Background
Polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes (POEMS) syndrome is a rare plasma cell dyscrasia [1]. However, the acronym presents less than half of the defining features of the disease [2]. It was argued that the treatment of POEMS syndrome needs reconsideration and a proper patient education should be stressed to optimize the management and thereby minimize the side effects. In this case, an atypical case of POEMS syndrome was reported with mixed lytic and sclerotic bone lesions complicated by deep vein thrombosis (DVT) as a side effect of lenalidomide therapy. In addition, several factors were emphasized, which might play a role in thromboembolic complications of this disease.
Case Presentation
A 43-year-old male patient was referred to the neurology clinic from the neurosurgery department with the insidious onset of progressive lower limb weakness with difficulty in walking and erectile dysfunction within 4 months’ duration, without any history of bladder or bowel disturbances. There was no recent history of diarrhea, viral illness, or any significant family history. The patient was shown to have bilateral foot drop and decreased sensation in the lower limbs, and deep tendon reflexes of the lower extremities were also absent. Subsequent visits revealed nail thickening, hepatomegaly, a plethoric face, and ascites. Before his referral, the patient had a magnetic resonance imaging (MRI) for a suspected lumbar disc prolapse, which was found to be normal. Later, nerve conduction studies were done, and a significant reduction in amplitude and velocity of the lower limb nerves was shown. On admission, complete blood count (CBC) tests revealed hemoglobin (Hb) levels of 19.4 g. The subsequent investigations showed that serum proteins were 7.5 g (albumin 4 g and globulin 3.5 g), and the serum protein electrophoresis showed a monoclonal band of IgG with lambda (λ) light chain restriction. Urinalysis was found negative for Bence-Jones proteins, and the serum levels of adrenocorticotropic hormone were less than 5 pg/ml. Full-body computed tomography (CT) scan showed hepatomegaly (Figure 1), inguinal lymphadenopathy (Figure 2), and multiple mixed lytic/sclerotic bone lesions scattered in the thoracic and lumbar vertebrae, sternum, and pelvis (Figures 3 and 4).
Bone marrow needle biopsy showed hypercellular bone marrow with estimated cellularity of 60% and up to 20% atypical plasma cells, which was unusual for POEMS syndrome that formed one large aggregate with lambda (λ) light chain restriction. The aspartate aminotransferase (AST) and alanine aminotransferase (ALT) levels were normal (39.6 and 15.7 U/L, respectively). However, the fundoscopy to check for papilledema was refused by the patient. A diagnosis for POEMS syndrome was made, and the patient was started on lenalidomide (25 mg PO qDay on days 1–21 of repeated 28-day cycles) plus dexamethasone (40 mg PO qDay, on days 1–4, 9–12, and 17–20 of each 28-day period; after two cycles, the patient was shifted to 40 mg once weekly).
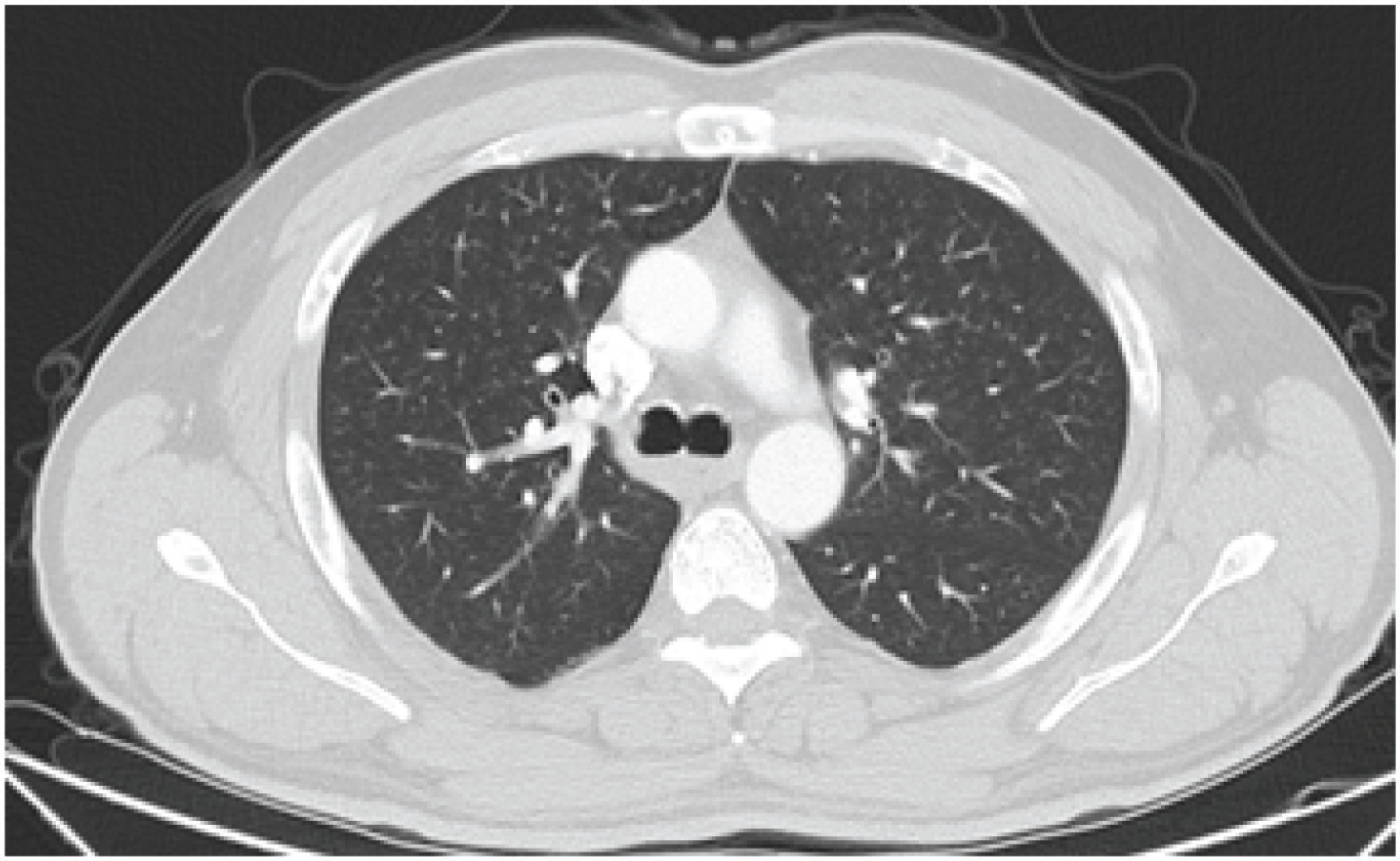
An axial CT scan showing sternal osteolytic lesion with sclerotic rim, accompanied by other sclerotic lesions in the sternum and the vertebral body.
