Introduction
Pulmonary blastomas are uncommon malignant tumors of the lung, accounting for only 0.25%–0.5% of all malignancies of the lung, and may be associated with the CTNNB1 mutation. Histopathologically, pulmonary blastomas have been subdivided into three distinct categories: biphasic pulmonary blastoma (BPB), well-differentiated fetal adenocarcinoma (WDFA), and pleuropulmonary blastoma. Typically, the WDFA and BPB are caused by the use of tobacco, with the average age of the patients at diagnosis ~ 43 years [1]. Albeit, a significant number (~40%) of the patients are clinically asymptomatic, the typical clinical features suggestive of pulmonary blastoma include respiratory distress or pneumothorax and pneumonia-like symptom (e.g., fever, cough, lethargy, opacity on chest radiograph, etc.) [2, 3]. The treatment of choice for pulmonary blastoma is surgery, while the role of chemotherapy and radiation therapy has not been well-established.
In this case report, we have presented a case of recurrent BPB whose management was carried out with surgery and multi-agent chemotherapy. Specifically, the patient remained disease-free for 3 years after complete tumor resection at the initial diagnosis. Afterward, the recurrent disease was treated with chemotherapy (ifosfamide, carboplatin, and etoposide).
Case Report
A 26-year-old female presented to us with major complaints of respiratory distress, cough, dyspnea, and wheezing for the past few months. The patient’s radiological workup revealed a mass in the left lower lobe of the right lung. Specifically, contrast-enhanced computerized tomography (CE-CT) of the thoracic region illustrated well-circumscribed mass lesion (size ~ 6 cm) in the lateral basal segment of the lower lobe of right lung, as depicted in Figure 1. The lesion expressed soft tissue component with patchy marginal calcification and was indicative of hydatid. The patient underwent lobectomy for the left lower lobe of the right lung.
