Background
Ectopic breast cancer is defined as breast cancer that occurs in ectopic sites of breast tissue. It is a rare occurrence, accounting for 0.3%–0.6% of all breast cancer, and represents important challenges, both in diagnosis and clinical management. These difficulties may lead to a delay in diagnosis, which can have an impact in clinical outcome. Here, we report a case of ectopic breast cancer in a female patient who was referenced to our Institution.
Case Presentation
We report the case of a 46-year-old female patient, a factory worker who lives in a metropolitan area in the north of Portugal. She was referred to our Institution in May 2018 with the diagnosis of ectopic breast invasive carcinoma on the left axilla.
The patient had previously undergone a bilateral resection of ectopic axillary breast tissue for cosmesis in a private practice in 2012 and presented with no other personal relevant history. She was premenopausal, and her gynecological history included one healthy pregnancy 26 years prior. She mentioned swelling of the left axilla while breastfeeding her daughter, that subsided after applying pressure and massaging the axilla, which stimulated lactation through the nipple. She took oral birth control for 27 years. The patient had a sister who was diagnosed with invasive breast cancer 6 years prior, at the age of 50, and was alive and without recurrence.
After noticing an increase in volume in the previously excised left axillary tissue in April 2017, the patient underwent an ultrasound, and was again submitted to surgery outside our Institution, in which a skin patch with an 8 mm adjacent nodular lesion were removed.
Pathology reported a grade 2 invasive carcinoma of no special type [ductal no special type (NST)] in ectopic breast tissue, with accompanying ductal carcinoma in situ of intermediate nuclear grade. The neoplasia measured 0.9 cm and infiltrated the deep dermis and subcutaneous tissue, without lymphovascular permeation, with positive margins. The tumor cells were strongly immunoreactive for estrogen and progesterone receptors and inconclusive for Human Epidermal growth factor Receptor-type 2 (HER-2) [classified as negative after Fluorescence in situ hybridization (FISH)] (Figure 2). She was then referenced to our Hospital.
A bilateral breast MRI identified a heterogeneous 2.3 cm area on the upper inner quadrant of the right breast, also apparent in ultrasound, which was biopsied and was compatible with a radial scar.
After discussion in a dedicated group meeting, it was decided to perform a surgical margin re-excision and sentinel node biopsy, and an excisional wire-guided biopsy of the right heterogeneous lesion, which took place in 24/08/2018, with no intra or post-operative complications. On the left side, histology showed no residual tumor and two non-involved sentinel lymph nodes. The lesion that was removed from the right breast was confirmed to be a radial scar.
The patient was staged as pT1bN0snM0 and, after discussion in a multidisciplinary meeting, was offered adju-vant radio and hormone therapy. Therefore, she initiated tamoxifen (200 mg/day) and goserelin in 26/09/2018. An adjuvant radiotherapy treatment was planned, to deliver 50 Gy in 25 fractions to the left breast and axilla, with 6 and 10 MV photons, employing a 3D conformal radiation therapy (3DCRT) technique, followed by a 10 Gy boost with bolus to the axilla (due to dermis invasion), with the same fractionation, energy, and technique (Figure 1, 3 and 4). The patient completed treatment in 30/11/2018, in 38 days, without interruptions, with grade 3 radiodermitis on the axilla. She remains in follow-up in our Institution, with no significant side effects or signs of recurrence (clinical or imagiologic) 1 year after adjuvant radiotherapy.
Discussion
Ectopic breast tissue (EBT) is rare (0.2%–6% of the population) [1] and develops as a consequence of the embryologic involution of the mammary ridge that forms across the milk line during the 4th week of gestation. This ectodermal structure slowly disappears during the 5th week, leaving behind the mammary sketch in the 4th intercostal space, a structure that will originate the adult mammary gland. Therefore, when present, ectopic breast tissue is located across the line that extends from the axilla (most frequently, in 58%–70% cases) to the inguinal region [2,3].
EBT is more common in Asian populations and appears to be associated with urological malformations [1]. In Europe, it can be found in 0.22% of the population [4]. The male-to-female ratio of the incidence of breast cancer in EBT seems to be higher than in orthotopic tissue (0.035 in the first and 0.01 in the latter). It seems to affect younger individuals than breast cancer in eutopic tissue but appears mainly in individuals older than 40 years [1]. Although most cases are sporadic, an autosomal dominant inheritance pattern with incomplete penetrance has been described in around 10% cases [4,5]. Around 200 ectopic breast carcinoma cases have been reported in the literature to date, most commonly in the axilla (also the most common location for EBT) [1,2].