| Mandatory criteria | Polyneuropathy (typically demyelinating) Monoclonal plasma cell proliferative disorder (almost always lambda) |
| Major criteria | Castleman disease Sclerotic bone lesions Vascular endothelial growth factor elevation |
| Minor criteria | Organomegaly (hepatomegaly, splenomegaly, or lymphadenopathy) Extravascular fluid volume overload Endocrinopathy Skin changes Papilledema Thrombocytosis/polycythemia |
| Other signs and symptoms | Digital clubbing, weight loss, hyperhidrosis, pulmonary hypertension/restrictive lung disease, thrombotic diathesis, diarrhea, low Vitamin B12 values. |
Due to the high thromboembolic risk of lenalidomide, the patient was also given prophylactic low molecular weight heparin (tinzaparin 4,500 mg once daily). At the end of the second lenalidomide cycle, the patient did not take his prophylactic heparin dose, after which lenalidomide was stopped in the 4th week of the period. The patient reported that he took low-dose aspirin instead because tinzaparin was not available at nearby pharmacies.
Consequently, a DVT was developed. Tinzaparin dose was increased to 14,000 mg qDay for treatment. On subsequent visits, the patient’s peripheral neuropathy improved, and the patient was able to walk with crutches after using a wheelchair. Later, the patient was transferred from the present institute to King Hussein Cancer Center for a scheduled bone marrow transplantation.
Discussion
Clinical suspicion of POEMS should be evoked in patients with peripheral neuropathy of unknown origin accompanied by other multisystemic findings. The case was initially presented with insidious onset of lower limb weakness of 4 months’ duration. To establish the diagnosis of POEMS syndrome, the International Myeloma Working Group criteria were derived from previously published Mayo Clinic studies. The standards implied that all patients should have peripheral neuropathy and a monoclonal plasma cell disorder as mandatory criteria. The rest of the clinical features had been divided into major and minor criteria. To make the diagnosis, the patient must have the necessary criteria, plus one major and one minor rule (Table 1). The reported case was manifested with all the classified mandatory, major, and minor standards at the time of presentation except for papilledema. Lymph node biopsy was refused by the patient to see whether Castleman disease was present. However, the patient had multiple enlarged lymph nodes on the CT scan, which might be indicative of Castleman disease. The co-occurrence of these findings in a single patient was considered rare [3]. Bone lesions were the defining feature of this syndrome, most injuries were sclerotic, and lytic lesions with a sclerotic rim or a mixed soap-bubble appearance have been reported rarely [4]. The patient had a diffused vertebral involvement of mixed lytic and sclerotic lesions, which was uncommon. In contrast to multiple myelomas, there was no standard treatment for POEMS syndrome available in literature [5].
The mainstay of therapy includes bone irradiation, systemic corticosteroids, high-dose chemotherapy, and peripheral blood stem cell transplantation [5]. Lenalidomide is one of the indicated chemotherapeutic agents [6]. The patient had an episode of DVT, which could be attributed to several factors in patients with POEMS syndrome generally, such as immobilization (due to neuropathy and lower limb weakness), disease-related polycythemia and thrombocytosis. Furthermore, the chronic inflammatory state the patient was involved in and lenalidomide therapy, which is well known for its significant venous thromboembolic effects, are also thought to be potential triggers of DVT in these patients. Menon et al. [7] had reviewed the incidents of lenalidomide associated with venous thromboembolism among patients with multiple myeloma. It was argued that lenalidomide should be replaced with another chemotherapeutic agent to limit the potential triggers of DVT in these patients for better long-term management and prevention of other thromboembolic complications.
Conclusion
Alternative treatment options that are used for POEMS syndrome include bortezomib-based therapy. Bortezomib is associated with peripheral neuropathy, which may worsen this patients’ preexisting peripheral neuropathy. In contrast, melphalan plus prednisone had shown reasonable chemotherapeutic response rates in the Mayo Clinic case series with a low side effect profile [3].
Although rare, the diagnosis of POEMS syndrome should be suspected in a patient with gradual onset peripheral neuropathy accompanied by other systemic manifestations. The case represents an atypical presentation of POEMS syndrome, in which the disease-related thromboembolic burden is highlighted. Given this fact, using a medication such as lenalidomide might be hazardous in these patients. Further studies should be conducted to compare the available regimens for the treatment of POEMS syndrome.




