Background
Cryptorchidism is the absence of one or both testicles from the scrotal sac. This is a Greek word which means hidden testicle. The incidence is higher in premature to 30% as compared to a full term being 3%. The incidence is 1-6% of male children. This is called as monorchism if only one testis is present. Monorchism cryptorchidism is single undescended testis. Ectopic testis differs from this as in that case there is deviation of the testicle from the normal descent path and can lie somewhere else. The entity should also not be confused with retractile testis which is a normal phenomenon.
Case presentation
A 2 year old male child (Figure 1) was brought to children outpatient department by the parents with missing testes in the scrotal sac. The child was of full term delivery without any complications.
On examination, the child physical parameters were as per his age. Systemic examination was unremarkable. On local examination, it was found that the scrotal sac was empty as testes were not palpable. All the blood investigations were within normal limits. Plain skiagram for abdomen did not reveal anything. The visible bone structures were normal. The child underwent ultrasound (US) study which revealed empty scrotal sac without any anything within it. There was another well-defined testis-like hypoechoic structure seen in the left inguinal region. No other finding was noticed in the vicinity or on the contra lateral side (Figure 2).
Color Doppler did not show any flow in the testis and the surrounding region was unremarkable (Figure 3). The child was planned for magnetic resonance study of the abdomen. MRI study revealed a mixed intensity mass in T2W on the left inguinal region but there was no such structure seen on right side. T1W images were equivocal. Diffusion weighted imaging (DWI) had revealed a well-defined hyper intense structure in the left inguinal region. This is the same structure which was seen in T1W sequences (Figures 4 a, b,c, 5 a, b and 6).