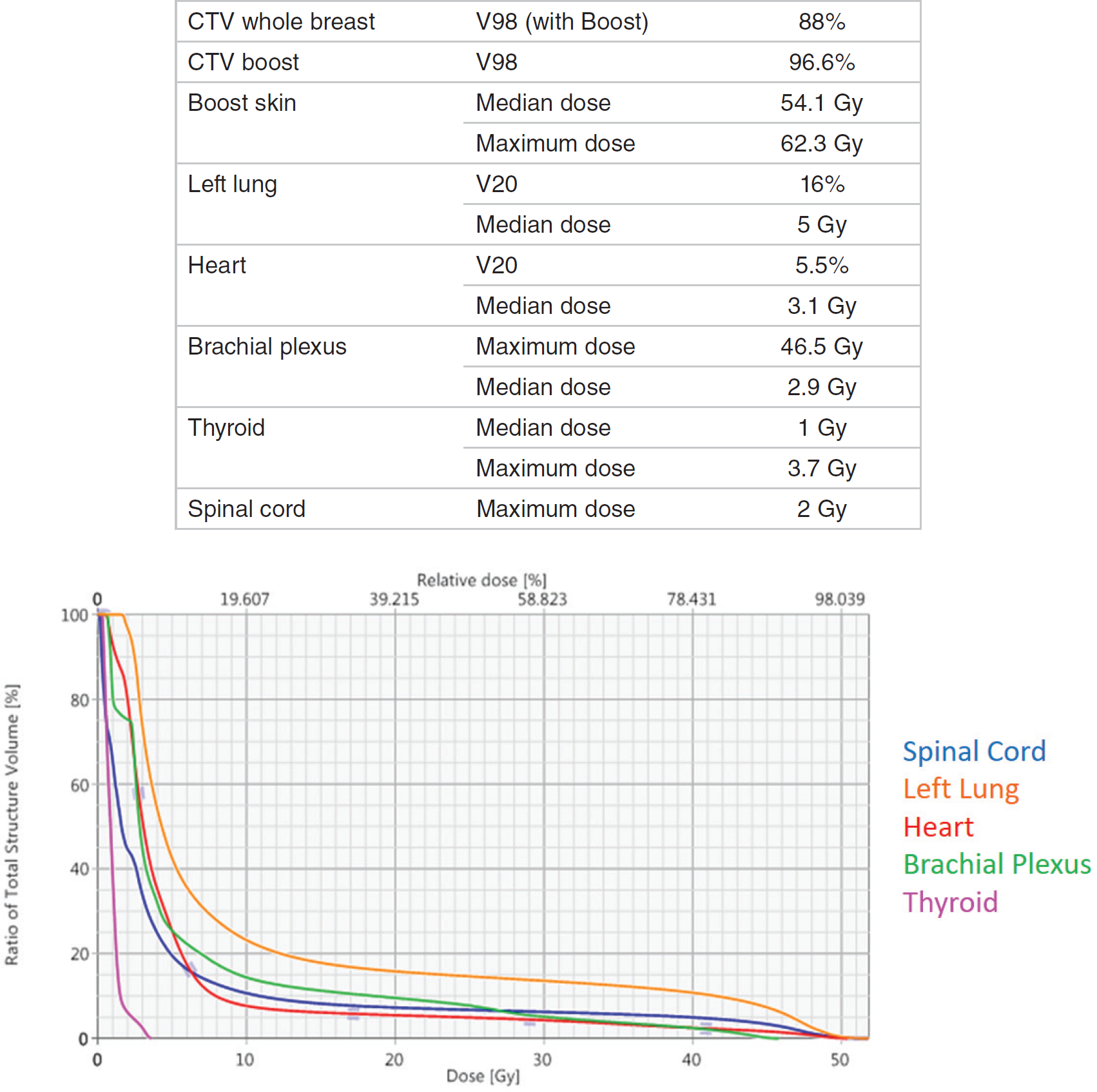
Radiotherapy treatment plan characteristics (dose coverage and dose to the organs at risk) and dose-volume histogram.
