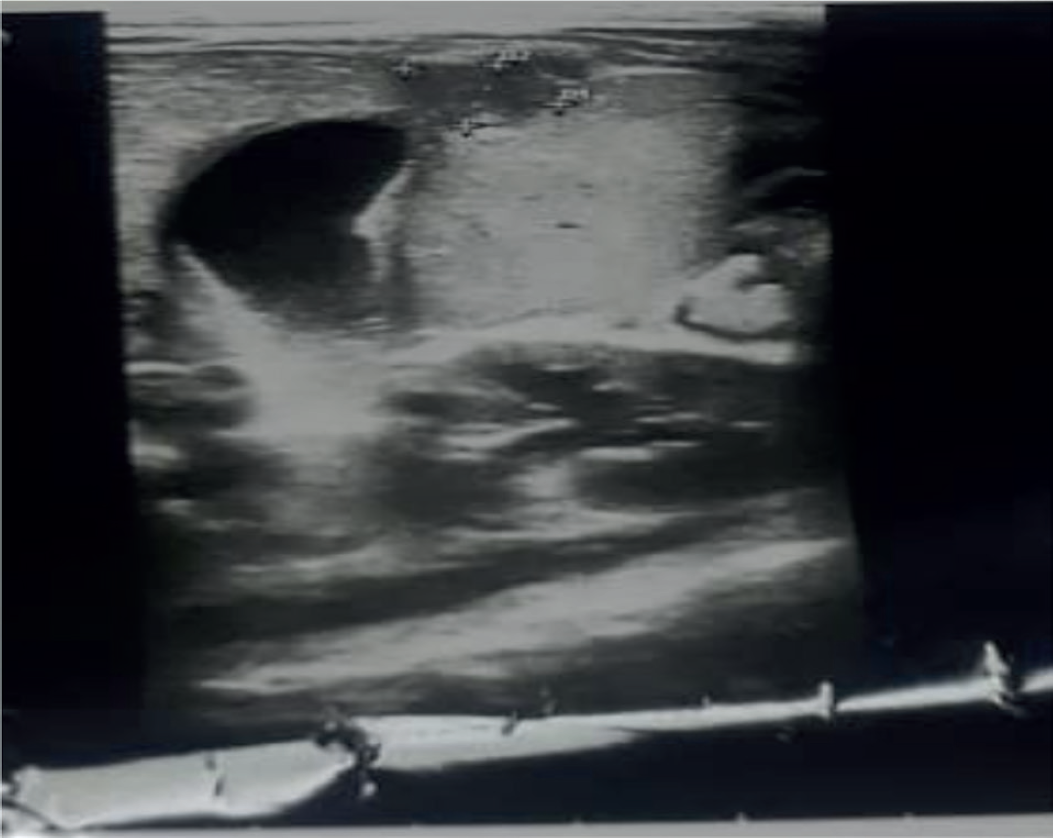
Ultrasound of the abdomen showing heterogeneous ill-defined areas in the right lobe of the liver, suggesting multiple liver abscesses, with the largest one measuring 33.6 × 13.2 × 26 mm, with a volume of 6.1 ml, and the other one measuring 20.9 × 14.7 × 17.5 mm, with a volume of 2.8 ml. The smallest one measured 15.2 × 9.4 × 11.2 mm, with a volume of 0.8 ml.
Discussion
Amoebiasis is caused by Entamoeba histolytica, which is endemic in developing countries [1]. The most common intestinal manifestation is colitis, whereas the most common extraintestinal illness is amoebic liver abscess. Liver abscess is prevalent in areas with overcrowding, poor hygiene, and low standards of sanitation. The spread is through the orofecal route. It is further influenced by the nutritional status of the population, making undernourished people more vulnerable to the disease [7]. In developed countries, it is more common among travelers and immigrants from endemic areas [8].
