Background
Mediastinal cysts are benign lesions and according to Takeda et al. represent 12%–18% or according to Gursoy et al. 20%–32% of all mediastinal masses [1,2]. Although cystic lesions surrounding the heart had been reported since 1854, according to the review of Lillie et al. [1], the first published pathoanatomic case series including 1 cyst was completed in 1903 [3].
Pleuropericardial cysts (PPCs) account for 5%–10% of mediastinal tumors and 11% or 30% of mediastinal cysts. They are usually congenital [4,5]. However, other causes have been reported, including inflammatory, traumatic, and other causes [6–9]. Even though all ages may be affected, PPCs are most often detected between the third and fifth decade of life. The most common site of occurrence is the right cardiophrenic angle (51%–75%), followed by the left (28%–38%). PPCs usually have a diameter 3–15 cm and weigh 100–200 g. Most of PPCs are asymptomatic (50%–75%), so they are found post-mortem or incidentally on routine chest X-ray (CXR). When they are symptomatic, the symptoms are generally dominated by respiratory signs, such as chest discomfort or dyspnea, circulatory signs, and signs of nervous compression. Moreover, although they have almost always-benign clinical course, they can occasionally lead to complications due to compression of adjacent organs or inflammatory or other complications. As far as diagnosis is concerned, after the initial detection, further imaging, including multi detector computed tomography, Magnet Resonance Imaging, and other methods are used complementarily to confirm the diagnosis mainly in difficult cases. Given that PPCs are usually asymptomatic, and it has not been reported to have malignant potential, the majority of them can be left without treatment. When management is required, surgical resection by means of traditional open surgery or minimally invasive methods is considered to be the gold standard and along with percutaneous aspiration are the methods that have been mostly performed [10].
We report below a peculiar case of a 37-year-old woman who referred to the Emergency Room (ER) because of suspected asthma exacerbation and computed tomography (CT) revealed a probably acquired large PPC of unknown cause.
Case Presentation
A 37-year-old Caucasian woman with medical history of focal epilepsy and asthma, referred to our ER because of suspected asthma exacerbation (palpitations and dyspnea). Clinical investigation was suspected of pneumonia. Biochemical tests revealed a slight increase of C-reactive protein and leucocytosis which raised the suspicion of infection. A CXR revealed an intermediate pneumonia (Figure 1a). A control radiograph 2 weeks later under Penicillin treatment revealed remaining findings, but the patient was asymptomatic (Figure 1b). A new CXR 2 months after the first demonstrated a slight progress of chest mass (Figure 1c). A contrast thoracic CT (Siemens SOMATOM Sensation 64 slice) with a 3 mm slice thickness, confirmed the presence of an anterior basal right-sided PPC sized 5.5 cm craniocaudally, 5 cm anteroposterior, and 6 cm laterally (Figure 2) without contrast agent assuming, pathologically enlarged lymph nodes and pleural effusion.
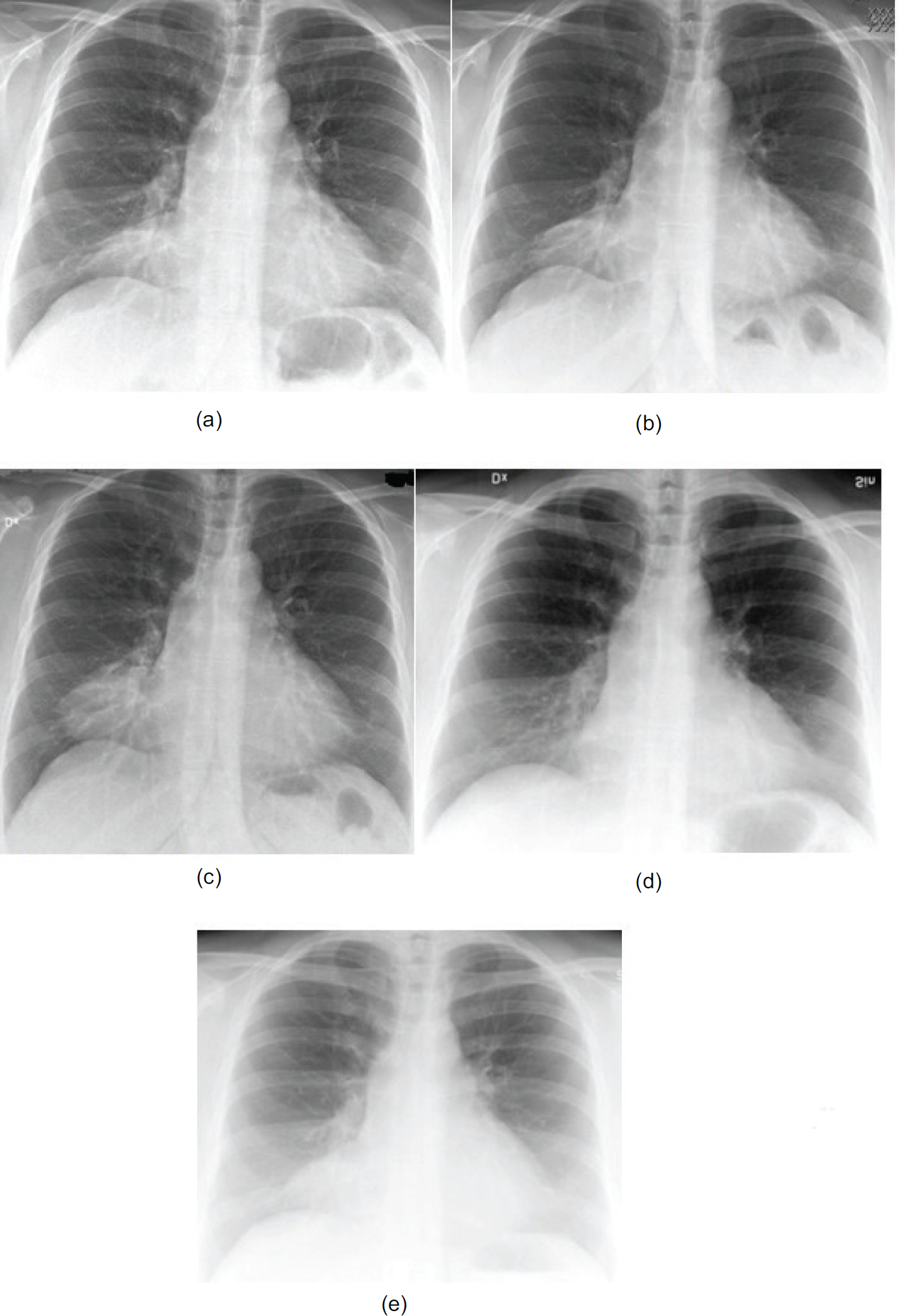
