Background
Subclavian pseudoaneurysm is a rare complication of clavicular bone fracture occurring in about 0.4% of all fractures [1–3]. The unopposed bone edges may injure the underneath subclavian artery. When breach of the injured vessel wall is concealed by hematoma, then a pseudoaneurysm is formed. The turbulence of blood flow within this pseudoaneurysm may cause thrombus formation. This thrombus may dislodge and cause embolization distally to cause an ischemic limb. Theoretically this thrombus may embolized rostrally to the cerebral circulation causing a stroke or transient ischemic attack. However, such is not usually the case as embolus would likely takes the path of least resistance to the limbs rather than to the cerebral circulation. We illustrate a case of subclavian pseudoaneurysm who presented with concurrent upper limb ischemia and transient ischemic attack.
Case Presentation
A 57-year old man presented with sudden onset of left-sided body weakness and inability to speak while reaching out for a drink from his home refrigerator, with his right hand. The deficits lasted for 10 minutes and by the time he presented to the emergency department, it had completely resolved. Nevertheless, the acute stroke team was called upon to attend the patient. The patient was promptly sent for an urgent plain computed tomography (CT) of brain.
His vital signs were as follows: blood pressure 135/85 mmHg, heart rate 80 beats/minute, regular rhythm without discernible neck bruit and auscultation revealed first and second heart sound without additional heart murmur. The plain CT brain revealed neither new, old ischemic stroke changes nor intracranial bleed. He was not given thrombolytic therapy as he was presumed to have had transient ischemic attack. However, his right upper limbs appeared pale and cold on palpation. His right radial and brachial pulses were absent with capillary refilling time of 4 seconds. An impression of acute right ischemic upper limb was entertained. Both vascular and interventional radiology team were referred urgently.
The angiogram study involved the right upper limb, neck, and brain vessels revealed an occlusion of the right ulnar artery with a pseudoaneurysm of the right subclavian artery (Figure 1). The neck and brain arteries were unremarkable, without any stenosis, occlusion, or dissection seen. A CT thorax and neck also revealed an incidental finding of a mal-united right clavicular bone fracture. Hence, a diagnosis of right ulnar artery thrombosis secondary to right subclavian pseudoaneurysm due to recent clavicular bone fracture was made.
A detailed angiography was repeated the next day and the pseudoaneurysm segment was stented by the interventional radiologist. Intravenous heparin infusion was initiated for the right ulnar artery embolic occlusion. Arterial bypass was not performed for the involved upper limb artery as there were adequate collaterals compensating for the thrombosed vessel. The heparin was adjusted based on activated partial thromboplastin time ratio as per local protocol. The malunited right clavicle fracture, which was just adjacent to the pseudoaneurysm, was judged to be stable and hence, no operative intervention was performed (Figure 2).
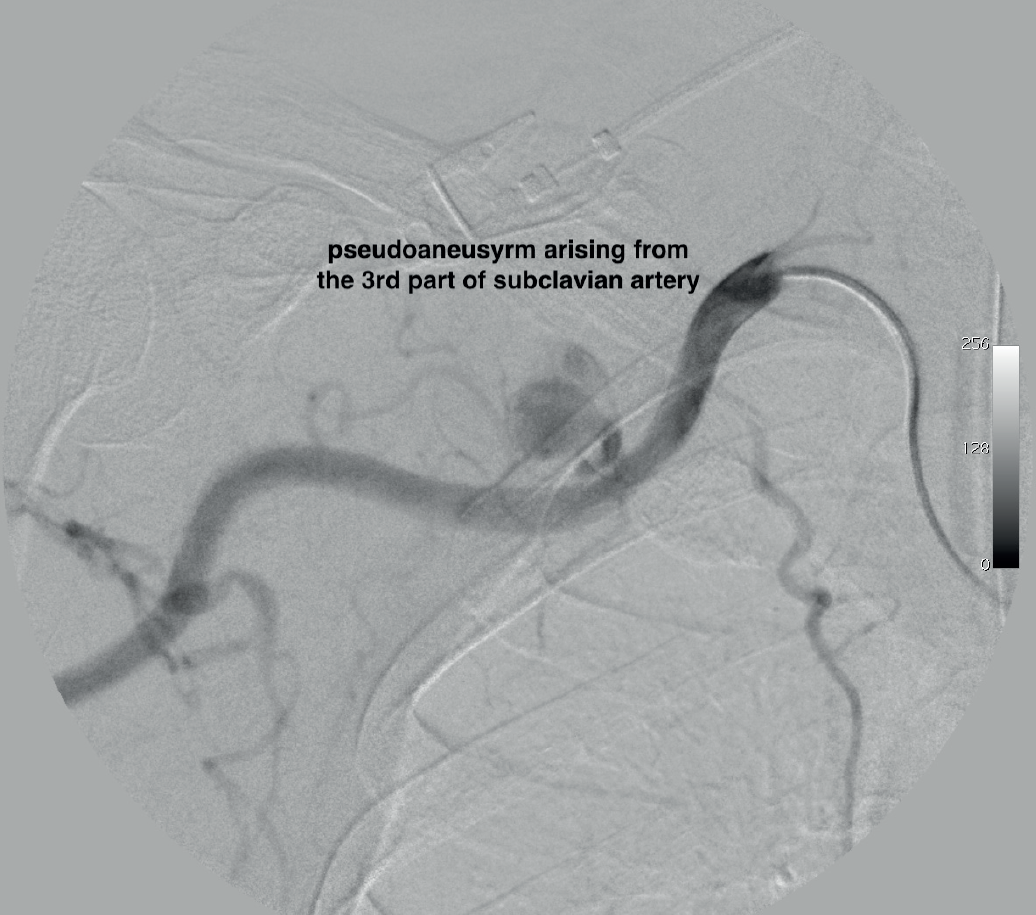
Angiography image depicting the pseudoaneurysm, arising from the 3rd part of the right subclavian artery.
