Background
Synovial lipoma is also known as lipoma arborescens or villous lipomatous proliferation of the synovial membrane. It is an uncommon, benign proliferation of subsynovial membrane containing infiltrating and proliferating fat. The lesion is common in the articular synovium of knee joints of adult patients. It can occasionally be bilateral and may involve multiple joint. Although this process is more likely reactive than neoplastic in origin, it is rare with unknown etiology. There is limited literature on this topic to guide both diagnosis and optimal treatment of this disease [1]. In majority of cases, synovial lipoma occurs de novo. Previous trauma, chronic rheumatoid arthritis, osteoarthritis, psoriasis, and baker cyst are among the associated conditions [2,3]. Patients typically present with pain and swelling of the affected joint. In our case, synovial lipoma was an incidental finding in a patient suffering from unilateral knee joint chronic synovitis for a long duration. Although it appears to have a predilection for the knee, synovial lipoma has also been reported in the wrist and ankle, indicating that it could be a rarer cause of pain in smaller joints [4]. The recommended treatment is complete synovectomy either arthroscopically or via formal open debridement.
Case Presentation
A 17-year-old female with high body mass index, had presented with pain and swelling in her left knee from past two years. In its early course pain was episodic in nature. Gradually it became progressive. Pain was also associated with stiffness in her knees. No history of trauma was present. No family history of similar complains was present in the family. Physical examination revealed swelling and crepitation in her left knee joint. There was no tenderness along with the joint line. Redness and local rise of temperature was present. Her routine hematological workup was negative for any inflammatory arthritis. Erythrocyte Sedimentation Rate was 15 mm in first hour. C-Reactive protein was 0.84 mg/dl. Serum uric acid and serum calcium levels were within normal limits. There was no history or clinico -pathological findings which were suggestive of tuberculosis. Rheumatoid Arthritis (RA) factor was negative. Synovial fluid aspiration smears were non-haemorrhagic and non-inflammatory and they did not reveal any organism on microbiological examination. X-ray findings showed a soft tissue shadow which measured 2.5 × 1cm. She was planned for left knee synovectomy due to progression of the disease, pain and disability. Intraoperatively a yellowish, fatty, soft tissue measuring 6 × 3 × 1 cm was removed from her left knee joint. A hypertrophic lipomatous nodule was sent for histopathological examination to our department (Figure 1)
Grossly the tissue has a yellow fatty appearance with papillary projections. Microscopy of the received specimen showed multiple villi like projections lined by hyperplastic synovium and the subepithelial tissue was infiltrated by abundant benign mature adipocytes. Synovial tissue also showed moderate degree of infiltration by lymphoplasmacytic cells and dilated and congested blood vessels. The overall appearance was consistent with synovial lipoma (Figure 2). Her postoperative recovery was uneventful.
Discussion
Synovial lipoma is a rare benign disease which typically presents with symptoms of swelling and joint pain [5]. An intra-articular lipoma is a variant which is defined by its typical intra-articular location, which constitutes less than 1% of all lipomas [6]. In the intra-articular location, the knee joint is most commonly involved. Other sites which are less commonly involved are hip elbow, shoulder, and spine [7]. The review of literature reveals that synovial lipoma commonly affects males. Commonest age group is between 50 and 70 years with mean age of 45.6 years [8]. The exact aetiopathogenesis of synovial lipoma is not clear. It is often diagnosed in patients with inflammatory diseases [9]. It has been documented that it can be due to trauma, inflammation, rheumatism, development of neoplastic pathology and obesity. Patients usually present with pain and swelling of the affected joint with or without restriction of movements. Proliferation of synoviocytes may result in joint effusion [4].
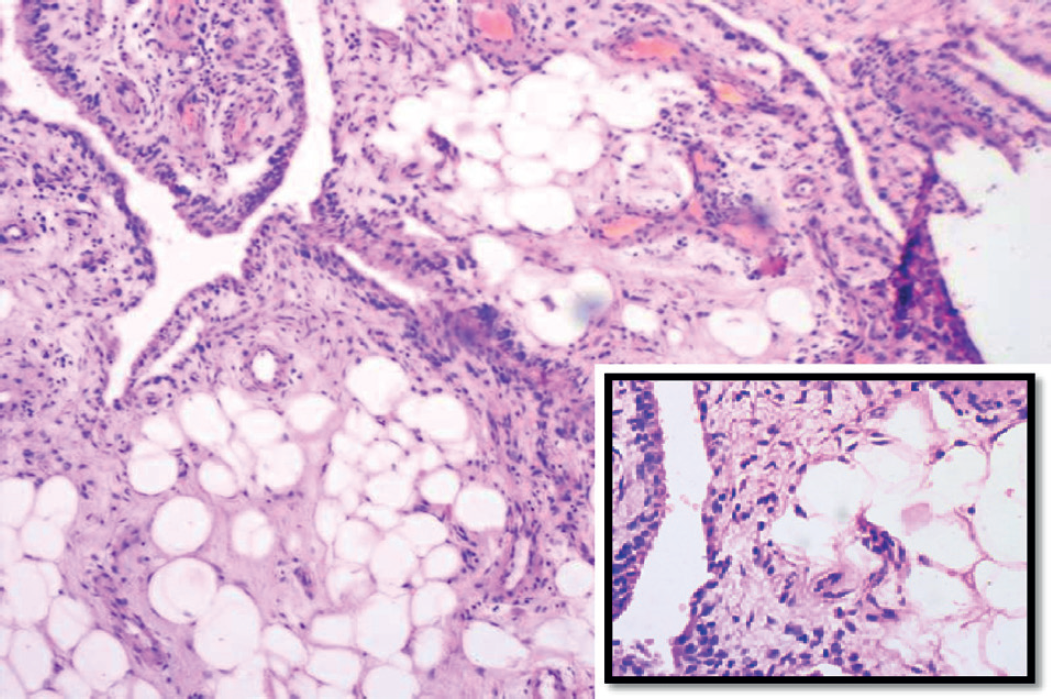
Microphotographs showing villi-like structures lined by synovial epithelium. The subepithelial area show focal infiltration by mature adipocytes (Hematoxylin and eosin, ×10), inset show fat cells in tissue lined by synoviocytes (Hematoxylin and eosin, ×40).
Synovial lipoma can be differentiated from other diagnoses by particular characteristics. Differential diagnoses are synovial chondromatosis, pigmented villonodular synovitis (PVNS), synovial hemangioma, RA, and osteoarthritis. When compared to PVNS, synovial lipoma can be differentiated by lack of hemorrhage and hemosiderin on histology. Hoffa disease is limited to the infrapatellar fat pad and is typically post traumatic [1]. Thorough knowledge of the differential is imperative in attaining the correct diagnosis.
Treatment of synovial lipoma consists of arthroscopic synovectomy or open synovectomy depending on the extent of the lesion [9].
Conclusion
Synovial lipoma is a rare diagnosis, but should be considered in the setting of refractory chronic joint effusions and knee pain. The etiology is currently unknown. This is often diagnosed in patients with inflammatory diseases. However, high body index can be one of the causes as seen in this case. Either way, more research is needed to better understand the cause of this disorder, the optimal diagnostic evaluation and treatment. This case increases awareness of this rare disease. This entity may be missed if the clinician does not have a high index of suspicion, especially in the setting of a young patient with chronic refractory knee pain and an otherwise negative work up. Our case presentation is limited to one individual; however, it demonstrates the need for further studies as this is an identifiable entity with successful treatment options.


