Background
Kaposiform hemangioendothelioma (KH) is a rare locally aggressive vascular tumor that commonly affects infants and adolescents [1]. Kasabach-Merritt phenomenon is known to be associated with KH [2]. The first case of Kasabach-Merritt syndrome with the constellation of thrombocytopenia and cavernous hemangioma was described by Kasabach and Merritt [3]. The diagnosis of Kasabach-Merritt syndrome is based on the association between a vascular lesion, thrombocytopenia, consumptive coagulopathy, and microangiopathic hemolytic anemia. The pathophysiology is believed to be due to platelet destruction by the intravascular coagulation within the tumor [4]. Magnetic resonance imaging (MRI) is a helpful tool in this field. In our case, the diagnosis of KH was made by radiological findings in MRI with a clinical correlation.
Case Presentation
A 2-month-old male child presented as a casualty with rapid breathing and interrupted feeding for 2 weeks. There was no history of documented fever, trauma, or foreign body ingestion. He was delivered via spontaneous vaginal delivery to non-consanguineous parents. He was diagnosed to have right lower limb and right scrotal hemangioma since birth. The abdomen was distended with hemihypertrophy of the right lower limb (Figure 1). Bruises along the right side of the abdomen and right lower limb were noted to be worsened in parallel with his illness. Blood investigations in the casualty showed severe uncompensated coagulopathy: hemoglobin = 2.7g/dl, platelets = 64 × 109/l (normal 150-450 × 109⁄l), prothrombin time = 18.7 seconds (normal: 10.0-14.2), activated partial thromboplastin time = 41.1 seconds (normal 28.1-42.9), and INR = 1.72. Physical examination noted violaceous discoloration of the abdomen and right leg with dilated vessels visible in his abdominal wall. Biopsy was deferred due to his critical status and coagulopathy. The patient received several packed-cell and platelet transfusions but without successful increment of the cell counts significantly. The hemoglobin level raised up to 5.1g/dl, but the platelet count drastically dropped to 3 × 109/l 4 days later.
Radiography showed diffuse opacity in the subcutaneous tissues of the right side of the abdomen and right lower limb (Figure 2). Ultrasound abdomen showed multiple cystic lesions in the pelvis with bilateral mild hydronephrosis. Otherwise, there was no focal lesion in the liver, spleen, and both kidneys. The differential diagnosis of Kasabach-Merrit syndrome was raised in view of underlying cutaneous hemangioma with concurrent coagulopathy. MRI of the brain, abdomen, and right lower limb was carried out to obtain better resolutions of the mass and information regarding its vascularization. MRI revealed a large right-sided mass with ill-defined borders that permeated through the surrounding fat tissues extending from the right side of the trunk to the right lower limb, consistent with a Kaposiform hemangioendothelioma (Figures 3 and 4). These lesions were heterogeneously hyperintense on T2-weighted images and isointense on T1-weighted images, compared with the skeletal muscle. There were multiple cystic structures in the pelvis causing compression of the ureters resulting in bilateral mild hydronephrosis (Figure 5). The diagnosis was then rectified to Kasabach-Merritt syndrome (KMS) with the constellation of thrombocytopenia, consumptive coagulopathy, and KH.
