Background
Even minor trauma can cause bleeding. The presence of an underlying liver disease may itself be the cause of bleeding. Although rare [3%–15% of hepatocellular carcinomas (HCCs)], bleeding from a liver mass is an event that can lead to death [1]. The focused assessment with sonography in trauma (FAST) is an ultrasound protocol developed to assess for hemoperitoneum and hemopericardium. The FAST exam evaluates three potential spaces within the peritoneal cavity for pathologic fluid; however, the evaluation does not include an assessment of the presence of solid liver lesions [2].
The presence of a liver mass may not be known to the patient. It is important to investigate the possible presence of liver alterations that can cause bleeding, especially during mild trauma.
Case Presentation
We describe the case of a 42-year-old Chinese man admitted to the emergency for a minor road trauma. At first, no CT scan was performed due to the negative eco- FAST results, the mechanism of trauma and the patient hemodynamic stability; the patient was then discharged. One week later, he was readmitted to the Emergency Department for abdominal pain and signs of hemorrhagic shock. CT scan revealed the presence of a hepatic hematoma with a subcapsular hematoma and hemoperitoneum; there were no signs of active bleeding (interventional radiology involvement was not indicated) (Figure 1 A and B). The patient was hemodynamically stabilized. CT also detected the presence of a solid mass in the context of the hematoma of the right hepatic lobe associated with right portal vein thrombosis (PVT), probably HCC (Figure 1 C and D). The patient had no significant past medical history. A 24-hours control CT scan showed an increase in hemoperitoneum. After performing the indocyanine green clearance (PDR 17.9 and R15 6.8), the patient underwent a laparoscopic right liver hepatectomy combined with PVT removal.
Discussion
The hypothesis was “post-traumatic bleeding of HCC”, histologically confirmed (Figure 1 E and F). Bleeding from liver tumors is rare but it can be a life-threatening event [3,4]. Hematoma can make it difficult to diagnose HCC on CT examination [5]. Surgery may be necessary as first line treatment [6]. CT scan can be difficult to interpret precisely due to the presence of bleeding. There are CT signs that can help to suspect, if present, the presence of a liver mass such as a) the inhomogeneity of liver enhancement after administration of contrast media with wash-out areas in the venous phase (corresponding to focal lesion); b) the presence of “mass effect” (distortion of vascular architecture and liver profiles); c) vascular or biliary infiltration. The presence on non-contrast CT of spontaneously hyperdense material (due to bleeding) can hide the presence of the liver mass. Even the patient’s medical history (in this case recent trauma and lack of knowledge of hepatic mass) can be confusing. This case reminds us that we must not exclude the possibility of preexisting pathologies (such as the presence of an HCC) in the evaluation of trauma, even minor ones.
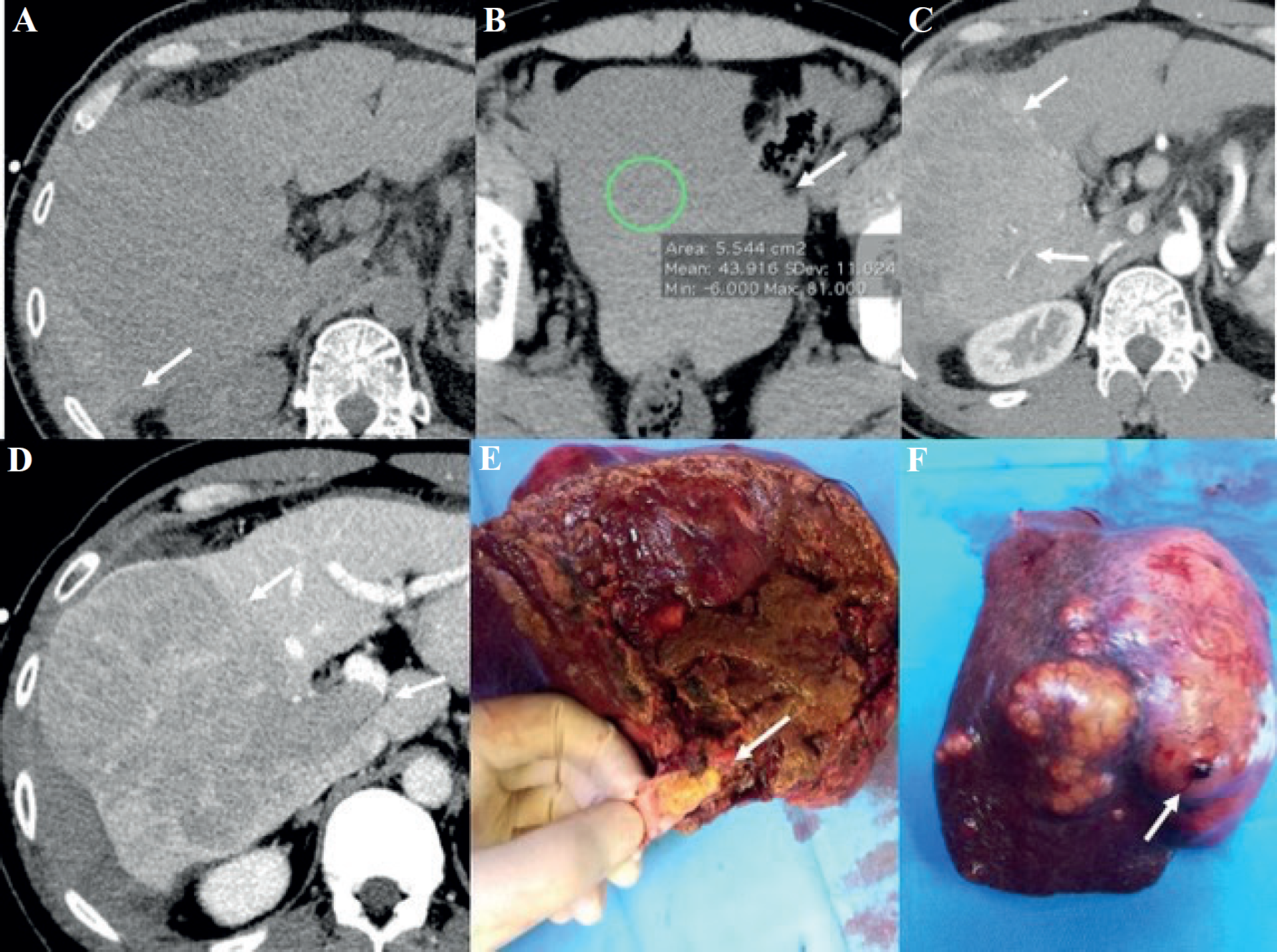
(A) The scans without contrast show a large inhomogeneous, hypodense, hepatic area (right lobe) associated with a subcapsular and perihepatic hyperdense layer (arrow) matching the hematoma; (B) presence of blood in the pelvis (arrow). (C) Post-contrast arterial phase- parenchyma and vessels enhancement (arrows) without signs of active bleeding. The arterial branches are small irregular ones likely to be compressed or infiltrated (D) The portal phase shows a large area of contrast wash-out not typical for hematoma, indicative of the presence of a mass (arrow). The right portal branch cannot be visualized (suspicion of portal vein thrombosis, arrow). (E) Surgical specimen of HCC demonstrates right portal infiltration (arrow), (F) and bleeding area (arrow).
Bleeding, which is not recognized promptly, can lead to patient’s death. The correct diagnosis that includes both the recognition of bleeding and the presence of the mass is essential to choose the correct treatment.
Conclusion
In case of a minor trauma, as in our case, in the absence of indicative symptoms the patient can be discharged. However pre-existing conditions (such as the presence of a liver mass, in this case unknown at the time of trauma) can complicate the course. It is essential in this case that the contrast CT examen can highlight both the bleeding and the presence of the liver mass. The characterization of the mass guides us in choosing the type of treatment (in this case surgical).
What is new?
Hemoperitoneum secondary to liver HCC rupture is a rare but potentially lethal condition. In our case the tumor was not known, and the bleeding was slow. It is important to recognize the typical characteristics of liver lesion presence to Imaging in order to quickly decide the treatment. Proper management of this condition remains the subject of some debates; in patients with a resectable tumor, surgery may be an option.

