Background
Jaffe put osteoid osteoma lesion in a separate category in 1935 [1]. This is constituted by central nidus rich in osteoid tissue with variable amount of calcification. There is normal sclerotic bone tissue in the surrounding region. This can either be at solitary or multiple locations in different bones.
Case presentation
15-years old boy reported to the pediatric outpatient department with complaints of backache since two months duration. This pain was severe at night and used to get relieved with analgesics. Then the intensity of pain increased and the patient reported to the hospital accordingly. There was no history of trauma or any other systemic disease. He was of averagely built physique. All the biochemical parameters were within normal limits. Systemic examination was unremarkable. Plain lumbo-sacral and abdomen skiagram were normal (Figure 1).
The boy was subjected to cross-sectional imaging. Magnetic resonance imaging study was performed which revealed subtle signal intensity changes in sacral region in T1W, T2W and STIR images (Figure 2 and 3). There was post gadolinium enhancement of the lesion (Figure 4).
NCCT of lumbosacral region was performed with the consent of the patient. This revealed a radiolucent focus with central radiodense nidus which measured 0.9 × 0.9 cm (Figure 5a, b and c). The working diagnosis of osteoid osteoma was kept in consideration. Later, the patient underwent radio-nuclear study which confirmed the diagnosis. This had shown increased uptake of the lesion region (Figure 6a and b). The child had been put on symptomatic treatment with future plan for the radiofrequency ablation. Three months follow-up had been advised before deciding about any RF ablation or surgical intervention.
Plain pelvis skiagram including sacral region antero-posterior view. There is no evidence of any lesion or pathology seen in the sacral region.
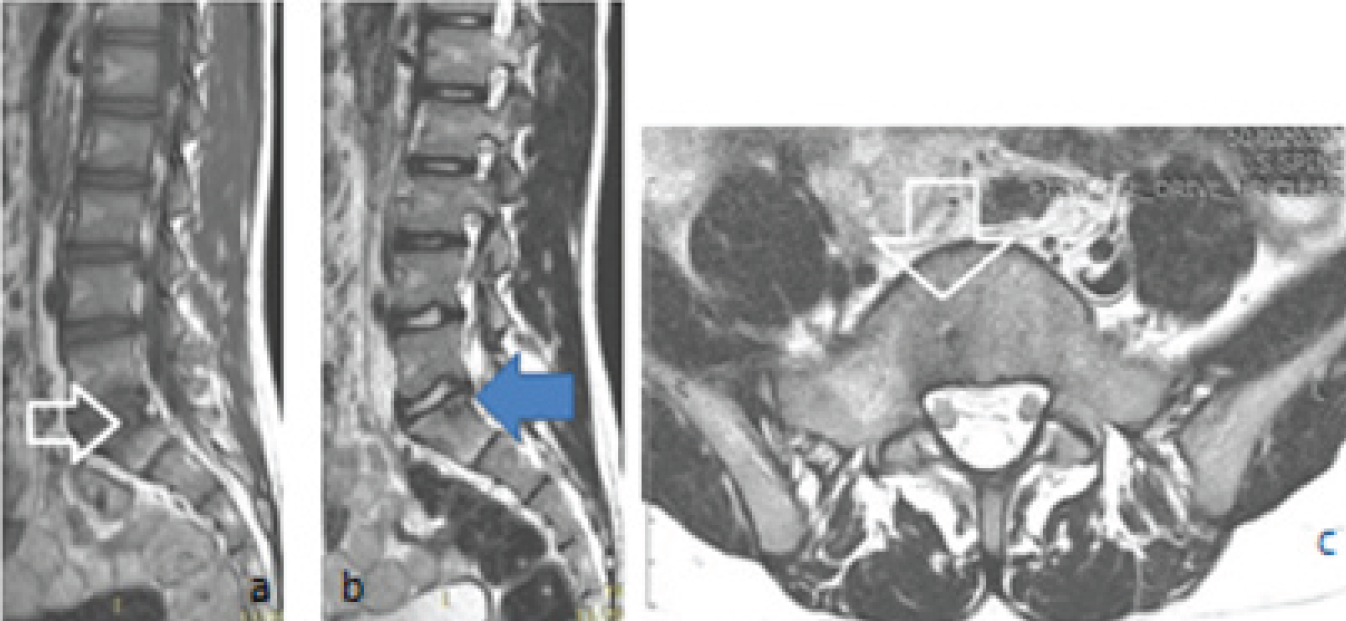
Magnetic resonance images, (a) T1W sagittal section shows a slightly low intensity region in the body of S1 sacral vertebra (white hollow arrow), (b) T2W sagittal section reveals mixed intensity lesion at the same location (blue horizontal arrow), (c) T2W axial section shows round hypointense lesion with surrounding hyperintensity (white hollow arrow).