(a) First CXR. Intermediate pneumonia. (b) Control CXR 2 weeks after the first. Remaining findings while patient was asymptomatic under penicillin treatment. (c) Control CXR 2 months after the first. Slight progress of chest mass while patient was still asymptomatic. (d) Previous CXR in the last 8 years. (e) Previous CXR in the last 8 years.
According to the literature, on CT scan, the PPC is thin-walled, well-marginated, oval homogeneous mass, usually unilocular, while multilocular cysts have also been reported. Their attenuation is low (0–20 HU) although sometimes it may be a little higher than water density (30–40 HU). This is probably interpreted by a high protein and cells content due to bleeding or infection [10]. As they are commonly avascular, they don’t enhance with contrast agents. Abdominal CT and echocardiogram were performed and both were normal without pathological focal changes. The differential diagnostic approach was challenging. Radiological investigation combined with a normal laboratory control excluded pericardial or pleural effusion, aneurysms, fluid-filled superior aortic recess, varicose pericardial vein, lipoma, hydatic heart disease, germ cell tumors, diaphragmatic hump, mecechymal tumors, brochogenic carcinoma, and mediastinal abscess, as a possible diagnosis. After the examination of previous radiographies in the last 8 years, this cyst was not observed (Figure 1d and e). Therefore, this event constitutes a peculiar case of an asymptomatic probably acquired PPC with unknown cause according to patient's medical history. After consultation with lung specialists and thoracic surgeons, ultrasound-guided punctuation was recommended in the event of symptoms. Video-assisted thoracoscopic surgery could be a further choice of management in case of cyst's refill within a short period after punctuation. Eventually, no surgical intervention was performed, as the patient did not develop any cyst-associated symptoms, after a 5-year follow up.
Conclusion
PPCs are rare and usually clinically silent, but can occasionally cause life-threatening complications. The majority of them is congenital due to developmental deficits and is most commonly found incidentally via routine radiography between the third and fifth decade of life. The management of a PPC should be based on an algorithm taking into consideration cyst's size, shape, and compressibility as well as clinical presentation and patient’s fitness and preference. Surgical resection by means of traditional open surgery or minimally invasive methods is considered to be the gold standard and along with percutaneous aspiration are the methods that have been mostly performed. Finally, we reported an unusual case of possible infection which revealed an asymptomatic large PPC which was detected accidentally via CXR and was left untreated. Not having observed in earlier imaging studies this cyst is believed to be acquired, but the exact etiology has remained unknown as aspiration which could exclude inflammatory causes has not been required.
What is new?
To our knowledge, it is the first time that a pleuropericardial cyst reveals in an asymptomatic patient who is presented to emergency department with pneumonia. Patients’ infection-related symptoms disappeared after antibiotics, but the radiological investigation showed an unchanged huge pleuropericardial cyst.


