Introduction
Shin splints injuries occur in 13-17% of all the sport injuries and slightly more in aerobic dancers. Sine splints is described as pain on the inner aspect of the shin as per American Academy of Orthopedic Surgeons. Drez in 1980 used the term medial tibial stress syndrome first time. These are predominantly found in athletes but the incidence is not uncommon in dancers and those performing aerobics and military training [1]. Biomechanical factors have been attributed to that. The muscle like gastrocnemus, soleus and flexor digitorum longus are closely adhered to shin of tibia. The stress of these muscles leads to these types of injuries. The region of tibial shaft affected had been shown in the diagrammatic representation (Figure 1).
Case Presentation
A 22 year old male reported to the outpatient department with the complaints of slight pain on the shin of left leg. The pain was mild one year back and now the intensity has slightly increased. There was no history of obvious trauma, fever or any surgical intervention. On examination, the boy is well built and is an athlete in his college team. He frequently practiced as a long distance runner. Systemic examination was unremarkable except slight tenderness on the distal two third of shin of the left leg. There was no discoloration or injury mark on the left leg. One leg hop test was negative. All the biochemical parameters were normal. Plain X-ray of left leg had revealed a subtle increase in cortical thickness in the middle part of tibia. No fracture was seen (Figure 2).
Patient was subjected to non-contrast computerized tomography of the left leg to find out any other pathology. There was no additional finding except the increased cortical thickness in the lower part of tibia (Figure 3a and b).
Patient had undergone magnetic resonance imaging. There was marrow edema seen in T1W, T2W and STIR sequences. Periosteal edema was seen in T2W and post contrast fat suppressed T1W sequences in the form of crescentric enhancement (Figure 4a,b,c and 5a,b,c).
On the basis of all the findings and clinical examination the patient was diagnosed as that of medial tibial stress syndrome. As per Fredericson grading it was placed in Type III as the marrow edema is visible in both T1W and T2W sequences. Patient had been advised conservative treatment with follow up after three weeks.
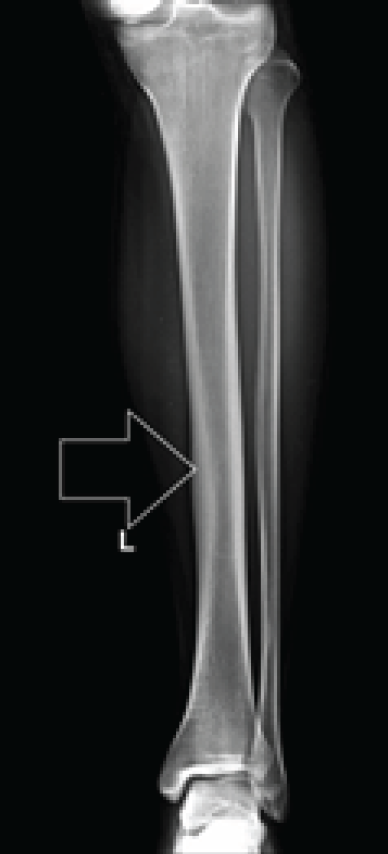
Plain X-ray anteroposterior view of left leg. There is subtle increase in cortical thickness on the medial aspect of the tibial shaft.