Patient’s affected limb showed gradual improvement in circulation during the first week of heparin infusion. There was neither further transient ischemic attack nor stroke during the admission. On Day 3 of heparin infusion, warfarin was initiated, and heparin was stopped once INR of 2.0 was achieved. He was discharged with warfarin as the etiology of the transient ischemic attack (TIA) was felt to be due to embolism from the pseudoaneurysm which had since been stented.
Retrospectively, patient related to us that he had sustained injury to his right shoulder 2 months ago when he was trying to resolve a fight between two individuals and was hit on the right side, between his neck and shoulder. The affected area had swollen up, which had prompted him to seek medical treatment at a general practitioner clinic where he was given painkiller without any X-ray being carried out. He started to have numbness and paresthesia of his right hand, 3 weeks after the injury accompanied by discoloration. This had prompted him to seek treatment and subsequently diagnosed as having acute ischemia of right upper limb. An embolectomy to the distal limb artery was performed. However, the history of right shoulder injury was not offered by patient as he perceived that piece of information as trivial. There was no swelling seen at the right shoulder during the first encounter. The pseudoaneurysm was only detected 1 month later, when he came again with TIA and recurrence ischemia of right upper limb.
Discussion
Stroke consists of ischemic stroke (80%) and hemorrhagic stroke (20%) [4–6]. The etiologies of ischemic stroke include small vessel lipohyalinosis, large vessel atherosclerosis, embolism from vessel, and heart as well as other rare causes, like thrombophilia [4–6]. When the neurological deficit resolved within 24 hours without any stroke findings in the imaging, then this is termed as TIA [7,8]. TIA is an important syndrome to be recognized because patient with recent TIA may go on to develop full-blown stroke. Hence, an ABCD2 score had been established to determine the risk of TIA progressing to stroke within 48-hours and 7-days period. An ABCD2 score of four and above is considered high risk for stroke, having 4.1% and 5.9% risk of stroke at 2 days and 7 days after TIA, respectively [9]. These high-risk patients may benefit from double antiplatelet agents [10].
Our case highlights a rare possible cause of transient ischemic attack. We have looked at the literature and our case of subclavian pseudoaneurysm as a cause of transient ischemic attack has not been described before. However, cases of innominate artery and brachiocephalic artery pseudoaneurysm causing stroke has been described in the literature [11,12]. One possible mechanism of cerebral embolism for our patient could be due to transient compression distal to the pseudoaneurysm when he flexed his right upper limb to reached out for a drink in the fridge. The transient distal occlusion might have caused differential pressure between the proximal and distal part resulting in embolization to the proximal cerebral circulation. The other postulated mechanism would be a subclavian steal syndrome as a result of differential pressure gradient created due to a proximal subclavian artery stenosis, before the origin of vertebral artery. However, this was unlikely in this case because the pseudoaneurysm was at the distal portion of the subclavian artery.
A complication of subclavian artery pseudoaneurysm as a result of clavicular bone fracture complication is very uncommon and reportedly only occurs in about 0.4% of all clavicular closed fracture [1–3]. This rarity needs to be suspected when a patient complains of ipsilateral limb paresthesia and numbness, few weeks after a fracture. Sometimes a pulsating mass may be appreciated at the supraclavicular fossa representing the pseudoaneurysm. In such complicated cases, vascular repair either through a surgical operation or by interventional radiology procedure of stenting will be required. The fractured clavicle may need to be openly reduced to prevent further vessel injury [1–3].
Conclusion
Although subclavian artery pseudoaneurysm as a cause for transient ischemic attack has not been described in literature, we believe that our case highlighted the possibility of such association. Our case emphasized the importance of comprehensive clinical assessment of acute neurology case so as not to miss out another clinical problem which might be related.
What is New?
Subclavian artery pseudoaneurysm with distal embolization caudally causing ipsilateral limb ischemia is well described in literature. However, this is not the case with distal emboliza-tion cranially to the brain causing transient ischemic attack/stroke. Hence, we are reporting a case of transient ischemic attack who presented with concurrent ischemic limb and subclavian pseudoaneurysm following untreated clavicular bone fracture.