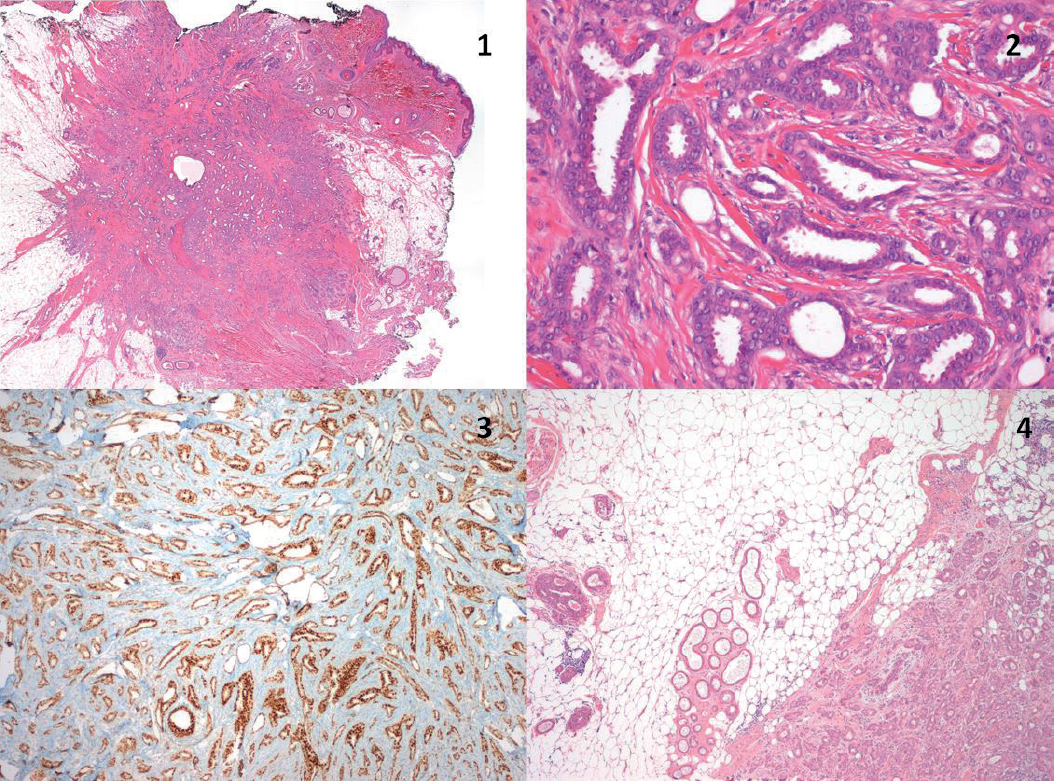
Histology—Institutional review of the specimen removed in 2017. 1—Neoplasia is centered on the subcutaneous tissue with infiltrative boundaries, involving the deep dermis. The surgical margin was positive (in black). (HE, 20×); 2—The tumor exhibits a predominantly glandular pattern, with cells with vesiculated nuclei, accentuated pleomorphism and low mitotic activity (invasive ductal NST carcinoma, grade 2). (HE, 200×); 3—The hormonal estrogen and progesterone receptors were imunorre-active in 90%–100% cells. (ER and PR, 40×); 4—The neoplasia appears in a background of normal breast tissue and adnexal glands of the axilla (HE, 40×).
Several systems for classification were postulated. The most used was published by Kajava [6] and divides EBT in eight categories, according to the supernumerary structures (Table 1). Copeland and Geschickter [7] proposed a different system, in which EBT was more simply classified as supernumerary breast (glandular tissue with an associated nipple or areola) or aberrant breast (glandular tissue without nipple or areola).
Most commonly, EBT becomes evident under hormonal stimulation, such as puberty or lactation, and can present with symptoms, such as tenderness, swelling, discomfort limiting arm movement, or secretion [1,3]. When in the axilla, the most relevant differential diagnosis is benign or malignant (primary or secondary) lymphadenopathy, sebaceous cyst, lipoma, lymphadenitis, and hidradenitis suppurativa [3,8].
There are no specific imagiologic features [2]. Fine needle aspiration, along with imagiology and clinical features, can be helpful in suggesting the presence of an ectopic breast carcinoma. However, in a retrospective study by Nihon-Yanagi et al. [2], an excisional biopsy or surgery specimen were needed to obtain a definitive diagnosis in most cases. Carcinoma in ectopic breast tissue must be differentiated from an axillary lymph node metastasis and eccrine carcinomas. The presence of adjacent normal breast ducts or lobules, the absence of lymph node tissue and the association with carcinoma in situ supports the diagnosis [3,9].