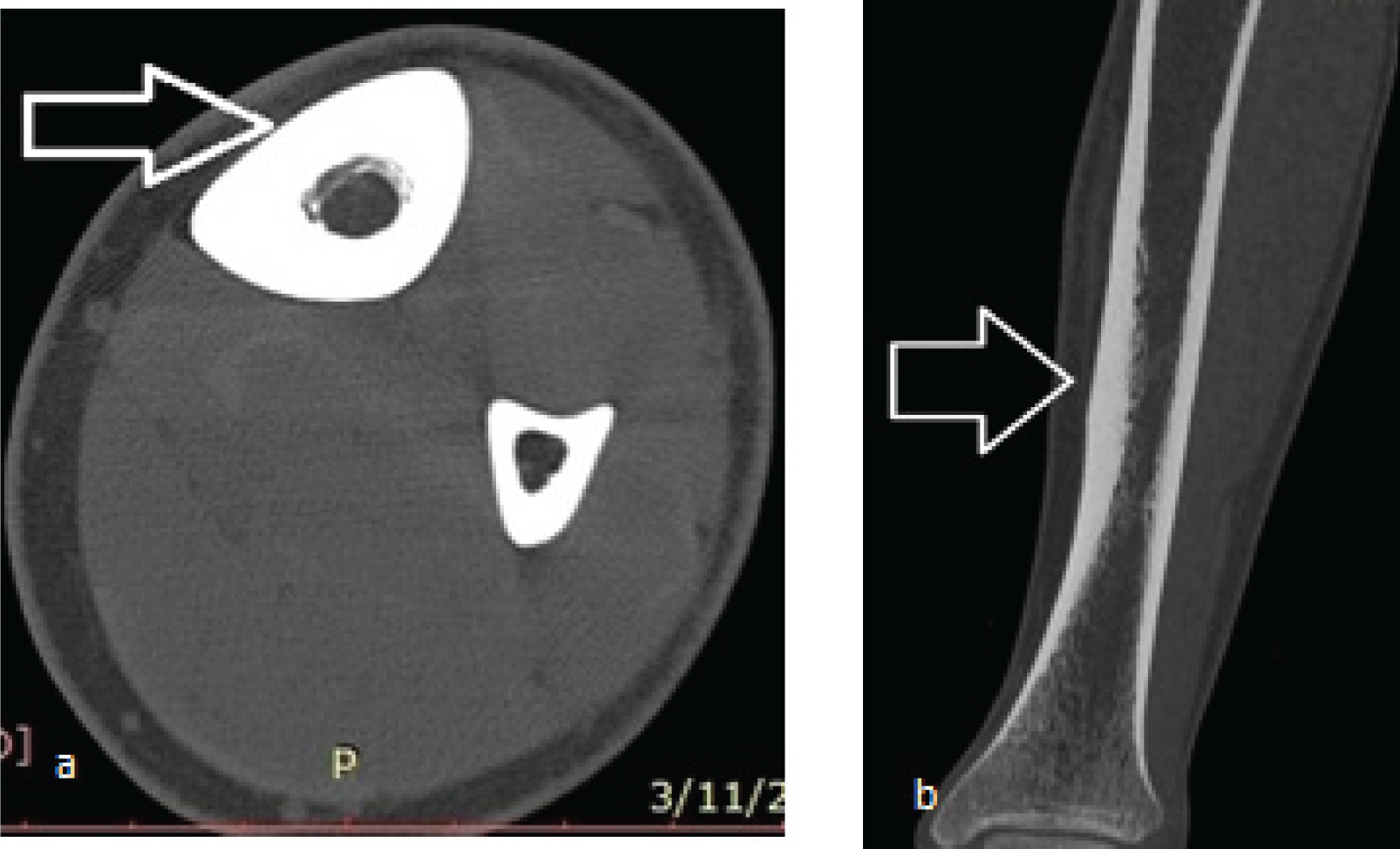
NCCT of left leg. (a) Axial section of the tibial shaft shows increased cortical thickness on the anteromedial aspect (white arrow), (b) reformat coronal section shows increased cortical thickness (white arrow).