The child was diagnosed with absence of right testis with single left undescended testis. The hormonal estimation had been sent and the child is planned for orchidopexy.
Photo of the two year old male child with normal height, weight and other physical parameters.
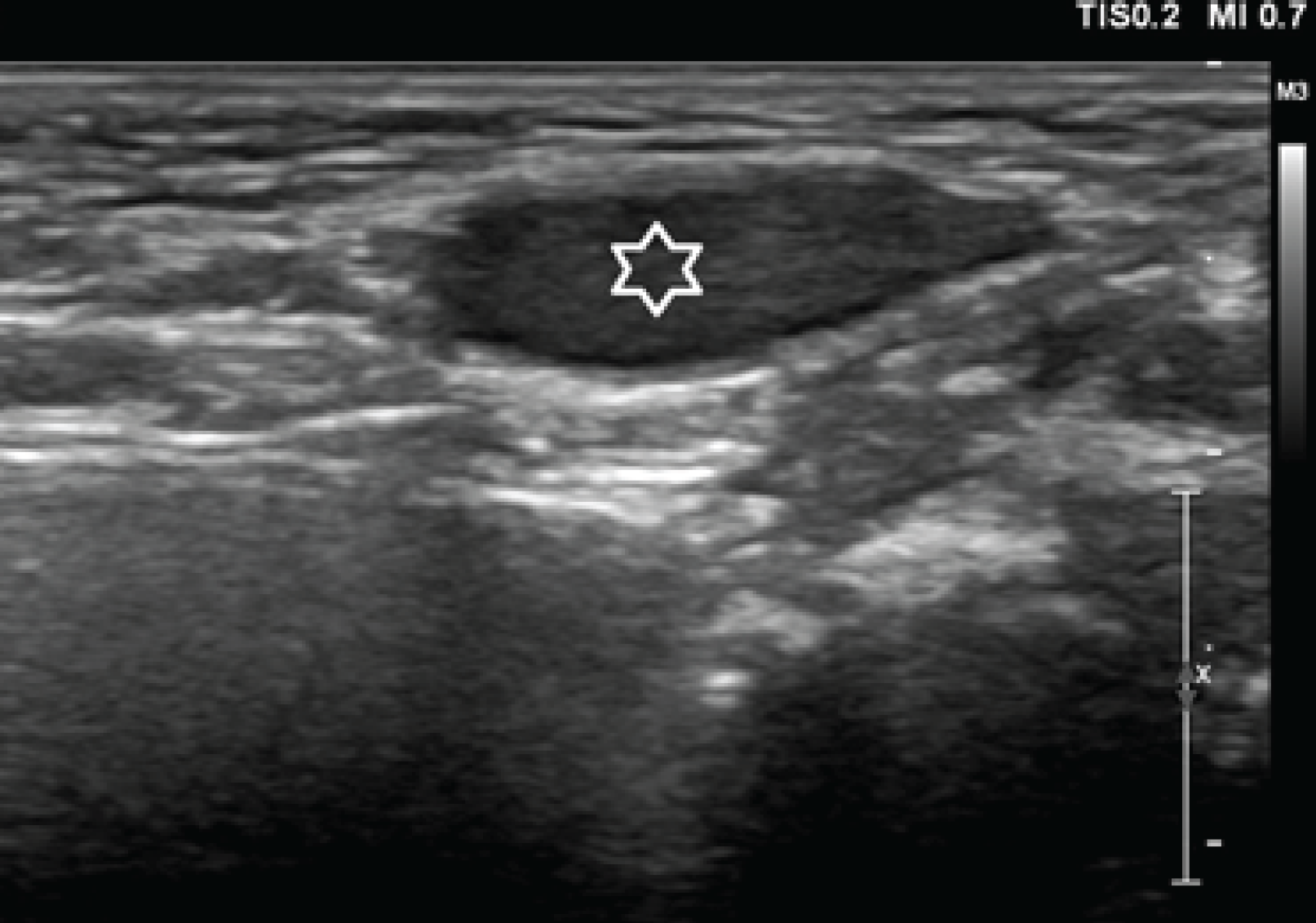
Ultrasound of the left inguinal region with 7.5 MHz linear probe. There is a well-defined oval hypoechoic region which is suspicious of left testis (white star).
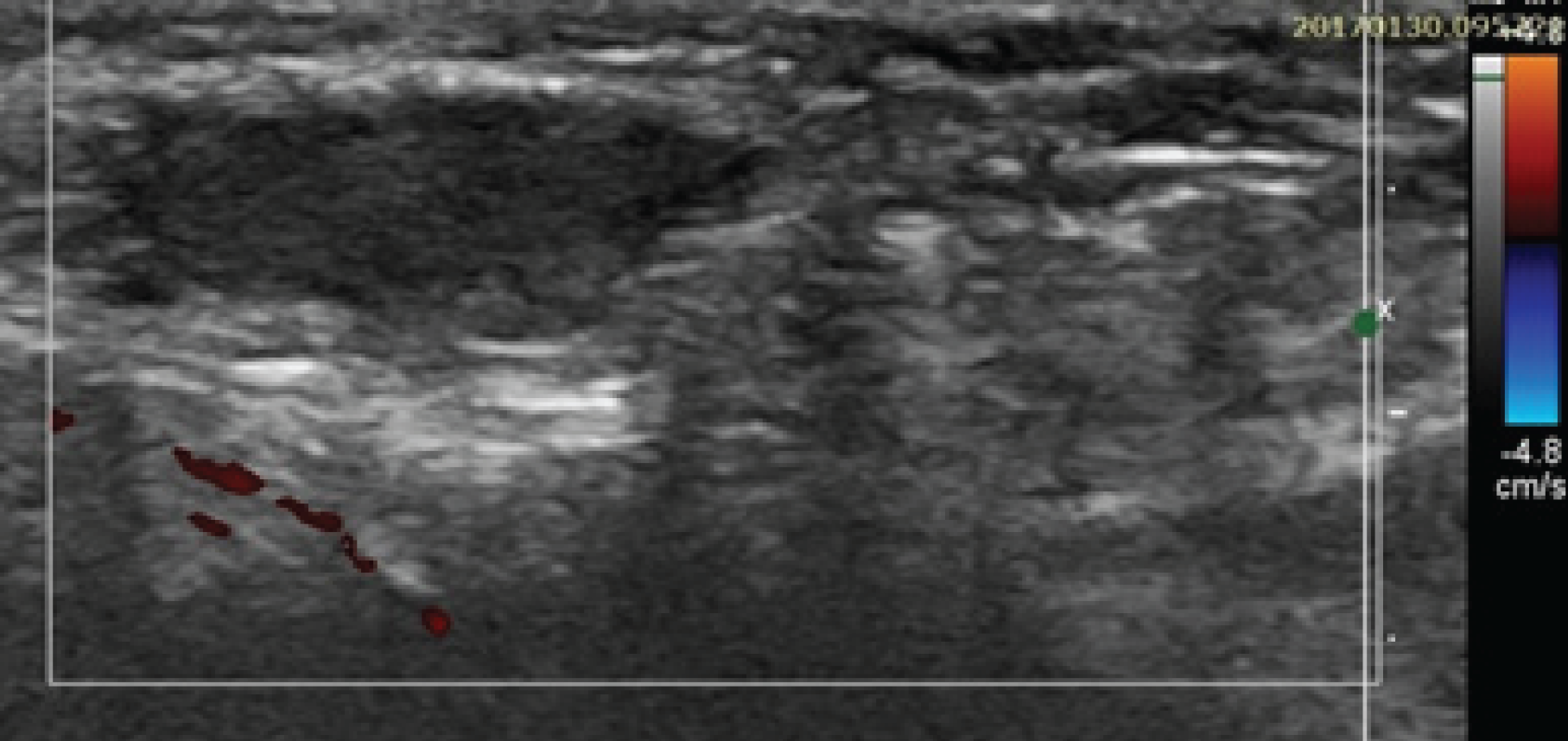
Color Doppler of the left testis in the inguinal canal region did not reveal any vascularity and the margins were very clear.

Axial sections of magnetic resonance imaging study. (a) T2W image at the level of left testis in inguinal canal (inverted white arrow). The testis is slightly hyperintense comparing to muscles. (b) T2W at slightly lower level shows only white intensity of the inguinal canal (white hollow arrow). (c) Balanced Turbo Field Echo (BTFE) image shows testis of hyperintensity in the canal (white arrow).
Discussion
Monorchism cryptorchidism is the presence of single undescended testis. Scrotal sac is usually empty. The embryonic development of testis starts at the 10th week of gestation in the abdominal cavity and comes to lie in inguinal canal and further to scrotal sac between 28th to 40th weeks of gestation. The gubernaculum (Latin word which means rudder) ligament under the influence of testosterone hormone contracts and brings the testes in the scrotal sac. In general, 60% cases shows normal descend of both the testes in scrotal sac by the end of one year. There can be various permutation and combinations during this descent and child can present accordingly with various congenital entities.
In 72% cases, the cryptorchid testis lies in inguinal canal as in our case, 20% lies in prescrotal and only 8% are seen in intra-abdominal location. The chance of testicular descent after one year is unlikely. Our case was having only one testis and that too undescended, lying in inguinal canal. There are