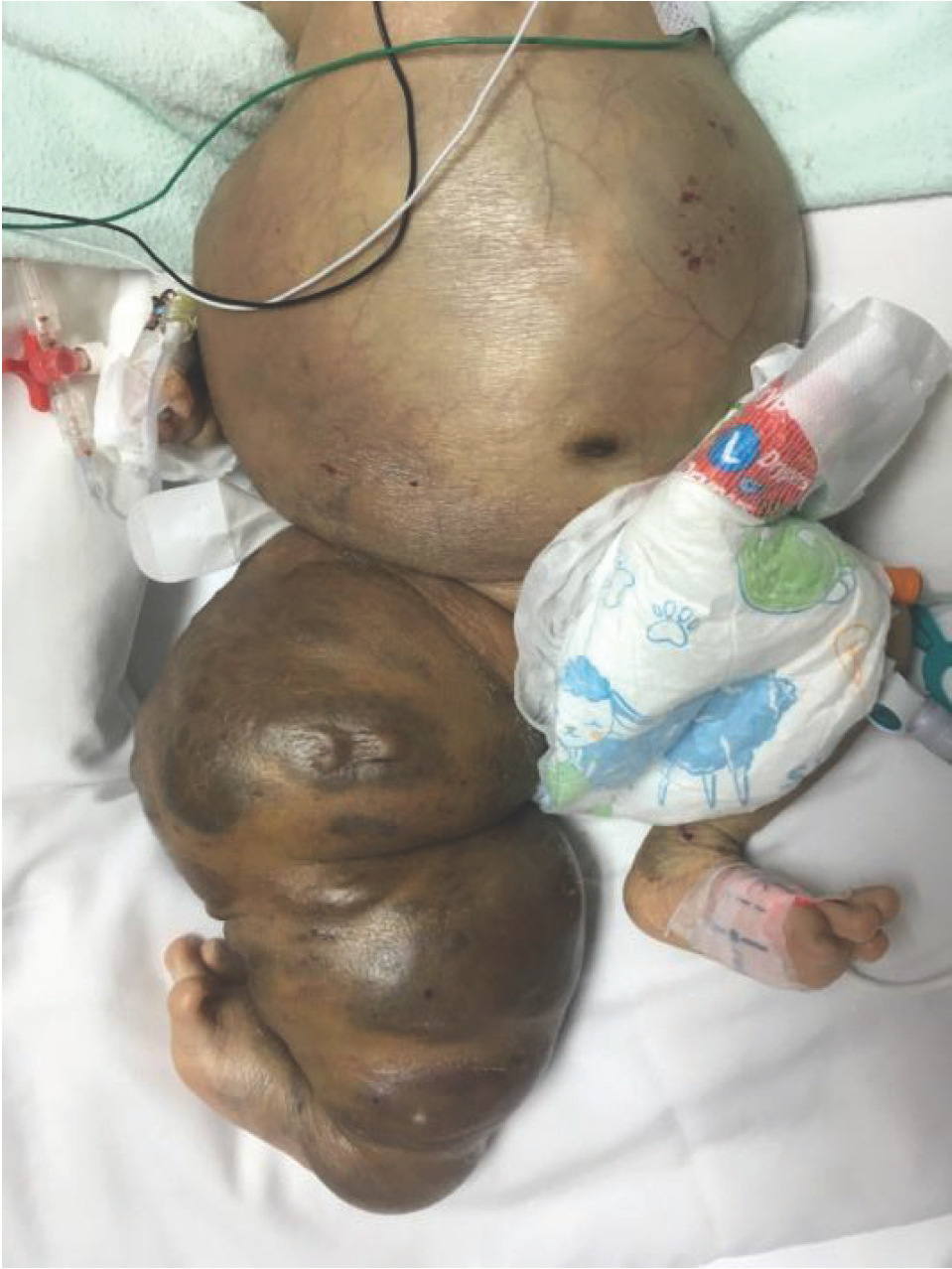
Violaceous discoloration, purpura, and woody induration of the abdomen and right lower limb at presentation.
His hospitalization was complicated with blood stream infections in which the blood culture grew Morganella morganii that further suspended the initiation of chemotherapy. He was treated with IV antibiotics and blood transfusions. The patient was referred to a higher specialized center for further evaluation by the pediatric dermatologist, who agreed with the plan of management. His condition deteriorated with time and sadly he succumbed to the illness after a month in the hospital despite the continuous supportive treatment.