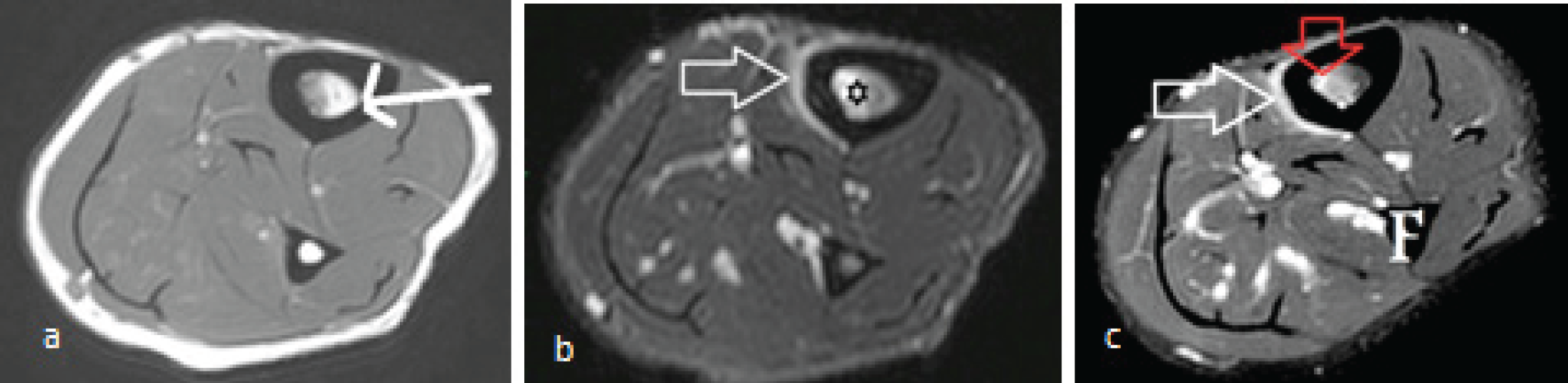
MRI of left leg (a) T1W shows normal marrow signal (white arrow) with adjoining hypointensity depicting marrow edema, (b) STIR image shows marrow edema (black star) and diagnostic moderate tibial periosteal edema in the form of hyperintensities, (c) Contrast T1W fat suppressed image shows subtle enhancement of the periosteum (white arrow) and adjoining marrow of the region (red arrow).
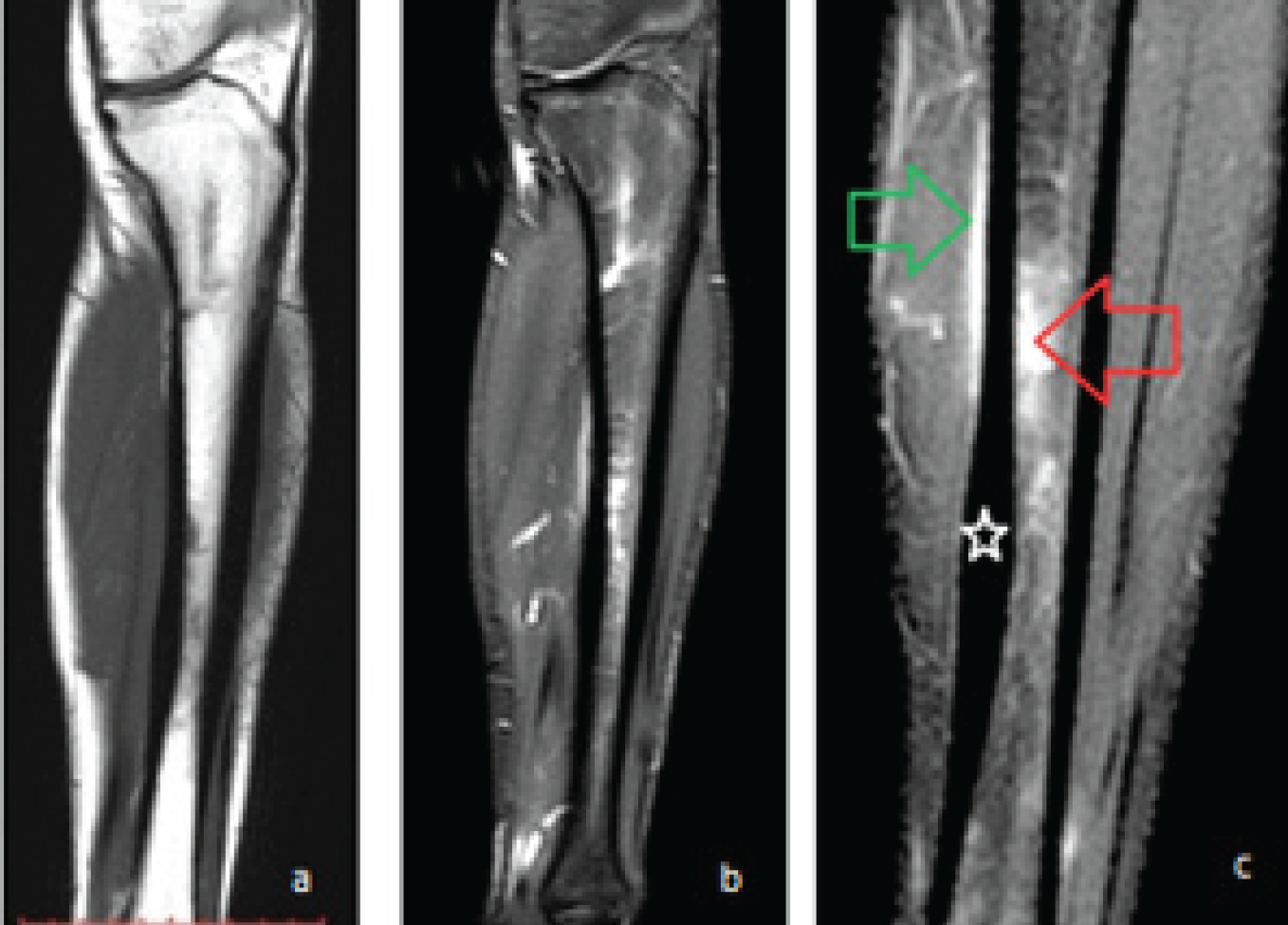
MRI sagittal sections of left leg. (a) T1W shows hypointensity in the middle shaft region, (b) T2W shows mild edema of the same region with adjacent periosteal hyperintensity, (c) STIR image show marrow hyperintensity (red arrow) and periosteal edema (green arrow). The cortical thickness of the lower shaft region is also increased (white star) as seen in the plain skiagram.
Discussion
Medial tibial stress syndrome is considered to be a type of periostitis which is seen as cortical thickening. Bone is formed of organic as well as inorganic substances. This dynamic tissue changes as per the stress and again remodel to come to the normal texture. Tibial bone of the lower leg is constantly under stress when there is overuse of the leg muscles. Tibialis posterior and soleus muscles are attached to the medial shin of the tibia. There can be mismatch between the tolerance of the bone and physical stress [2]. These biomechanical variations which can lead to medial tibial stress syndrome. Some authors suggest the pain due to the tearing of interosseous membrane. Flat foot had also been found as the causative factor [3,4]. The bone constituents can also result in easy target for the injury. This can lead to major morbidity by not allowing to proper physical activity. There is vague pain in the leg along the medial side of the shin which can disappear with some exercises but with the chronicity the pain persists. Females are 1.5 to 3.5 times more prone to stress fractures. There is triad of osteoporosis, amenorrhea and undisciplined eating seen among female athletes [5]. Any musculoskeletal injury can be evaluated by mnemonics TART (tenderness, asymmetry, restricted movement and tissue texture).
