Background
Carotid body tumors (CBTs) are the carotid body paragangliomas which are highly vascular. There is a great need for careful diagnosis and surgical management due to their morphological character. Scudder performed the first successful surgery in 1903 in the United States [1]. These tumors required complete removal, but Harrington et al. in 1941 mentioned that 50% of this tumor shows histological malignancy [2]. Now, the studies have been conducted establishing the more benign clinical course without any distant metastasis. LeCompte had advised against surgical management because of the morbidity and mortality.
Case Presentation
A 48-year-old female reported to the otolaryngology outpatient department with a palpable swelling on the right side of the neck (Figure1).
This was not causing any pain, but there was a slight increase in the size for the past 1 year. There were no associated complaints of dysphagia, headache, ear discharge, or visual disturbances. There was no history of any trauma. The swelling was noticed on local examination and measured almost 2.0 cm × 1.5 cm. It was mobile side to side but not up and down. It was soft firm palpable swelling without any pulsation. Systemic examination was normal. Biochemical screening for plasma metanephrine and urinary catecholamines was normal. Other biochemical evaluation was within normal limits. The patient underwent plain X-ray Neck Anteroposterior and lateral projection which was normal (Figure 2a and b).
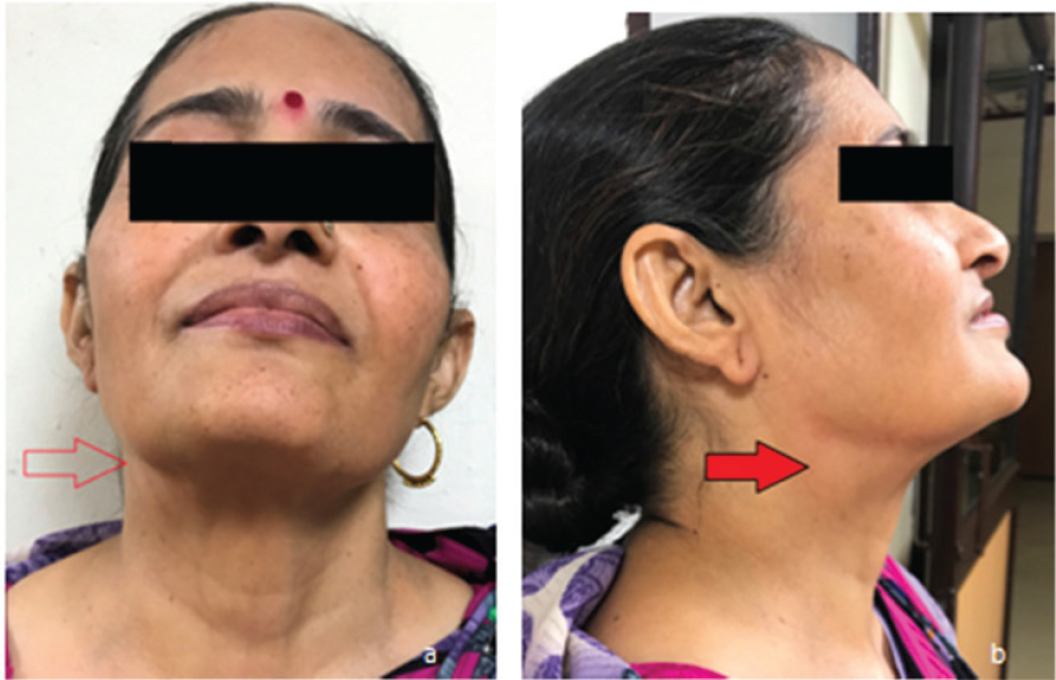
Photograph of the 48-year-old female patient. (a) Front view shows slight fullness on the right side of the neck in submandibular region (red hollow arrow). (b) Oblique view shows the fullness at the site of swelling (horizontal red arrow).
Ultrasonography (USG) evaluation revealed an almost well-defined hypoechoic mass at the region of the bifurcation of the common carotid artery on the right side (Figure 3). Color flow imaging (CFI) revealed that the mass was splaying the external carotid artery (ECA) and internal carotid artery (ICA). The mass had internal vascularity. No calcification was seen (Figure 4).