Discussion
Kaposiform hemangioendothelioma is a rare vascular neoplasm that is of endothelium-derived spindle cell origin and is seen predominantly in the pediatric age group. The incidence is estimated to be 0.07/1000,000 children per year [5]. It is usually locally aggressive and rarely demonstrates a metastatic potential [1]. It was first described by Zukerbert et al. [6] in 1993. KH tends to be a locally aggressive tumor that may involve superficial or deep soft tissues [4]. Majority of the cases (75%) present as cutaneous lesions of trunk and extremities, followed by retroperitoneal involvement (18%) [2,7]. The limbs, retroperitoneal and mediastinal lesions are generally related to KMS and lymphangiomatosis [8]. Lesions in the extremities and the retroperitoneum are more likely to be associated with Kasabach-Merritt phenomenon (KMP). The association between rapidly enlarging capillary hemangioma and thrombocytopenic purpura was first reported by Haig Haigouni Kasabach and Katharine Krom Merritt in 1940 [3]. The combination of vascular tumor (that can be found in cutaneous plane, retroperitoneum, mediastinum, pelvis, visceral organs, and mesentery), thrombocytopenia, and consumptive coagulopathy is well recognized in KMS or KMP [4]. KMS is complicated with a variety of vascular tumors and KH is a vascular tumor known to cause KMS according to the International Society for the Study of Vascular Anomalies [9]. KMS should be at the top of the list with the presence of unexplained thrombocytopenia and consumptive coagulopathy. Common presenting features include purpura, edema, induration, and ecchymotic margin as seen in our case [10]. The incidence
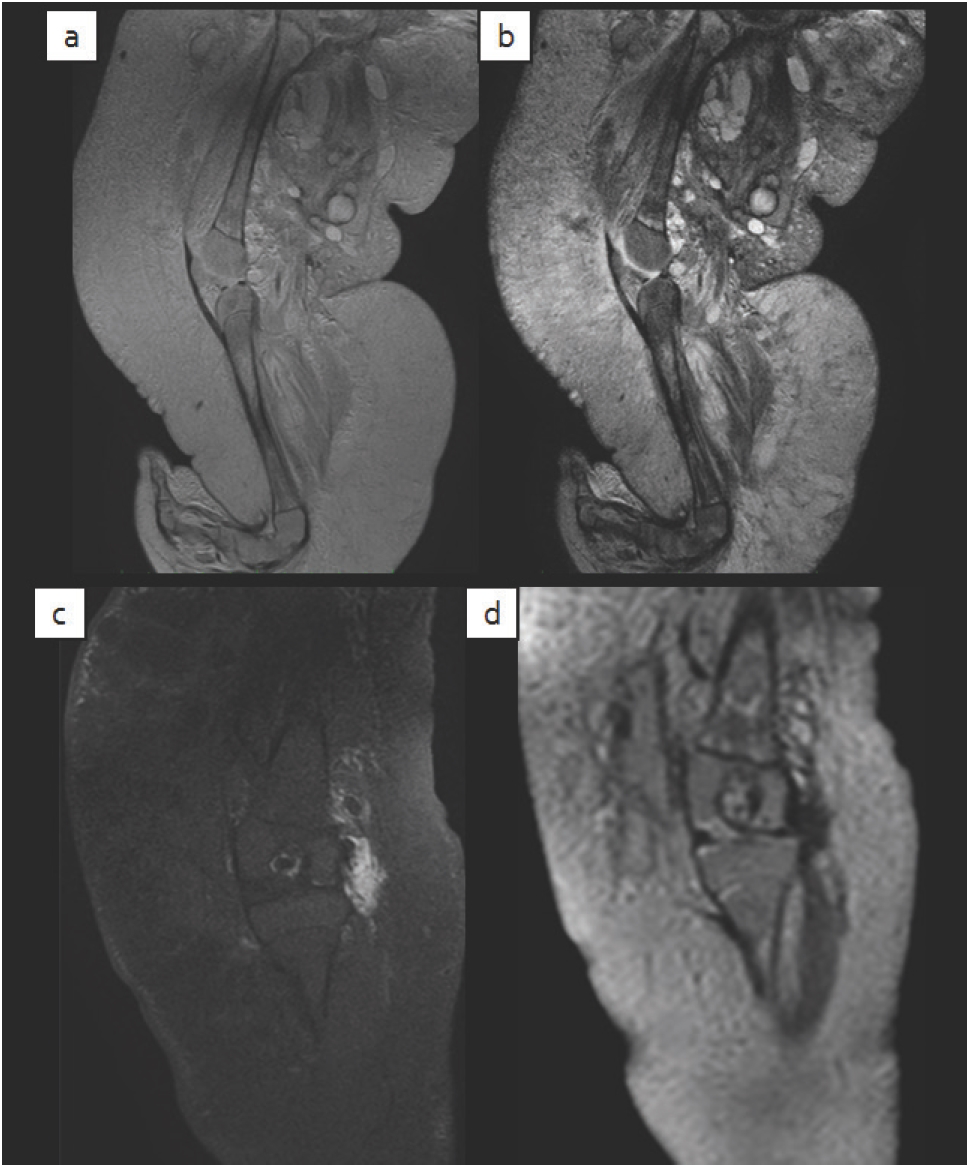
(a) Sagittal T2WI, (b) sagittal PD, (c) coronal T1WI, and (d) coronal T1WI post-contrast. MRI of right thigh demonstrate ill-defined minimally enhancing infiltrative large T2WI hyperintense and T1WI hypointense lesions involving the subcutaneous layer of the thigh associated with dermal and subcutaneous thickening and infiltration. Extension into the adjacent muscles with edema is also noted and suggestive of KH.
of KMS in patients with KH is 70% [5]. Generally, the overall mortality rate ranges from 12% to 30% [2]. This is commonly caused by catastrophic bleeding related to disseminated intravascular coagulation, local infiltration of the vital organs, high output cardiac failure, multiorgan failure, or septicemia [10]. Our case was diagnosed to be infantile hemangioma in the beginning as the infant was born with right lower limb swelling and skin discoloration without noticing the derangement of the blood parameters. A malignant vascular tumor cannot be suggested