Histopathology of the excised pulmonary tissue revealed a neoplastic lesion having a biphasic pattern of growth and well-differentiated malignant tubular glands in a cellular stroma. The stroma also showed undifferentiated small oval/spindle cells with few immature mesenchymal components and much mitosis. The glands were lined up by columnar epithelium and showed many subnuclear and supranuclear cytoplasmic vacuoles imparting a fetal lung-type appearance. Immunohistochemical staining was positive for Creatine Kinase (CK) and Periodic Acid -Schiff (PAS), while negative for Periodic Acid-Schiff with diastase (PASD) and Mucin, as shown in Figure 3. These findings were consistent with biphasic pulmonary blastoma. Post-surgical CE-CT study of chest and abdomen showed no residual mass. Moreover, no parenchymal infiltration and nodal or visceral metastasis were visualized. The patient was kept on close follow-up, without any oncological intervention. The patient remained disease-free for 3 years. It may be of interest that the patient was being pregnant during this period and normally delivered the baby.
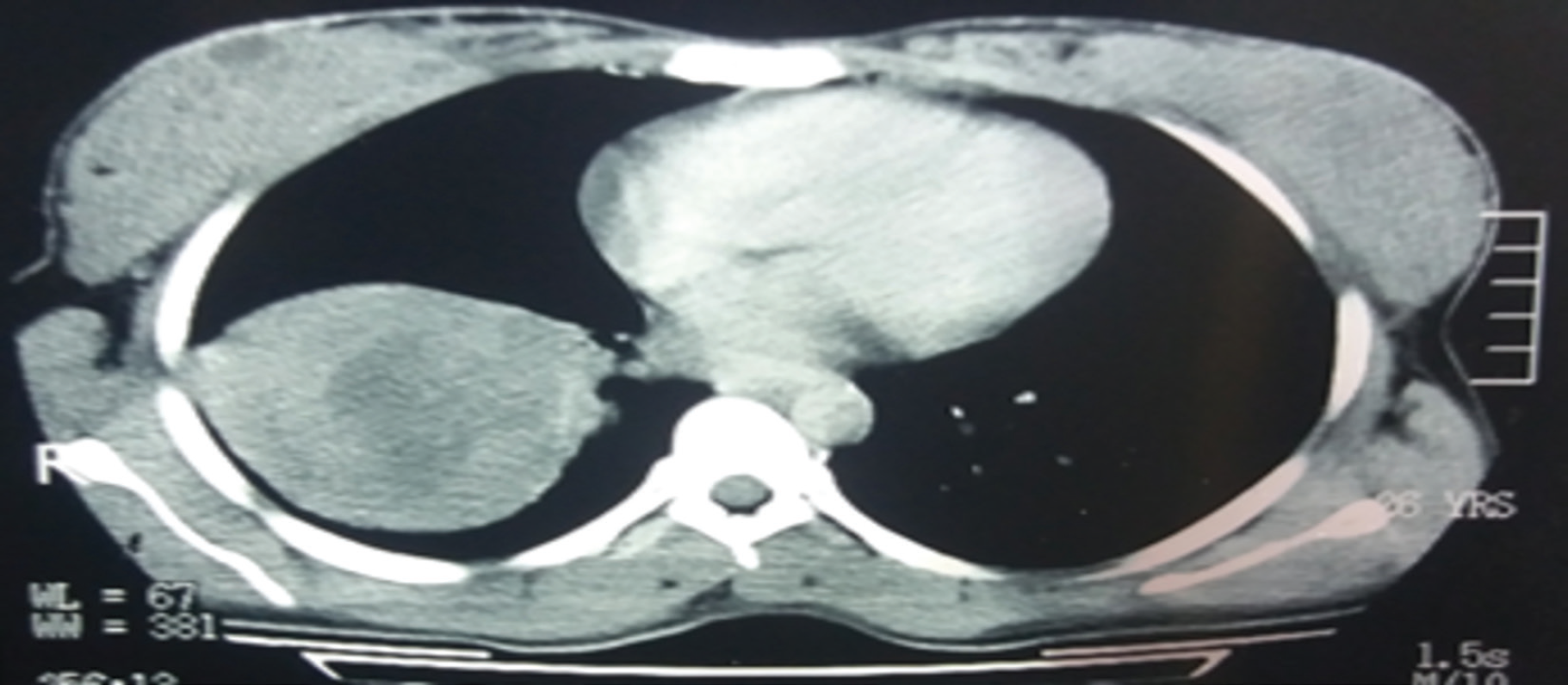
Initial CT image of the patient illustrating well-circumscribed mass lesion (size ~ 6 cm) in the lateral basal segment of the lower lobe of right lung.
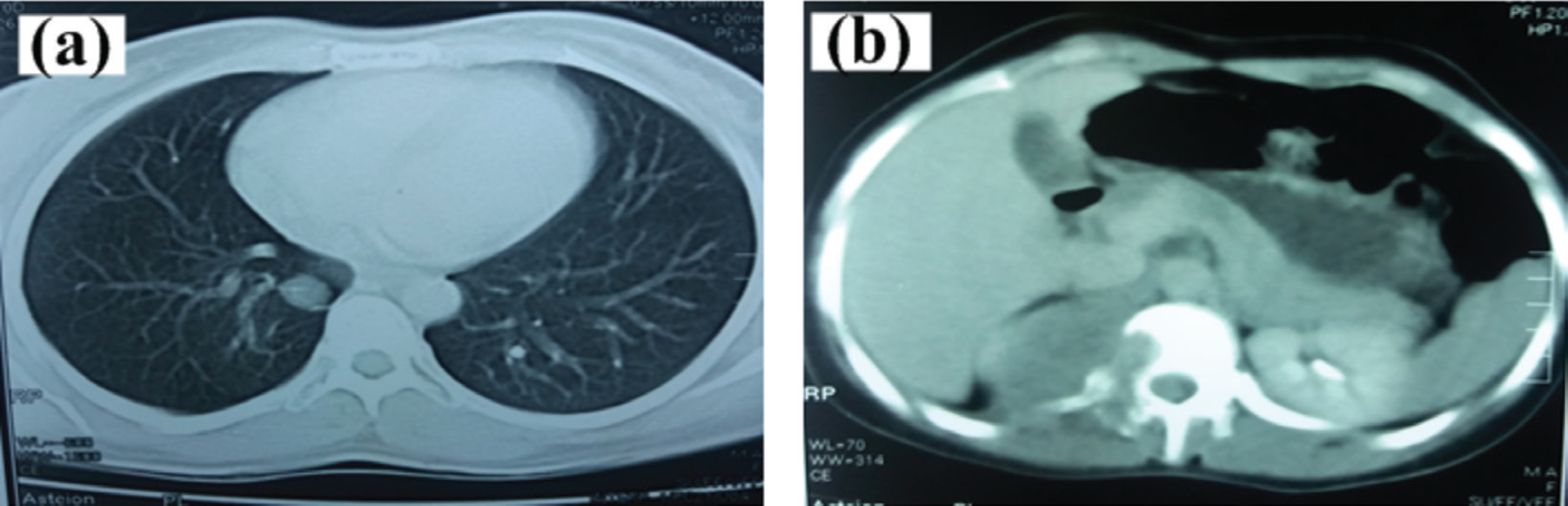
Follow-up (3 years) CT image of the patient illustrating a) an oval nodule (size ~ 1.4 × 1.2 cm) in the medial segment of right lung and b) a mass lesion (size ~ 5.5 × 3.8 cm) in the right renal region, which involved the right-side pedicle and transverse process of adjacent vertebra.