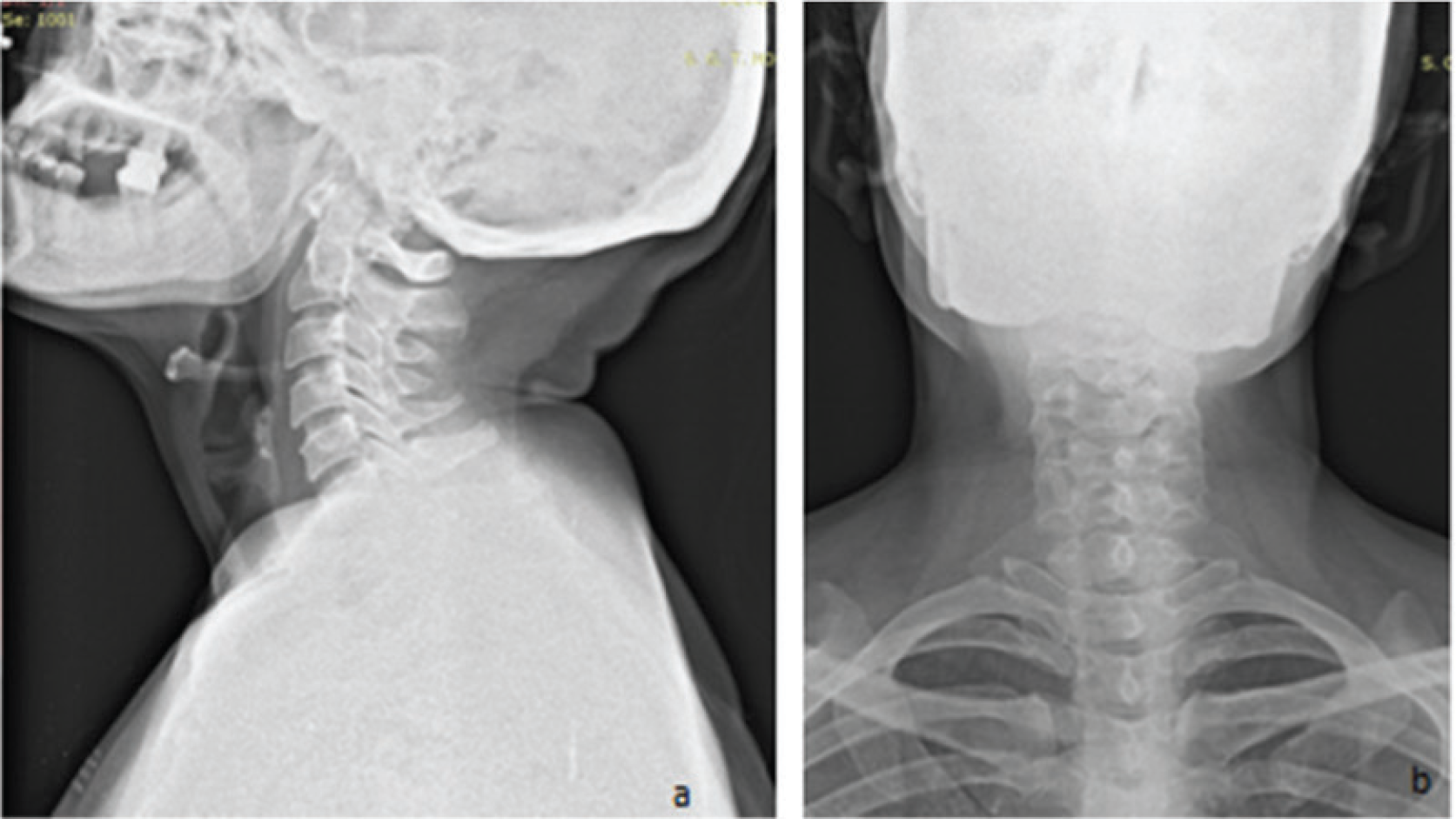
Plain radiograph of the neck region (a) lateral projection and (b) anteroposterior view. No abnormality was detected.