until further imaging follow-up is carried out. The rapid progression of right lower limb swelling associated with multifocal bruises led to the consideration of a more aggressive tumor than hemangioma. Thrombocytopenia, derangement of the coagulation profile, and the presence of vascular tumor from radiological evaluation eventually led to the diagnosis of KMS secondary to KH in this case. Imaging evaluation is useful in establishing the diagnosis and in determining the extent of involvement. It also plays an important role in monitoring the treatment response. Ultrasound imaging is fundamental in delineating and characterizing a vascular lesion in the pediatric group [11]. However, due to its intrinsic limitation for instance, to clearly define the extension of a deep lesion as present in this case, MRI is particularly valuable to further evaluate the lesion. Angiography is useful in mapping the feeding vessels when embolization is planned. Sarkar et al. [2] described KH as a lesion that was poorly defined, involving multiple tissue planes and associated with cutaneous thickening and edema in MRI. The feeding and draining vessels are relatively small and infrequent in comparison with common hemangioma. Biopsy of the lesion confirms diagnosis and aids in planning the type and duration of chemotherapy. KH is congenital in majority of the cases, while infantile hemangioma is not fully developed at birth [12,13]. Hemangioma is usually not yet visualized at birth but rapidly progresses in the first week. Our patient was noted to have right lower limb abnormality at birth, whereby the possibility of a more sinister diagnosis needs to be considered than a benign condition like hemangioma. In contrast to infantile hemangioma, which has a tendency to regress spontaneously, KH results in higher mortality and morbidity due to its local invasive behavior. KH usually presents as an infiltrating soft tissue lesion with associated violet skin discoloration in contradistinction to infantile hemangioma that tends not to penetrate into the adjacent structures (14). As in this case, imaging could be the key factor to make the diagnosis right from the beginning. By and large, ultrasonogram shows a well-demarcated high-flow lesion with possible shunting in infantile hemangioma [14]. In studies by Young et al. [15], all KHs are ill-delineated, heterogeneous in echotexture, and predominantly hyperechoic in ultrasound. 57% of the cases were noted to be marked hypervascular mass, whereas the rest showed mild increment in vascularity. Most of the infantile hemangiomas manifest as well-defined, marked T2-hyperintense lesions with homogeneous enhancement