After 3 years of the initial diagnosis, the patient presented with recurrent disease. Specifically, the CE-CT study of chest, abdomen, and pelvis demonstrated an oval nodule (size ~ 1.4 ×1.2 cm) as shown in Figure 2 in the medial segment of the right lung (Figure 4). Furthermore, there was a mass lesion (size ~ 5.5 ×3.8 cm) in the right renal region, which involved the right-side pedicle and the transverse process of the adjacent vertebra. Trucut biopsy of the adrenal mass was performed. Histopathology of the excised adrenal tissue revealed well-differentiated malignant tubular glands lined by columnar epithelium with cytoplasmic vacuoles. Immunohistochemical staining was positive for CK and PAS, while negative for CK7, Paired Box (PAX)8, CK20, and PASD. These findings were consistent with recurrent/metastatic pulmonary blastoma. Magnetic resonance (MR) imaging (after 2 months without any intervention) showed a large lobulated abnormal signal intensity lesion involving the right T12-Lumber Vertebrae (LV)1 and LV2 vertebral levels (Figure 5). The lesion was extending into the spinal canal through the neural foramina, causing compression and displacement of the conus medularis of the left side. Vertebral bodies and right para-spinal muscles were also involved. Bone scintigraphy illustrated lytic lesion involving T12 and L1 regions.
The oncological management of the patient was carried out with multi-agent chemotherapy. Specifically, ICE (ifosfamide 1,800 g/m2 on days 1–4, carboplatin 450 mg/m2 on day 2, and etoposide 120 mg/m2 on days 1–3) was administered. After three courses of the aforementioned chemotherapy, reassessment of the patient showed disease progression. Specifically, the CE-CT study of chest, abdomen, and pelvis demonstrated a mass lesion in the right renal gland and adjacent D11 and D12 vertebral bodies. However, no pulmonary alveolar or nodular shadows were seen (Figure 5).
Discussion
BPB is a very rare malignant neoplasm of lung parenchyma presenting in adulthood. The primary, and most effective, intervention for BPB is the complete surgical resection of the lesion. Frequently, BPB appears as large tumors, with their largest average diameter of more than 10 cm, which sometimes confounds the margin-free tumor resection [4]. Alternatively, neoadjuvant chemotherapy may be considered to reduce the tumor size to the point where complete tumor removal becomes possible. Our patient underwent complete tumor resection at diagnosis and remained disease-free for 3 years.
