Background
Primary malignant melanoma (PMM) of the parotid is a very rare neoplasm, most likely arising from the melanocytes present in the interlobular duct of the parotid gland [1]. Typically, these are aggressive tumors which occur invariably as metastases from primary tumors located in the region of scalp, mucous membranes of nose, paranasal sinuses, throat, etc. Clinically, PMM of the parotid present as progressively enlarging, firm, asymptomatic, and fixed tumors [2]. However, these tumors often exhibit high potential for metastatic spread to both regional lymph nodes and distant sites, such as liver, lungs, brain, and bones. At the treatment side, total parotidectomy and neck dissection have been advocated as the first line treatment; the role of chemotherapy, radiotherapy, and immunotherapy remains inconclusive. Parotid melanoma, in general, offer poor prognosis and the long-term survival are scarce.
In this study, we present a case of 25-year-old male patient diagnosed with PMM of the parotid. Extensive metastases of the tumor to regional lymph nodes, bones, liver, and pancreas were observed at the time of presentation. This case report illustrates that the PMM of parotid is a highly aggressive malignancy with poor prognosis.
Case Report
A 25-year-old male presented to us with the complaints of a small, firm, progressively increasing nodule over right parotid region for one year duration. Afterward, the patient developed right sided facial palsy for which he underwent total parotidectomy. One month after the surgery, he presented to our Oncology Department. Clinically, there was a 4 × 4 × 5 cm hard fixed mass over right parotid region, a hard fixed mass of 3 × 2 × 3 cm at right submandibular region and right side facial palsy. The patient was addictive of Naswar (tobacco) and possessed lower socio-economic status. The Eastern Cooperative Oncology Group performance status of the patient was one at the time of presentation. Contrast enhanced computed tomography (CT) imaging of the head and neck region demonstrated lobulated mass in the right parotid region (Figure 1) and right deep cervical lymphadenopathy.