Detailed Imaging work up is very important to rule out other pathologies. The role of plain x-ray is early but MRI is required if patient fails to respond to the conservative management. Plain radiograph and NCCT can show focal increased cortical thickening or exostosis in long standing cases [6,7]. MRI has replaced bone scan which used to pick up early signs. This reveals three-dimensional study and the adjoining soft tissue structures are best delineated. The surrounding periosteal edema can also tell the severity. This is as per covering the tibial circumference. This is mild if <30%, moderate if 30-50% and severe if >50%. MRI is best for the grading as per Fredericson as this helps in the management [8,9,10]. Following are the grades for this type of trauma:
Grade 1: only periosteal edema
Grade 2: T2W MRI depicts bone marrow edema.
Grade 3: T1W and T2W MRI depict edema.
Grade 4: a) multiple intracortical signal changes. b) frank stress fractures.
Our present case falls in Type III category as there was bone marrow edema seen in both T1W and T2W MRI sequences.
The diagnosis requires to be differentiated from anterior and posterior compartmental syndromes and peripheral vascular disease where pain is always on the lateral side of the shin. Focal entrapment and rediculopathy also have to be ruled out before concluding the diagnosis. The management includes rest, on-steroidal anti-inflammatory drugs, elevation, ice therapy and compression. Other part of the management includes flexibility exercises, supportive shoes, orthotics and return to exercises as soon as possible [11]. Surgery is reserved for Grade 3b and 4 types of injuries. Proper running gear, fitness level and bare foot running can prevent these types of injuries.
Conclusion
MTSS is found as a common injury among athletes who report to the sports injury centers. Though there is no need of the imaging studies in the early cases but the detailed study is required in long standing cases of the leg pain. MRI is the best modality to grade these types of injuries so that proper management can be undertaken. In majority of the cases conservative treatment is sufficient.