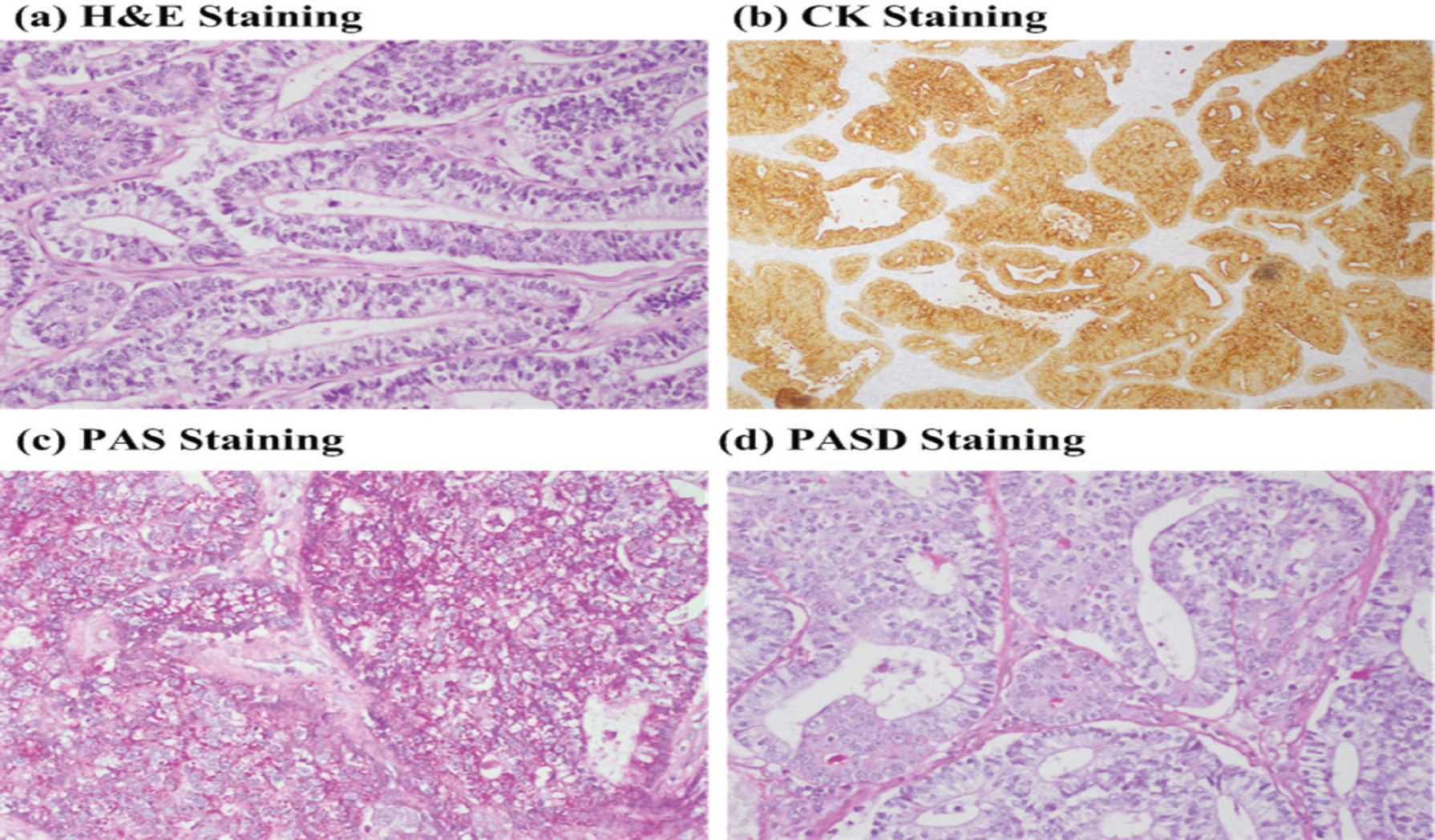
Illustrative histopathology and IHC images. a) H&E staining (40×), b) CK staining, c) PAS staining, and d) PASD staining.