Histopathological study of the excised mass (specimen size = 7.5 × 5.3 × 4.5 cm) from right parotid showed a tumor composed of solid nodules and sheets, abundant eosinophilic cytoplasm and prominent nucleoli. Immunohistochemical (IHC) stains showed positivity for HMB45 and S100, while negativity for cytokeratin. These features favored malignant melanoma.
To rule out any possible cutaneous melanoma, complete dermatological survey was performed; however, no positive clinical findings were observed. Additionally, no abnormal mucosal lesions were found on either endoscopy or colonoscopy. Both eyes examination was normal excluding choroidal melanoma.
Post-operatively, the patient had metastatic workup including CT scan imaging of the head and neck region, ultrasound abdomen and pelvis and bone scintigraphy. These studies showed few enlarged lymph nodes in the right deep cervical region and posterior triangle of neck
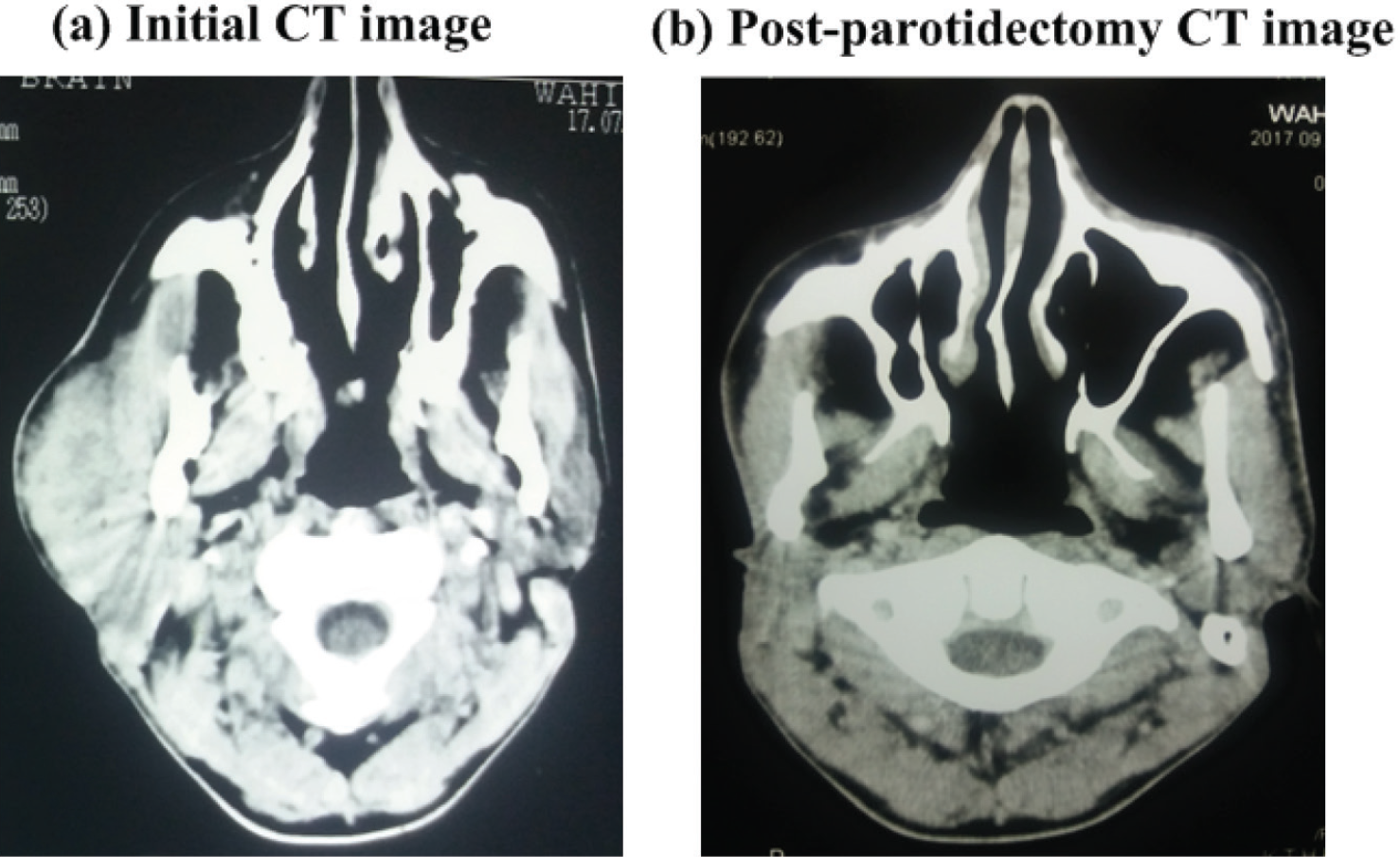
(a) Initial CT image of the head and neck region demonstrating large lobulated mass in the right parotid region, (b) Post-perotidectomy image shows that the mass has been excised; the surgical changes are also evident.
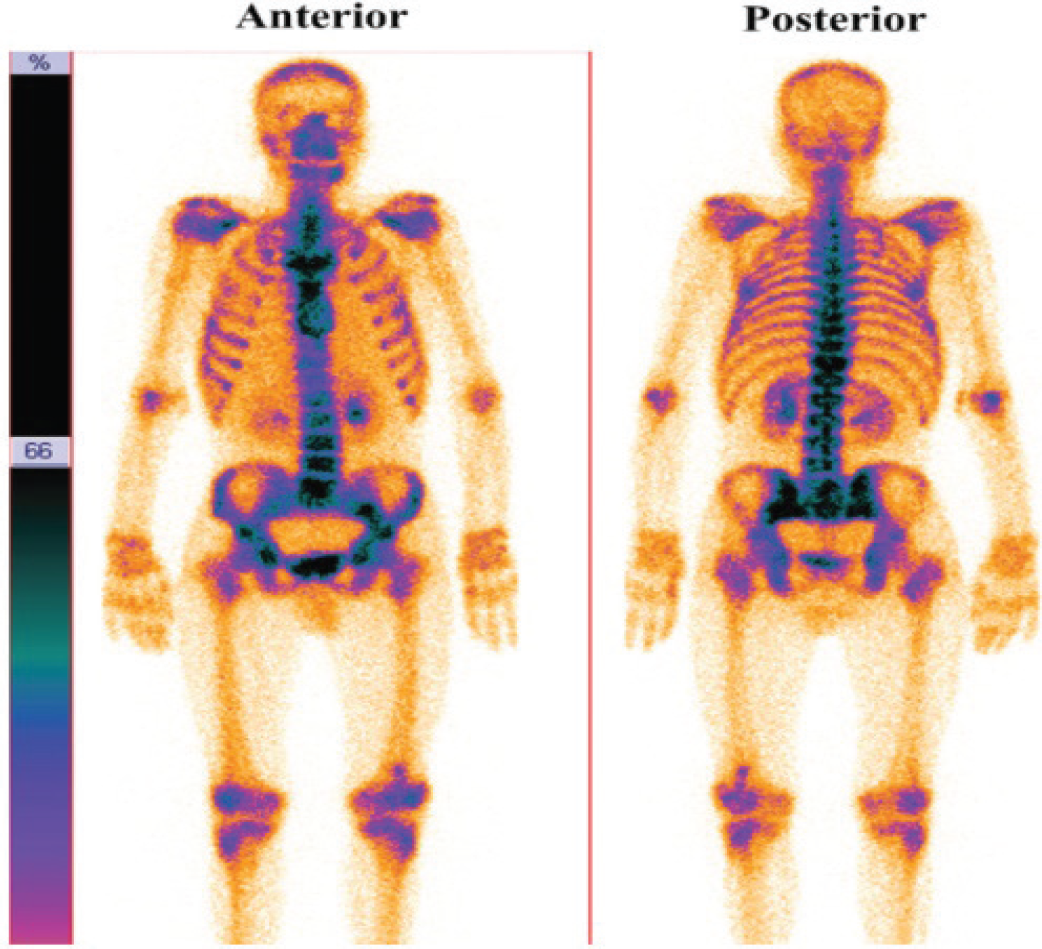
Skeletal scintigraphy demonstrating abnormal radiotracer (methylene diphosphonate labeled Technetium-99m; 99mTc-MDP) uptake in the vertebrae T11 and L5, left sacro-iliac joint and a small focus in distal end of left femur.
(level II and V), multiple hypoechoic variable sized lesions (largest lesion size = 4.5 × 3.9 cm) in the liver, pancreas, multiple lymph nodes in epigasterium and para-aortic regions, and abnormal radiotracer uptake in vertebrae T11 and L5, left sacro-iliac joint and in distal end of left femur, respectively (Figure 2). These findings were most suggestive of metastatic involvement of these sites. All these findings rendered the disease as stage IV.