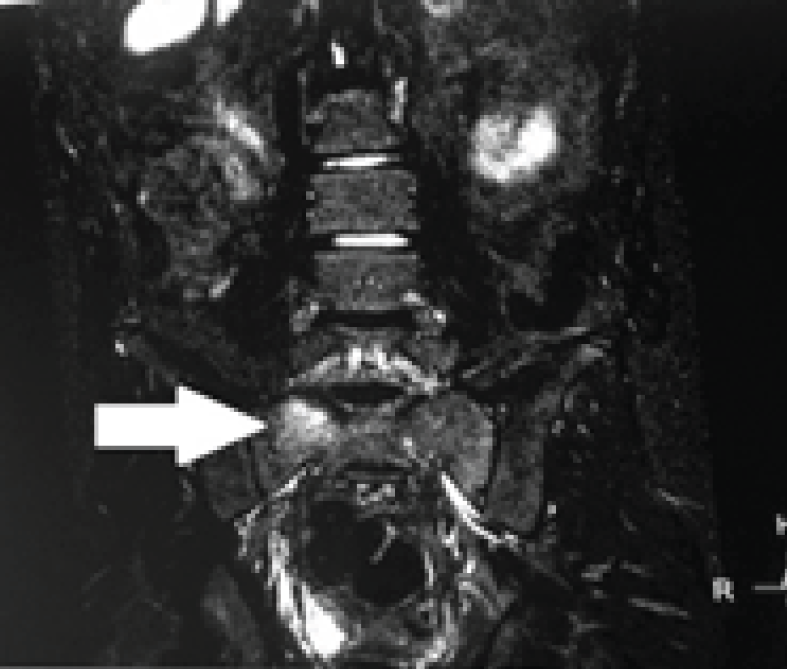
STIR magnetic resonance image show subtle hyperintensity in the body of S1 sacral vertebra suggestive of edema (solid white arrow).
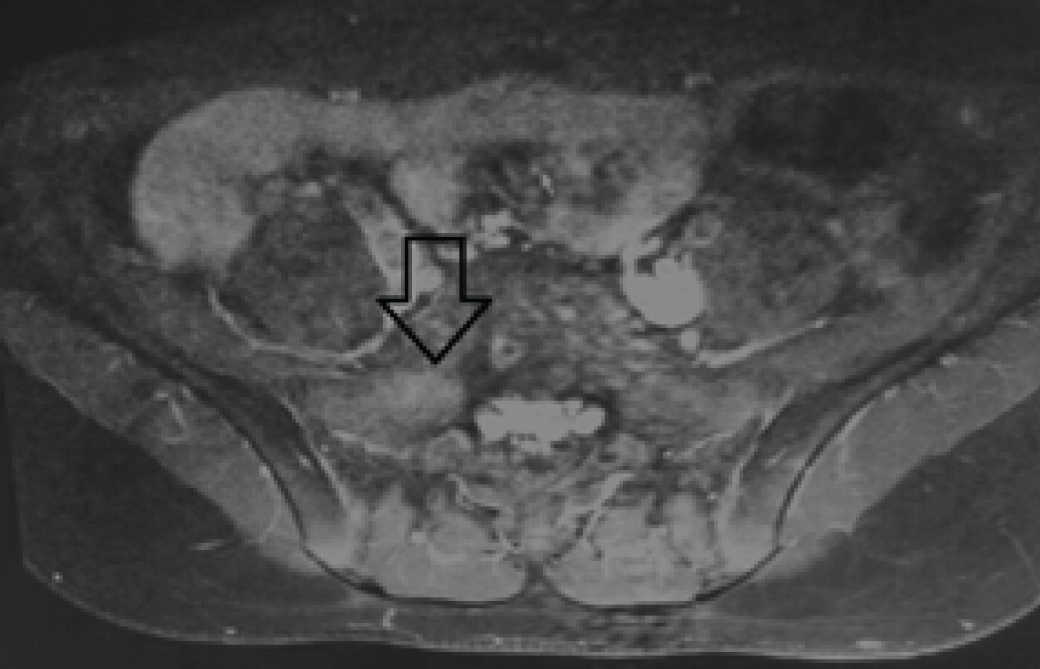
Contrast enhanced T1W fat saturated image. There is enhancement seen on the right side of the body of S1 vertebra (black vertical hollow arrow). The region corresponds to the location of the osteoid osteoma.