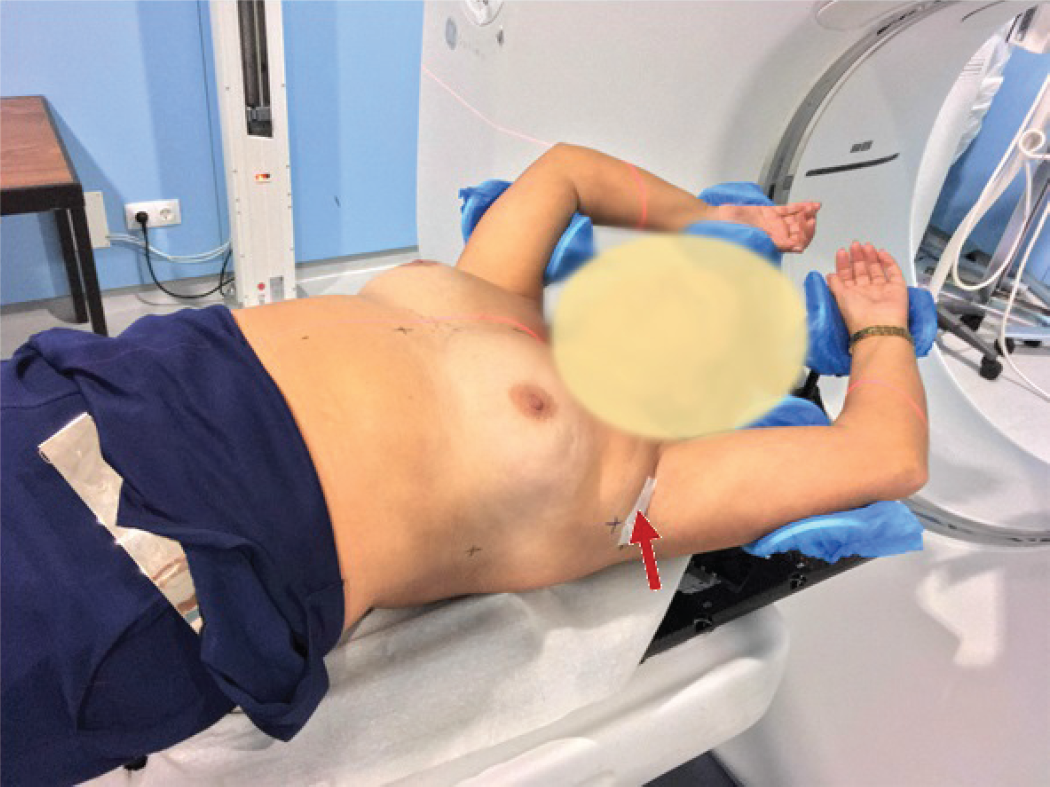
Positioning for external beam radiation therapy, with a radiopaque marker signaling the surgical scar (red arrow).
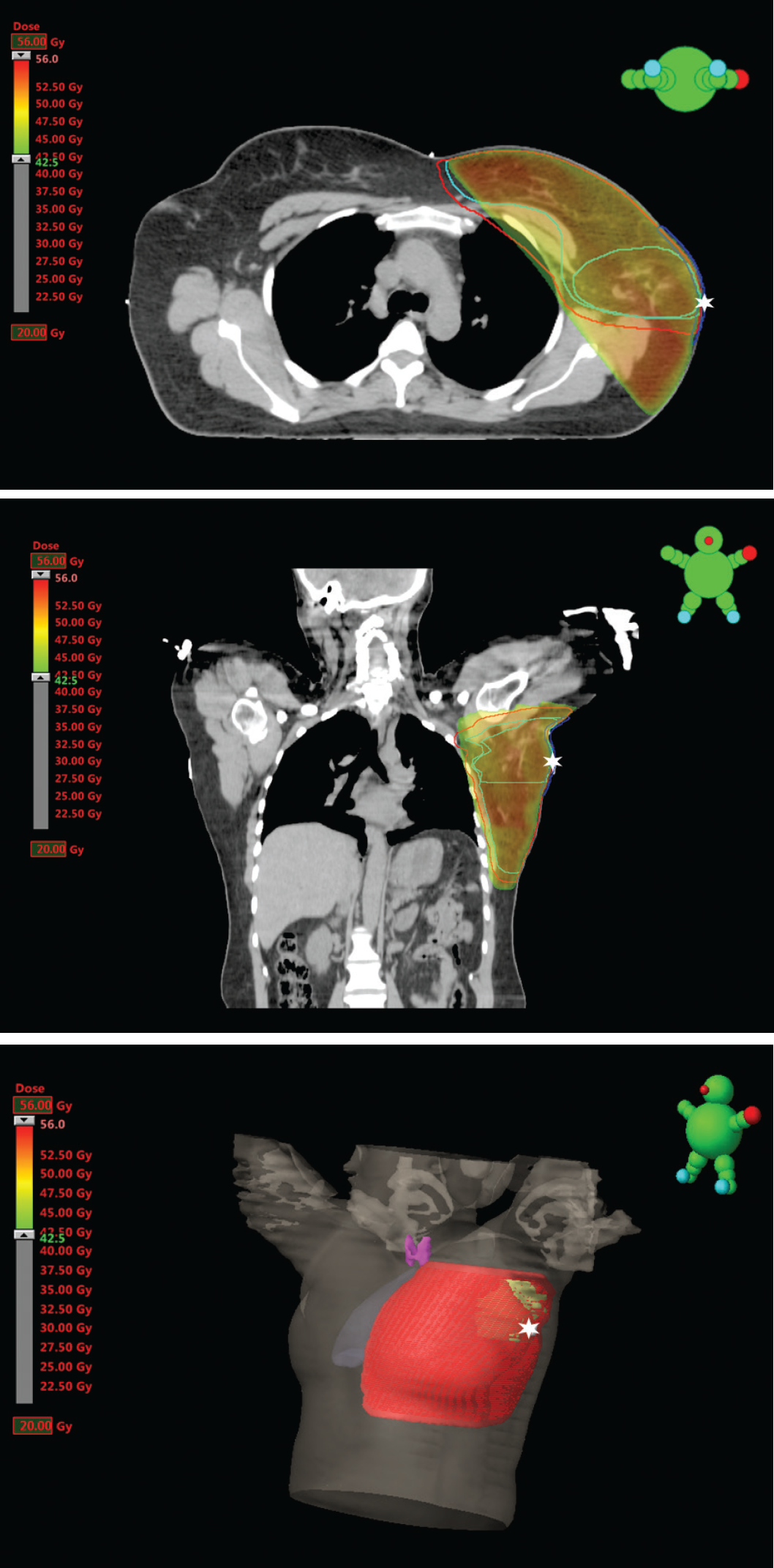
Adjuvant radiation therapy plan (Red—PTV; Light Blue—CTV whole breast and CTV boost; Dark Blue—Boost skin; White Star—radiopaque marker over surgical scar).
| I | Complete supernumerary breast (polymastia—nipple, areola and glandular tissue) |
| II | Supernumerary nipple and glandular tissue (no areola) |
| III | Supernumerary areola and glandular tissue (no nipple) |
| IV | Glandular tissue only |
| V | Supernumerary areola and nipple (pseudomamma—no glandular tissue, fat only) |
| VI | Supernumerary nipple only (polythelia) |
| VII | Supernumerary areola only (polythelia areolaris) |
| VIII | Patch of hair only (polythelia pilosa) |
Histologically, most are ductal carcinomas (72%– 79%), followed by lobular and medullary carcinomas (12%), and mucinous carcinomas (7.8%) in retrospective series by Marshall [10], Visconti [1], and Nihon-Yanagi [2]. In the latter, medullary, mucinous and apocrine carcinomas were more common in EBT than in orthotopic tissue [2]. Other histological types are reported to be rare [5].