more chances of 20-48 times for malignant transformation. There is an incidence of 5-10% undescended testis in testicular cancers [3]. This is also one of the causes of infertility and sometimes leads to hernia. Cross-sectional Imaging plays a pivotal role in locating the undescended testis. Ultrasonography (US), computerized tomography (CT), magnetic resonance imaging (MRI) and arteriography along with laparoscopy are the methods to find out cryptorchid testis. Ultrasonography remains the first choice to locate the testis below internal inguinal ring. This is noninvasive and without any radiation.
The testis is seen as oval region of low or midlevel echogenicity. This has got 91% accuracy [4]. Color Doppler shows low resistance flow spectrum in the testis [5,6]. CT is avoided because of radiation issue; otherwise this scores over US in differentiating testis from surrounding lymph node. This has got 96% accuracy. MRI is of great importance because of better tissue characterization, multiplanar capabilities, noninvasive and without any radiation. Testis is seen as hypointense in T1W and hyperintense on T2W images. DWI shows markedly Hyperintensity which is characteristic of the testis [7,8].
Orchidopexy is the choice of management [9,10]. The main aim of the surgery is to bring back the testicle to the normal position, to preserve hormonal function, fertility and to avoid future malignancy [11]. This is performed from 5 to 15 months of age. Hormonal therapy is also helpful to some extent but the results are not encouraging. Surgery should be performed in the first year otherwise, this will lead to loss of testicular functions and the condition is labeled as vanishing testis.
Conclusion
Undescended testes pose a great diagnostic challenge for their localization. The diagnosis is important because of the fear of malignant potential. The radiation should be avoided in children. Though ultrasound is the first screening modality of the diagnosis but DWI in MRI has got more diagnostic value.