Post-surgically, the patient was not fit for any oncological treatment (i.e., chemo- or radio-therapy) due to markedly decreased liver function tests, presumably due to the presence of multiple metastatic lesions in the liver.
Discussion
PMM of the parotid is an extremely uncommon malignancy; the typical clinical presentations include solitary, asymptomatic, progressively enlarging, firm, fixed tumors combined with facial nerve palsy [1,2]; the last four of these symptoms were also presented by our patient. Interestingly, amelanotic melanomas may present low or no pigmentation [3]. Additionally, the previously reported mean patient age at diagnosis of PMM is 50–60 years, in contrast to the young patient (age = 25 years) reported in this study [1]. It may be noted that this study is the continuation of our recently initiated program, centralized registry program for uncommon tumors, where incidence of several rare tumors from Pakistan have been reported [4–6].
A distinction between primary and metastatic parotid malignancy can be confounding but essentially required for assessing the therapeutic options and prognosis. That said, although parotid melanomas often represent metastatic lesions, typically from the primary tumors of the cutaneous head and neck regions; PMM of the parotid may also arise from the melanocytes present in the intralobular duct of the parotid gland [7]. In this context, the following criteria have been proposed to differentiate the primary from metastatic parotid melanoma [8]: a) the bulk of the tumor is within the parotid gland; (b) no identifiable lymph node present in the tumor; (c) no evidence of malignant melanoma elsewhere in the body; and (d) no evidence of previous excisions of malignant melanoma or progression of a pigmented lesion. To this end, a detailed history of the lesions that have undergone biopsy is essential. Moreover, a thorough examination of the eyes, nose, pharynx, mouth, skin, esophagus, anogenital region, and meninges of any patient with a parotid melanoma may help in differentiating primary versus metastatic parotid melanoma.