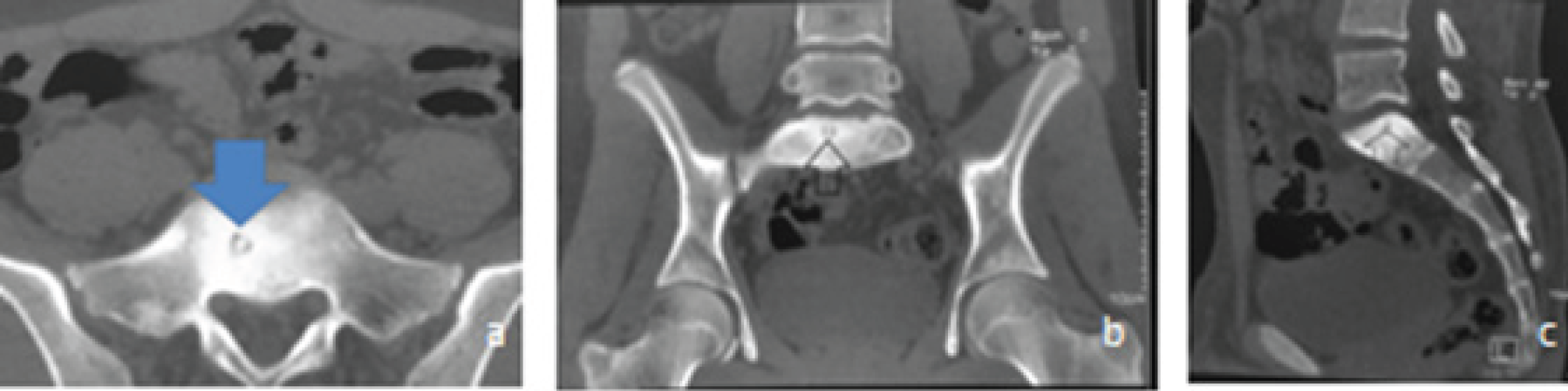
NCCT of pelvis and sacral region, (a) axial section shows small hypodense lesion with hyperdense central nidus (blue vertical arrow), (b) Coronal reformatted image shows the same lesion in the body of S1 vertebra (black hollow vertical arrow), (c) Sagittal reformatted image shows S1 vertebral hyper density (vertical hollow black arrow).

Nuclear scan for the bones, (a) axial sections (vertical white arrow) and sagittal section (horizontal white arrow) shows the increased early uptake of the tracer in the S1 vertebral lesion, (b) whole body scan shows the increased abnormal uptake at the sacral region (white horizontal arrow).
Discussion
Osteoid osteomas are benign bony lesions with osteoblastic activity. Though these can occur in any age group but 10-30 years is the most common group. Barei et al have noticed that the majority of osteoid osteomas occur below 20 years of age [2]. Lower extremities are the most common for their occurrence. Femur is the most common bone affected and cortical region of the long bones is the common most site.80-90% cases occur in the shafts of long bones and rest in other different locations. 7-20% have been observed in the spinal region. 78% of the cases in the lumbar region have been associated with scoliosis [3,4]. Following is the predilection for the occurrence in the spine as per the region involved:
Well at al have shown that in the majority of the cases there is a predilection for the posterior elements and the vertebral body is rarely involved [5]. Male are affected more than females and ratio is 2-3:1. Our case was male and falls in the younger age group. He had shown the involvement of the first sacral vertebral body which is slightly unusual site. The entity requires to be differentiated from eosinophilic granulomas, Brodie abscess and other cystic bone pathologies. Radiographically, these lesions may not be picked up at the first time because of their atypical complaints and presentations. Plain x-ray and NCCT scan delineate the central nidus with surrounding sclerotic zone. Bone scan confirms the diagnosis by early radiotracer uptake and delayed accumulation. This differentiates it from many other similar types of pathologies. Atar et al have divided this entity into two stages as acutely painful which is early and recovery stage which is later [6]. The second stage, in fact, corresponds to the healing because of ossification of the nidus. The management of these lesions in childhood is a challenge for the clinicians. There are various treatment options for the entity and radiofrequency ablation remains the choice in selected cases with the appropriate setting [7]. The lesion should not be near to the thecal sac and there should be enough cortical bone in the surrounding region. Air in the region can be of benefit being non-conduction of heat.
Conclusion
Backache in children is slightly uncommon feature. When the child is investigated for unexplained backache than the possibility for the search of other differentials must be kept in mind. There can be atypical presentation of osteoid osteomas at some uncommon sites. There may be a small navigating clue which can lead to the diagnosis. These are usually diagnosed through cross sectional imaging like MRI and NCCT. The management depends on the location, size and the symptoms of the patient.