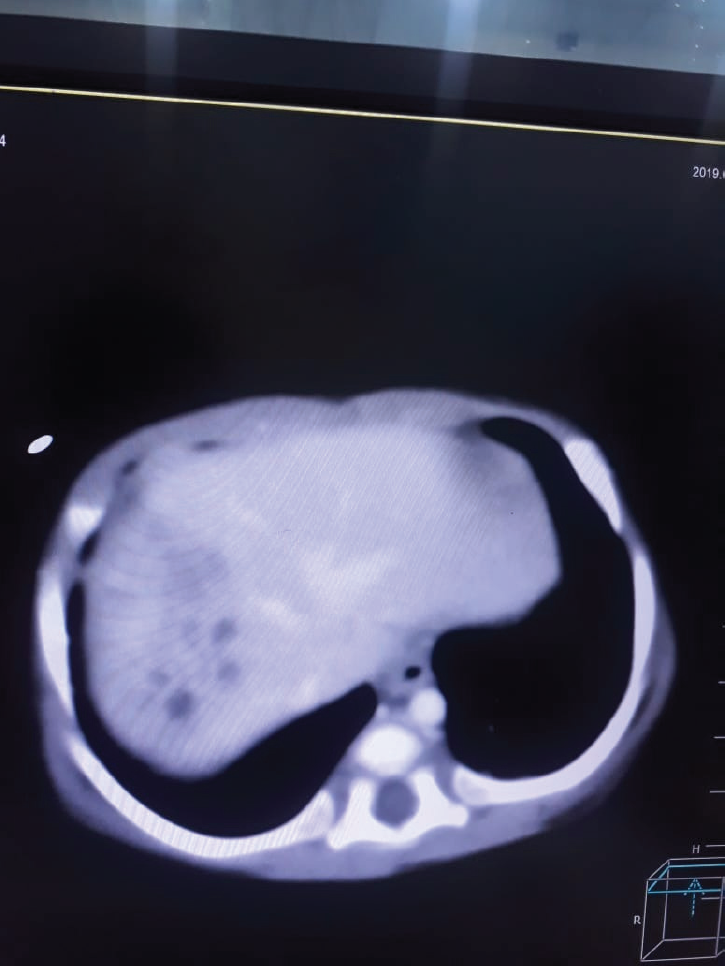
CT of the abdomen showing multiple heterogeneous density areas with internal cystic spaces in the right lobe of the liver.

CT of the abdomen showing multiple heterogeneous density areas with internal cystic spaces in the right lobe of the liver.
Amoebic liver abscess presents with fever, abdominal pain, and occasional gastrointestinal symptoms, like diarrhea .There is hepatic tenderness and its presentation is mostly acute [9]. It is diagnosed by identification of cystic lesions in the liver and positive serological tests for amoebiasis [10]. The most common differential is echinococcus cysts and malignant disease of the liver. The standard treatment in uncomplicated amoebic liver abscess is metronidazole along with intraluminal amoebicide, like paromomycin. Drainage is usually not required in the right lobe abscess, unless it is bigger than 6 cm or in the left lobe of the liver [11].
Amoebic liver abscess is a rare condition and very few cases have been reported in neonates and infants. One case study reported on a 19-day-old baby who was orally given sugar solution and was treated successfully with metronidazole [12]. Another case report showed that a 20-day-old newborn was diagnosed with amoebic liver abscess who presented with a cystic lesion in the right lobe of the liver. The liver abscess was drained, which confirmed the amoebic pathology; however, the baby died due to necrotizing enterocolitis [13]. Another case study showed three neonates with amoebic liver abscess, whose presentation was similar to our case and were diagnosed on serology and microscopic examination of the abscess content. These cases had a history of umbilical catheter infection, prematurity, and necrotizing enterocolitis [14].
In our case, the baby had no history of umbilical catheterization or any other predisposing factors leading to the hematogenous spread of infection. The mother had no antenatal history of any illnesses and there was no maternal and baby contact with a tuberculosis patient. The stool test was negative. There was no evidence of immune deficiency and the child recovered fully after the treatment. The cause of liver abscess seemed to be the contaminated water source. The baby was taking formula feed and normal tap water was being used for preparing the milk without boiling it. The family was living in an overcrowded locality with low standards of personal hygiene and sanitation. At the time of discharge, she was referred to the health educator for proper counseling and advice on hygiene and feeding practices.
Conclusion
Amoebic liver abscess is rare and can have serious consequences in infants. This highlights the fact that we need a high degree of suspicion to diagnose such an illness in infants. It is important to create awareness among people about hygiene and sanitation. Water should be used after boiling or disinfecting.