Differential diagnosis of malignant melanoma is often challenging, as the histopathology substrate may have epithelioid, plasmacytoid, spindled, or clear cell characteristics [9]. Furthermore, the malignant tumors of the parotid gland have been reported to comprise of 24 histological types, arising from either epithelial or mesenchymal origin [2]. Nevertheless, the commonly observed histopathology features of malignant melanoma include diffuse cellular arrangement with prominent granular eosinophilic cytoplasm, amphophilic nucleoli, large eccentric nuclei, pigment within adjacent histiocytes, etc. [9,10]. The IHC study, in tandem with histopathology, facilitate the definitive diagnosis of malignant melanoma. Typically, all melanomas illustrate positive staining trend of S-100, HMB-45, vimentin and Melan-A, and negativity of cytokeratin and Pan CK [2,3,9–12], as were seen in this study.
PMM of the parotid is very uncommon but highly aggressive tumor. Previously, the susceptibility for developing metastasis from the parotid tumor has been correlated to four factors: time from initial diagnosis, histopathological type, stage and location of the primary tumor [1]. The parotid PMM express high tendency to metastasize to both regional and distant sites. Metastasis spread occurs predominantly to regional lymph nodes, liver, brain, lungs, and bones [1,13,14]. We also observed extensive metastatic spread to the lymph nodes of ipsilateral cervical, epigasterium and para-aortic, and submandibular region, liver, bone, and pancreas. Moreover, involvement of the facial nerve palsy by parotid malignancy has been reported in approximately 20% cases, as also seen in this study [3,15].
The standard treatment of parotid PMM seems unclear, primarily due to the rarity of the malignancy; nevertheless, total parotidectomy appears the primary therapeutic option of every management strategy. Importantly, several crucial parameters (e.g., primary tumor size, involvement of facial nerve palsy, expertize of the surgeon, etc.) markedly influence the extent of surgical resection and, subsequently, the prognosis. For instance, partial parotidectomy is associated with high risk of recurrence for patients with infiltration of the tumor to the facial palsy [3]. Post-surgical radiotherapy has been speculated as an alternative to the cervical lymph node dissection. Post-surgically, the role of radiotherapy to the tumor bed has been debatable; however, radiotherapy can control the burden of microscopic disease and thereby reduce the risk of recurrence by approximately 6% [14]. The 5-year local control and survival rates for parotidectomy for metastatic melanoma of parotid with adjuvant radiotherapy are 94% and 46%, respectively [9]. Malignant melanoma has been shown to respond to chemotherapy agents, such as dacarbazine, temozolomide, paclitaxel, cisplatinum, docetaxel, and the dacarbazine analogue temozolomide, have been shown to be active in MM [9].
Prognosis of PMM of parotid gland is generally very poor, presumably due to the aggressive nature and high potential of metastasis to local and distant sites. For instance, it has been reported that the cervical lymph nodes involvement by the tumor significantly worsens the prognosis [9]. Notably, Breslow thickness has been speculated as the most important prognostic factor for malignant melanoma. The probability of regional metastasis increases as the thickness of the primary melanoma increases [14]. Additionally, metastasis measuring ≥ 6 cm in diameter and facial nerve palsy are also considered as unfavorable prognostic indicators [10]. The time interval between detection of primary lesion and metastasis is also a crucial prognostic factor [10]. Overall, despite the multimodality treatment, the reported median survival period after metastases from malignant melanoma is eight months [12].
Conclusion
We presented a very uncommon case of PMM of the
parotid gland with extensive locoregional and distant metastatic spread, whose management was carried out with total parotidectomy. Post-surgical radiology studies demonstrated positive lymph nodes in the ipsilateral cervical, epigasterium and para-aortic regions and metastasis to the submandibular region, liver, bones and pancreas. The patient was not fit for any oncologic treatment due to the marked deterioration of the liver function, and thereby kept on the best supportive care. Our study confirmed that the PMM of the parotid is a highly aggressive disease with poor prognosis.