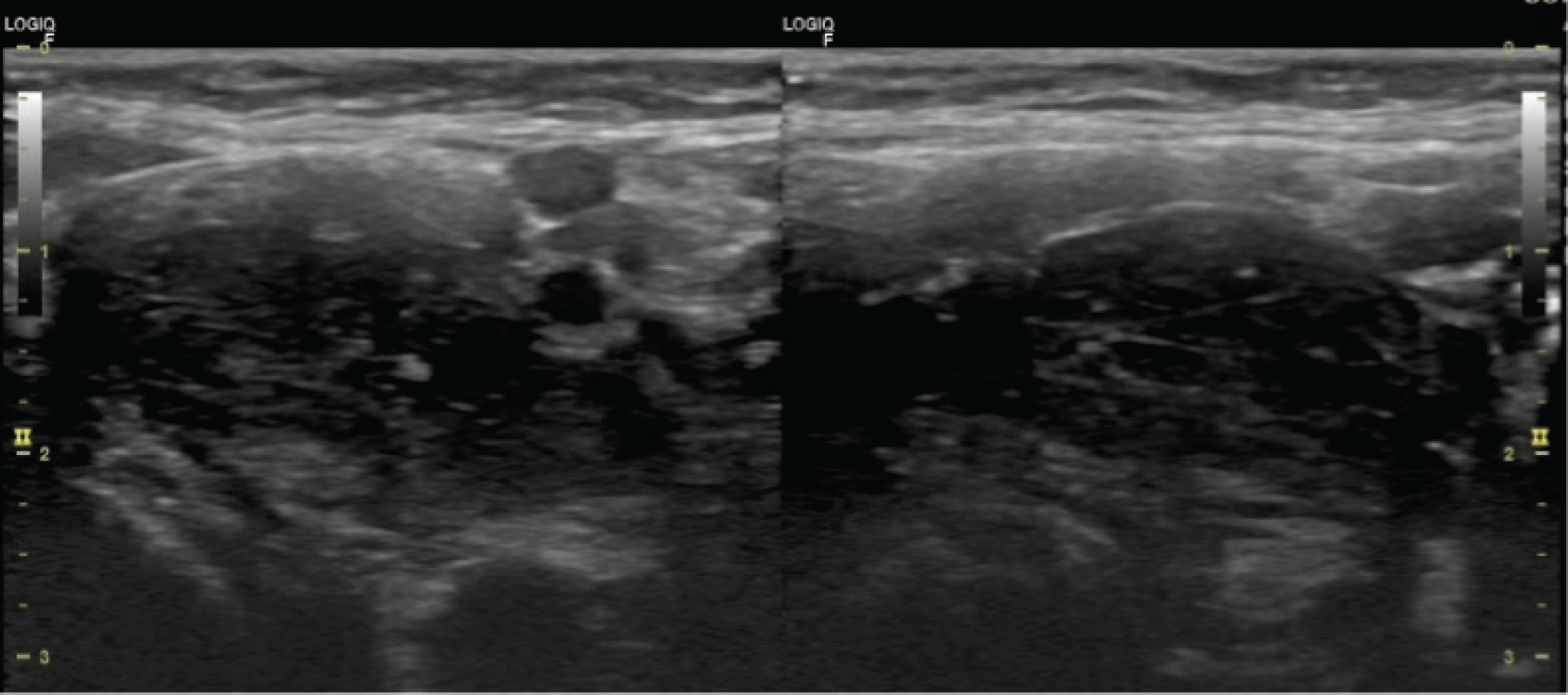
USG evaluation of carotid body tumor seen in gray scale in the long axis and short axis.The mass is more elongated rather than short axis.Tumor is well defined and slightly hypoechoic. No calcification or necrotic areas were seen.
Contrast-enhanced computerized tomography (CECT) evaluation revealed a well-defined avid by enhancing mass at the bifurcation. This mass was lying on the medial side of the bifurcation. Some branches of the ECA were seen feeding this mass. The mass was covering around 250° of the circumference.of ICA. This was categorized as type II as per Shamblin classification (Figures 5a and b and 6a and b).
Magnetic Resonance Imaging evaluation was done subsequently using the standard protocol along with magnetic resonance angiography (MRA). This revealed a classical “salt pepper” appearance of the mass in T1W. This is because of slow flow punctate foci (salt) and flow void dots (pepper). The mass was slightly hyperintense on T2W as compared to muscles, and there was no restriction in Diffusion Weighted Imaging. MRA shows “lyre sign” as splaying of the ICA and ECA. This can also be seen in source axial images (Figure 7a and b).