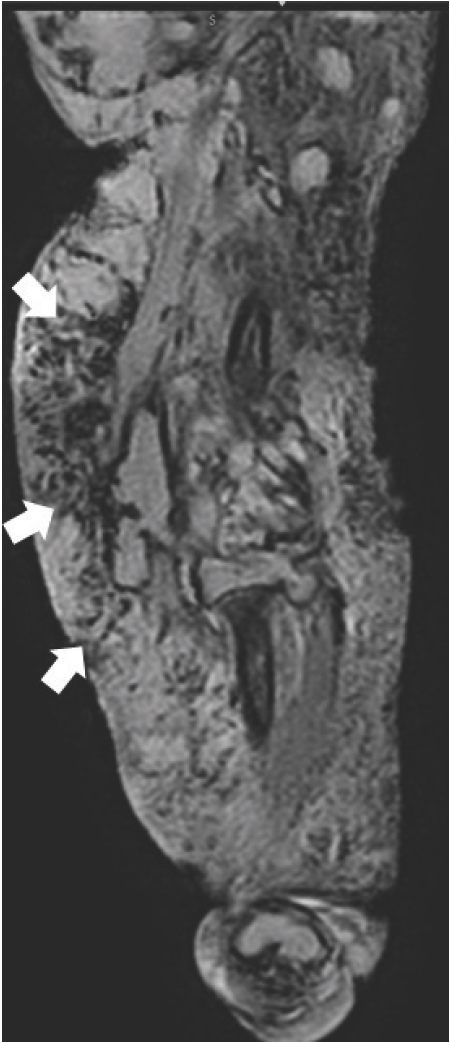
Sagittal GRE sequence demonstrating multiple engorged vessels (white arrows) in the periphery of the lesion in the right lower limb.
and without local invasion [16]. Young et al. [15] reported that the majority of the KH masses are relatively large, with a mean maximum diameter of 8.6 cm. Our case showed that the lesion is extensive involving the entire right lower limb and occupying almost the whole abdomen with local infiltration, which is quite characteristic of KH. Besides, it has poorly delineated borders extending into the contiguous subcutaneous tissue and muscle layers. KHs exhibited a heterogeneous enhancement in all cases reported by Young et al. [15]. However, we have not found this distinction (contrast enhancement) to be helpful in our decision-making as the lesion did not demonstrate significant enhancement. The outcome of KH is influenced by the characteristics of the tumor, timing of the diagnosis, and commencement of proper treatment [17]. The mainstay of treatment is to involute the tumor in alleviating the life-threatening coagulopathy [18]. Surgical excision remains as the curative treatment but most lesions are not feasible to this option. High-dose systemic corticosteroids are the first line of treatment. However, poor response to the drug was reported and rapid relapse had occurred after the treatment was withdrawn [12]. Also, inevitable adverse effects following high-dose steroids are well recognized. Recombinant interferon α (both 2a and 2b) has been tried with variable results in cases of steroid-resistant vascular tumor [19]. Some alternative therapies, like cryotherapy and laser therapy, are limited to relatively small and superficial tumors. Radiation and chemotherapeutic agents, such as vincristine and actinomycin, are other modalities of treatment. Only supportive treatment was given to our patient as the infection was limiting. Surgical intervention was impossible with coagulopathy. In conclusion, KH is a rare extremity and retroperitoneal tumor and may easily be overlooked as hemangioma on initial assessment. When evaluating a pediatric patient with vascular tumor and coagulopathy, its association with KMS should always be borne in mind so that aggressive and optimal treatment can be delivered on time with early diagnosis. The clinical, imaging, and pathologic features of KH are different from those of infantile hemangioma. Imaging plays an important role in helping to establish the diagnosis if pathological diagnosis is not feasible. In reference to most of the clinical studies, the use of medical treatment is rather encouraging but the patients have to be monitored for the complications.