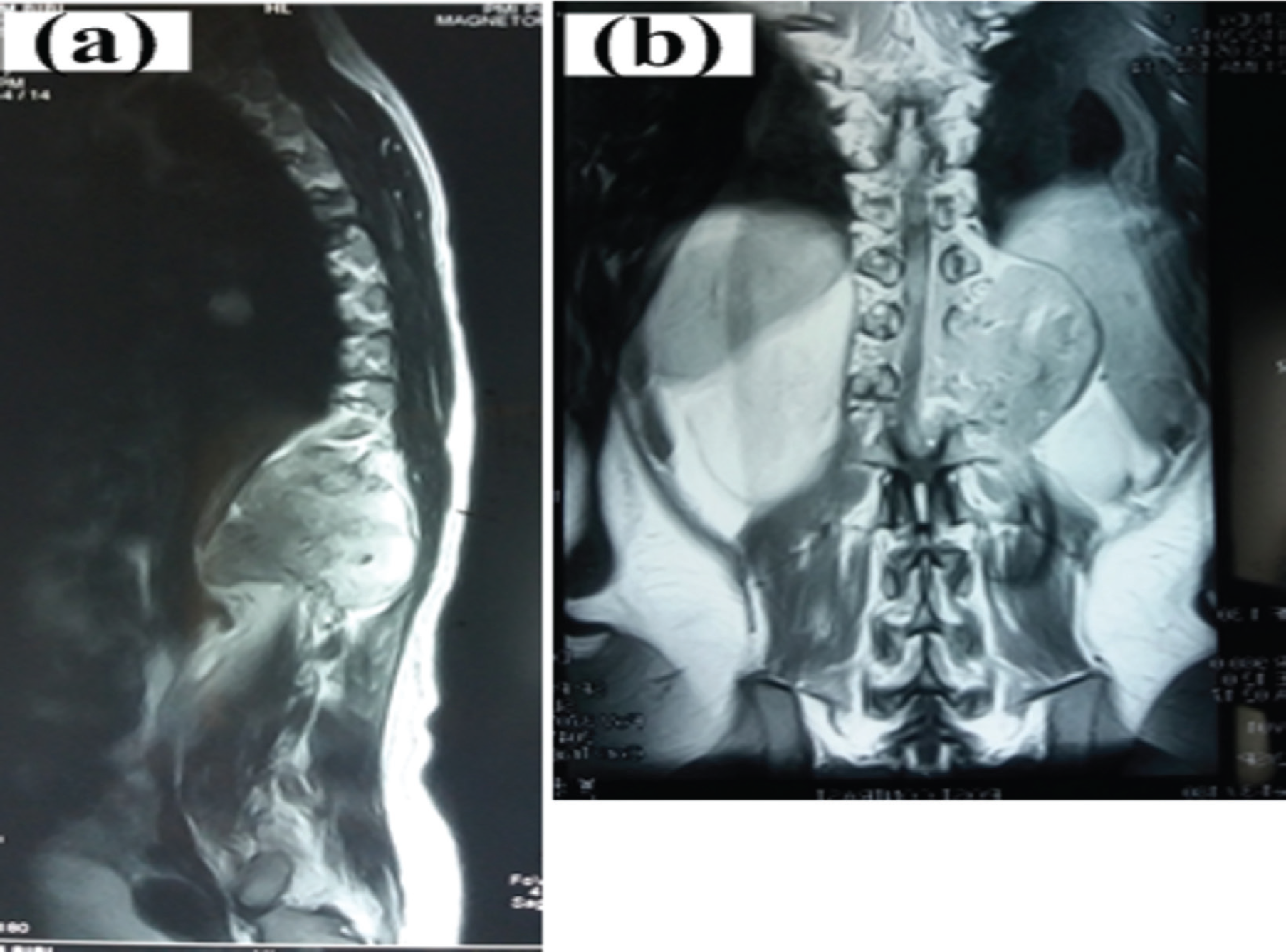
MR images illustrating large lobulated abnormal signal intensity lesion involving the right T12-LV1 and LV2 vertebral levels.
Multi-agent chemotherapy, including VA, IVA, VAIA, CEV/AIE, ICE/VAC, and IVAD (where I = ifosfamide, C = carboplatin, E = etoposide, V = vincristine, A = actinomycin-D, C = cyclophosphamide, and D = doxorubicin) has been previously administered [5]–[8]. We used the ICE regimen (ifosfamide 1,800 g/m2 on days 1–4, carboplatin 450 mg/m2 on day 2, and etoposide 120 mg/m2 on days 1–3); however, the disease responded poorly. Moreover, the role of radiation therapy in the management of BPB has not been fully established, particularly with the curative intend.