After ruling out other differentials such as schwannoma, neurofibroma, lymph node mass, or glomus vagale tumor pathologies, the working diagnosis was made as carotid body tumor of Shamblin type II. The diagnosis was straightforward on the basis of clinical and radiological evaluation. Now, the patient was advised a planned surgical management and kept under 6-month follow-up.
Discussion
CBTs are paragangliomas of the carotid bodies occuring at the bifurcation of common carotid in to ECA and ICA. These are also called as chemodectomas [2–4]. These cervical paragangliomas arise in close relation to the extracranial arterial system and cranial nerves. These tumors arise in adventitia which lies in the carotid sheath. The origin is from neural crest, so these are responsible for the adaptation of carbon dioxide, pH, and oxygen in the body [5,6]. These tumors are bilateral in about 5% of the cases. The mechanism is by releasing neurotransmitters which increase the ventilation after their stimulation. These tumors splay both the ECA and ICA. They are benign and asymptomatic in nature. They represent 65% of the cervical region paragangliomas. They can be either familial, sporadic, or hyperplastic as per their subsets in origin. The sporadic variety constitutes the majority of tumors to the tune of 85% and is found in the age group of 40–70 years. The malignant variety in these subsets occurs in 20–40 years age group [7,8]. The hyperplastic variety is found among those where hypoxia is the underlying factor such as high altitude, chronic obstructive pulmonary disease, or congenital heart disease. The surgical management of these types of tumor involves a lot of complications. The main complication is intraoperative bleeding. USG in combination with CFI depicts the reason well about the status of the vascularity and the origin of CBTs. CECT shows the evidence of vascularity in the form of avid enhancement and displacement of the main vessels [8]. The surgical Shamblin classification of CBTs (Figure 8a and b) is good predictor for the preoperative bleeding and morbidity. This is as per the size and extent of tumor. A preoperative MRA Shamblin classification [9] is as follows:
Type I: circumferential contact 180° or less.
Type II: circumferential contact between 180° and 270°.
Type III: circumferential contact > 270°.
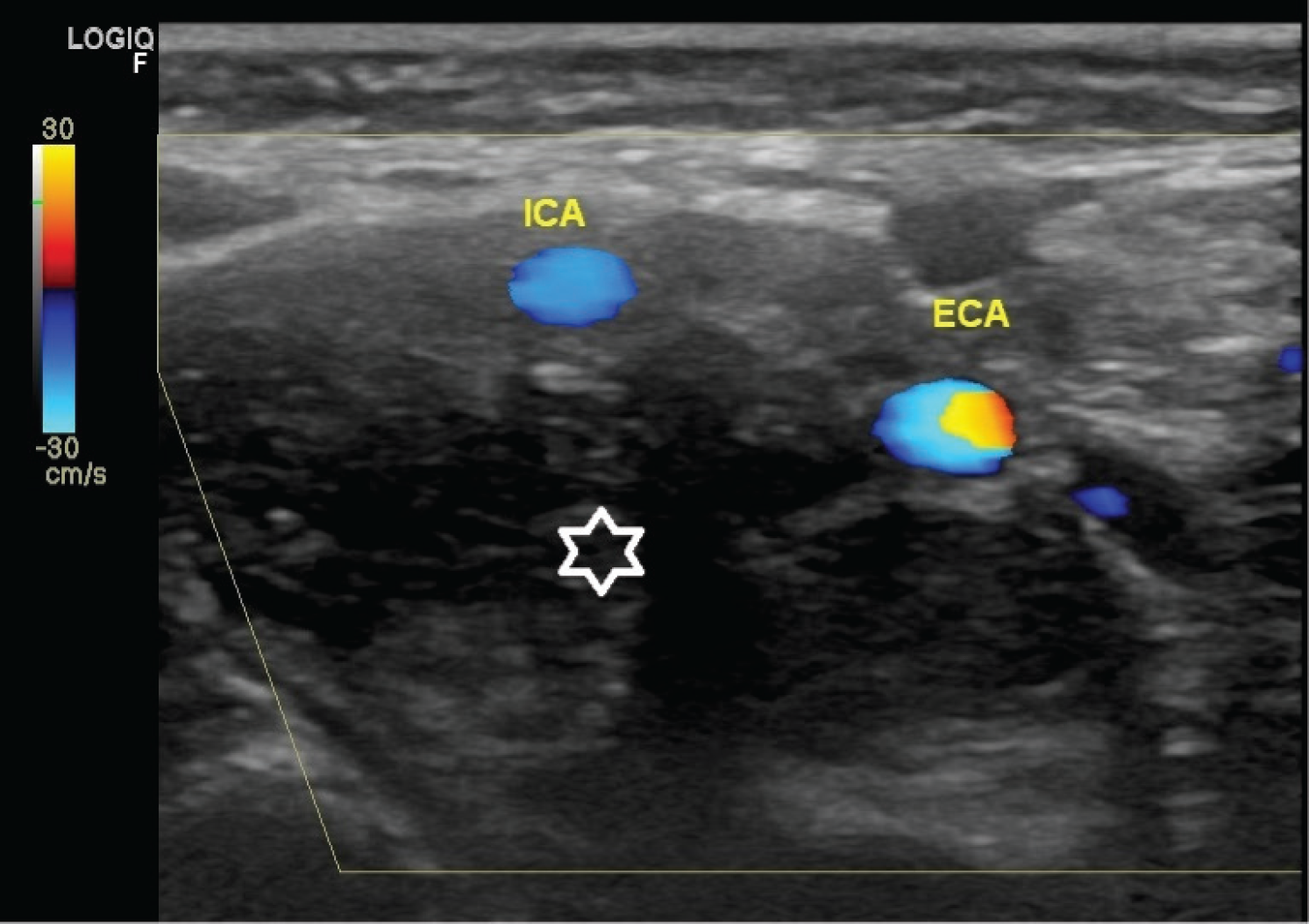
CFI of CBT.The hypoechoic mass (white star) is splaying the ICA and ECA.The velocity of ECA can be recognized by the color spectrum.
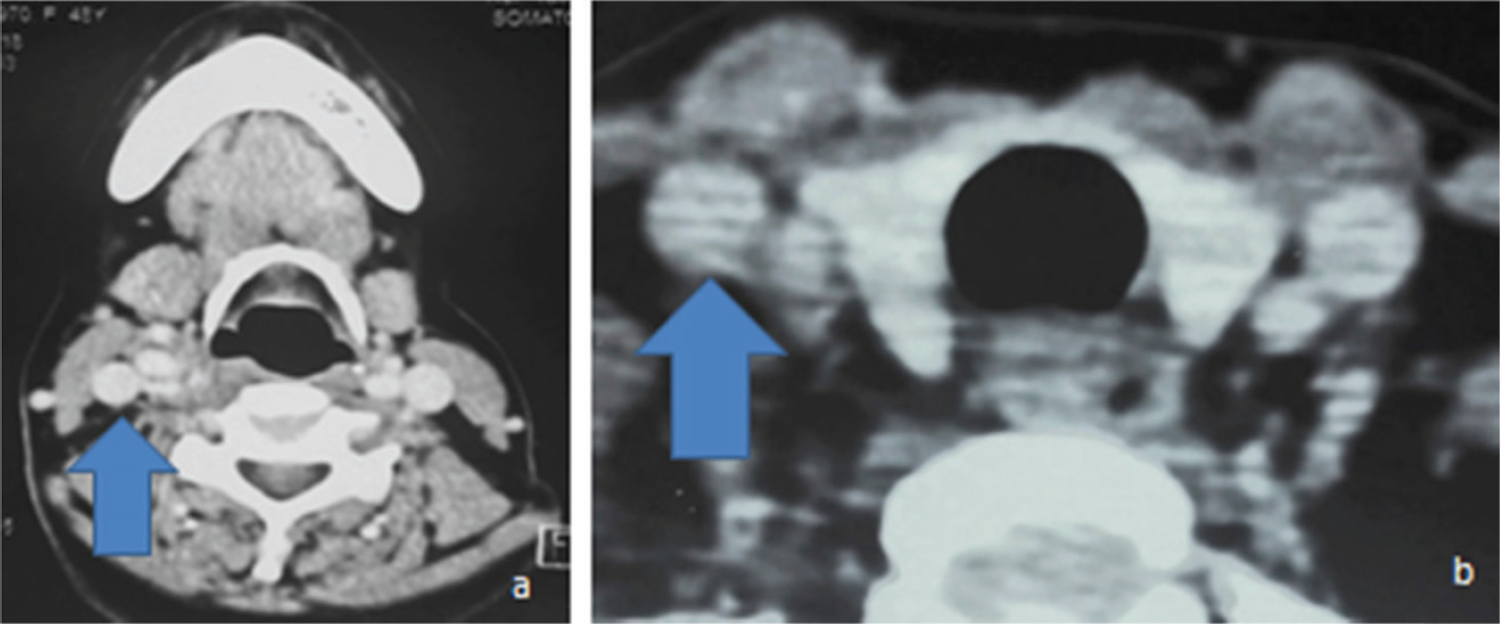
CECT axial section at various levels. (a) Right common carotid artery is seen normal at hyoid bone level (upward arrow). (b) Right CCA is normal at thyroid level (upward arrow).
