Background
The differentiation between organic/secondary and functional/primary psychosis is an area of contention between psychiatrists and neurologists and also within each of these specialties. In describing psychopathology, a distinction between delusion, illusion, and hallucination terminologies is made to provide diagnostic demarcations between various psychiatric disorders. However, this does not help in understanding the basic mechanisms behind symptoms at a neurological level. In contrast, one aspect of neurology is to study the aetiology of these terminologies at the organic interface of epilepsy, where intracranial stereo-electroencephalography (SEEG) is used to provide a more synoptical definition [1]. The overlap in the physiological basis of these phenomena has resulted in the conclusion that there is little point in differentiating hallucination from illusion or delusion.
Case Report
We present the case of a 51-year-old single female patient with a diagnosis of treatment-resistant schizophrenia who over the course of 28 years had been trialed on multiple antipsychotics including combined therapies with little effect on her unremitting symptoms. Over this period she also had four psychiatric admissions in the context of psychosocial stressors and poor adherence to medications.
The patient’s reported psychopathology at her first encounter with us was that of chronic beliefs that her brain was missing and she was seeing her organs move in and out of her body. This triggered anxiety as she was spending a great deal of time “willing” her organs to work. Additional beliefs were that she could read minds and control others using her thoughts. She reported seeing her thoughts in the form of bubbles floating outside of her body and her “spirit” as a shadow moving around her. Apart from experiencing auditory hallucinations at the onset of her illness in her early 20s, this was not a prominent symptom that persisted. She had mixed feelings about her symptoms as she believed these experiences made her “special” but also viewed her symptoms as distressing and unwanted.
Previous therapeutic trials included pimozide, olanzapine, and risperidone, then more recently zuclopenthixol decanoate depot intramuscular injection. She experienced a mild reduction in her symptoms on zuclopenthixol depot medication but continued to have unremitting visual and somatic perceptual and delusional disturbances. She denied any recreational drug use and drank alcohol moderately.
Past medical history includes chronic dermatitis, idiopathic bilateral pulmonary emboli (PE) for which she received anticoagulation therapy, bilateral thinning corneas and chronic blepharitis, renal stones with intermittent hematuria, cervical degenerative disc disease and chronic arthritis. The peculiarity of this patient’s psychopathology comprised the predominately visual hallucinations and somatic delusions that were unremitting on antipsychotics for years. Moreover, she had a consistently warm affect and ability to demonstrate empathy. The course of her illness also notably lacked the usual deterioration of personality that is commonly seen in schizophrenia. Therefore, further investigations and referral to specialists were instigated to consider organic/secondary causes for her symptomatology.
Investigations and special referrals
Investigation of dermatological conditions
Longstanding chronic dermatitis and excoriation of skin were present since early childhood. Skin biopsies confirmed a diagnosis of chronic spongiotic changes in keeping with chronic dermatitis. Topical steroid cream was offered as a systemic approach but was known to aggravate her psychosis.
Laboratory investigations
Routine tests. Routine bloodwork for glucose, liver and renal functions, as well as thyroid functions, were all essentially normal.
Her prolactin was found to be consistently raised, as expected, from treatment with antipsychotic medication. There were also occasions dating back from 2010, where there were changes in urea, potassium, and sodium that were not attributable to medications or any clear medical condition. The presence of syndrome of inappropriate antidiuretic hormone (SIADH) was hence considered (see Figure 1A for trends). Her International Normalized Ratio (INR) was raised between 2014 and 2015 while on anticoagulation therapy for a PE and it is noted to have crossed the upper recommended threshold of three (Figure 1A).
Porphyria screening. In view of the patient’s multiple comorbidities (i.e., psychosis, chronic dermatitis, bilateral cornea thinning, and possible SIADH), screening tests for various types of porphyria that may present with such features were conducted. However, the results of these tests excluded this condition.