Since there are no specific guidelines for the treatment of EBT carcinomas, they are usually treated in the same way as orthotopic breast tumors [5]. Local excision and axillary dissection is the procedure of choice for axillary EBT malignant lesions, since studies have shown that there is no evidence of ipsilateral breast involvement in radical mastectomy and autopsy specimens, even in patients with distant metastasis. Therefore, mastectomy does not seem to be necessary [2,11] and a multimodal approach is employed, with surgery, radiation, and systemic treatment on indication (chemo or hormonal therapy). Postoperative irradiation of the tumor site and regional lymph nodes is indicated [4]. In this case, we included the whole breast in the radiotherapy volume due to the history of lactation in the axillary tissue that drained through the nipple, probably indicating that the lymph drainage also followed the usual path, accompanying the ducts.
Given the rarity of EBT carcinoma, prognosis is difficult to establish. However, due to the frequent delay in diagnosis and clinical management of these cases, it seems to be worse than that of orthotopic breast carcinomas [5,10].
In our case, histology of the surgical specimen established diagnosis, which allowed for a timely re-intervention and subsequent adjuvant treatments. This was eased by the patient’s medical history, which comprised a previous surgery for removal of axillary EBT for aesthetic reasons (which was not complete). The patient will remain in follow-up in our Institution.