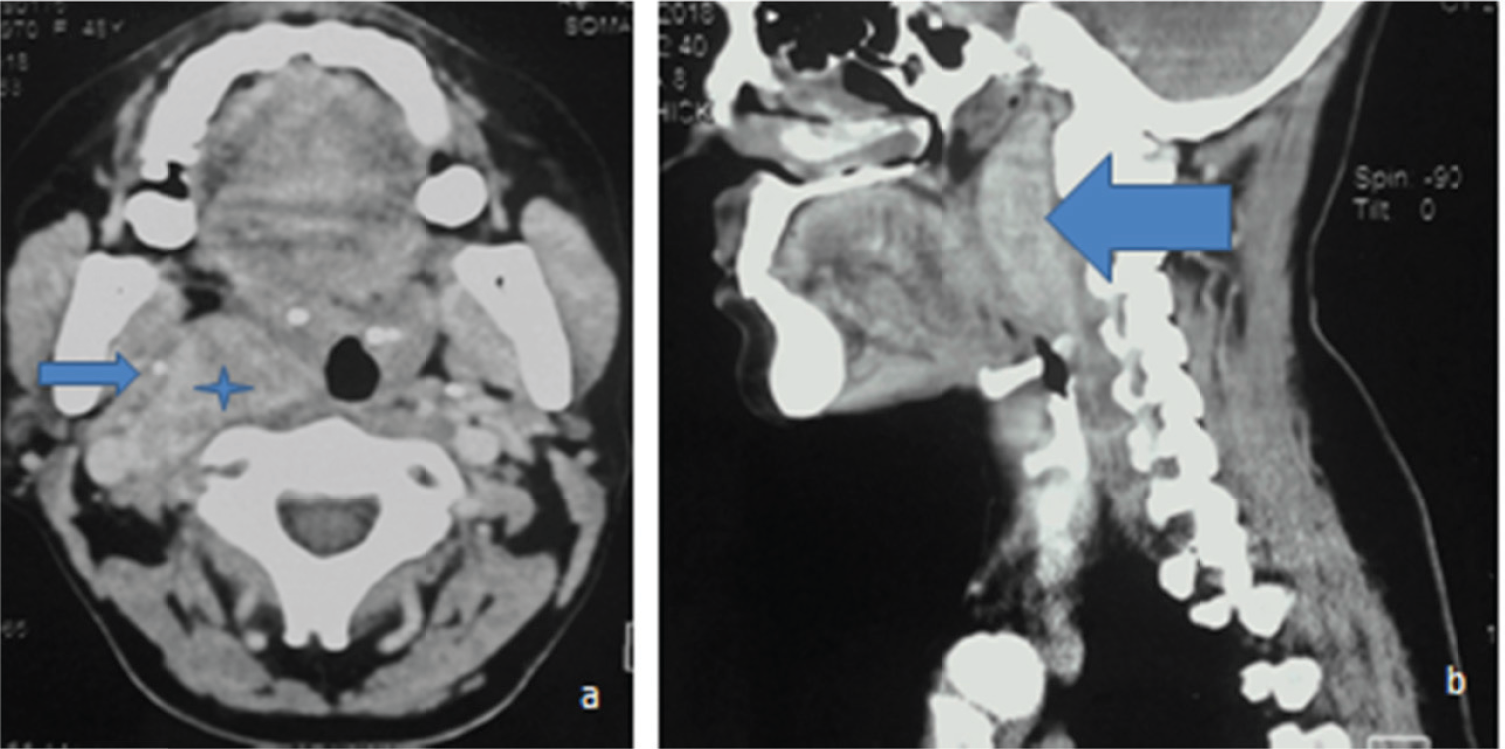
CECT neck region. (a) Axial section shows the avid-enhancing CBT (blue star) displacing the right ICA (blue horizontal arrow). (b) Reconstructed sagittal format showing the enhancing mass growing in superoinferior direction (blue horizontal arrow).