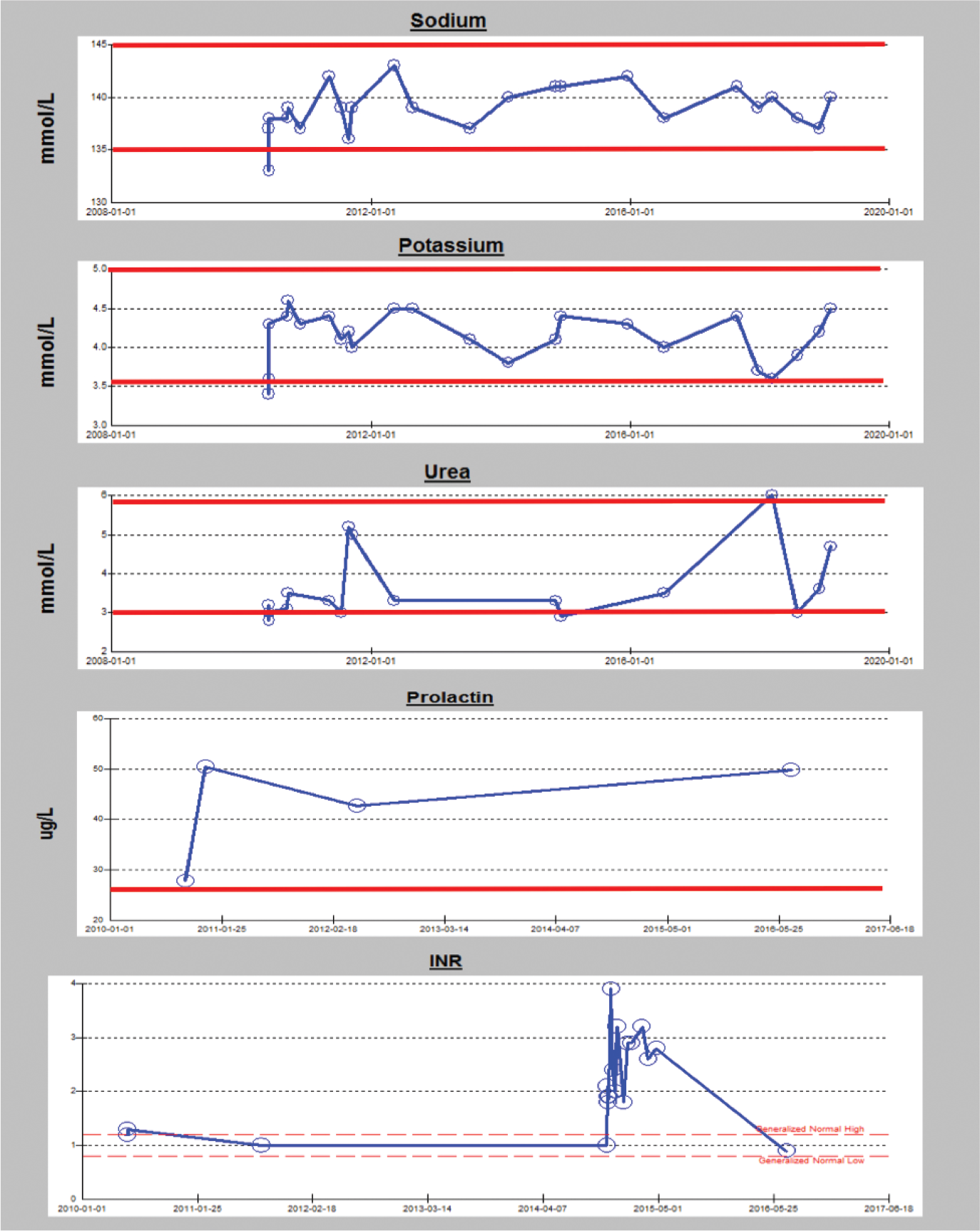
Trends for sodium, potassium, urea, prolactin and INR since 2010. The red lines demarcate the expected upper and lower reference values for sodium, potassium and urea and the upper limit of reference range for prolactin.
Autoimmune screen. The patient’s history of chronic dermatitis triggered testing for possible autoimmune conditions, which were all negative.
Diagnostic tests
Brain scans (CT & MRI). There was a focus of nonspecific increased T2/FLAIR signal within the left centrum ovale. The scan was otherwise unremarkable including no evidence of previous bleeds that may have been a consideration at the time of her raised INR (Figure 1-B).
Electroencephalograph (EEG) . Revealed dysrhythmia grade four independent bi-temporal spikes. On two separate occasions, EEG demonstrated possible interictal epileptic abnormality from the left and right (independently) temporal regions.
Double length deprived EEG. Recoding revealed sharply contoured waves in the temporal regions that were perceived as benign spikes, however, there were epileptic spikes on two occasions of the entire recording emanating from the temporal lobes (Figure 1C).
Neurological examination
Neurological examination of the patient was unremarkable other than demonstrating generalized reduced reflexes. The patient had no history of episodes that would suggest an overt seizure disorder or “attacks" that are reminiscent of focal aware seizures. There were no reports of episodes, where she awoke in the morning with features suggestive of a nocturnal convulsive event. However, she did have an episode, where she lost consciousness and her "eyes rolled up", but this was attributed by her neurologist to a protracted bout of coughing.
Further management
The patient remained symptomatic despite compliance with different antipsychotic medications which included depot medication to ensure adherence. Given her history and somewhat suspicious EEG results, divalproex sodium was trialed with gradual dose titration. Within one month of this, the patient reported a 50% reduction in the experience of seeing her spirit and that the “fogginess” that had constantly shrouded her mind was lifted to a similar degree. The phenomena of seeing her organs move in and out of her body were also reported to have diminished by 20% and her visual hallucinations were described as less vivid. The most pronounced impact reported by the patient after starting antiepileptic medication was the complete abolition of the distressing “thought bubbles” emanating from her head.
The remarkable improvement triggered further dose optimization of the divalproex sodium and discontinuation of her antipsychotic medication. Eight weeks later, the patient reported complete abolition of visual hallucinations and reduction of her somatic phenomena “of moving organs” by 80% according to her own account. This progress has been maintained for eight months to date since the initiation of treatment.