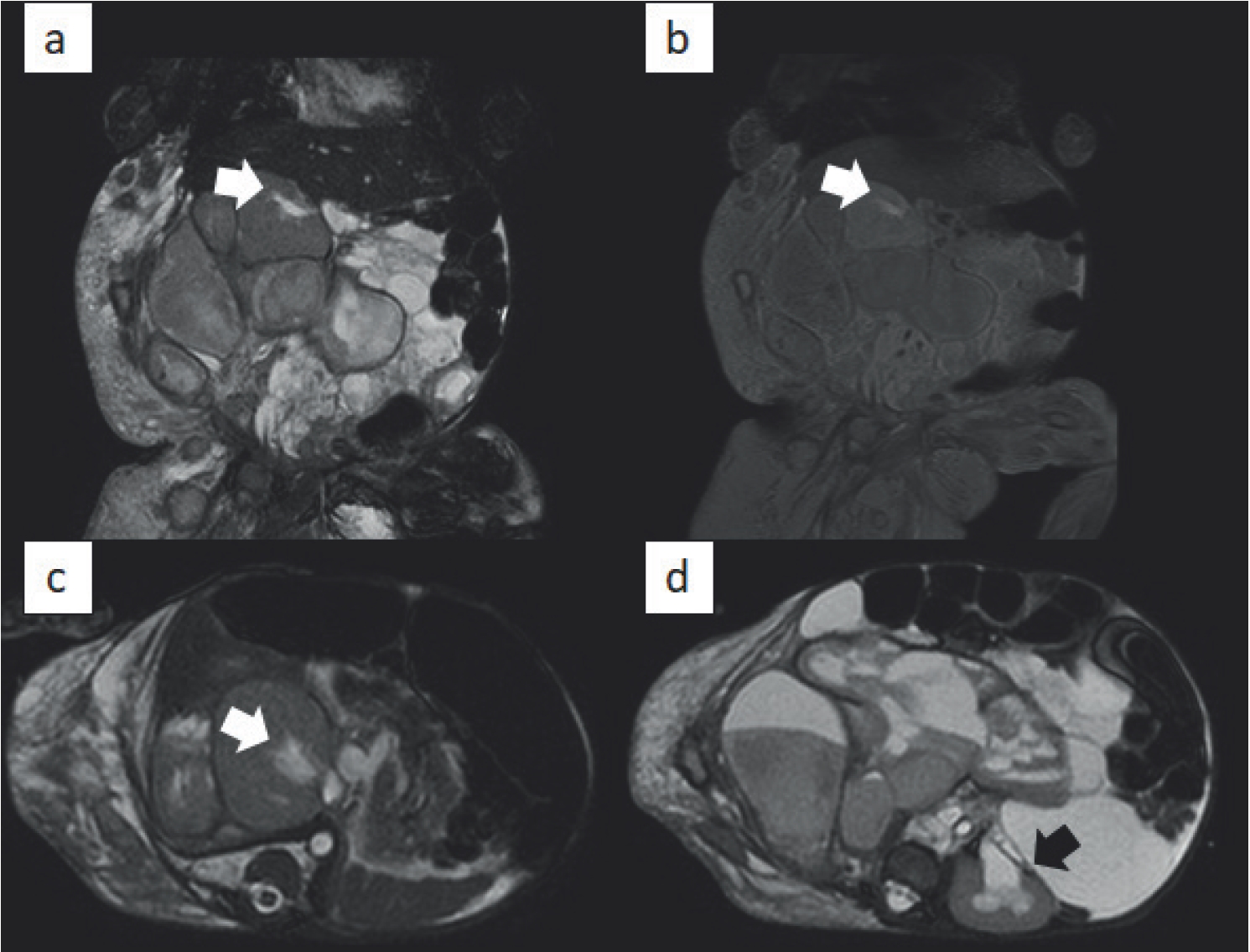
(a) Coronal BTFE, (b) coronal T1W FS post-contrast, (c, d) axial BTFE MRI of the abdomen. Multiple cystic lesions exhibiting heterogeneous signal intensity and minimal enhancement with extensive subcutaneous thickening and edema. Mass effecting the ureters resulting in hydronephrosis (white arrow: right kidney and black arrow: left kidney) is also noted.