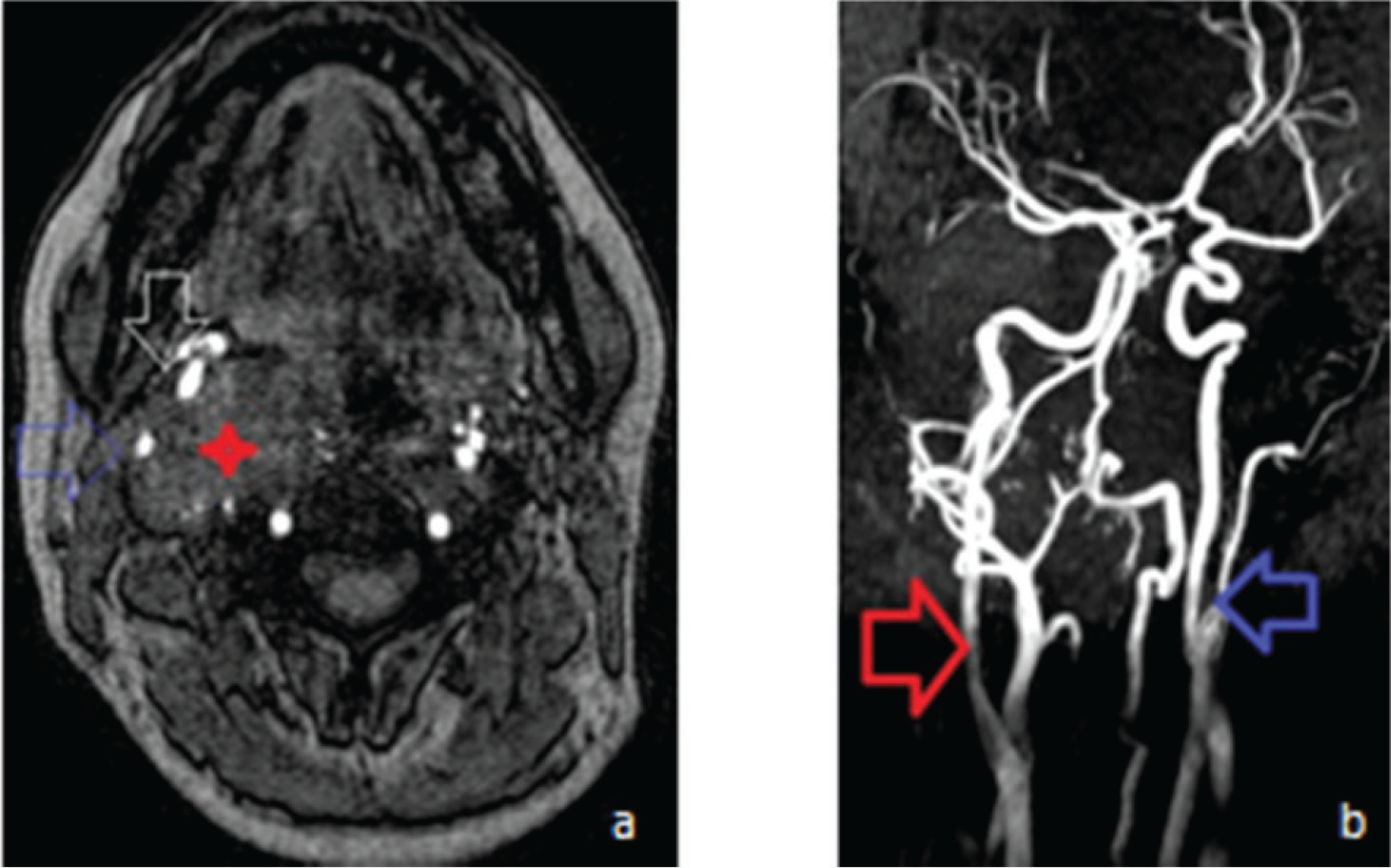
Magnetic resonance imaging evaluation. (a) Source axial section shows the CBT mass on the right side (red arrow) displacing ICA(blue hollow faint arrow) and ECA (inverted white hollow arrow). (b) MRA shows the splaying of ICA and ECA at the bifurcation of right CCA as “lyre sign” (red arrow) and the normal CCA bifurcation on the left side (blue arrow).