Discussion
The conundrum of this patient’s diagnosis and management could be summarized as follows: the rather unusual nature of her psychopathology that was difficult to treat; her extensive multisystem comorbidities were challenging to gather under a single syndrome; and her EEG recordings showed independent epileptic spikes on both temporal lobes despite having no history of a seizure disorder. While this may be viewed as an unusual constellation of symptoms, non-convulsive epileptic psychosis is a known phenomenon based on compelling evidence from intracranial SEEG studies [1]. Complex partial status epilepticus of temporal lobe origin may significantly alter mental states and present similar to functional/primary psychoses. The non-convulsive state may be associated with prolonged epileptic discharges on intracranial SEEG in hippocampal and other mesotemporal structures or may show no abnormality. These discharges can produce a myriad of complex psychotic states [2], paranoid schizophreniform psychosis [3], internal dialogue with voices, restlessness, anxiety, and fearful effect [4], Capgras syndrome [5], and paranoid/hallucinatory interictal psychosis [6].
Postictal psychosis was coined by Jackson [7] and is noted for its similarity to schizophrenia-like paranoid and affective psychoses. There is also convincing SEEG evidence that, for some cases at least, the psychosis is rather ictal due to ongoing limbic seizure activity and is a form of non-convulsive status epilepticus.
While interictal hallucinosis in epilepsy has been sparsely studied [6], its occurrence may be more common than appreciated. It remains contentious; however, as to what extent it represents subclinical epileptic discharges, i.e., auras [8]. More relevantly, the interictal psychosis of epilepsy is often indistinguishable from primary schizophrenia. It occurs more often in temporal lobe (limbic) epilepsy, in those with frequent seizures and in patients with enduring history of epilepsy. There are several mechanisms by which epilepsy may be associated with schizophrenia-like psychosis. It is likely that epilepsy sets up a neuronal network which results in psychotic symptoms. Chronic seizure discharges can result in structural brain abnormalities that may represent a common final pathway for psychosis [9,10].
It is questionable, whether this form of psychosis is directly ‘driven’ by subclinical electrographic activity or is an indirect consequence of related functional changes. An intriguing question is whether similar electrophysiological changes could underpin psychosis in the non-epilepsy population, but evidence on this is scarce [1].
An early clinical distinction between organic (epileptogenic) and functional (schizophrenic) psychosis is crucial as this will impact the treatment. In organic psychosis, patients may experience positive symptoms very similar to those of functional psychosis, including delusions or hallucinations. The main differences would be that patients with organic psychosis may present with fewer negative symptoms, better insight, and a more preserved and appropriate affect [3,11].
This reported case illustrates that subclinical/non-convulsive epilepsy can result in positive psychotic symptoms that are indistinguishable from those of primary psychosis. Interictal hallucinosis is probably more common than is appreciated in epilepsy; however, it is still unknown to what extent patients are misdiagnosed with functional psychosis when the etiology is actually organic in nature (i.e., subclinical epileptic discharges). Evidence from Silberman et al. [8] suggests that a kindling effect from chronic seizure discharges could alter an individual’s affective response to environmental stimuli.
Interictal psychosis could be an interesting focus of study as it can result in chronic psychosis with clear consciousness. This type of psychosis most commonly originates in the temporal lobe (limbic) region and is therefore more likely to occur when there are bilateral temporal discharges, similar to those reported in this patient.
Contentiously, if a schizophrenia-like state arises in patients with epilepsy as a result of neurophysiological changes secondary to chronic epileptogenic discharges [2,6,8,12], it would be interesting to speculate on whether functional psychosis might share a similar underlying pathophysiology. Similarities in positive symptoms between organic and functional psychosis are rather misleading. It is therefore imperative that physicians pay close attention to cases that may be missed due to inexact attribution of psychopathology to a functional (primary) condition when, in fact, it is organic in origin. This insight into diagnostic formulation would subsequently guide a different management strategy that would in turn improve the quality of care provided to patients similar to the reported case.
Despite the fact that the changes in this patient’s brain MRI were non-specific and her bi-temporal epileptic spikes on EEG were not diagnostically perceived as a seizure disorder, the patient’s unremitting psychopathology on a myriad of antipsychotics was suggestive of an atypical illness course. Furthermore, her remarkable improvement after initiation of antiepileptic medication and discontinuation of antipsychotics is probably the most conclusive evidence that her psychotic condition was organic rather than functional in nature.
Conclusion
We hope that by sharing this case study with the scientific community that our colleagues find it both intriguing and helpful when trying to differentiate their patients’ psychopathology at the interface between organic and functional conditions.
Finally, we would like to quote Wieser [13] when he wrote “Paralleled by clear cut time related epileptic discharges in hidden brain areas the phasic psychical disturbance of some patients would not have been accepted as an epileptic dysfunction without depth recordings. Such observations are perhaps first steps in building a long desired bridge to psychiatry, because it can hardly be denied that in innumerable patients with transient mental changes, the same might be true if they were explored with depth electrodes.”