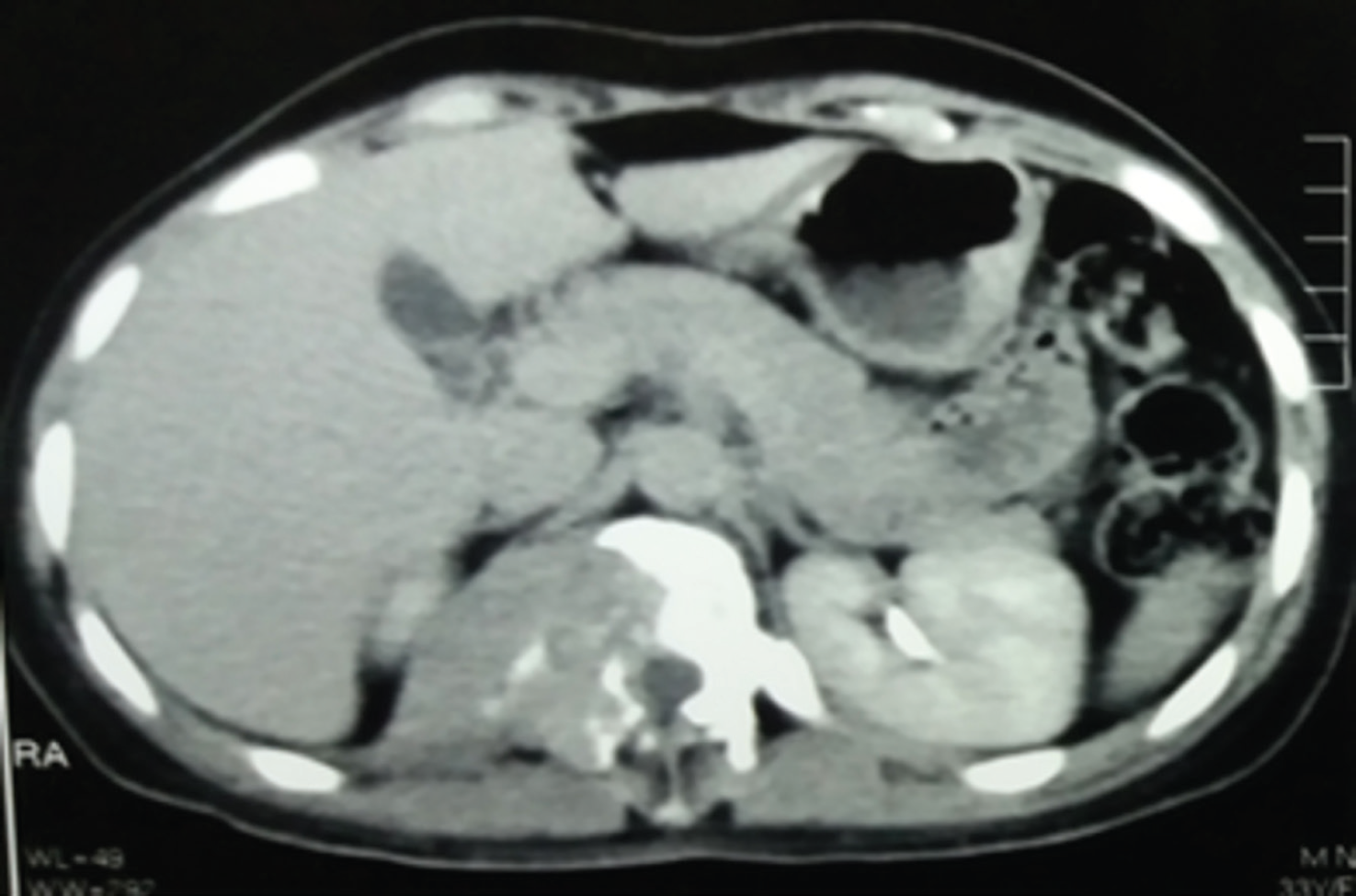
Follow-up CT image of the patient after three cycles of chemotherapy (i.e., ICE), illustrating a mass lesion in the right renal gland and adjacent vertebrae.
Understanding the cohort of prognostic factors for rare tumors such as BPB is one of the great challenges in their effective management. Nevertheless, the prognosis of BPB is very poor; Adverse prognostic factors for pulmonary blastoma are the biphasic type, tumor recurrence, metastasis at initial presentation, the large size of the tumor (>5 cm), and lymph node metastasis [1,3]. Moreover, BPB has a tendency for metastasizing to the pleura, diaphragm, brain, liver, mediastinum, heart, and soft tissues of the extremities and a recurrence rate of 43% [4,6]. In our patient, the disease metastasized to the renal region. Moreover, it has been reported that the recurrence seems to occur during the first 12 months; however, our patient remained disease-free for 3 years.
Conclusion
In this study, we presented a case report of recurrent biphasic pulmonary blastoma in a young patient. Our case demonstrated that complete surgical resection remains an effective intervention in biphasic pulmonary blastoma patients. Albeit chemotherapy has been advocated, it offered limited prognosis benefit to the biphasic pulmonary blastoma patients. This case report illustrates that biphasic pulmonary blastoma is a rear but aggressive malignancy.