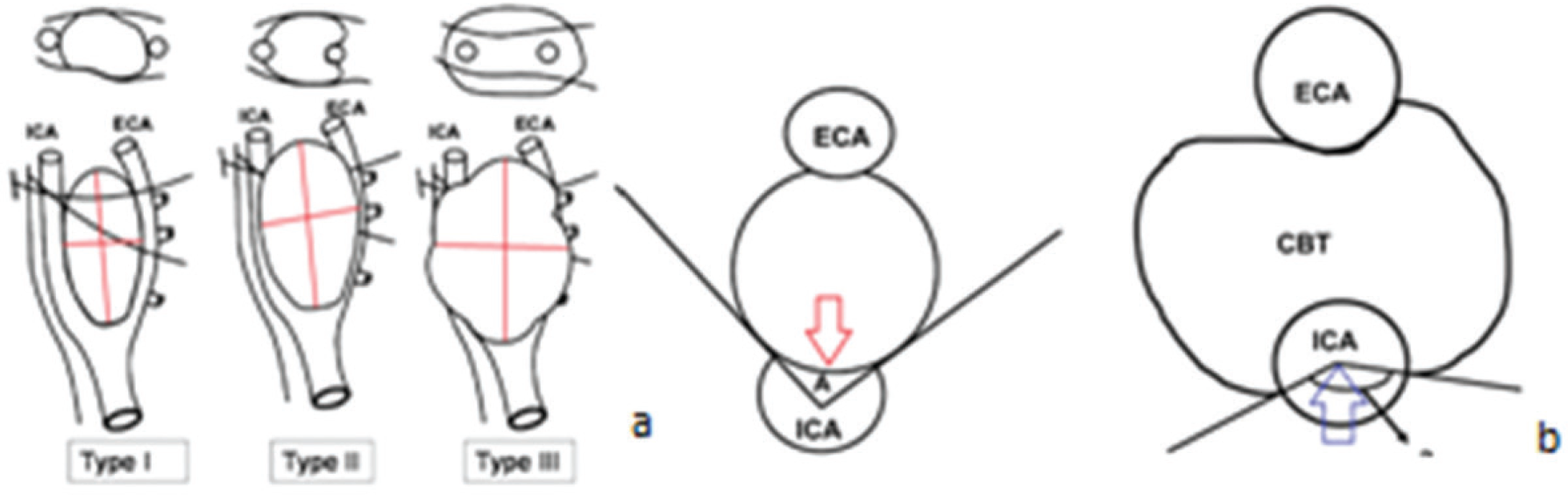
Diagrammatic representation of CBT as per Shamblin classification. (a) Mass splaying of ICA and ECA (red cross lines) as seen in angiography as per various types. (b) As seen in cross-sectional CECT images as per circumference.Type I is up to 180° (inverted red arrow) and Types II and III are between 180° onward (upward blue arrow).
An imaging evaluation shows a classical hypervascular, hypoechoic tumor mass with splaying of carotid bifurcation. The management warrants the multidisciplinary approach involving interventional radiologist and the surgeon [10]. Shamblin III group definitely requires preoperative embolization [11,12]. This leads to the safe and effective management of these notorious tumors. Conventional digital subtraction angiography shows a typical blush and early filling of vein because of arteriovenous shunting. The main nerves involved during the surgical intervention are vagus, hypoglossal, sympathetic chain, or marginal mandibular branch of the facial nerve. The literature accounts for 11%–50% of such injuries [13–15]. Preoperative embolization can prevent 75% of the blood loss, and this is usually done in ascending pharyngeal branch of the ECA [16]. Radiological evaluation always leads to the maximum safety of such surgical interventions and can be the best predictor for the complications [17].
Conclusion
The management of CBTs is a very controversial issue as the procedure is not free of complications. Intraoperative bleeding during the surgery is the most challenging issue. As these are benign tumors, the decision of surgical management should be as per the weight age of the advantages. Preoperative embolization is the most effective step to avoid blood loss during the surgery.

